Abstract
Purpose
To report a case of psoriasis triggered by anti-tumor necrosis factor-alpha (TNF-α) therapy in a uveitis patient with Behçet’s disease.
Case report
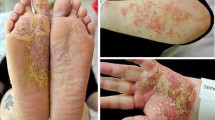
A 34-year-old man with established Behçet’s disease was started on infliximab therapy for recurrent uveitis and showed an excellent response. After 2 years of infliximab treatment, he developed erythematous scaly plaques on both of his palms and heels. No clinical or serological evidence of infection was found, and there was no personal/family history of psoriasis. Histological examination of one lesion showed that it was consistent with psoriasis. Because of the development of hyperkeratotic skin lesions consistent with guttate psoriasis, the infliximab treatment was discontinued. Six months later, the psoriasis had resolved.
Conclusions
Blockade of TNF-α is an effective treatment for psoriasis as well as Behçet’s disease. However, we have to consider new-onset psoriasis as an adverse side effect that can be triggered by anti-TNF-α therapy in Behçet’s disease.


Similar content being viewed by others
References
Shergy WJ, Isern RA, Cooley DA, Harshbarger JL, Huffstutter JE, Hughes GM, et al. Open label study to assess infliximab safety and timing of onset of clinical benefit among patients with rheumatoid arthritis. J Rheumatol. 2002;29:667–77.
Hanauer SB, Feagan BG, Lichtenstein GR, Mayer LF, Schreiber S, Colombel JF, et al. Maintenance infliximab for Crohn’s disease: the ACCENT I randomised trial. Lancet. 2002;359:1541–9.
Schopf RE, Aust H, Knop J. Treatment of psoriasis with the chimeric monoclonal antibody against tumor necrosis factor alpha, infliximab. J Am Acad Dermatol. 2002;46:886–91.
Ohno S, Nakamura S, Hori S, Shimakawa M, Kawashima H, Mochizuki M, et al. Efficacy, safety, and pharmacokinetics of multiple administration of infliximab in Behçet disease with refractory uveoretinitis. J Rheumatol. 2004;31:1362–8.
Sfikakis PP, Kaklamanis PH, Elezoglou A, Katsilambros N, Theodossiadis PG, Papaefthimiou S, et al. Infliximab for recurrent, sight-threatening ocular inflammation in Adamantiades-Behçet disease. Ann Intern Med. 2004;140:404–6.
Yamada Y, Sugita S, Tanaka H, Kamoi K, Kawaguchi T, Mochizuki M. Comparison of infliximab versus cyclosporine during the initial 6-month treatment period in Behçet disease. Br J Opthalmol. 2010;94:284–8.
Keino H, Okada AA, Watanabe T, Taki W. Decreased ocular inflammatory attacks and background retinal and disc vascular leakage in patients with Behcet’s disease on infliximab therapy. Br J Ophthalmol. 2011;95:1245–50.
Wang Y, Gaudio PA. Infliximab therapy for 2 patients with Vogt–Koyanagi–Harada syndrome. Ocul Immunol Inflamm. 2008;16:167–71.
Ito T, Sonoda KH, Hijioka K, Fujimoto T, Ishibashi T. Acquired resistance to infliximab against uveitis due to Behçet’s disease after one year of administration. Jpn J Ophthalmol. 2010;54:502–4.
Sfikakis PP, Iliopoulos A, Elezoglou A, Kittas C, Stratigos A. Psoriasis induced by anti-tumor necrosis factor therapy. Arthr Rheum. 2005;52:2513–8.
Kary S, Worm M, Audring H, Huscher D, Renelt M, Sörensen H, et al. New onset or exacerbation of psoriatic skin lesions in patients with definite rheumatoid arthritis receiving tumour necrosis factor alpha antagonists. Ann Rheum Dis. 2006;65:405–7.
Matthews C, Rogers S, FitzGerald O. Development of new-onset psoriasis while on anti-TNFalpha treatment. Ann Rheum Dis. 2006;65:1529–30.
Collamer AN, Battafarano DF. Psoriatic skin lesions induced by tumor necrosis factor antagonist therapy: clinical features and possible immunopathogenesis. Semin Arthr Rheum. 2010;40:233–40.
Laga AC, Vleugels RA, Qureshi AA, Velazquez EF. Histopathologic spectrum of psoriasiform skin reactions associated with tumor necrosis factor-α inhibitor therapy. A study of 16 biopsies. Am J Dermatopathol. 2010;32:568–73.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kawazoe, Y., Sugita, S., Yamada, Y. et al. Psoriasis triggered by infliximab in a patient with Behçet’s disease. Jpn J Ophthalmol 57, 95–97 (2013). https://doi.org/10.1007/s10384-012-0198-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-012-0198-4