Summary
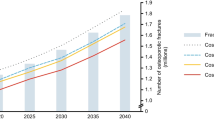
Worldwide osteoporosis is underestimated and despite availability of effective and cost effective treatments, these are often not implemented. Apart from a demographically driven increase in disease cases, failure to implement or tardy implementation of preventive measures as well as poor treatment compliance leads to a deterioration of the health economic outcomes. This in turn causes considerable costs to the health care system and to society, through ineffective intake of medication, diminished quality of life and inability to work as well as substantial costs of rehabilitation of patients. Health economic analyses and methods are increasingly used by decision makers to set priorities and evaluate alternative treatment measures about their cost-effectiveness. In order to be able to capture the costs of illness incurred by osteoporosis, different diseases specific models and methods have been developed, such as the reference model of the IOF, an osteoporosis-specific Markov model or internationally comparable intervention thresholds. Health economists estimate that osteoporosis-related costs will double by 2050 in both Europe and the individual countries. For Europe this means an increase from €40 billion in 2000 to almost €80 billion in 2050. In Austria, an aggregation of the different costs of osteoporosis is not possible, due to a lack of comparability and availability of data. The international ICUROS study and the Austrian Osteoporosis Report 2007 are the first steps towards counteracting this situation.
Zusammenfassung
Osteoporose wird weltweit unterdiagnostiziert und trotz wirksamer und kosten-effektiver Therapien werden diese oft nicht angewandt. Abgesehen von einem demographisch bedingten Anstieg an Osteoporosefällen führen fehlende bzw. zu spät einsetzende Präventionsmaßnahmen und eine geringe Therapie-Compliance zu einer Verschlechterung des gesundheitsökonomischen Outcomes. Dies wiederum verursacht erhebliche Kosten im Gesundheitssystem und in der Gesellschaft, durch ineffektive Medikamenteneinnahme, Arbeitsunfähigkeit sowie erhebliche Kosten in der Rehabilitation der Patientinnen und Patienten. Dazu kommt die verminderte Lebensqualität der Betroffenen. Gesundheitsökonomische Bewertungen und Analysen werden immer häufiger von Entscheidungsträgern verwendet, um Prioritäten zu setzen und alternative Behandlungskonzepte auf ihre Kosten-Effektivität zu bewerten. Zur Bestimmung der Krankheits- und Folgekosten von Osteoporose wurden eigene Modelle entwickelt. So gibt es das Referenzmodell der IOF, ein eigenes validiertes Markov-Modell und Ansätze zur Ermittlung international vergleichbarer Schwellenwerte. Gesundheitsökonomen schätzen, dass sich die Osteoporose-bedingten Kosten sowohl für Europa als auch für die einzelnen Länder bis 2050 verdoppeln werden. Für Europa bedeutet dies einen Anstieg von etwa €40 Milliarden im Jahr 2000 auf fast €80 Milliarden 2050. Für Österreich ist eine Aggregierung der einzelnen Kostenblöcke derzeit nur schwer möglich, da sich Erhebungsmethoden und verwendetes Datenmaterial oft erheblich voneinander unterscheiden. Die ICUROS-Studie sowie der Österreichische Osteoporosebericht 2007 bieten erste Unterlagen, dieser Situation entgegen zu wirken.
Similar content being viewed by others
Literatur
European Parliament Osteoporosis Interest Group and EU Osteoporosis Consultation Panel. Osteoporosis in Europe: Indicators of progress, 2004
Fleurence RL, Iglesias CP, Torgerson DJ. Economic evaluations of interventions for the prevention and treatment of osteoporosis: a structured review of the literature. Osteoporos Int, 17: 29–40, 2006
Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen. Allgemeine Methoden. Version 3.0 vom 27.05.2008. http://www.iqwig.de/download/IQWiG_Methoden_Version_3_0.pdf, letzter Zugriff, 28.12.2008
Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen. Technischer Anhang Modellierung. Version 1.0 vom 09.10.2008. http://www.iqwig.de/download/TA_KNB_Modellierung_v_1_0.pdf, letzter Zugriff, 28.12.2008
Urdahl H, Manca A, Sculpher MJ. Assessing generalisability in model-based economic evaluation studies: a structured review in osteoporosis. Pharmacoeconomics, 24: 1181–1197, 2006
Morrison A, Wertheimer AI. Types of pharmacoeconomic evaluation. In: Morrison A, Wertheimer AI (eds) Pharmacoeconomics. A primer for the pharmaceutical industry. Temple University, Philadelphia, 2002
Dzajkovska B, Wertheimer AI, Mrhar, A. The burden-of-illness study on osteoporosis in the Slovenian female population. Pharm World Sci, 29: 404–411, 2007
Kamel HK, Hussain MS, Tariq S, et al. Failure to diagnose and treat osteoporosis in elderly patients hospitalized with hip fracture. Am J Med, 109: 326–328, 2000
Gehlbach SH, Bigelow C, Heimisdottir M, et al. Recognition of vertebral fracture in a clinical setting. Osteoporos Int, 11: 577–582, 2000
Burge RT, King AB, Balda E, Worley D. Methodology for estimating current and future burden of osteoporsis in state populations: application to Florida in 2000 through 2025. Value Health, 6: 574–583, 2006
Melton LJ III, Thamer M, Ray NF, et al. Fractures attributable to osteoporosis: report from the National Osteoporosis Foundation. J Bone Miner Res, 12: 16–23, 1997
Tosteson ANA, Jonsson B, Grima DT, et al. Challenges for model-based economic evaluations of postmenopausal osteoporosis interventions. Osteoporos Int, 12: 849–857, 2001
Zethraeus N, Borgström F, Ström O, Kanis JA, Jönsson B. Cost-effectiveness of the treatment and prevention of osteoporosis – a review of the literature and a reference model. Osteoporos Int, 18: 9–23, 2007
Ström O, Zethraeus N, Borgström F, Johnell O, Jönsson B, Kanis J. IOF cost-effectiveness modell. Background Document, issued November 2006. http://www.iofbonehealth.org/health-professionals/health-economics/cost-effectiveness-model.html, letzter Zugriff Juli 2008
Ström O, Borgström F, Kanis JA, Jönsson B. Incorporating adherence into health economic modelling of osteoporosis. Osteoporos Int, 20: 23–34, 2009
Boonen S, Singer AJ. Osteoporosis management: impact of fracture type on cost and quality of life in patients at risk of fracture (part 1 of 2). Curr Med Res Opin, 24: 1783–1790, 2008
Borgström F, Johnell O, Kanis JA, Jönsson B, Rehnberg C. At what hip fracture risk is it cost-effective to treat? International intervention thresholds for the treatment of osteoporosis. Osteoporos Int, 17: 1459–1471, 2006
Kanis JA, Borgström F, Zethraeus N, Johnell O, Odén A, Jönsson B. Intervention thresholds for osteoporosis in the UK. Bone, 36: 22–32, 2005
Kanis JA, Johnell O, Odén A, Borgström F, Johansson H, De Laet C, Jönsson B. Intervention thresholds for osteoporosis in men and women: a study based on data from Sweden. Osteoporos Int, 16: 6–14, 2005
Tosteson ANA, Melton LJ III, Dawson-Hughes B, et al. Cost-effective osteoporosis treatment thresholds: the United States perspective. Osteoporos Int, 19: 437–447, 2008
Kanis JA, Black D, Cooper C, et al. IOF/NOF. A new approach to the development of assessment guidelines for osteoporosis. Osteoporos Int, 13: 527–536, 2002
Kanis JA, Oden A, Johnell O, Jönsson B, de Laet C, Dawson A. The burden of osteoporotic fractures: a method for setting intervention thresholds. Osteoporos Int, 12: 417–427, 2001
Kanis JA, Brazier JE, Stevenson M, Calvert NW, Lloyd Jones M. Treatment of established osteoporosis: a systematic review and cost-utility analysis. Health Technol Assess, 6: 1–146, 2002
Lips P, van Schoor NM. Quality of life in patients with osteoporosis. Osteoporos Int, 16: 447–455, 2005
Salaffi F, Cimmino MA, Malavolta N, et al. On behalf of the Italian Multicentre Osteoporotic Fracture (IMOF) Study Group. J Rheumatol, 34: 1551–1560, 2007
Tosteson ANA, Gabriel SE, Grove MR, Moncur MM, Kneeland TS, Melton LJ III. Impact of hip a vertebral fractures on quality-adjusted life years. Osteoporos Int, 12: 1042–1049, 2001
Finnern HW, Sykes DP. The hospital cost of vertebral fractures in the EU: estimates using national data sets. Osteoporos Int, 14: 429–436, 2003
European Commission. Summary report on osteoporosis in the European Community – Action for prevention. European Communities/European Foundation for Osteoporosis (EFFO – now IOF), 1998
Lindsay R, Burge RT, Strauss DM. One year outcomes and costs following a vertebral fracture. Osteoporos Int, 16: 78–85, 2005
Weber K. Volkskrankheit Osteoporose: die Situation spitzt sich zu. Rheuma Plus, 4: 3, 2004
Rabenda V, Manette C, Lemmens R, Mariani A-M, Struvay N, Reginster J-Y. The direct and indirect costs of the chronic management of osteoporosis: a prospective follow-up of 3440 active subjects. Osteoporos Int, 17: 1346–1352, 2006
Kowalski SC, Szenzfeld VL, Ferraz MB. Resource utilisation in postmenopausal osteoporosis without incident fractures. J Rheumatol, 31: 938–942, 2004
Seeman E, Compston J, Adachi J, et al. Non-compliance: the Achilles' heel of anti-fracture efficacy. Osteoporos Int, 18: 711–719, 2007
Iskedjian M, Einarson TR, MacKeigan LD, Shear N, Addis A, Mittmann , Ilersich AL. Relationship between daily dose frequency and adherence to antihypertensive pharmacotherapy: evidence from a meta-analysis. Clin Ther, 24: 302–316, 2002
Cramer J, Silverman S. Persistence with bisphosphonate treatment for osteoporosis: finding the root of the problem. Am J Med, 119(4 Suppl 1): 12–17, 2006
Brucksch M, Teyke T, Schurr MO. Compliance bei Arzneimitteln: ein unterschätztes Problem. Pharmacoeconomics, 1: 3–8, 2005
Weichselbaum E, Dorner T, Lawrence K, Rieder A. Österreichischer Osteoporosebericht 2007. Verein Altern mit Zukunft, Vienna 2007
Sander B, Elliot-Gibson V, Beatin DE, Bogoch ER, Maetzel A. A coordinator program in post-fracture osteoporosis management improves outcomes and saves costs. J Bone Joint Surg Am, 90: 1197–1205, 2008
Jaglal SB, Hawker G, Bansod V, et al. A demonstration project of a multi-component educational intervention to improve integrated post-fracture osteoporosis care in five rural communities in Ontario, Canada. Osteoporos Int, 20: 265–274, 2009
Ayoub WT, Newman ED, Blosky MA, Stewart WF, Wood GC. Improving detection and treastment of osteoporosis: redesigning care usin the electronic medical record and shared medical appointments. Osteoporos Int, 20: 37–42, 2009
Brennan A, Chick SE, Davies R. A taxonomy of model structures for economic evaluation of health technologies. Health Econ, 15: 1295–1310, 2006
Reed J, Cook G, Childs S, McCormack B. A literature review to explore integrated care for older people. Int J Integr Care, 5: e17, 2005. (Epub, Jan. 14, 2005)
Leichsenring K. Developing integrated health and social care services for older persons in Europe. Int J Integr Care, 4: e10, 2004. (Epub, Sept. 3, 2004)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Viktoria Stein, K., Dorner, T., Lawrence, K. et al. Ökonomische Konzepte zur Erfassung der Krankheitskosten von Osteoporose: Österreich im internationalen Vergleich. Wien Med Wochenschr 159, 253–261 (2009). https://doi.org/10.1007/s10354-009-0674-8
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s10354-009-0674-8