Abstract
Purpose
Many studies have demonstrated the convergence of vagal inputs into brainstem centers with inputs from the urinary bladder and colon, as well as the convergence of vagal inputs into other centers controlling the urinary bladder and colon reflexes. However, the effect of the vagal inputs on the interaction between the urinary bladder and other pelvic organs has not been studied. In this study, the effect of bilateral cervical vagotomy on the distal colon to urinary bladder reflex was examined.
Methods
Changes to cystometry parameters in response to increased distal colon distensions (1, 2, and 3 ml) were tested in urethane-anesthetized male rats with or without bilateral cervical vagotomy.
Results
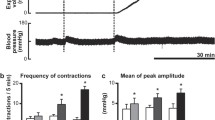
In animals with intact vagus nerves, 1 and 2 ml distal colon distentions had no significant effects on micturition frequency; however, 3 ml distal colon distention significantly decreased the frequency of micturition cycles. Also, 3 ml distal colon distention inhibited micturition cycles in 37.5 % of these animals. On the other hand, following cervical vagotomy, 1 ml distal colon distention was enough to significantly decrease the frequency of micturition cycles and to inhibit the cycles in 75 % of the animals.
Conclusion
These results demonstrate the presence of supraspinal inhibitory regulation, via the vagus nerve, over the distal colon to urinary bladder inhibitory reflex.






Similar content being viewed by others
References
Baez MA, Brink TS, Mason P (2005) Roles for pain modulatory cells during micturition and continence. J Neurosci 25:384–394
Berkley KJ, Hubscher CH, Wall PD (1993) Neuronal responses to stimulation of the cervix, uterus, colon, and skin in the rat spinal cord. J Neurophysiol 69:545–556
Charach G, Greenstein A, Rabinovich P, Groskopf I, Weintraub M (2001) Alleviating constipation in the elderly improves lower urinary tract symptoms. Gerontology 47:72–76
Chen SL, Wu XY, Cao ZJ, Fan J, Wang M, Owyang C, Li Y (2008) Subdiaphragmatic vagal afferent nerves modulate visceral pain. Am J Physiol Gastrointest Liver Physiol 294:G1441–G1449
Christianson JA, Liang R, Ustinova EE, Davis BM, Fraser MO, Pezzone MA (2006) Convergence of bladder and colon sensory innervation occurs at the primary afferent level. Pain 128(3):235–243
de Groat WC (1998) Anatomy of the central neural pathways controlling the lower urinary tract. Eur Urol 34(Suppl 1):2–5
Floyd K, McMahon SB, Morrison JF (1978) Inhibition of the micturition reflex by stimulation of pelvic nerve afferents from the colon [proceedings]. J Physiol 284:39P–40P
Floyd K, McMahon SB, Morrison JF (1979) Inhibitory interactions between the colonic and vesical branches of the pelvic nerve in the cat [proceedings]. J Physiol 290:50P–51P
Halachmi S, Farhat WA (2008) The impact of constipation on the urinary tract system. Int J Adolesc Med Health 20:17–22
Heinricher MM, Tavares I, Leith JL, Lumb BM (2009) Descending control of nociception: specificity, recruitment and plasticity. Brain Res Rev 60:214–225
Hummel T, Barz S, Holscher T, Neuhuber WL (2003) Differences in responses to nociceptive stimulation of the oral and aboral oesophagus. J Clin Neurosci 10:223–225
Kaddumi EG, Hubscher CH (2006) Convergence of multiple pelvic organ inputs in the rat rostral medulla. J Physiol 572:393–405
Kaddumi EG, Qnais EY, Allouh MZ (2012) Effect of esophagus distention on urinary bladder function in rats. Neurourol Urodyn 31:174–177
Karimnamazi H, Travers SP, Travers JB (2002) Oral and gastric input to the parabrachial nucleus of the rat. Brain Res 957:193–206
McMahon SB, Spillane K (1982) Brain stem influences on the parasympathetic supply to the urinary bladder of the cat. Brain Res 234:237–249
Meyer RE, Fish RE (2008) Pharmacology of injectable anesthetics, sedatives, and tranquilizeres. In: Fish RE, Danneman PJ, Brown M, Karas A (eds) Anesthesia and analgesia in laboratory animals. American college of laboratory animal medicine series. Academic Press, London, p 57
Monnikes H, Ruter J, Konig M, Grote C, Kobelt P, Klapp BF, Arnold R, Wiedenmann B, Tebbe JJ (2003) Differential induction of c-fos expression in brain nuclei by noxious and non-noxious colonic distension: role of afferent C-fibers and 5-HT3 receptors. Brain Res 966:253–264
Mtui EP, Anwar M, Reis DJ, Ruggiero DA (1995) Medullary visceral reflex circuits: local afferents to nucleus tractus solitarii synthesize catecholamines and project to thoracic spinal cord. J Comp Neurol 351:5–26
Ness TJ, Piper JG, Follett KA (1999) The effect of spinal analgesia on visceral nociceptive neurons in caudal medulla of the rat. Anesth Analg 89:721–726
Peng HY, Chen GD, Tung KC, Lai CY, Hsien MC, Chiu CH, Lu HT, Liao JM, Lee SD, Lin TB (2009) Colon mustard oil instillation induced cross-organ reflex sensitization on the pelvic–urethra reflex activity in rats. Pain 142:75–88
Qin C, Foreman RD (2004) Viscerovisceral convergence of urinary bladder and colorectal inputs to lumbosacral spinal neurons in rats. NeuroReport 15:467–471
Qin C, Malykhina AP, Akbarali HI, Foreman RD (2005) Cross-organ sensitization of lumbosacral spinal neurons receiving urinary bladder input in rats with inflamed colon. Gastroenterology 129:1967–1978
Rong PJ, Zhu B, Huang QF, Gao XY, Ben H, Li YH (2005) Acupuncture inhibition on neuronal activity of spinal dorsal horn induced by noxious colorectal distention in rat. World J Gastroenterol 11:1011–1017
Rouzade-Dominguez ML, Pernar L, Beck S, Valentino RJ (2003) Convergent responses of Barrington’s nucleus neurons to pelvic visceral stimuli in the rat: a juxtacellular labelling study. Eur J Neurosci 18:3325–3334
Shefchyk SJ (2001) Sacral spinal interneurones and the control of urinary bladder and urethral striated sphincter muscle function. J Physiol 533:57–63
Sugaya K, Nishijima S, Miyazato M, Ogawa Y (2005) Central nervous control of micturition and urine storage. J Smooth Muscle Res 41:117–132
Van Bockstaele EJ, Peoples J, Telegan P (1999) Efferent projections of the nucleus of the solitary tract to peri-locus coeruleus dendrites in rat brain: evidence for a monosynaptic pathway. J Comp Neurol 412:410–428
Whorwell PJ, Lupton EW, Erduran D, Wilson K (1986) Bladder smooth muscle dysfunction in patients with irritable bowel syndrome. Gut 27:1014–1017
Wyndaele M, De Wachter S, De Man J, Minagawa T, Wyndaele JJ, Pelckmans PA, De Winter BY (2013) Mechanisms of pelvic organ crosstalk: 1. Peripheral modulation of bladder inhibition by colorectal distention in rats. J Urol 190:765–771
Acknowledgments
The author is grateful for the support of the Deanship of Scientific Research and Graduate Studies at The Hashemite University, Zarqa, Jordan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaddumi, E.G. Cervical vagotomy increased the distal colon distention to urinary bladder inhibitory reflex in male rats. Clin Auton Res 26, 33–39 (2016). https://doi.org/10.1007/s10286-015-0326-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10286-015-0326-6