Abstract
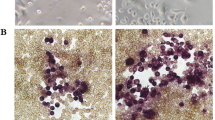
Porphyromonas gingivalis strongly correlates with periodontitis, but the underlying mechanisms causing dentoalveolar bone resorption are not fully understood. As contradictory effects of P. gingivalis on osteoclastogenesis have been reported, this study investigates the effect of P. gingivalis extract on osteoclast formation. Osteoclast formation in mouse bone marrow (MBM) cell cultures and RAW 264.7 cells was stimulated by nuclear factor-κB ligand (RANKL) or parathyroid hormone (PTH). Cells were cultured with and without P. gingivalis surface-associated material and phenotypic characteristics were examined using microscopy, flow cytometry, and RT-PCR. P. gingivalis significantly decreased osteoclast formation and the expression of osteoclast phenotypic markers in PTH-stimulated MBM cultures. Additionally, P. gingivalis inhibited expression of osteoclast differentiation factors and stimulated expression of the mouse macrophage marker F4/80. The presence of P. gingivalis in RANKL-stimulated MBM cultures and RAW 264.7 cells inhibited osteoclastogenesis. Interestingly, a transient exposure with P. gingivalis before PTH stimulation increased osteoclastogenesis in MBM cultures. Flow cytometric analyses of cells transiently exposed to P. gingivalis demonstrated an increased proportion of potential osteoclast precursor cells. We conclude that a transient exposure of MBM cultures to P. gingivalis increases the number of osteoclast precursors and osteoclast formation, whereas a prolonged exposure completely abolishes osteoclastogenesis.









Similar content being viewed by others
References
Taylor JJ. Cytokine regulation of immune responses to Porphyromonas gingivalis. Periodontology 2000. 2010;54:160–94.
Pihlstrom BC, Michalowicz BS, Johnson DW. Periodontal diseases. Lancet. 2005;366:1809–20.
Darveau RP. Periodontitis: a polymicrobial disruption of host homeostasis. Nat Rev Microbiol. 2010;8:481–90.
Cochran DL. Inflammation and bone loss in periodontal disease. J Periodontol. 2008;79(Suppl):1569–76.
Teitelbaum SL. Bone resorption by osteoclasts. Science. 2000;289:1504–8.
Boyce BF, Schwarz EM, Xing L. Osteoclast precursors: cytokine-stimulated immunomodulators of inflammatory bone disease. Curr Opin Rheumatol. 2006;18:427–32.
Trouvin AP, Goëb V. Receptor activator of nuclear factor-κB ligand and osteoprotegerin: maintaining the balance to prevent bone loss. Clin Interv Aging. 2010;5:345–54.
Takayanagi H. New immune connections in osteoclast formation. Ann N Y Acad Sci. 2010;1192:117–23.
Ukai T, Yumoto H, Gibson FC 3rd, Genco CA. Macrophage-elicited osteoclastogenesis in response to bacterial stimulation requires Toll-like receptor 2-dependent tumor necrosis factor-alpha production. Infect Immun. 2008;76:812–9.
Kelk P, Claesson R, Hänström L, Lerner UH, Kalfas S, Johansson A. Abundant secretion of bioactive IL-1β by human macrophages induced by Actinobacillus actinomycetemcomitans leukotoxin. Infect Immun. 2005;73:453–8.
Koide M, Kinugawa S, Takahashi N, Udagawa N. Osteoclastic bone resorption induced by innate immune responses. Periodontol. 2000;2010(54):235–46.
Kelk P, Claesson R, Chen C, Sjöstedt A, Johansson A. IL-1ß secretion induced by Aggregatibacter (Actinobacillus) actinomycetemcomitans is mainly caused by the leukotoxin. Int J Med Microbiol. 2008;298:529–41.
Kawai T, Matsuyama T, Hosokawa Y, Makihira S, Seki M, Karimbux NY, Goncalves RB, Valverde P, Dibart S, Li YP, Miranda LA, Ernst CW, Izumi Y, Taubman MA. B and T lymphocytes are the primary sources of RANKL in the bone resorptive lesion of periodontal disease. Am J Pathol. 2006;169:987–98.
Lamont RJ, Jenkinson HF. Subgingival colonization by Porphyromonas gingivalis. Oral Microbiol Immunol. 2000;15:341–9.
Imamura T. The role of gingipains in the pathogenesis of periodontal disease. J Periodontol. 2003;74:111–8.
Johansson A, Kalfas S. Characterization of protease-dependent cytotoxicity of Porphyromonas gingivalis. Eur J Oral Sci. 1998;106:863–71.
Meka A, Bakthavatchalu V, Sathishkumar S, Lopez MC, Verma RK, Wallet SM, Bhattacharyya I, Boyce BF, Handfield M, Lamont RJ, Baker HV, Ebersole JL, Kesavalu L. Porphyromonas gingivalis infection-induced tissue and bone transcriptional profiles. Mol Oral Microbiol. 2010;25:61–74.
Fujimura Y, Hotokezaka H, Ohara N, Naito M, Sakai E, Yoshimura M, Narita Y, Kitaura H, Yoshida N, Nakayama K. The hemoglobin receptor protein of Porphyromonas gingivalis inhibits receptor activator NF-kappaB ligand-induced osteoclastogenesis from bone marrow macrophages. Infect Immun. 2006;74:2544–51.
Scheres N, de Vries TJ, Brunner J, Laine ML, Everts V. Diverse effects of Porphyromonas gingivalis on human osteoclast formation. Microb Pathog. 2011;51:149–55.
Belibasakis GN, Bostanci N, Hashim A, Johansson A, Aduse-Opoku J, Curtis MA, Hughes FJ. Regulation of RANKL and OPG gene expression in human gingival fibroblasts and periodontal ligament cells by Porphyromonas gingivalis: a putative role of the Arg-gingipains. Microb Pathog. 2007;43:46–53.
Reddi D, Bostanci N, Hashim A, Aduse-Opoku J, Curtis MA, Hughes FJ, Belibasakis GN. Porphyromonas gingivalis regulates the RANKL-OPG system in bone marrow stromal cells. Microbes Infect. 2008;10:1459–68.
Liu J, Wang S, Zhang P, Said-Al-Naief N, Michalek SM, Feng X. Molecular mechanism of the bifunctional role of lipopolysaccharide in osteoclastogenesis. J Biol Chem. 2009;284:12512–23.
Lombardo E, Alvarez-Barrientos A, Maroto B, Boscá L, Knaus UG. TLR4-mediated survival of macrophages is MyD88 dependent and requires TNF-alpha autocrine signalling. J Immunol. 2007;178:3731–9.
Hajishengallis G, Wang M, Liang S, Shakhatreh MA, James D, Nishiyama S, Yoshimura F, Demuth DR. Subversion of innate immunity by periodontopathic bacteria via exploitation of complement receptor-3. Adv Exp Med Biol. 2008;632:203–19.
Ransjö M, Lie A, Mackie EJ. Cholera toxin and forskolin stimulate formation of osteoclast-like cells in mouse marrow cultures and cultured mouse calvarial bones. Eur J Oral Sci. 1999;107:45–54.
Paster BJ, Olsen I, Aas JA, Dewhirst FE. The breadth of bacterial diversity in the human periodontal pocket and other oral sites. Periodontol. 2000;2006:80–7.
Fitzpatrick RE, Campbell PD, Sivagurunathan S, Pagel CN, Potempa J, Mackie EJ, Pike RN. The gingipains from Porphyromonas gingivalis do not directly induce osteoclast differentiation in primary mouse bone marrow cultures. J Periodontal Res. 2009;44:565–7.
Flad HD, Grage-Griebenow E, Petersen F, Scheuerer B, Brandt E, Baran J, Pryjma J, Ernst M. The role of cytokines in monocyte apoptosis. Pathobiology. 1999;67:291–3.
Väänänen HK, Laitala-Leinonen T. Osteoclast lineage and function. Arch Biochem Biophys. 2008;473:132–8.
Muto A, Mizoguchi T, Udagawa N, Ito S, Kawahara I, Abiko Y, Arai A, Harada S, Kobayashi Y, Nakamichi Y, Penninger JM, Noguchi T, Takahashi N. Lineage-committed osteoclast precursors circulate in blood and settle down into bone. J Bone Miner Res. 2011;12:2978–90.
Behl Y, Siqueira M, Ortiz J, Li J, Desta T, Faibish D, Graves DT. Activation of the acquired immune response reduces coupled bone formation in response to a periodontal pathogen. J Immunol. 2008;181:8711–8.
Acknowledgments
This study was supported by the Swedish Dental Association and Research Fund (TUA) of Västerbotten County, Sweden.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bougas, K., Ransjö, M. & Johansson, A. Effects of Porphyromonas gingivalis surface-associated material on osteoclast formation. Odontology 101, 140–149 (2013). https://doi.org/10.1007/s10266-012-0068-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-012-0068-z