Abstract
Objective
The aim of our study was to compare the magnetic resonance imaging (MRI)-defined cross-sectional area and semi-quantitative grading of fatty degeneration of lumbar paravertebral muscles in patients with non-radiographic axial spondyloarthritis (nr-axSpA) and established ankylosing spondylitis (AS).
Methods
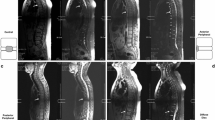
Cross-sectional area (CSA) of lumbar paravertebral muscles, including the right and left multifidus (MF), erector spina (ES), psoas (PS), vertebral body and muscle:vertebra ratio (MVr), was measured. Fat infiltration of the paravertebral muscles was graded semi-quantitatively.
Results
The CSA of the MF, ES and PS muscles and the MVr (at the L2, L3, L4 and L5 levels) were quite similar between patients with nr-axSpA (n = 14) and AS (n = 22). However, patients with AS had higher grades of fat infiltration than those with nr-axSpA (Right L4 grading of MF + ES muscles: 1.4 ± 0.73 vs. 0.51 ± 0.52, respectively, p = 0.001; left L4 grading: 1.36 ± 0.65 vs. 0.38 ± 0.50, respectively, p < 0.0001). This difference remained significant after adjusting for age and symptom duration. The inter-rater reliability was good (intraclass correlation coefficient 0.75 and 0.85).
Conclusions
This is first study demonstrating that MRI-defined fatty degeneration differs between patients with nr-axSpA and established AS. Semi-quantitative grading is reliable, and fatty degeneration of paravertebral muscles seems to be related to chronicity and spinal functions in patients with nr-axSpA and AS.

Similar content being viewed by others
References
Rudwaleit M, van der Heijde D, Landewe R, Listing J, Akkoc N, Brandt J, et al. The development of assessment of spondyloarthritis international Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis. 2009;68:777–83.
Cooper RG, Freemont AJ, Fitzmaurice R, Alani SM, Jayson MI. Paraspinal muscle fibrosis: a specific pathological component in ankylosing spondylitis. Ann Rheum Dis. 1991;50:755–9.
Braun J, van den Berg R, Baraliakos X, Boehm H, Burgos-Vargas R, Collantes-Estevez E, et al. 2010 update of the ASAS/EULAR recommendations for the management of ankylosing spondylitis. Ann Rheum Dis. 2011;70:896–904.
Hopkins GO, McDougall J, Mills KR, Isenberg DA, Ebringer A. Muscle changes in ankylosing spondylitis. Br J Rheumatol. 1983;22:151–7.
Berman L, Isaacs H, Pickering A. Structural abnormalities of muscle tissue in ankylosing spondylitis. S Afr Med J. 1976;50:1238–40.
Pohl W, Sievers BU. Muscular changes in ankylosing spondylitis. Z Rheumatol. 1974;33:249–53.
Gordon TP, Sage MR, Bertouch JV, Brooks PM. Computed tomography of paraspinal musculature in ankylosing spondylitis. J Rheumatol. 1984;11:794–7.
Hides JA, Richardson CA, Jull GA. Magnetic resonance imaging and ultrasonography of the lumbar multifidus muscle. Comparison of two different modalities. Spine (Phila Pa 1976) 1995;20:54–8.
Cooper RG, St Clair Forbes W, Jayson MI. Radiographic demonstration of paraspinal muscle wasting in patients with chronic low back pain. Br J Rheumatol 1992;31:389–94.
Danneels LA, Vanderstraeten GG, Cambier DC, Witvrouw EE, De Cuyper HJ. CT imaging of trunk muscles in chronic low back pain patients and healthy control subjects. Eur Spine J. 2000;9:266–72.
Parkkola R, Rytokoski U, Kormano M. Magnetic resonance imaging of the discs and trunk muscles in patients with chronic low back pain and healthy control subjects. Spine (Phila Pa 1976) 1993;18:830–6.
Muche B, Bollow M, Francois RJ, Sieper J, Hamm B, Braun J. Anatomic structures involved in early- and late-stage sacroiliitis in spondylarthritis: a detailed analysis by contrast-enhanced magnetic resonance imaging. Arthritis Rheum. 2003;48:1374–84.
van der Linden S, Valkenburg HA, Cats A. Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum. 1984;27:361–8.
Sahin N, Ozcan E, Baskent A, Karan A, Kasikcioglu E. Muscular kinetics and fatigue evaluation of knee using by isokinetic dynamometer in patients with ankylosing spondylitis. Acta Reumatol Port. 2011;36:252–9.
Hagberg M, Hagner IM, Bjelle A. Shoulder muscle strength, endurance and electromyographic fatigue in ankylosing spondylitis. Scand J Rheumatol. 1987;16:161–5.
Faus-Riera S, Martinez-Pardo S, Blanch-Rubio J, Benito-Ruiz P, Duro-Pujol JC, Corominas-Torres JM. Muscle pathology in ankylosing spondylitis: clinical, enzymatic, electromyographic and histologic correlation. J Rheumatol. 1991;18:1368–71.
Khedr EM, Rashad SM, Hamed SA, El-Zharaa F, Abdalla AK. Neurological complications of ankylosing spondylitis: neurophysiological assessment. Rheumatol Int. 2009;29:1031–40.
Kjaer P, Bendix T, Sorensen JS, Korsholm L, Leboeuf-Yde C. Are MRI-defined fat infiltrations in the multifidus muscles associated with low back pain? BMC Med. 2007;5:2.
Lee JC, Cha JG, Kim Y, Kim YI, Shin BJ. Quantitative analysis of back muscle degeneration in the patients with the degenerative lumbar flat back using a digital image analysis: comparison with the normal controls. Spine (Phila Pa 1976) 2008;33:318–25.
Ozgocmen S, Akgul O, Altay Z, Altindag O, Baysal O, Calis M, et al. Expert opinion and key recommendations for the physical therapy and rehabilitation of patients with ankylosing spondylitis. Int J Rheum Dis. 2012;15(3):229–38.
Erkintalo MO, Salminen JJ, Alanen AM, Paajanen HE, Kormano MJ. Development of degenerative changes in the lumbar intervertebral disk: results of a prospective MR imaging study in adolescents with and without low-back pain. Radiology. 1995;196:529–33.
Mooney V, Gulick J, Perlman M, Levy D, Pozos R, Leggett S, et al. Relationships between myoelectric activity, strength, and MRI of lumbar extensor muscles in back pain patients and normal subjects. J Spinal Disord. 1997;10:348–56.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Akgul, O., Gulkesen, A., Akgol, G. et al. MR-defined fat infiltration of the lumbar paravertebral muscles differs between non-radiographic axial spondyloarthritis and established ankylosing spondylitis. Mod Rheumatol 23, 811–816 (2013). https://doi.org/10.1007/s10165-012-0750-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10165-012-0750-6