Abstract
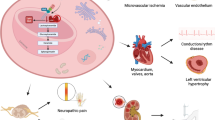
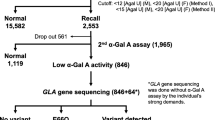
The prevalence rate for Fabry disease is conventionally considered to be 1 case in 40,000; however, due to increased screening accuracy, reports now suggest that prevalence is 1 case in 1,500 among male children, and it is likely that the clinical importance of the condition will increase in the future. In dialysis patients to date, prevalence rates are between 0.16 and 1.2 %. Globotriaosylsphingosine (Lyso-GL-3), which is a substrate of α-galactosidase A (α-Gal A), has surfaced as a new biomarker, and is also effective in the determination and monitoring of the effects of enzyme replacement therapy. In terms of genetic abnormalities, the E66Q mutation has recently become a topic of discussion, and although doubts have been expressed over whether or not it is the gene responsible for Fabry disease, there is still a strong possibility that it is a functional genetic polymorphism. At present, the standard treatment for Fabry disease is enzyme replacement therapy, and in order to overcome the problems involved with this, a method of producing recombinant human α-Gal A using methanol-assimilating yeast, and chemical or medicinal chaperone treatment are of current interest. Migalastat hydrochloride is known as a pharmacological chaperone, but is currently in Phase III global clinical trials. Adding saposin B to modified α-N-acetyl galactosaminidase is also under consideration as a treatment method.

Similar content being viewed by others
References
Doi K, Noiri E, Ishizu T, Negishi K, Suzuki Y, Hamasaki Y, et al. High-throughput screening identified disease-causing mutants and functional variants of α-galactosidase A gene in Japanese male hemodialysis patients. J Hum Genet. 2012;57:575–9.
Spada M, Pagliardini S, Yasuda M, Tukel T, Thiagarajan G, Sakuraba H, et al. High incidence of later-onset fabry disease revealed by newborn screening. Am J Hum Genet. 2006;79(1):31–40.
Hwu WL, Chien YH, Lee NC, Chiang SC, Dobrovolny R, Huang AC, et al. Newborn screening for Fabry disease in Taiwan reveals a high incidence of the later-onset GLA mutation c.936 + 919G > A (IVS4 + 919G > A). Hum Mutat. 2009;30(10):1397–405.
The state of chronic dialysis therapy in Japan (as of 31st December 2010). J Jpn Soc Dial Ther 2012;45:1–47.
Auray-Blais C, Ntwari A, Clarke JT, Warnock DG, Oliveira JP, Young SP, et al. How well does urinary lyso-Gb3 function as a biomarker in Fabry disease? Clin Chim Acta. 2010;411(23–24):1906–14.
Togawa T, Kodama T, Suzuki T, Sugawara K, Tsukimura T, Ohashi T, et al. Plasma globotriaosylsphingosine as a biomarker of Fabry disease. Mol Genet Metab. 2010;100(3):257–61.
Kobayashi M, Ohashi T, Fukuda T, Yanagisawa T, Inomata T, Nagaoka T, et al. No accumulation of globotriaosylceramide in the heart of a patient with the E66Q mutation in the α-galactosidase A gene. Mol Genet Metab. 2012;107:711–5.
Takenaka T, Murray GJ, Qin G, Quirk JM, Ohshima T, Qasba P, et al. Long-term enzyme correction and lipid reduction in multiple organs of primary and secondary transplanted Fabry mice receiving transduced bone marrow cells. Proc Natl Acad Sci USA. 2000;97(13):7515–20.
Jung SC, Han IP, Limaye A, Xu R, Gelderman MP, Zerfas P, et al. Adeno-associated viral vector-mediated gene transfer results in long-term enzymatic and functional correction in multiple organs of Fabry mice. Proc Natl Acad Sci USA. 2001;98(5):2676–81.
Eng CM, Guffon N, Wilcox WR, Germain DP, Lee P, Waldek S, et al. International collaborative Fabry disease study group. Safety and efficacy of recombinant human alpha-galactosidase A–replacement therapy in Fabry’s disease. N Engl J Med. 2001;345(1):9–16.
Schiffmann R, Kopp JB, Austin HA 3rd, Sabnis S, Moore DF, Weibel T, et al. Enzyme replacement therapy in Fabry disease: a randomized controlled trial. JAMA. 2001;285(21):2743–9.
Tsukimura T, Kawashima I, Togawa T, Kodama T, Suzuki T, Watanabe T, et al. Efficient uptake of recombinant α-galactosidase A produced with a gene-manipulated yeast by Fabry mice kidneys. Mol Med. 2012;10(18):76–82.
Tsukimura T, Chiba Y, Ohno K, Saito S, Tajima Y, Sakuraba H. Molecular mechanism for stabilization of a mutant α-galactosidase A involving M51I amino acid substitution by imino sugars. Mol Genet Metab. 2011;103(1):26–32.
Tajima Y, Kawashima I, Tsukimura T, Sugawara K, Kuroda M, Suzuki T, et al. Use of a modified alpha-N-acetylgalactosaminidase in the development of enzyme replacement therapy for Fabry disease. Am J Hum Genet. 2009;85(5):569–80.
Acknowledgments
We received a research fund of Japan Kidney Foundation. We really appreciate Ms Aiko Ooashi for her secretarial assistance in conducting J-FAST and preparing this manuscript.
Conflict of interest
The authors have declared that no Conflict of interest exists.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kusano, E., Saito, O., Akimoto, T. et al. Fabry disease: experience of screening dialysis patients for Fabry disease. Clin Exp Nephrol 18, 269–273 (2014). https://doi.org/10.1007/s10157-013-0897-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-013-0897-2