Abstract
Background
In adult-onset minimal-change disease (MCD) the predictors of remission and relapse of proteinuria and corticosteroid-related adverse events remain unknown.
Methods
The multicenter retrospective cohort study, the STudy of Outcomes and Practice patterns of Minimal-Change Disease (STOP-MCD), included 142 adult-onset MCD patients in 5 nephrology centers in Japan. Primary outcomes were first remission of proteinuria defined by urinary protein (UP) <0.3 g/day, UP/creatinine ratio (UPCR) <0.3, and/or negative/trace by dipstick test and first relapse of proteinuria defined by UP ≥1.0 g/day, UPCR ≥1.0, and/or dipstick test ≥1+ followed by immunosuppressive therapy. Secondary outcomes were corticosteroid-related adverse events.
Results
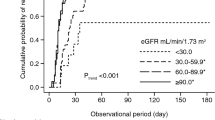
During the median 3.6 (interquartile range, 2.0–6.9) years of the entire observational period, 136 (95.8 %) and 79 (58.1 %) patients developed at least 1 remission and 1 recurrence within a median of 15 (10–34) days and 0.90 (0.55–1.57) years, respectively. Compared with younger patients aged 15–29 years at kidney biopsy, elderly patients aged ≥60 years developed remission significantly later [hazard ratio 0.53 (95 % confidence interval 0.32–0.88)], while older patients aged ≥45 years were at a significantly lower risk of relapse [45–59 years, 0.46 (0.22–0.96); 60–83 years, 0.39 (0.21–0.74)]. However, older patients were significantly more vulnerable to severe infection, diabetes, and cataract as compared with younger patients.
Conclusion
Younger patients had a higher risk of relapse while older patients had a lower risk of relapse but a higher risk of corticosteroid-related adverse events.


Similar content being viewed by others
References
Fogo A, Horn RG. A 51-year-old woman with nephrotic syndrome, hematuria, and renal insufficiency. Am J Kidney Dis. 1997;29(5):806–10.
Polito MG, de Moura LA, Kirsztajn GM. An overview on frequency of renal biopsy diagnosis in Brazil: clinical and pathological patterns based on 9,617 native kidney biopsies. Nephrol Dial Transplant. 2010;25(2):490–6.
Kazi JI, Mubarak M, Ahmed E, Akhter F, Naqvi SA, Rizvi SA. Spectrum of glomerulonephritides in adults with nephrotic syndrome in Pakistan. Clin Exp Nephrol. 2009;13(1):38–43.
Perera SA, Gregusova A, Bartlett RJ. First calculations of 15N–15NJ values and new calculations of chemical shifts for high nitrogen systems: a comment on the long search for HN5 and its pentazole anion. J Phys Chem A. 2009;113(13):3197–201.
Yokoyama H, Taguchi T, Sugiyama H, Sato H. Membranous nephropathy in Japan: analysis of the Japan Renal Biopsy Registry (J-RBR). Clin Exp Nephrol. 2012;16(4):557–63.
Chang JH, Kim DK, Kim HW, Park SY, Yoo TH, Kim BS, et al. Changing prevalence of glomerular diseases in Korean adults: a review of 20 years of experience. Nephrol Dial Transplant. 2009;24(8):2406–10.
Tennakoon S, Perera B, Haturusinghe L. Intentional poisoning cases of animals with anticholinesterase pesticide-carbofuran in Sri Lanka. Leg Med (Tokyo). 2009;11(Suppl 1):S500–2.
Nolasco F, Cameron JS, Heywood EF, Hicks J, Ogg C, Williams DG. Adult-onset minimal change nephrotic syndrome: a long-term follow-up. Kidney Int. 1986;29(6):1215–23.
Nair RB, Date A, Kirubakaran MG, Shastry JC. Minimal-change nephrotic syndrome in adults treated with alternate-day steroids. Nephron. 1987;47(3):209–10.
Korbet SM, Schwartz MM, Lewis EJ. Minimal-change glomerulopathy of adulthood. Am J Nephrol. 1988;8(4):291–7.
Fujimoto S, Yamamoto Y, Hisanaga S, Morita S, Eto T, Tanaka K. Minimal change nephrotic syndrome in adults: response to corticosteroid therapy and frequency of relapse. Am J Kidney Dis. 1991;17(6):687–92.
Mak SK, Short CD, Mallick NP. Long-term outcome of adult-onset minimal-change nephropathy. Nephrol Dial Transplant. 1996;11(11):2192–201.
Huang JJ, Hsu SC, Chen FF, Sung JM, Tseng CC, Wang MC. Adult-onset minimal change disease among Taiwanese: clinical features, therapeutic response, and prognosis. Am J Nephrol. 2001;21(1):28–34.
Nakayama M, Katafuchi R, Yanase T, Ikeda K, Tanaka H, Fujimi S. Steroid responsiveness and frequency of relapse in adult-onset minimal change nephrotic syndrome. Am J Kidney Dis. 2002;39(3):503–12.
Tse KC, Lam MF, Yip PS, Li FK, Choy BY, Lai KN, et al. Idiopathic minimal change nephrotic syndrome in older adults: steroid responsiveness and pattern of relapses. Nephrol Dial Transplant. 2003;18(7):1316–20.
Takei T, Koike M, Suzuki K, Shirota S, Itabashi M, Ohtsubo S, et al. The characteristics of relapse in adult-onset minimal-change nephrotic syndrome. Clin Exp Nephrol. 2007;11(3):214–7.
Waldman M, Crew RJ, Valeri A, Busch J, Stokes B, Markowitz G, et al. Adult minimal-change disease: clinical characteristics, treatment, and outcomes. Clin J Am Soc Nephrol. 2007;2(3):445–53.
Fukudome K, Fujimoto S, Sato Y, Kitamura K. Comparison of the effects of intravenous methylprednisolone pulse versus oral prednisolone therapies on the first attack of minimal-change nephrotic syndrome in adults. Nephrology. 2012;17(3):263–8.
Chou YH, Lien YC, Hu FC, Lin WC, Kao CC, Lai CF, et al. Clinical outcomes and predictors for ESRD and mortality in primary GN. Clin J Am Soc Nephrol. 2012;7(9):1401–8.
Toruner M, Loftus EV Jr, Harmsen WS, Zinsmeister AR, Orenstein R, Sandborn WJ, et al. Risk factors for opportunistic infections in patients with inflammatory bowel disease. Gastroenterology. 2008;134(4):929–36.
Crowson CS, Hoganson DD, Fitz-Gibbon PD, Matteson EL. Development and validation of a risk score for serious infection in patients with rheumatoid arthritis. Arthritis Rheum. 2012;64(9):2847–55.
Albert K, Sennesael J, Haentjens P. Incidence and risk factors for posttransplant subcapsular cataract: a long-term retrospective cohort study. Transplant Proc. 2011;43(9):3465–9.
Uzu T, Harada T, Sakaguchi M, Kanasaki M, Isshiki K, Araki S, et al. Glucocorticoid-induced diabetes mellitus: prevalence and risk factors in primary renal diseases. Nephron Clin Pract. 2007;105(2):c54–7.
Ha Y, Lee KH, Jung S, Lee SW, Lee SK, Park YB. Glucocorticoid-induced diabetes mellitus in patients with systemic lupus erythematosus treated with high-dose glucocorticoid therapy. Lupus. 2011;20(10):1027–34.
Kim SY, Yoo CG, Lee CT, Chung HS, Kim YW, Han SK, et al. Incidence and risk factors of steroid-induced diabetes in patients with respiratory disease. J Korean Med Sci. 2011;26(2):264–7.
Nakamura J, Saisu T, Yamashita K, Suzuki C, Kamegaya M, Takahashi K. Age at time of corticosteroid administration is a risk factor for osteonecrosis in pediatric patients with systemic lupus erythematosus: a prospective magnetic resonance imaging study. Arthritis Rheum. 2010;62(2):609–15.
Shigemura T, Nakamura J, Kishida S, Harada Y, Ohtori S, Kamikawa K, et al. Incidence of osteonecrosis associated with corticosteroid therapy among different underlying diseases: prospective MRI study. Rheumatology. 2011;50(11):2023–8.
Schimmer BP, Parker KL. Adrenocorticotropic hormone; adrenocortical steroids and their synthetic analogs; inhibitors of the synthesis and actions of adrenocortical hormones. Goodman & Gilman’s the pharmacological basis of therapeutics. 9th ed. New York: McGraw-Hill; 1996. p. 1459–85.
Donohoue P, Kappy M, Allen D, Geffner M. The adrenal gland and its disorders. In: Principles and practice of pediatric endocrinology; Springfield: Charles Thomas, 2005. p. 403.
The primary nephrotic syndrome in children. Identification of patients with minimal change nephrotic syndrome from initial response to prednisone. A report of the International Study of Kidney Disease in Children. J Pediatr. 1981;98(4):561–4.
Acknowledgments
The authors thank Kakuya Niihiata, M.D., for data management.
Conflict of interest
The authors have no potential conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Shinzawa, M., Yamamoto, R., Nagasawa, Y. et al. Age and prediction of remission and relapse of proteinuria and corticosteroid-related adverse events in adult-onset minimal-change disease: a retrospective cohort study. Clin Exp Nephrol 17, 839–847 (2013). https://doi.org/10.1007/s10157-013-0793-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-013-0793-9