Abstract
Background
The benefit of adding oral antibiotic prophylaxis (OA) to intravenous prophylaxis (IV) in elective colorectal surgery to prevent surgical site infection (SSI) and whether the benefit of OA requires a mechanical bowel cleansing (MBP) are assessed in a systematic review. Meta-analyses compare randomized trials of IV versus IV plus OA, both with MBP; OA versus IV plus OA, both again with MBP; OA plus IV in studies randomizing patients to MBP or no MBP; and IV versus IV plus OA in patients with no MBP.
Methods
MEDLINE, EMBASE, and the Cochrane Library were searched for eligible studies from 1965 to April 1, 2020. The outcome assessed was SSI, superficial and deep, but not organ space. For each included study, risk of bias was assessed using the Cochrane Risk of Bias tool version 1. For each comparison, meta-analysis was performed from data from eligible studies to obtain a summary effect and heterogeneity using RevMan. Sensitivity analyses were performed excluding studies of poor quality. Certainty of evidence was assessed using GRADE for each comparison.
Results
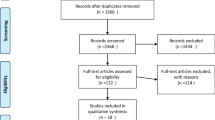
Sixty-one studies published in 1971–2020 from 55 publications reporting 12,297 patients were eligible for inclusion. A total of 36 studies compared IV to OA plus IV with MBP. The risk ratio (RR) and 95% confidence interval (CI) for SSI with oral and IV vs. IV alone are 0.47, 0.40–0.56. The RR in 19 studies for IV plus OA versus OA alone is 0.48, 0.38–0.62. The RR for OA plus IV with MBP versus without MBP in 5 studies is 1.17, 0.84–1.64. The RR for OA plus IV versus IV alone when no bowel prep was used in two studies is 0.36, 0.18–0.72. RRs were similar in sensitivity analyses. The GRADE is high for the first two comparisons, moderate for the 3rd, and low for the 4th due to imprecision and heterogeneity.
Conclusions
Combined OA and IV is superior to either alone in preventing SSI. The certainty of evidence is such that further research is unlikely to alter this relationship when MBP is used. In randomized trials of MBP, OA plus IV shows no benefit from MBP versus no MBP. The last comparison shows in just two studies that as in the first meta-analysis, but in the absence of MBP, combined OA plus IV is also superior to IV alone.







Similar content being viewed by others
References
Dellinger EP (2018) When will the surgical community acknowledge the evidence regarding prophylaxis with oral antibiotics for scheduled colorectal operations? JAMA Netw Open 1(6):e183257. https://doi.org/10.1001/jamanetworkopen.2018.3257(PubMed PMID: 30646230)
Basson MD (2018) Oral antibiotics for colon surgery: the questions remain the same, as do the answers. JAMA Surg 153(2):121–122. https://doi.org/10.1001/jamasurg.2017.3843(PubMed PMID: 29049520)
Garfinkle R, Abou-Khalil J, Morin N, Ghitulescu G, Vasilevsky CA, Gordon P, Demian M, Boutros M (2017) Is There a Role For Oral Antibiotic Preparation Alone Before Colorectal Surgery? ACS-NSQIP analysis by coarsened exact matching. Dis Colon Rectum 60(7):729–737
Slim K, Kartheuser A (2018) Mechanical bowel preparation before colorectal surgery in enhanced recovery programs: discrepancy between the American and European guidelines. Dis Colon Rectum 61(2):e13–e14. https://doi.org/10.1097/DCR.0000000000000992(PubMed PMID: 29337786)
Rollins KE, Javanmard-Emamghissi H, Lobo DN (2018) Impact of mechanical bowel preparation in elective colorectal surgery: a meta-analysis. World J Gastroenterol 24(4):519–536
Vignaud M, Paugam-Burtz C, Garot M, Jaber S, Slim K, Panis Y, Lucet JC, Bourdier J, Morand D, Pereira B, Futier E, COMBINE trial management committee (2018) COMBINE trial management committee. Comparison of intravenous versus combined oral and intravenous antimicrobial prophylaxis (COMBINE) for the prevention of surgical site infection in elective colorectal surgery: study protocol for a multicentre, double-blind, randomised controlled clinical trial. BMJ Open 8(4):e020254
Mulder T, Kluytmans-van den Bergh MFQ, de Smet AMGA, van ‘t Veer NE, Roos D, Nikolakopoulos S, Bonten MJM, Kluytmans JAJW, PreCaution Study Group (2018) Prevention of severe infectious complications after colorectal surgery using preoperative orally administered antibiotic prophylaxis (PreCaution): study protocol for a randomized controlled trial. Trials 19(1):51
Higgins JPT, Green S (eds) (2011) Cochrane handbook for systematic reviews of interventions version 5.1.0 [updated March 2011]. The Cochrane Collaboration. Available from https://handbook.cochrane.org
Armijo-Olivo S, Warren M (2009) Intention to treat, compliance, drop outs and how to deal with missing data in clinical research: a review. Phys Therapy Rev 14(1):36–49
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, Norris S, Falck-Ytter Y, Glasziou P, DeBeer H, Jaeschke R, Rind D, Meerpohl J, Dahm P, Schünemann HJ (2011) GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 64(4):383–394
GRADE handbook. https://gdt.guidelinedevelopment.org/central_prod/_design/client/handbook/handbook.html
Guyatt GH, Oxman AD, Kunz R, Woodcock J, Brozek J, Helfand M, Alonso-Coello P, Glasziou P, Jaeschke R, Akl EA, Norris S, Vist G, Dahm P, Shukla VK, Higgins J, Falck-Ytter Y, Schünemann HJ, GRADE Working Group (2011) GRADE guidelines: 7. Rating the quality of evidence—inconsistency. J Clin Epidemiol. 64(12):1294–1302
Guyatt GH, Oxman AD, Kunz R, Brozek J, Alonso-Coello P, Rind D, Devereaux PJ, Montori VM, Freyschuss B, Vist G, Jaeschke R, Williams JW Jr, Murad MH, Sinclair D, Falck-Ytter Y, Meerpohl J, Whittington C, Thorlund K, Andrews J, Schünemann HJ (2011) GRADE guidelines 6. Rating the quality of evidence–imprecision. J Clin Epidemiol. 64(12):1283–1293
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. BMJ 339:b2700
Included studies
Abis GSA, Stockmann HBAC, Bonjer HJ, van Veenendaal N, van Doorn-Schepens MLM, Budding AE et al (2019) Randomized clinical trial of selective decontamination of the digestive tract in elective colorectal cancer surgery (SELECT trial). Br J Surg 106(4):355–363
Moral A, Aracil XS, Juncá JB, López LM, Tavira RH, Garnica IA, Rodríguez OA, Soto SN (2009) A prospective, randomised, controlled study on the need to mechanically prepare the colon in scheduled colorectal surgery. Cir Esp. 85(1):20–25
Ammann J, Blessing H, Marti WK (1981) Antibiotic prophylaxis in elective colon surgery: comparison of the combination of metronidazole (Flagyl)/cefazolin (Kefzol) with cefazolin alone [Antibiotikaprophylaxe in der elektiven Kolonchirurgie: Vergleich der Kombination Metronidazol (Flagyl)/Cefazolin (Kefzol) mit Cefazolin allein]. Helvetica Chirurgica Acta 48(1–2):235–242
Anjum N, Ren J, Wang G, Li G, Wu X, Dong H et al (2017) A randomized control trial of preoperative oral antibiotics as adjunct therapy to systemic antibiotics for preventing surgical site infection in clean contaminated, contaminated, and dirty type of colorectal surgeries. Dis Colon Rectum 60(12):1291–1298
Cuthbertson AM (1983) Clinical trial of prophylaxis of wound sepsis in elective colorectal surgery. Cephamandole with tinidazole versus tinidazole alone. Med J Aust 2(9):440–443
Barber MS, Hirschberg BC, Rice CL, Atkins CC (1979) Parenteral antibiotics in elective colon surgery? A prospective, controlled clinical study. Surgery 86(1):23–29
Barker K, Graham NG, Mason MC, De Dombal FT, Goligher JC (1971) The relative significance of preoperative oral antibiotics, mechanical bowel preparation, and preoperative peritoneal contamination in the avoidance of sepsis after radical surgery for ulcerative colitis and Crohn's disease of the large bowel. Br J Surg 58(4):270–273
Beggs FD, Jobanputra RS, Holmes JT (1982) A comparison of intravenous and oral metronidazole as prophylactic in colorectal surgery. Br J Surg 69(4):226–227
Cafiero F, Gipponi M, Bonalumi U, Piccardo A, Sguotti C, Corbetta G (1992) Prophylaxis of infection with intravenous immunoglobulins plus antibiotic for patients at risk for sepsis undergoing surgery for colorectal cancer: results of a randomized, multicenter clinical trial. Surgery 112(1):24–31
Coppa GF, Eng K, Gouge TH, Ranson JH, Localio SA (1983) Parenteral and oral antibiotics in elective colon and rectal surgery. A prospective, randomized trial. Am J Surg 145(1):62–65
Condon RE, Bartlett JG, Greenlee H, Schulte WJ, Ochi S, Abbe R et al (1983) Efficacy of oral and systemic antibiotic prophylaxis in colorectal operations. Arch Surg (Chicago, Ill: 1960) 118(4):496–502
Dion YM, Richards GK, Prentis JJ, Hinchey EJ (1980) The influence of oral versus parenteral preoperative metronidazole on sepsis following colon surgery. Ann Surg 192(2):221–226
Espin-Basany E, Sanchez-Garcia JL, Lopez-Cano M, Lozoya-Trujillo R, Medarde-Ferrer M, Armadans-Gil L et al (2005) Prospective, randomised study on antibiotic prophylaxis in colorectal surgery. Is it really necessary to use oral antibiotics? Int J Colorectal Dis 20(6):542–546
Eloy Espin-Basani, Solis-Pena A (2020) Preoperative oral antibiotics and surgical site infection in colon surgery without mechanical bowel prep. A prospective, multicenter single blinded, randomized trial (ORALEV study). Lancet 5:729–738
Favre JP, Bouchet Y, Clotteau JE, Hypousteguy L, Marchal G, Mercier R et al (1984) Prophylactic use of cefotaxime in colonic and rectal surgery. J Antimicrob Chemother 14(Suppl B):247–253
Goto S, Hasegawa S, Hata H, Yamaguchi T, Hida K, Nishitai R et al (2016) Differences in surgical site infection between laparoscopic colon and rectal surgeries: sub-analysis of a multicenter randomized controlled trial (Japan-Multinational Trial Organization PREV 07–01). Int J Colorectal Dis 31(11):1775–1784
Gruttadauria G, La Barbera F, Cutaia G, Salanitri G (1987) Prevention of infection in colonic surgery by rifaximin. A controlled, prospective, randomized trial. Rivista europea per le scienze mediche e farmacologiche European review for medical and pharmacological sciences Revue Europeenne pour les Sciences Medicales et Pharmacologiques 9(1):101–105
Hanel KC, King DW, McAllister ET, Reiss-Levy E (1980) Single-dose parenteral antibiotics as prophylaxis against wound infections in colonic operations. Dis Colon Rectum 23(2):98–101
Ikeda A, Konishi T, Ueno M, Fukunaga Y, Nagayama S, Fujimoto Y et al (2016) Randomized clinical trial of oral and intravenous versus intravenous antibiotic prophylaxis for laparoscopic colorectal resection. Br J Surg 103(12):1608–1615
Ishida H, Yokoyama M, Nakada H, Inokuma S, Hashimoto D (2001) Impact of oral antimicrobial prophylaxis on surgical site infection and methicillin-resistant Staphylococcus aureus infection after elective colorectal surgery. Results of a prospective randomized trial. Surg Today 31(11):979–983
Jagelman DG, Fazio VW, Lavery IC, Weakley FL (1985) A prospective, randomized, double-blind study of 10% mannitol mechanical bowel preparation combined with oral neomycin and short-term, perioperative, intravenous Flagyl as prophylaxis in elective colorectal resections. Surgery 98(5):861–865
Jung B, Påhlman L, Nyström PO, Nilsson E, Mechanical Bowel Preparation Study Group (2007) Multicentre randomized clinical trial of mechanical bowel preparation in elective colonic resection. Br J Surg. 94(6):689–695
Kaiser AB, Herrington JL Jr, Jacobs JK, Mulherin JL Jr, Roach AC, Sawyers JL (1983) Cefoxitin versus erythromycin, neomycin, and cefazolin in colorectal operations. Importance of the duration of the surgical procedure. Ann Surg 198(4):525–530
Kobayashi M, Mohri Y, Tonouchi H, Miki C, Nakai K, Kusunoki M (2007) Randomized clinical trial comparing intravenous antimicrobial prophylaxis alone with oral and intravenous antimicrobial prophylaxis for the prevention of a surgical site infection in colorectal cancer surgery. Surg Today 37(5):383–388
Koskenvuo L, Lehtonen T, Koskensalo S, Rasilainen S, Klintrup K, Ehrlich A et al (2019) Mechanical and oral antibiotic bowel preparation versus no bowel preparation for elective colectomy (MOBILE): a multicentre, randomised, parallel, single-blinded trial. Lancet (London, England) 394(10201):840–848
Khubchandani IT, Karamchandani MC, Sheets JA, Stasik JJ, Rosen L, Riether RD (1989) Metronidazole vs. erythromycin, neomycin, and cefazolin in prophylaxis for colonic surgery. Dis Colon Rectum 32(1):17–20
Lazorthes F, Legrand G, Monrozies X, Fretigny E, Pugnet G, Cordova JA et al (1982) Comparison between oral and systemic antibiotics and their combined use for the prevention of complications in colorectal surgery. Dis Colon Rectum 25(4):309–311
Lau WY, Chu KW, Poon GP, Ho KK (1988) Prophylactic antibiotics in elective colorectal surgery. Br J Surg 75(8):782–785
Lewis RT (1990s) Oral versus systemic antibiotic prophylaxis in elective colon surgery: a randomized study and meta-analysis send a message from the 1990s. Can J Surg J Can Chir 45(3):173–180
McArdle CS, Morran CG, Pettit L, Gemmell CG, Sleigh JD, Tillotson GS (1995) Value of oral antibiotic prophylaxis in colorectal surgery. Br J Surg 82(8):1046–1048
McDermott FT, Polglase AL, Johnson WR, Hughes ES (1981) Prevention of wound infection in elective colorectal resections by preoperative cephazolin with and without metronidazole. Aust NZ J Surg 51(4):351–353
Mehigan D, Zuidema GD, Cameron JL (1981) The role of systemic antibiotics in operations upon the colon. Surg Gynecol Obstet 153(4):573–576
Mihara (2015) 下部消化管待機手術における化学的腸管処置の有用性に関する検討. J Jpn Soc Ext Relat 76(8):1825–1830
Moen OO, Tveter KJ (1980) The value of the prophylactic use of doxycycline and tinidazole in elective colorectal surgery. Scand J Gastroenterol Suppl 59:17–20 (PubMed PMID: 6988946)
Monrozies X, Lazorthes F, Fretigny E, Chiotasso P, Massip P (1983) Evaluation of systemic antibiotic preventive treatment in colorectal surgery [Appreciation de l'antibio-prophylaxie systemique en chirurgie colo-rectale]. J Chir 120(6–7):393–396
Mulder T Prevention of severe infectious complications after colorectal surgery. PhD thesis, Utrecht University, The Netherlands. https://dspace.library.uu.nl/handle/1874/383687
Nohr M (1990) Prophylactic single dose fosfomycin and Met with Neo, Bac, Met and amp in elective colorectal operations. Act Chir Scand 156(3):223–230
Oshima T, Takesue Y, Ikeuchi H, Matsuoka H, Nakajima K, Uchino M et al (2013) Preoperative oral antibiotics and intravenous antimicrobial prophylaxis reduce the incidence of surgical site infections in patients with ulcerative colitis undergoing IPAA. Dis Colon Rectum 56(10):1149–1155
Peruzzo L, Savio S, De Lalla F (1987) Systemic versus systemic plus oral chemoprophylaxis in elective colorectal surgery. Chemioterapia Int J Mediterr Soc Chemother 6(2 Suppl):601–603
Petrelli NJ, Conte CC, Herrera L, Stulc J, O'Neill P (1988) A prospective, randomized trial of perioperative prophylactic cefamandole in elective colorectal surgery for malignancy. Dis Colon Rectum 31(6):427–429
Playforth MJ, Smith GM, Evans M, Pollock AV (1988) Antimicrobial bowel preparation. Oral, parenteral, or both? Dis Colon Rectum 31(2):90–93
Portnoy J, Kagan E, Gordon PH, Mendelson J (1983) Prophylactic antibiotics in elective colorectal surgery. Dis Colon Rectum 26(5):310–313
Reynolds JR, Jones JA, Hardcastle JD (1989) Do preoperative oral antibiotics influence sepsis rates. Surg Res Commun 7:71–77
Reddy BS (2007) Randomized clinical trial of effect of synbiotics, neomycin and mechanical bowel prep on intestinal barrier function in patients undergoing colectomy. Br J Surg 94:546–554
Sadahiro S, Suzuki T, Tanaka A, Okada K, Kamata H, Ozaki T et al (2014) Comparison between oral antibiotics and probiotics as bowel preparation for elective colon cancer surgery to prevent infection: prospective randomized trial. Surgery 155(3):493–503
Schoetz DJ Jr, Roberts PL, Murray JJ, Coller JA, Veidenheimer MC (1990) Addition of parenteral cefoxitin to regimen of oral antibiotics for elective colorectal operations. A randomized prospective study. Ann Surg 212(2):209–212
Stellato TA, Danziger LH, Gordon N, Hau T, Hull CC, Zollinger RM Jr et al (1990) Antibiotics in elective colon surgery. A randomized trial of oral, systemic, and oral/systemic antibiotics for prophylaxis. Am Surg 56(4):251–254
Suzuki T, Sadahiro S, Tanaka A, Okada K, Saito G, Miyakita H, Ogimi T (2019) Usefulness of preoperative mechanical bowel preparation in patients with colon cancer who undergo elective surgery: a prospective randomized trial using oral antibiotics. Dig Surg. 3:1–7
Takesue A (2000) Brief Course Of Colon Preparation With Oral Antibiotics. Surg Today 30:112–116
Takesue (2009) Bowel preparation with antibiotics for the surgery in patients with ulcerative colitis (UC) and colorectal cancer (CRC); prospective randomized study. Surg Infect 10(2):223–224
Taylor EW, Lindsay G (1994) Selective decontamination of the colon before elective colorectal surgery. West of Scotland Surgical Infection Study Group. World J Surg 18(6):926–931 (discussion 931–932)
Uchino M, Ikeuchi H, Bando T, Chohno T, Sasaki H, Horio Y et al (2019) Efficacy of preoperative oral antibiotic prophylaxis for the prevention of surgical site infections in patients with Crohn disease: a randomized controlled trial. Ann Surg 269(3):420–426
Viddal KO, Semb LS (1980) Tinidazole and doxycycline compared to doxycycline alone as prophylactic antimicrobial agents in elective colorectal surgery. Scand J Gastroenterol Suppl 59:21–24
Yabata (1997) Comparison of oral, systemic and intraluminal preparations. J Med Dent Sci 44(4):75–80
Zmora (2003) Colon and rectal surgery without mechanical bowel preparation. Ann Surg 237(3):363
Discussion references
Nelson RL, Gladman E, Barbateskovic M (2014) Antimicrobial prophylaxis for colorectal surgery. Cochrane Database Syst Rev (5):CD001181
Koullouros M, Khan N, Aly EH (2017) The role of oral antibiotics prophylaxis in prevention of surgical site infection in colorectal surgery. Int J Colorectal Dis. 32(1):1–18 (Review. PubMed PMID: 27778060)
Moustgaard H, Clayton GL, Jones HE, Boutron I, Jørgensen L, Laursen DRT, Olsen MF, Paludan-Müller A, Ravaud P, Savović J, Sterne JAC, Higgins JPT, Hróbjartsson A (2020) Impact of blinding on estimated treatment effects in randomised clinical trials: meta-epidemiological study. BMJ 21(368):l6802
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guidelines for prevention of surgical site infection. Infect Control Hosp Epidemiol 20:247–278
Guglielmo BJ, Hohn DC, Koo PJ, Hunt TK, Sweet RL, Conte JE Jr (1983) Antibiotic prophylaxis in surgical procedures. A critical analysis of the literature. Arch Surg 118(8):943–955 (Review)
Galandiuk S, Polk HC Jr, Jagelman DG, Fazio VW (1989) Re-emphasis of priorities in surgical antibiotic prophylaxis. Surg Gynecol Obstet 169(3):219–222
Bellows CF, Mills KT, Kelly TN, Gagliardi G (2011) Combination of oral non-absorbable and intravenous antibiotics versus intravenous antibiotics alone in the prevention of surgical site infections after colorectal surgery: a meta-analysis of randomized controlled trials. Tech Coloproctol 15(4):385–395
Chen M, Song X, Chen LZ, Lin ZD, Zhang XL (2016) Comparing mechanical bowel preparation with both oral and systemic antibiotics versus mechanical bowel preparation and systemic antibiotics alone for the prevention of surgical site infection after elective colorectal surgery: a meta-analysis of randomized controlled clinical trials. Dis Colon Rectum 59(1):70–78
Toh JWT, Phan K, Hitos K, Pathma-Nathan N, El-Khoury T, Richardson AJ, Morgan G, Engel A, Ctercteko G (2018) Association of mechanical bowel preparation and oral antibiotics before elective colorectal surgery with surgical site infection: a network meta-analysis. JAMA Netw Open 1(6):e183226
Rollins KE, Javanmard-Emamghissi H, Acheson AG, Lobo DN (2019) The role of oral antibiotic preparation in elective colorectal surgery: a meta-analysis. Ann Surg 270(1):43–58
McSorley ST, Steele CW, McMahon AJ (2019) Authors' reply: Meta-analysis of oral antibiotics, in combination with preoperative intravenous antibiotics and mechanical bowel preparation the day before surgery, compared with intravenous antibiotics and mechanical bowel preparation alone to reduce surgical-site infections in elective colorectal surgery (BJS Open 2018; 2: 185–194). BJS Open 3(6):883–884
Nygren J, Thacker J, Carli F, Enhanced Recovery After Surgery (ERAS) Society, for Perioperative Care, European Society for Clinical Nutrition, and Metabolism (ESPEN), International Association for Surgical Metabolism, and Nutrition (IASMEN) et al (2013) Guidelines for perioperative care in elective rectal/pelvic surgery: enhanced recovery after surgery (ERAS(®)) Society recommendations. World J Surg. 37:285–305
Güenaga KF, Matos D, Wille-Jørgensen P (2011) Mechanical bowel preparation for elective colorectal surgery. Cochrane Database Syst Rev (9):CD001544
Slim K, Vicaut E, Launay-Savary MV et al (2009) Updated systematic review and meta- analysis of randomized clinical trials on the role of mechanical bowel preparation before colorectal surgery. Ann Surg 249:203–209
Nelson R (2011) Oral non-absorbable antibiotics for colorectal surgery. Tech Coloproctol 15(4):367–368
Nelson RL (2018) Oral antibiotics without a mechanical bowel preparation in colorectal surgery. Dis Colon Rectum 61(9):e362
Badia JM, Arroyo-García N (2018) Mechanical bowel preparation and oral antibiotic prophylaxis in colorectal surgery: analysis of evidence and narrative review. Cir Esp. 96(6):317–325
Mulder T, Kluytmans JAJW (2019) Oral antibiotics prior to colorectal surgery: do they have to be combined with mechanical bowel preparation? Infect Control Hosp Epidemiol 40(8):922–927
Duff SE, Battersby CLF, Davies RJ, Hancock L, Pipe J, Buczacki S, Kinross J, Acheson AG, Walsh CJ (2020) The use of oral antibiotics and mechanical bowel preparation in elective colorectal resection for the reduction of surgical site infection. Colorectal Dis 22(4):364–372
Dahabreh IJ, Steele DW, Shah N, Trikalinos TA (2015) Oral mechanical bowel preparation for colorectal surgery: systematic review and meta-analysis. Dis Colon Rectum 58:698–707
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals by any of the authors.
Informed consent
No participants were identified or contacted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Search strategy
MEDLINE (OVID)
1. exp Surgical Wound Infection/
2. exp Postoperative Complications/
3. exp Bacterial Infections/
4. exp Infection/
5. exp Sepsis/
6. (postoperative complication* or infection* or sepsis).mp.
7. 1 or 2 or 3 or 4 or 5 or 6
8. exp Anti-Infective Agents/
9. exp Anti-Bacterial Agents/
10. (Anti infective or antibiotic* or antimicrobial* or anti bacterial*).mp.
11. exp Colorectal Surgery/
12. exp Colon/
13. exp Rectum/
14. exp Colectomy/
15. exp Colostomy/
16. (colon or rectum or rectal or colorectal or colectomy or colostomy).mp.
17. 8 or 9 or 10
18. 11 or 12 or 13 or 14 or 15 or 16
19. 7 and 17 and 18
20. randomized controlled trial.pt.
21. controlled clinical trial.pt.
22. randomized.ab.
23. placebo.ab.
24. clinical trial.sh.
25. randomly.ab.
26. trial.ti.
27. 20 or 21 or 22 or 23 or 24 or 25 or 26
28. humans.sh.
29. 27 and 28
30. 19 and 29
EMBASE (OVID)
1. exp surgical infection/
2. exp postoperative complication/
3. exp bacterial infection/
4. exp infection/
5. exp sepsis/
6. (postoperative complication* or infection* or sepsis).m_titl.
7. 1 or 2 or 3 or 4 or 5 or 6
8. exp antiinfective agent/
9. exp antibiotic agent/
10. (anti infective or antibiotic* or antimicrobial* or anti bacterial).m_titl.
11. 8 or 9 or 10
12. exp colorectal surgery/
13. exp colon/
14. exp rectum/
15. exp colon resection/
16. exp colostomy/
17. (colon or rectum or rectal or colorectal or colectomy or colostomy).m_titl. 18. 12 or 13 or 14 or 15 or 16 or 17
18. 7 and 11 and 18
19. randomized controlled trial/
20. randomization/
21. controlled study/
22. multicenter study/
23. phase 3 clinical trial/
24. phase 4 clinical trial/
25. double blind procedure/
26. single blind procedure/
27. ((singl* or doubl* or trebl* or tripl*) adj (blind* or mask*)).ti,ab.
28. (random* or cross* over* or factorial* or placebo* or volunteer*).ti,ab. 30. 25 or 22 or 26 or 28 or 21 or 27 or 23 or 20 or 29 or 24
29. "human*".ti,ab.
30. (animal* or nonhuman*).ti,ab.
33. 32 and 31
34. 32 not 33
35. 30 not 34
36. 19 and 35
The Cochrane Library
#1 MeSH descriptor Surgical Wound Infection explode all trees
#2 MeSH descriptor Postoperative Complications explode all trees #3 MeSH descriptor Bacterial Infections explode all trees
#4 MeSH descriptor Infection explode all trees #5 MeSH descriptor Sepsis explode all trees
#6 (postoperative complication* or infection* or sepsis):ti,ab,kw #7 (#1 OR #2 OR #3 OR #4 OR #5 OR #6)
#8 MeSH descriptor Anti-Infective Agents explode all trees #9 MeSH descriptor Anti-Bacterial Agents explode all trees
#10 (anti infective or antibiotic* or antimicrobial* or anti bacterial*):ti,ab,kw #11 (#8 OR #9 OR #10)
#12 MeSH descriptor Colorectal Surgery explode all trees #13 MeSH descriptor Colon explode all trees
#14 MeSH descriptor Rectum explode all trees #15 MeSH descriptor Colectomy explode all trees #16 MeSH descriptor Colostomy explode all trees
#17 (colon or rectum or rectal or colorectal or colectomy or colostomy):ti,ab,kw #18 (#12 OR #13 OR #14 OR #15 OR #16 OR #17)
#19 (#7 AND #11 AND #18)
Rights and permissions
About this article
Cite this article
Nelson, R.L., Hassan, M. & Grant, M.D. Antibiotic prophylaxis in colorectal surgery: are oral, intravenous or both best and is mechanical bowel preparation necessary?. Tech Coloproctol 24, 1233–1246 (2020). https://doi.org/10.1007/s10151-020-02301-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-020-02301-x