Abstract
Background
Diverticulitis is a common complication of diverticular disease of the colon. While complicated diverticulitis often warrants intervention, acute uncomplicated diverticulitis (AUD) is usually managed conservatively. The aim of the present review was to evaluate the efficacy and safety of conservative treatment of AUD without antibiotics compared to standard antibiotic treatment.
Methods
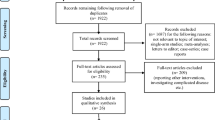
A systematic literature review in compliance with PRISMA guidelines was conducted. Electronic databases including PubMed/Medline, Scopus, Embase and Cochrane central register of controlled trials were searched. Studies that assessed efficacy and safety of treatment of AUD without antibiotics were included. Outcome parameters were rates of treatment failure, recurrence of diverticulitis, complications and mortality, readmission to hospital, and need for surgery.
Results
Nine studies including 2565 patients were included to the review. Of these patients, 65.1% were treated conservatively without antibiotics. Treatment failure was observed in 5.1% of patients not-given-antibiotic treatment versus 3.4% of those given antibiotic treatment. Recurrent diverticulitis occurred in 9.3% of patients in the non-antibiotic group versus 12.1% of patients in the antibiotic group. On meta-analysis of the studies, there were no significant differences between non-antibiotic and antibiotic treatment groups regarding rates of treatment failure (OR = 1.5, p = 0.06), recurrence of diverticulitis (OR = 0.81, p = 0.2), complications (OR = 0.56, p = 0.25), readmission rates (OR = 0.97, p = 0.91), need for surgery (OR = 0.59, p = 0.28), and mortality (OR = 0.64, p = 0.47). The only variable that was significantly associated with treatment failure in the non-antibiotic treatment group was associated comorbidities (standard error (SE) = − 0.07, 95% CI − 0.117 − 0.032; p < 0.001).
Conclusions
Treatment of AUD without antibiotics is feasible, safe, and effective. Adding broad-spectrum antibiotics to the treatment regimen did not serve to decrease treatment failure, recurrence, complications, hospital readmissions, and need for surgery significantly compared to non-antibiotic treatment.





Similar content being viewed by others
References
Elisei W, Brandimarte G, Tursi A (2017 Oct) Management of diverticulosis: what’s new? Minerva Med 108(5):448–463
Shahedi K. Diverticulitis. Medscape [database on the internet]. Available at http://emedicine.medscape.com/article/173388-overview#a1. Accessed online on 5 Sep 2017
Shaikh S, Krukowski ZH (2007) Outcome of a conservative policy for managing acute sigmoid diverticulitis. Br J Surg 94:876–879
Ricciardi R, Baxter NN, Read TE, Marcello PW, Hall J, Roberts PL (2009 Sep) Is the decline in the surgical treatment for diverticulitis associated with an increase in complicated diverticulitis? Dis Colon Rectum 52(9):1558–1563
Sirany AE, Gaertner WB, Madoff RD, Kwaan MR (2017 Jul) Diverticulitis diagnosed in the emergency room: is it safe to discharge home? J Am Coll Surg 225(1):21–25
Jackson JD1, Hammond T (2014 Jul) Systematic review: outpatient management of acute uncomplicated diverticulitis. Int J Colorectal Dis 29(7):775–781. https://doi.org/10.1007/s00384-014-1900-4
[Guideline] World Gastroenterology Organisation (WGO). Practice Guidelines 2007. Diverticular disease. Available at http://www.worldgastroenterology.org/diverticular-disease.html. Accessed online: 5 Sep 2017
Tursi A, Brandimarte G, Giorgetti G, Elisei W, Maiorano M, Aiello F (2008) The clinical picture of uncomplicated versus complicated diverticulitis of the colon. Dig Dis Sci 53:2474–2479
Feingold D, Steele SR, Lee S, Kaiser A, Boushey R, Buie WD et al (2014) Practice parameters for the treatment of sigmoid diverticulitis. Dis Colon Rectum 57:284–294. 9
Sartelli M, Viale P, Catena F, Ansaloni L, Moore E, Malangoni M et al (2013) 2013 WSES guidelines for management of intra-abdominal infections. World J Emerg Surg 8:3
[Guideline] Stollman N, Smalley W, Hirano I, AGA Institute Clinical Guidelines Committee (2015 Dec) American Gastroenterological Association Institute guideline on the management of acute diverticulitis. Gastroenterology 149(7):1944–1949
De Korte N, Klarenbeek BR, Kuyvenhoven JP, Roumen RM, Cuesta MA, Stockmann HB (2011) Management of diverticulitis: results of a survey among gastroenterologists and surgeons. Colorectal Dis 13:e411–e417
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP et al (2009) The PRISMA statement for reporting systematic reviews and metaanalyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700. https://doi.org/10.1136/bmj.b2700
National Institute for Health and Clinical Excellence. NICE clinical guidelines, Appendix 4 Quality of case series form. http://www.nice.org.uk/ nicemedia/ pdf/Appendix_04_qualityofcase_series_form_preop.pdf
Scottish Intercollegiate Guidelines Network (SIGN) guidelines, methodology checklist 3. http://www.sign.ac.uk/methodology/checklists.html
Ambrosetti P, Grossholz M, Becker C, Terrier F, Morel P (1997) Computed tomography in acute left colonic diverticulitis. Br J Surg 84(4):532–534
Wasvary H, Turfah F, Kadro O, Beauregard W (1999) Same hospitalization resection for acute diverticulitis. Am Surg 65:632–635 (discussion 636)
Wallace BC, Schmid CH, Lau J, Trikalinos TA (2009) Meta-Analyst: software for meta-analysis of binary, continuous and diagnostic data. BMC Med Res Methodol 9:80. https://doi.org/10.1186/1471-2288-9-80
Daniels L, Ünlü Ç, de Korte N, van Dieren S, Stockmann HB, Vrouenraets BC et al (2017) Randomized clinical trial of observational versus antibiotic treatment for a first episode of CT-proven uncomplicated acute diverticulitis. Br J Surg 104(1):52–61. https://doi.org/10.1002/bjs.10309
Brochmann ND, Schultz JK, Jakobsen GS, Øresland T (2016) Management of acute uncomplicated diverticulitis without antibiotics: a single-centre cohort study. Colorectal Dis 18(11):1101–1107. https://doi.org/10.1111/codi.13355
Mali JP, Mentula PJ, Leppäniemi AK, Sallinen VJ (2016) Symptomatic treatment for uncomplicated acute diverticulitis: a prospective cohort study. Dis Colon Rectum 59(6):529–534. https://doi.org/10.1097/DCR.0000000000000579
Estrada Ferrer O, Ruiz Edo N, Hidalgo Grau LA, Abadal Prades M, Del Bas Rubia M, Garcia Torralbo EM et al. Selective non-antibiotic treatment in sigmoid diverticulitis: is it time to change the traditional approach? Tech Coloproctol 2016 20(5):309–315. https://doi.org/10.1007/s10151-016-1464-0
Isacson D, Thorisson A, Andreasson K, Nikberg M, Smedh K, Chabok A (2015) Outpatient, non-antibiotic management in acute uncomplicated diverticulitis: a prospective study. Int J Colorectal Dis 30(9):1229–1234. https://doi.org/10.1007/s00384-015-2258-y
Isacson D, Andreasson K, Nikberg M, Smedh K, Chabok A (2014 Dec) No antibiotics in acute uncomplicated diverticulitis: does it work? Scand J Gastroenterol 49(12):1441–1446. https://doi.org/10.3109/00365521.2014.968861
Chabok A, Påhlman L, Hjern F, Haapaniemi S, Smedh K, AVOD Study Group (2012) Randomized clinical trial of antibiotics in acute uncomplicated diverticulitis. Br J Surg 99(4):532–539. https://doi.org/10.1002/bjs.8688
de Korte N, Kuyvenhoven JP, van der Peet DL, Felt-Bersma RJ, Cuesta MA, Stockmann HB. Mild colonic diverticulitis can be treated without antibiotics. A case-control study. Colorectal Dis. 2012 14(3):325–330. https://doi.org/10.1111/j.1463-1318.2011.02609.x
Hjern F, Josephson T, Altman D, Holmström B, Mellgren A, Pollack J et al (2007) Conservative treatment of acute colonic diverticulitis: are antibiotics always mandatory? Scand J Gastroenterol 42(1):41–47
O’Leary DP, Lynch N, Clancy C, Winter DC, Myers E. International (2015) Expert-based, consensus statement regarding the management of acute diverticulitis. JAMA Surg 150:899–904
Vennix S, Morton DG, Hahnloser D, Lange JF, Bemelman WA (2014) Systematic review of evidence and consensus on diverticulitis: an analysis of national and international guidelines. Colorectal Dis 16:866
Almy TP, Howell DA (1980) Medical progress. Diverticular disease of the colon. N Engl J Med 302:324–331
Ridgway PF1, Latif A, Shabbir J, Ofriokuma F, Hurley MJ, Evoy D et al (2009) Randomized controlled trial of oral vs intravenous therapy for the clinically diagnosed acute uncomplicated diverticulitis. Colorectal Dis 11(9):941–946. https://doi.org/10.1111/j.1463-1318.2008.01737.x
Biondo S, Golda T, Kreisler E, Espin E, Vallribera F, Oteiza F et al (2014) Outpatient versus hospitalization management for uncomplicated diverticulitis: a prospective, multicenter randomized clinical trial (DIVER Trial). Ann Surg 259(1):38–44
Tandon A, Fretwell VL, Nunes QM, Rooney PS (2018) Antibiotics versus no antibiotics in the treatment of acute uncomplicated diverticulitis—a systematic review and meta-analysis. Colorectal Dis. https://doi.org/10.1111/codi.14013 [Epub ahead of print]
Acknowledgements
The authors would like to express their thanks and gratitude to Professor Basem Eldeek, PhD for his sincere help in conducting and reviewing the statistical analyses used in the present systematic review and meta-analysis.
Author information
Authors and Affiliations
Contributions
SHE designed the review. SHE, HE, MS, and AS participated in data collection and analysis, writing and drafting of the manuscript. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study informed consent is not required.
Rights and permissions
About this article
Cite this article
Emile, S.H., Elfeki, H., Sakr, A. et al. Management of acute uncomplicated diverticulitis without antibiotics: a systematic review, meta-analysis, and meta-regression of predictors of treatment failure. Tech Coloproctol 22, 499–509 (2018). https://doi.org/10.1007/s10151-018-1817-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-018-1817-y