Abstract
Background
The aim of this study was to assess sexual function and quality of life (QoL) in patients after surgery for perianal Crohn’s disease.
Methods
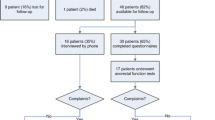
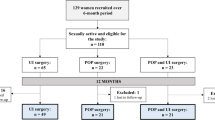
Eighty-eight consecutive patients with perianal Crohn’s disease, operated on at the Medical University of Vienna, completed a self-administered questionnaire including the International Index of Erectile Function (IIEF), Female Sexual Function Index (FSFI), Short Form-12 Health Survey (SF-12), and the Inflammatory Bowel Disease Questionnaire (IBDQ). Patients with a current stoma were excluded from further analysis. The median follow-up time was 104 months (range 3–186 months). Healthy subjects served as controls for each case and were matched by age (±6 years) and gender. Forty-seven (68 %) female and 22 male patients with a median age of 46.5 years (range 18–64 years) were analyzed. Eleven (16 %) patients had simple and 58 (84 %) complex anal fistulas.
Results
The median SF-12 physical health score of the patients was significantly lower (47.9 (range 25.5–57.2)) than that of the controls (54.3 (range 34.6–61.8); p = 0.03). Not surprisingly, the median total sore of the IBDQ of the controls was significantly better than that of the patients (controls: 188.5 (range 125–206.5), patients: 157 (range 60–199.5); p < 0.0001). Analysis with the multiple logistic regression test showed that type of operation, >1 perianal fistula opening, and active Crohn’s disease were independent risk factors for a worse IBDQ (p = 0.03, p = 0.015 and p < 0.0001). Interestingly, the median FSFI and IIEF score were not found to be significant different in any domain.
Conclusions
QoL but not sexual function is significantly influenced by surgery for perianal Crohn’s disease.
Similar content being viewed by others
References
Schwartz DA, Loftus EV Jr, Tremaine WJ et al (2002) The natural history of fistulizing Crohn’s disease in Olmsted County, Minnesota. Gastroenterology 122:875–880
Singh B, McC Mortensen NJ, Jewell DP, George B (2004) Perianal Crohn’s disease. Br J Surg 91:801–814
Taxonera C, Schwartz DA, Garcia-Olmo D (2009) Emerging treatments for complex perianal fistula in Crohn’s disease. World J Gastroenterol 15:4263–4272
Makowiec F, Jehle EC, Starlinger M (1995) Clinical course of perianal fistulas in Crohn’s disease. Gut 37:696–701
Kasparek MS, Glatzle J, Temeltcheva T, Mueller MH, Koenigsrainer A, Kreis ME (2007) Long-term quality of life in patients with Crohn’s disease and perianal fistulas: influence of fecal diversion. Dis Colon Rectum 50:2067–2074
Parks AG, Gordon PH, Hardcastle JD (1976) A classification of fistula-in-ano. Br J Surg 63:1–12
Dubsky PC, Stift A, Friedl J, Teleky B, Herbst F (2008) Endorectal advancement flaps in the treatment of high anal fistula of cryptoglandular origin: full-thickness vs. mucosal-rectum flaps. Dis Colon Rectum 51:852–857
Janke KH, Klump B, Steder-Neukamm U, Hoffmann J, Hauser W (2006) Validation of the German version of the inflammatory bowel disease questionnaire (competence network IBD, IBDQ-D). Psychother Psychosom Med Psychol 56:291–298
Ware J Jr, Kosinski M, Keller SD (1996) A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med Care 34:220–233
Rosen R, Brown C, Heiman J et al (2000) The female sexual function index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 26:191–208
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A (1997) The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 49:822–830
Wiegel M, Meston C, Rosen R (2005) The female sexual function index (FSFI): cross-validation and development of clinical cutoff scores. J Sex Marital Ther 31:1–20
Timmer A, Kemptner D, Bauer A, Takses A, Ott C, Furst A (2008) Determinants of female sexual function in inflammatory bowel disease: a survey based cross-sectional analysis. BMC Gastroenterol 8:45
El-Gazzaz G, Hull T, Mignanelli E, Hammel J, Gurland B, Zutshi M (2010) Analysis of function and predictors of failure in women undergoing repair of Crohn’s related rectovaginal fistula. J Gastrointest Surg 14:824–829
Takesue Y, Ohge H, Yokoyama T, Murakami Y, Imamura Y, Sueda T (2002) Long-term results of seton drainage on complex anal fistulae in patients with Crohn’s disease. J Gastroenterol 37:912–915
Delaney CP, Kiran RP, Senagore AJ et al (2003) Quality of life improves within 30 days of surgery for Crohn’s disease. J Am Coll Surg 196:714–721
Tillinger W, Mittermaier C, Lochs H, Moser G (1999) Health-related quality of life in patients with Crohn’s disease: influence of surgical operation—a prospective trial. Dig Dis Sci 44:932–938
Cadahia V, Garcia-Carbonero A, Vivas S et al (2004) Infliximab improves quality of life in the short-term in patients with fistulizing Crohn’s disease in clinical practice. Rev Esp Enferm Dig 96:369–374
Ng SC, Plamondon S, Gupta A, Burling D, Kamm MA (2009) Prospective assessment of the effect on quality of life of anti-tumour necrosis factor therapy for perineal Crohn’s fistulas. Aliment Pharmacol Ther 30:757–766
Sands BE, Anderson FH, Bernstein CN et al (2004) Infliximab maintenance therapy for fistulizing Crohn’s disease. N Engl J Med 350:876–885
Blondel-Kucharski F, Chircop C, Marquis P et al (2001) Health-related quality of life in Crohn’s disease: a prospective longitudinal study in 231 patients. Am J Gastroenterol 96:2915–2920
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Riss, S., Schwameis, K., Mittlböck, M. et al. Sexual function and quality of life after surgical treatment for anal fistulas in Crohn’s disease. Tech Coloproctol 17, 89–94 (2013). https://doi.org/10.1007/s10151-012-0890-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-012-0890-x