As is in life... In their quest for the truth, men make two steps ahead and one behind. Suffering, errors and boredom push them backwards, but thirst for the truth and obstinate will, pushes them forwards. And who knows? Perhaps they will find the truth.
Anton Checov
Abstract
Background
Transanal haemorrhoidal dearterialisation (THD) is a nonexcisional surgical technique for the treatment of piles, consisting in the ligation of the distal branches of the superior rectal artery, resulting in a reduction of blood flow and decongestion of the haemorrhoidal plexus. The aim of this study was to assess the long-term efficacy of this treatment.
Methods
The procedure was carried out using a proctoscope with a Doppler probe. The terminal branches were located with Doppler and then sutured.
Results
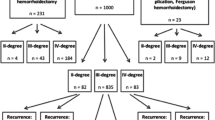
From January 2000 to May 2006, we performed THD in 330 patients (180 men; mean age, 52.4 years), including 138 second-degree, 162 third-degree and 30 fourth-degree haemorrhoids. There were 23 postoperative complications (7 cases of bleeding, 5 thrombosed piles, 4 rectal haematomas, 2 anal fissures, 2 cases of dysuria, 1 of haematuria and 2 needle ruptures). The mean postoperative pain score was 1.32 on a visual analog scale. 219 patients were followed for a mean of 46 months (range, 22–79), including 100 patients with second-degree, 104 with third-degree and 15 with fourth-degree haemorrhoids. The operation completely resolved the symptoms in 132 patients (92.5%) with preoperative bleeding and in 110 patients (92%) with preoperative prolapse.
Conclusions
The efficacy and relapse rate of this procedure appears to be similar to that of traditional surgery and stapled haemorrhoidopexy. The technique was effective and safe for all degrees of haemorrhoids because of the excellent results, low complication rate and minor postoperative pain.
Similar content being viewed by others
References
Fijten GH, Blijham GH, Knottnerus JA (1994) Occurrence and clinical significance of overt blood loss per rectum in the general population and in medical practice. Br J Gen Pract 44:320–325
Johanson JF, Sonnemberg A (1990) The prevalence of hemorrhoids and chronic constipation. An epidemiological study. Gastroenterology 98:380–386
Bleday R, Pena JP, Rothenberger DA, Goldberg SM, Buls JG (1992) Symptomatic hemorrhoids: current incidence and complications of operative therapy. Dis Colon Rectum 35:477–481
Haas PA, Haas GP, Schmaltz S, Fox TA (1983) The prevalence of haemorrhoids. Dis Colon Rectum 26:435–439
Milligan ETC, Morgan CN, Jones LE, Officer R (1937) Surgical anatomy of the anal canal and the operative treatment of haemorrhoids. Lancet II:1119–1123
Ferguson JA, Heaton JR (1959) Closed hemorrhoidectomy. Dis Colon Rectum 2:176–179
Chew SS, Marshall L, Kalish L, Tham J, Grieve DA, Douglas PR, Newstead GL (2003) Short-term and long-term results of combined sclerotherapy and rubber band ligation of hemorrhoids and mucosal prolapse. Dis Colon Rectum 46:1232–1237
Savioz D, Roche B, Glauser T, Dobrinov A, Ludwig C, Marti MC (1998) Rubber band ligation of hemorrhoids: relapse as a function of time. Int J Colorectal Dis 13:154–156
Iyer VS, Shrier I, Gordon PH (2004) Long-term outcome of rubber band ligation for symptomatic primary and recurrent internal hemorrhoids. Dis Colon Rectum 47:1364–1370
Longo A (1998) Treatment of hemorrhoids disease by reduction of mucosa and hemorrhoidal prolapse with a circular suturing device: a new procedure. Presented at: 6th World Congress of Endoscopic Surgery, Rome, 3–6 June 1998. Manduzzi, Rome, pp 777–784.
Ripetti V, Caricato M, Arullani A (2002) Rectal perforation, retropneumoperitoneum, and pneumomediastinum after stapling procedure for prolapsed hemorrhoids: report of a case and subsequent considerations. Dis Colon Rectum 45:268–270
Cheetham MJ, Mortensen NJ, Nystrom PO, Kamm MA, Phillips RK (2000) Persistent pain and faecal urgency after stapled haemorrhoidectomy. Lancet 356:730–733
Jongen J, Bock JU, Peleikis HG, Eberstein A, Pfister K (2006) Complications and reoperations in stapled anopexy: learning by doing. Int J Colorectal Dis 21:166–171
Aumann G, Petersen S, Pollack T, Hellmich G, Ludwig K (2004) Severe intra-abdominal bleeding following stapled mucosectomy due to enterocele: report of a case. Tech Coloproctol 8:41–43
Morinaga K, Hacuda K, Ikeda T (1995) A novel therapy for internal haemorrhoids: ligation of the haemorrhoidal artery with a newly devised instrument in conjunction with Doppler flow meter. Am J Gastroenterol 90(4):610–613
Sohn N, Aronoff JS, Cohen FS, Weinstein MA (2001) Transanal hemorrhoidal dearterialization is an alternative to operative hemorrhoidectomy. Am J Surg 182:515–519
Arnold S, Antonietti E, Rollinger G, Scheyer M (2002) Doppler ultrasound assisted hemorrhoid artery ligation. A new therapy in symptomatic hemorrhoids. Chirurg 73:269–273
Shelygin IuA, Titov AIu, Veselov VV, Kanametov MKh (2003) Results of ligature of distal branches of the upper rectal artery in chronic hemorrhoid with the assistance of Doppler ultrasonography. Khirurgiia (Mosk) 1:39–44 (article in Russian)
Charua Guindic L, Fonseca Munoz E, Garcia Perez NJ, Osorio Hernandez RM, Novarrete Cruces T, Avendano Espinosa O, Guerra Melgar LR (2004) Hemorrhoidal desarterialization guided by Doppler. A surgical alternative in hemorrhoidal disease management. Rev Gastroenterol Mex 69:83–87
Lienert M, Ulrich B (2004) Doppler-guided ligation of the hemorrhoidal arteries. Report of experiences with 248 patients. Dtsch Med Wochenschr 129:947–950
Infantino A, Amadio L, Bellomo R et al (2006) Doppler-guided transanal haemorrhoidal dearterialisation is a valid treatment option for II–III degrees haemorrhoidal disease. In: Proceedings of the Second Joint Meeting of the European Council of Coloproctology — ECCP and European Association of Coloproctology (EACP) and First National Congress of the Italian Society of Colorectal Surgery (SICCR) September 15–17, 2005. Monduzzi Editore, Bologna
Felice G, Privitera A, Ellul E, Klaumann M (2005) Doppler-guided hemorrhoidal artery ligation: an alternative to hemorrhoidectomy. Dis Colon Rectum 48:2090–2093
Ramirez JM, Aguilella V, Elia M, Gracia JA, Martinez MD (2005) Doppler-guided hemorrhoidal artery ligation in the management of symptomatic hemorrhoids. Rev Esp Enferm Dig 97:97–103
Greenberg R, Karin E, Avital S, Skornick Y, Werbin N (2006) First 100 cases with Doppler-guided hemorrhoidal artery ligation. Dis Colon Rectum 49:485–489
Scheyer M, Antonietti E, Rollinger G, Mall H, Arnold S (2006) Doppler-guided hemorrhoidal artery ligation. Am J Surg 191:89–93
Bursics A, Morvay K, Kupcsulik P, Flautner L (2004) Comparison of early and 1-year follow-up results of conventional hemorrhoidectomy and hemorrhoid artery ligation: a randomized study. Int J Colorectal Dis 1:176–180
Tagariello C, Dal Monte PP, Saragò M (2004) Doppler-guided transanal haemorrhoidal dearterialisation. Chir Ital 56:693–697 (article in Italian)
Thomson WHF (1975) The nature of haemorrhoids. Br J Surg 62:542–552
Thulesis Ø, Gjöres JE (1973) Arterio-venous anastomosis in the anal region with reference to the pathogenesis and treatment of haemorrhoids. Acta Chir Scand 139:476–478
Haas PA, Fox TA, Haas GP (1984) The pathogenesis of hemorrhoids. Dis Colon Rectum 27:442–450
Stelzner F, Staubesand J, Machleidt H (1962) Das corpus cavernosum recti — die Grundlage der inneren Hämorrhoiden. Langenbecks Arch klein Chir 299:302–312
Widmer O (1955) Die Rectalarterien des Menschen. Anat Entwicklungsgesch 118:398–416
Patricio J, Bernades A, Nuno D et al (1988) Surgical anatomy of the arterial blood-supply of the human rectum. Surg Radiol Anat 10:71–75
Shafik A, Mostafa H (1996) Study of the arterial pattern of the rectum and its clinical application. Acta Anat 157:80–86
Aigner F, Bodner G, Conrad F, Mbaka G, Kreczy A, Fritsch H (2004) The superior rectal artery and its branching pattern with regard to its clinical influence on ligation techniques for internal hemorrhoids. Am J Surg 187:102–108
Gibbons CP, Trowbridge EA, Bannister JJ, Read NW (1986) The role of the anal cushions in maintaining continence. Lancet 1:886–887
Lestar B, Penninckx F, Rigauts H, Kerremans R (1992) The internal anal sphincter can not close the anal canal completely. Int J Colorecal Dis 7:159–161
Penninckx F, Lestar B, Kerremans R (1992) The internal anal sphincter: mechanisms of control and its role in maintaining anal continence. Baill Clin Gastroenterol 6:193–214
Gass OC, Adams J (1950) Hemorrhoids: etiology and pathology. Am J Surg 79:40–43
Loder PB, Kamm MA, Nicholls RJ (1994) Haemorrhoids: pathology, pathophysiology and aetiology. Br J Surg 81:946–954
Sun WM, Read NW, Shorthouse AJ (1990) Hypertensive anal cushions as a cause of high anal canal pressures in patients with haemorrhoids. Br J Surg 77:458–462
Sun WM, Peck RJ, Shorthouse AJ, Read NW (1992) Haemorrhoids are associated not with hypertrophy of the internal sphincter, but with hypertension of the anal cushions. Br J Surg 78:592–594
References
Jayaraman S, Colquhoun PH, Malthaner RA (2007) Stapled hemorrhoidopexy is associated with a higher long-term recurrence rate of internal hemorrhoids compared with conventional excisional hemorrhoid surgery. Dis Colon Rectum 50:1297–1305
Carapeti EA, Kamm MA, McDonald PJ, Phillips RK (1998) Double-blind randomised controlled trial of effect of metronidazole on pain after day-case haemorrhoidectomy. Lancet 351(9097):169–172
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dal Monte, P.P., Tagariello, C., Giordano, P. et al. Transanal haemorrhoidal dearterialisation: nonexcisional surgery for the treatment of haemorrhoidal disease. Tech Coloproctol 11, 333–339 (2007). https://doi.org/10.1007/s10151-007-0376-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-007-0376-4