Abstract
Background
Alpha-Fetoprotein Producing Gastric Cancer (AFPGC) is an aggressive subgroup of gastric cancer. Recently ramucirumab has shown survival benefits in hepatocellular carcinoma, but only in those with higher Alpha-Fetoprotein (AFP) levels. However, the efficacy of ramucirumab-containing chemotherapy in AFPGC remains unclear.
Methods
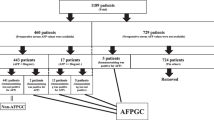
We retrospectively assessed 352 patients who received ramucirumab-containing chemotherapy between June 2015 and December 2019. AFPGC was defined when serum AFP levels were elevated at diagnosis and correlated with the disease state during treatment. Non-AFPGC was defined when serum AFP levels were normal at diagnosis.
Results
Among the 352 patients, 28 patients were defined as AFPGC and 246 patients were defined as non-AFPGC. AFPGC was characterized by high frequency of liver metastasis and low frequency of peritoneal metastasis compared to non-AFPGC. Ramucirumab containing chemotherapy showed higher response rates in AFPGC (39.1% vs 24.8%, p = 0.198) and disease control rates (86.9% vs 61.5%, p = 0.028) than those of non-AFPGC, respectively. Median progression-free survival (PFS) was 5.5 months (95%CI 3.9–7.1) in AFPGC and 4.0 months (95%CI 3.6–4.6) in non-AFPGC (HR: 0.91, 95% CI 0.61–1.36, p = 0.66), and median overall survival (OS) was 10.7 months (95% CI 7.4–20.8) in AFPGC and 9.2 months (95% CI 8.1–10.4) in non-AFPGC (HR: 0.72, 95% CI 0.48–1.08, p = 0.11), respectively. In multivariate analysis, AFPGC was not a negative prognostic factor both for PFS and OS.
Conclusion
Ramucirumab containing chemotherapy showed higher response and comparable survival in AFPGC compared to those of non-AFPGC. Considering the generally poor prognosis of AFPGC, ramucirumab-containing chemotherapy might be a promising treatment option in AFPGC.




Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article and its supplementary information files.
References
Bergstrand CG, Czar B (1956) Demonstration of a new protein fraction in serum from the human fetus. Scand J Clin Lab Invest 8:174–179
Smith CJ, Ajdukiewicz A, Kelleher PC (1983) Concanavalin-a-affinity molecular heterogeneity of human hepatoma AFP and cord-serum AFP. Ann N Y Acad Sci 417:69–74
Norgaard-Pedersen B, Albrechtsen R, Teilum G (1975) Serum alphafoetoprotein as a marker for endodermal sinus tumour (yolk sac tumour) or a vitelline component of “teratocarcinoma.” Acta Pathologica et Microbiologica Scand Sec A Pathol 83(6):573–589
European Association for the Study of the Liver (2019) EASL clinical practice guidelines management of hepatocellular carcinoma. J Hepatol 69(1):182–236
Metzgeroth G, Strobel P, Baumbusch T et al (2010) Hepatoid adenocarcinoma review of the literature illustrated by a rare case originating in the peritoneal cavity. Onkologie 33:263–269
Kinjo T, Taniguchi H, Kushima R et al (2012) Histologic and immunohistochemical analyses of α-fetoprotein-producing cancer of the stomach. Am J Surg Pathol 36:56–65
Yamagata T, Yamagata Y, Nakanishi M et al (2004) A case of primary lung cancer producing alpha-fetoprotein. Can Respir J 11:504–506
Matsueda K, Yamamoto H, Yoshida Y et al (2006) Hepatoid carcinoma of the pancreas producing protein induced by vitamin K absence or antagonist II (PIVKA-II) and alpha-fetoprotein (AFP). J Gastroenterol 41:1011–1019
Devi NR, Sathyalakshmi R, Devi J et al (2015) Hepatoid adenocarcinoma of the gall bladder-a rare variant. J Clin Diagn Res JCDR. https://doi.org/10.7860/JCDR/2015/10799.6324
Cappetta A, Bergamo F, Mescoli C et al (2012) Hepatoid adenocarcinoma of the colon: what should we target? Pathol Oncol Res 18:93–96
Bourreille J, Metayer P, Sauger F et al (1970) Existence of alpha feto protein during gastric-origin secondary cancer of the liver. Presse Med 78:1277–1278
McIntire KR, Waldmann TA, Moertel CG et al (1975) Serum alphafetoprotein in patients with neoplasms of the gastrointestinal tract. Cancer Res 35(4):991–996
Chang YC, Nagasue N, Kohno H et al (1990) Clinicopathologic features and long-term results of alphafetoprotein-producing gastric cancer. Am J Gastroenterol 85(11):1480–1485
Adachi Y, Tsuchihashi J, Shiraishi N et al (2003) AFP-producing gastric carcinoma: multivariate analysis of prognostic factors in 270 patients. Oncology 65(2):95–101
Bozkaya Y, Demirci NS, Kurtipek A et al (2017) Clinicopathological and prognostic characteristics in patients with AFP-secreting gastric carcinoma. Mol Clin Oncol 7(2):267–274
Fuchs CS, Tomasek J, Yong CJ et al (2014) Ramucirumab monotherapy for previously treated advanced gastric or gastro-oesophageal junction adenocarcinoma (REGARD): An international, randomised, multicentre, placebo-controlled, phase 3 trial. Lancet 383:31–39
Wilke H, Muro K, Van Cutsem E et al (2014) Ramucirumab plus paclitaxel versus placebo plus paclitaxel in patients with previously treated advanced gastric or gastro-oesophageal junction adenocarcinoma (RAINBOW): A double-blind, randomised phase 3 trial. Lancet Oncol 15:1224–1235
Zhu AX, Park JO, Ryoo BY et al (2015) Ramucirumab versus placebo as second-line treatment in patients with advanced hepatocellular carcinoma following first-line therapy with sorafenib (REACH): a randomised, double-blind, multicentre, phase 3 trial. Lancet Oncol 16(7):859–870
Zhu AX, Kang YK, Yen CJ et al (2019) Ramucirumab after sorafenib in patients with advanced hepatocellular carcinoma and increased α-fetoprotein concentrations (REACH-2): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol 20(2):282–296
Inagawa S, Shimazaki J, Hori M et al (2001) Hepatoid adenocarcinoma of the stomach. Gastric Cancer 4(1):43–52
Inoue M, Sano T, Kuchiba A et al (2010) Long-term results of gastrectomy for alpha-fetoprotein-producing gastric cancer. Br J Surg 97(7):1056–1061
Yoshizawa J, Ishizone S, Ikeyama M et al (2017) Gastric hepatoid adenocarcinoma resulting in a spontaneous gastric perforation: a case report and review of the literature. BMC Cancer 17(1):368
He R, Yang Q, Dong X et al (2017) Clinicopathologic and prognostic characteristics of alpha-fetoprotein-producing gastric cancer. Oncotarget 8(14):23817–23830
Wang Y-K, Shen L, Jiao Xi et al (2018) Predictive and prognostic value of serum AFP level and its dynamic changes in advanced gastric cancer patients with elevated serum AFP. World J Gastroenterol 24(2):266–273
Li N, Bai C, Zhang R et al (2021) Efficacy and safety of apatinib for the treatment of AFP-producing gastric cancer. Translat Oncolo 14(2):101004
Kanda Y (2013) Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant 48:452–458
Bang YJ, Van Cutsem E, Feyereislova A et al (2010) Trastuzumab in combination with chemotherapy versus chemotherapy alone for treatment of HER2-positive advanced gastric or gastro-oesophageal junction cancer (ToGA): a phase 3, open-label, randomised controlled trial. Lancet 376:687–697
Kang YK, Boku N, Satoh T et al (2017) Nivolumab in patients with advanced gastric or gastro-oesophageal junction cancer refractory to, or intolerant of, at least two previous chemotherapy regimens (ONO-4538-12, ATTRACTION-2): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 390(10111):2461–2471
Yoshioka M, Inoue N, Someda H et al (2011) A case of AFP-producing gastric cancer resected after efficient S-1/CDDP combination chemotherapy. Gan To Kagaku Ryoho 38(1):105
Fukuda K, Ito S, Shimizu K et al (2013) Retrospective analysis concerning AFP-producing gastric cancer. Gan Kagaku Ryoho 40(2):191
Kunoki N, Nishiyama R, Ryuzaki H et al (2008) A case of alpha-fetoprotein-producing gastric cancer with hepatic metastasis successfully treated with combination chemotherapy. Nihon Shokakibyo Gakkai Zasshi 105(10):1489
Arakawa Y, Tamura M, Aiba K et al (2017) Significant response to ramucirumab monotherapy in chemotherapy-resistant recurrent alpha-fetoprotein-producing gastric cancer: a case report. Oncol Lett 14(3):3039–3042
Takada J, Araki H, Ozawa N et al (2019) Effective treatment of cytotoxic agent refractory alpha-fetoprotein-producing gastric cancer with ramucirumab: a case report and review of the literature. J Gastrointest Canc 50:556–559
Iida A, Katayama K, Yamaguchi A (2013) Five-year survival of alpha-fetoprotein-producing gastric cancer with synchronous liver metastasis: a case report. J Gastric Cancer 13:58–64
Fang YU, Wang L, Yang N et al (2015) Successful multimodal therapy for an α-fetoprotein-producing gastric cancer patient with simultaneous liver metastases. Oncol Lett 10:3021–3025
Di Bartolomeo M, Niger M, Tirino G et al (2018) Ramucirumab as second-line therapy in metastatic gastric cancer: real-world data from the ramoss study. Target Oncol 13(2):227–234
Lu J, Ding Y, Chen Y et al (2021) Whole-exome sequencing of alpha-fetoprotein producing gastric carcinoma reveals genomic profile and therapeutic targets. Nat Commun 12(1):3946
Liu D, Li B, Yan B et al (2020) The clinicopathological features and prognosis of serum AFP positive gastric cancer: a report of 16 cases. Int J Clin Exp Pathol 13(9):2439–2446
Yamashita T, Forgues M, Wang W et al (2008) EpCAM and alpha-fetoprotein expression defines novel prognostic subtypes of hepatocellular carcinoma. Cancer Res 68:1451–1461
Shan YF, Huang YL, Xie YK et al (2011) Angiogenesis and clinicopathologic characteristics in different hepatocellular carcinoma subtypes defined by EpCAM and alpha-fetoprotein expression status. Med Oncol 28:1012–1016
Zucman-Rossi J, Villanueva A, Nault JC et al (2015) Genetic landscape and biomarkers of hepatocellular carcinoma. Gastroenterology 149:1226–1239
Koide N, Nishio A, Igarashi J et al (1999) Alpha-fetoprotein-producing gastric cancer: Histochemical analysis of cell proliferation, apoptosis, and angiogenesis. Am J Gastroenterol 94:1658–1663
Kamei S, Kono K, Amemiya H et al (2003) Evaluation of VEGF and VEGF-C expression in gastric cancer cells producing alpha-fetoprotein. J Gastroenterol 38:540–547
Wang Y, Sun L, Li Z et al (2019) Hepatoid adenocarcinoma of the stomach: a unique subgroup with distinct clinicopathological and molecular features. Gastric Cancer 22:1183–1192
Acknowledgements
The authors would like to thank all staff who managed the study patients at the ambulatory treatment center and on the wards.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
Daisuke Takahari reports receiving honoraria from Taiho Pharmaceutical Co., Ltd., Ono Pharmaceutical Co. and Eli Lilly. Kensei Yamaguchi reports receiving honoraria from Eli Lilly, receiving research funding from Eli Lilly. The other authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10147_2022_2263_MOESM3_ESM.pptx
Supplementary Fig.2 Correlations between the baseline AFP levels at the stating of 2nd-line treatment, PFS (a) and OS (b), respectively (PPTX 69 KB)
10147_2022_2263_MOESM4_ESM.pptx
Supplementary Fig.3 Comparison of PFS (a) and OS (b) according to the baseline AFP levels with the cutoff value of 1,200 ng/ml (PPTX 70 KB)
10147_2022_2263_MOESM5_ESM.pptx
Supplementary Fig.4 Comparison of ORR (a) and DCC (b) according to the baseline AFP levels with the cutoff value of 1,200 ng/ml (PPTX 67 KB)
10147_2022_2263_MOESM6_ESM.pptx
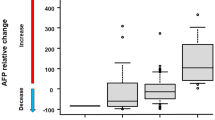
Supplementary Fig.5 Changes in AFP levels during 2nd-line treatment (a). Comparison of ORR (b) and DCR (c) according to changes in AFP levels during 2nd-line treatment (PPTX 73 KB)
10147_2022_2263_MOESM7_ESM.pptx
Supplementary Fig.6 Comparison of PFS (a) and OS (b) according to changes in AFP levels during 2nd-line treatment (PPTX 69 KB)
About this article
Cite this article
Kamiimabeppu, D., Wakatsuki, T., Takahari, D. et al. Treatment efficacy of ramucirumab-containing chemotherapy in patients with alpha-fetoprotein producing gastric cancer. Int J Clin Oncol 28, 121–129 (2023). https://doi.org/10.1007/s10147-022-02263-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-022-02263-0