Abstract
Background
The decline of health-related quality-of-life (QOL) during the year after radical prostatectomy is severe. General self-efficacy (GSE) is an effective psychological factor for long-term regulation of patient behavior and emotions. GSE is expected to facilitate enhanced health-related quality of life. We evaluated changes in GSE and analyzed the relationship between GSE and prostate cancer-specific and general health-related QOL.
Methods
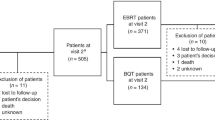
We conducted a longitudinal survey with 104 patients who underwent radical prostatectomy and administered the General Self-efficacy Scale (GSES), Expanded Prostate Cancer Index Composite (EPIC), and SF8 Health Survey (SF-8). ANCOVA was performed to compare EPIC and SF-8 between GSES high and low-medium groups.
Results
GSES scores increased significantly after 6 months. Regarding EPIC urinary summary scores, high GSES group was significantly higher than low-medium group at 1 month (mean score difference [MSD], 7.3; 95% CI 1.1–13.2, P = 0.016), 3 months (MSD, 6.8; 95% CI 0.7–12.8, P = 0.028), and 6 months (MSD, 6.3; 95% CI 0.9–11.7, P = 0.022). High GSES group had significantly higher SF-8 physical component summary score at 6 months (MSD, 3.2; 95% CI 1.4–5.0, P = 0.001), and significantly higher SF-8 mental component summary score at 1 month (MSD, 2.6; 95% CI 0.4–4.9, P = 0.022), 3 months (MSD, 2.7; 95% CI 0.8–4.6, P = 0.007), and 6 months (MSD, 2.8; 95% CI 1.0–4.6, P = 0.003).
Conclusion
This study suggests that high GSE was associated with better prostate cancer-specific and general health-related QOL after radical prostatectomy.


Similar content being viewed by others
References
Cancer Registry and Statistics: Cancer Information Service, National Cancer Center, Japan. https://ganjoho.jp/data/reg_stat/statistics/brochure/2018/cancer_statistics_2018.pdf
Ito Y, Miyashiro I, Ito H et al (2014) Long-term survival and conditional survival of cancer patients in Japan using population-based cancer registry data. Cancer Sci 105:1480–1486
Bill-Axelson A, Holmberg L, Garmo H et al (2014) Radical prostatectomy or watchful waiting in early prostate cancer. N Engl J Med 370(10):932–942
Barocas DA, Alvarez J, Resnick MJ et al (2017) Association between radiation therapy, surgery, or observation for localized prostate cancer and patient-reported outcomes after 3 years. JAMA 317(11):1126–1140
Resnick MJ, Koyama T, Fan KH et al (2013) Long-term functional outcomes after treatment for localized prostate cancer. N Engl J Med 368(5):436–445
Namiki S, Kaiho Y, Mitsuzuka K et al (2014) Long-term quality of life after radical prostatectomy: 8-year longitudinal study in Japan. Int J Urol 21(12):1220–1226
Inoue S, Shiina H, Hiraoka T et al (2009) Five-year longitudinal effect of radical perineal prostatectomy on health-related quality of life in Japanese men, using general and disease-specific measures. BJU Int 104(8):1077–1084
Baker H, Wellman S, Lavender V (2016) Functional quality-of-life outcomes reported by men treated for localized prostate cancer: a systematic literature review. Oncol Nurs Forum 43(2):199–218
Bourke L, Boorjian SA, Briganti A et al (2015) Survivorship and improving quality of life in men with prostate cancer. Eur Urol 68(3):374–383
Lev EL, Eller LS, Kolassa J et al (2007) Exploratory factor analysis: strategies used by patients to promote health. World J Urol 25(1):87–93
Bandura A (1977) Self-efficacy: toward unifying theory of behavioral change. Psychol Rev 84(2):191–215
Eton DT, Lepore SJ, Helgeson VS (2001) Early quality of life in patients with localized prostate carcinoma: an examination of treatment-related, demographic, and psychosocial factors. Cancer 92(6):1451–1459
Campbell LC, Keefe FJ, McKee DC et al (2004) Prostate cancer in African Americans: relationship of patient and partner self-efficacy to quality of life. J Pain Symptom Manage 28(5):433–444
Lev EL, Eller LS, Gejerman G et al (2009) Quality of life of men treated for localized prostate cancer: outcomes at 6 and 12 months. Support Care Cancer 17(5):509–517
Sakano Y, Tohjoh M (1986) The general self-efficacy scale (GSES): scale development and validation. Jap J Behav Ther 12(1):73–82
Sherer M, Maddux JE, Mercandante B et al (1982) The self-efficacy scale—construction and validation. Psychol Rep 51(2):663–671
Curtis R, Groarke A, Sullivan F (2014) Stress and self-efficacy predict psychological adjustment at diagnosis of prostate cancer. Sci Rep 4:5569
da Mata LR, de Carvalho EC, Gomes CR et al (2015) Postoperative self-efficacy and psychological morbidity in radical prostatectomy. Rev Lat Am Enfermagem 23(5):806–813
Knoll N, Scholz U, Burkert S et al (2009) Effects of received and mobilized support on recipients’ and providers’ self-efficacy beliefs: a 1-year follow-up study with patients receiving radical prostatectomy and their spouses. Int J Psychol 44(2):129–137
Kong EH, Deatrick JA, Bradway CK (2017) Men’s experiences after prostatectomy: a meta-synthesis. Int J Nurs Stud 74:162–171
Kakehi Y, Takegami M, Suzukamo Y et al (2007) Health-related quality of life in Japanese men with localized prostate cancer treated with current multiple modalities assessed by a newly developed Japanese version of the Expanded Prostate Cancer Index Composite. J Urol 177:1856–1861
Wei JT, Dunn RL, Litwin MS et al (2000) Development and validation of the expanded prostate cancer index composite (EPIC) for comprehensive assessment of health-related quality of life in men with prostate cancer. Urology 56(6):899–905
Fukuhara S, Suzukamo Y (2004) Manual of the SF-8: Japanese version. Institute for Health Outcomes & Process Evaluation Research, Kyoto
Mitsuzuka K, Koie T, Narita S et al (2013) Changes in Indications and oncological outcomes of radical prostatectomy after 2000—data from 1268 Japanese patients treated with radical prostatectomy between 2000 and 2009. Jpn J Clin Oncol 43(8):821–826
Gallina A, Chun FKH, Nazareno S et al (2008) Comparison of stage migration patterns between Europe and the USA: an analysis of 11,350 men treated with radical prostatectomy for prostate cancer. BJU Int 101(12):1513–1518
Luszczynska A, Mohamed NE, Schwarzer R (2005) Self-efficacy and social support predict benefit finding 12 months after cancer surgery: the mediating role of coping strategies. Psychol Health Med 10(4):365–375
Schwarzer R, Boehmer S, Luszczynska A et al (2005) Dispositional self-efficacy as a personal resource factor in coping after surgery. Pers Individ Differ 39(4):807–818
Skolarus TA, Dunn RL, Sanda MG et al (2015) Minimally important difference for the expanded prostate cancer index composite short form. Urology 85(1):101–106
Parahoo K, McDonough S, McCaughan E et al (2015) Psychosocial interventions for men with prostate cancer: a cochrane systematic review. BJU Int 116(2):174–183
Doda N, Tokuda Y, Saiki K et al (2016) Assessment of self-efficacy and its relationship with frailty in the elderly. Intern Med 55(19):2785–2792
Acknowledgments
We sincerely thank all participants and collaborators for their cooperation. This work was supported by JSPS KAKENHI [Grant Numbers 15H06060, 19K19596]. Some of the results of this study were presented at 55th and 56th Annual Meeting of Japan Society of Clinical Oncology.The paper was presented by the author as a dissertation for the degree of Doctor of Philosophy in Nursing at Yamagata University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No author has any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kawaguchi, K., Kawazoe, H., Sakurai, T. et al. Effect of general self-efficacy on promoting health-related quality of life during recovery from radical prostatectomy: a 1-year prospective study. Int J Clin Oncol 25, 2122–2129 (2020). https://doi.org/10.1007/s10147-020-01765-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-020-01765-z