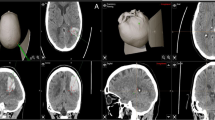
Abstract
Spontaneous intracerebral haemorrhage (ICH) is a devastating disease with a mortality rate of more than 40 % and a high morbidity rate with 10–15 % of survivors remaining fully dependent [11]. The role of surgical treatment of ICH remains a matter of controversy and ongoing investigation. Advances in neurosurgical techniques such as endoscopy and neuronavigation have been established in various fields of neurosurgery. Results of reported case series have suggested that some patients with ICH may benefit from haematoma evacuation through minimally invasive endoscopic procedures. In this article, we focus on the pathophysiologic rationales behind minimally invasive haematoma evacuation through endoscopic surgery and provide an overview of technical developments and reported patient series. In addition, the modalities of the surgical procedure at the authors’ institution are described. Controlled clinical trials are needed to evaluate the full potential and limitations of this promising technique.


Similar content being viewed by others
References
Altumbabic M, Peeling J, Bigio MRD (1998) Intracerebral hemorrhage in the rat: effects of hematoma aspiration. Stroke 29(9):1917–1923
Auer LM (1985) Endoscopic evacuation of intracerebral haemorrhage. High-tec-surgical treatment—a new approach to the problem? Acta Neurochir (Wien) 74(3–4):124–128
Auer LM, Ascher PW, Heppner F, Ladurner G, Boné G, Lechner H, Tölly E (1985) Does acute endoscopic evacuation improve the outcome of patients with spontaneous intracerebral hemorrhage? Eur Neurol 24(4):254–261
Bakshi A, Bakshi A, Banerji AK (2004) Neuroendoscope-assisted evacuation of large intracerebral hematomas: introduction of a new, minimally invasive technique. Preliminary report. Neurosurg Focus 16(6):e9
Broderick JP, Brott TG, Duldner JE, Tomsick T, Huster G (1993) Volume of intracerebral hemorrhage. A powerful and easy-to-use predictor of 30-day mortality. Stroke 24(7):987–993
Brott T, Broderick J, Kothari R, Barsan W, Tomsick T, Sauerbeck L, Spilker J, Duldner J, Khoury J (1997) Early hemorrhage growth in patients with intracerebral hemorrhage. Stroke 28(1):1–5
Chen C-C, Cho D-Y, Chang C-S, Chen J-T, Lee W-Y, Lee H-C (2005) A stainless steel sheath for endoscopic surgery and its application in surgical evacuation of putaminal haemorrhage. J Clin Neurosci 12(8):937–940
Cho D-Y, Chen C-C, Chang C-S, Lee W-Y, Tso M (2006) Endoscopic surgery for spontaneous basal ganglia hemorrhage: comparing endoscopic surgery, stereotactic aspiration, and craniotomy in noncomatose patients. Surg Neurol 65(6):547–555, discussion 555–556
Delcourt C, Huang Y, Arima H, Chalmers J, Davis SM, Heeley EL, Wang J, Parsons MW, Liu G, Anderson CS (2012) Hematoma growth and outcomes in intracerebral hemorrhage: the INTERACT1 study. Neurology 79(4):314–319
Delgado Almandoz JE, Yoo AJ, Stone MJ, Schaefer PW, Goldstein JN, Rosand J, Oleinik A, Lev MH, Gonzalez RG, Romero JM (2009) Systematic characterization of the computed tomography angiography spot sign in primary intracerebral hemorrhage identifies patients at highest risk for hematoma expansion: the spot sign score. Stroke 40(9):2994–3000
Dennis MS (2003) Outcome after brain haemorrhage. Cerebrovasc Dis 16(Suppl 1):9–13
Dye JA, Dusick JR, Lee DJ, Gonzalez NR, Martin NA (2012) Frontal bur hole through an eyebrow incision for image-guided endoscopic evacuation of spontaneous intracerebral hemorrhage. J Neurosurg 117(4):767–773
Elliott J, Smith M (2010) The acute management of intracerebral hemorrhage: a clinical review. Anesth Analg 110(5):1419–1427
Gingrich MB, Junge CE, Lyuboslavsky P, Traynelis SF (2000) Potentiation of NMDA receptor function by the serine protease thrombin. J Neurosci 20(12):4582–4595
Hsieh P-C, Cho D-Y, Lee W-Y, Chen J-T (2005) Endoscopic evacuation of putaminal hemorrhage: how to improve the efficiency of hematoma evacuation. Surg Neurol 64(2):147–153, discussion 153
Klatsky AL, Friedman GD, Sidney S, Kipp H, Kubo A, Armstrong MA (2005) Risk of hemorrhagic stroke in Asian American ethnic groups. Neuroepidemiology 25(1):26–31
Kuo L-T, Chen C-M, Li C-H, Tsai J-C, Chiu H-C, Liu L-C, Tu Y-K, Huang AP-H (2011) Early endoscope-assisted hematoma evacuation in patients with supratentorial intracerebral hemorrhage: case selection, surgical technique, and long-term results. Neurosurg Focus 30(4):E9
Lopez Valdes E, Hernandez Lain A, Calandre L, Grau M, Cabello A, Gomez-Escalonilla C (2000) Time window for clinical effectiveness of mass evacuation in a rat balloon model mimicking an intraparenchymatous hematoma. J Neurol Sci 174(1):40–46
Mayer SA, Sacco RL, Shi T, Mohr JP (1994) Neurologic deterioration in noncomatose patients with supratentorial intracerebral hemorrhage. Neurology 44(8):1379–1384
Mendelow AD, Gregson BA, Fernandes HM, Murray GD, Teasdale GM, Hope DT, Karimi A, Shaw MDM, Barer DH (2005) Early surgery versus initial conservative treatment in patients with spontaneous supratentorial intracerebral haematomas in the International Surgical Trial in Intracerebral Haemorrhage (STICH): a randomised trial. Lancet 365(9457):387–397
Mendelow AD, Gregson BA, Rowan EN, Murray GD, Gholkar A, Mitchell PM, Investigators STICHII (2013) Early surgery versus initial conservative treatment in patients with spontaneous supratentorial lobar intracerebral haematomas (STICH II): a randomised trial. Lancet 382(9890):397–408
Mendelow AD, Unterberg A (2007) Surgical treatment of intracerebral haemorrhage. Curr Opin Crit Care 13(2):169–174
Miller CM, Vespa P, Saver JL et al (2008) Image-guided endoscopic evacuation of spontaneous intracerebral hemorrhage. Surg Neurol 69(5):441–446, discussion 446
Morgenstern LB, Hemphill JC 3rd, Anderson C et al (2010) Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 41(9):2108–2129
Nagasaka T, Inao S, Ikeda H, Tsugeno M, Okamoto T (2008) Inflation-deflation method for endoscopic evacuation of intracerebral haematoma. Acta Neurochir (Wien) 150(7):685–690, discussion 690
Nagasaka T, Tsugeno M, Ikeda H, Okamoto T, Inao S, Wakabayashi T (2011) Early recovery and better evacuation rate in neuroendoscopic surgery for spontaneous intracerebral hemorrhage using a multifunctional cannula: preliminary study in comparison with craniotomy. J Stroke Cerebrovasc Dis 20(3):208–213
Nagasaka T, Tsugeno M, Ikeda H, Okamoto T, Takagawa Y, Inao S, Wakabayashi T (2009) Balanced irrigation-suction technique with a multifunctional suction cannula and its application for intraoperative hemorrhage in endoscopic evacuation of intracerebral hematomas: technical note. Neurosurgery 65(4):E826–827, discussion E827
Nakano T, Ohkuma H, Ebina K, Suzuki S (2003) Neuroendoscopic surgery for intracerebral haemorrhage—comparison with traditional therapies. Minim Invasive Neurosurg 46(5):278–283
Nishihara T, Morita A, Teraoka A, Kirino T (2007) Endoscopy-guided removal of spontaneous intracerebral hemorrhage: comparison with computer tomography-guided stereotactic evacuation. Childs Nerv Syst 23(6):677–683
Nishihara T, Nagata K, Tanaka S, Suzuki Y, Izumi M, Mochizuki Y, Akabane A, Ochiai C (2005) Newly developed endoscopic instruments for the removal of intracerebral hematoma. Neurocrit Care 2(1):67–74
Nishihara T, Teraoka A, Morita A, Ueki K, Takai K, Kirino T (2000) A transparent sheath for endoscopic surgery and its application in surgical evacuation of spontaneous intracerebral hematomas. Technical note. J Neurosurg 92(6):1053–1055
Ochalski P, Chivukula S, Shin S, Prevedello D, Engh J (2013) Outcomes after endoscopic port surgery for spontaneous intracerebral hematomas. J Neurol Surg A Cent Eur Neurosurg. doi:10.1055/s-0033-1348348
Orakcioglu B, Becker K, Sakowitz OW, Herweh C, Köhrmann M, Huttner HB, Steiner T, Unterberg A, Schellinger PD (2008) MRI of the perihemorrhagic zone in a rat ICH model: effect of hematoma evacuation. Neurocrit Care 8(3):448–455
Orakcioglu B, Uozumi Y, Unterberg A (2011) Endoscopic intra-hematomal evacuation of intracerebral hematomas - a suitable technique for patients with coagulopathies. Acta Neurochir Suppl 112:3–8
Patil CG, Alexander AL, Gephart MGH, Lad SP, Arrigo RT, Boakye M (2011) A population based study of inpatient outcomes after operative management of non-traumatic intracerebral hemorrhage in the United States. World Neurosurg. doi:10.1016/j.wneu.2011.10.042
Prasad K, Mendelow AD, Gregson B (2008) Surgery for primary supratentorial intracerebral haemorrhage. Cochrane Database Syst Rev (4):CD000200
Rincon F, Mayer SA (2004) Novel therapies for intracerebral hemorrhage. Curr Opin Crit Care 10(2):94–100
Samadani U, Rohde V (2009) A review of stereotaxy and lysis for intracranial hemorrhage. Neurosurg Rev 32(1):15–21, discussion 21–22
Schellinger PD, Fiebach JB, Hoffmann K et al (2003) Stroke MRI in intracerebral hemorrhage: is there a perihemorrhagic penumbra? Stroke 34(7):1674–1679
Shen AY-J, Yao JF, Brar SS, Jorgensen MB, Chen W (2007) Racial/ethnic differences in the risk of intracranial hemorrhage among patients with atrial fibrillation. J Am Coll Cardiol 50(4):309–315
Silva Y, Leira R, Tejada J, Lainez JM, Castillo J, Dávalos A (2005) Molecular signatures of vascular injury are associated with early growth of intracerebral hemorrhage. Stroke 36(1):86–91
Steiner T, Bösel J (2010) Options to restrict hematoma expansion after spontaneous intracerebral hemorrhage. Stroke 41(2):402–409
Turrentine FE, Wang H, Simpson VB, Jones RS (2006) Surgical risk factors, morbidity, and mortality in elderly patients. J Am Coll Surg 203(6):865–877
Upadhyay UM, Golby AJ (2008) Role of pre- and intraoperative imaging and neuronavigation in neurosurgery. Expert Rev Med Devices 5(1):65–73
Waran V, Vairavan N, Sia SF, Abdullah B (2009) A new expandable cannula system for endoscopic evacuation of intraparenchymal hemorrhages. J Neurosurg 111(6):1127–1130
Wong GKC, Siu DYW, Abrigo JM, Poon WS, Tsang FCP, Zhu XL, Yu SCH, Ahuja AT (2011) Computed tomographic angiography and venography for young or nonhypertensive patients with acute spontaneous intracerebral hemorrhage. Stroke 42(1):211–213
Xi G, Fewel ME, Hua Y, Thompson BG Jr, Hoff JT, Keep RF (2004) Intracerebral hemorrhage: pathophysiology and therapy. Neurocrit Care 1(1):5–18
Yamamoto T, Nakao Y, Mori K, Maeda M (2006) Endoscopic hematoma evacuation for hypertensive cerebellar hemorrhage. Minim Invasive Neurosurg 49(3):173–178
Zan X, Li H, Liu W, Fang Y, Ma J, Lan Z, Li X, Liu X, You C (2012) Endoscopic surgery versus conservative treatment for the moderate-volume hematoma in spontaneous basal ganglia hemorrhage (ECMOH): study protocol for a randomized controlled trial. BMC Neurol 12(1):34
Zhu H, Wang Z, Shi W (2012) Keyhole endoscopic hematoma evacuation in patients. Turk Neurosurg 22(3):294–299
Acknowledgments
We thank Dr. T. Nagasaka (Nagoya University Graduate School of Medicine, Aichi, Japan) for introducing the endoscopic balanced irrigation-suction technique with a multifunctional suction cannula to the Department of Neurosurgery at Heidelberg University Hospital.
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
Waleed A. Azab, New York, USA
The manuscript by Dr. Beynon and colleagues deals with a relatively underutilized modality of surgical evacuation of spontaneous ICH. With the recent technical innovations like endoscopic transparent sheaths and irrigation-suction devices, endoscopic ICH evacuation is becoming technically more feasible. In a patient subpopulation where a short operating time and a limited yet effective procedure are evidently beneficial, endoscopic ICH evacuation seems to hold a great promise.
Michael Buchfelder, Erlangen, Germany
In this review, the authors discuss the current possibilities and limitations of endoscopic minimally invasive endoscopic surgery for spontaneous intracerebral haematomas. Whether surgical evacuation of spontaneous intracerebral haematomas at all causes an improvement of patient outcome in terms of mortality and neurological outcome and if so, which patients will profit from such an operation is an ongoing matter of controversy. During the last 30 years, gradually minimally invasive techniques, utilizing endoscopes, have been developed for haematoma evacuation that largely avoids major brain manipulation and retraction. This started with individual case report and expanded to small series.
There are several technical variations and implementation of additional technology such as neuronavigation, ultrasonic aspiration, guiding tubes and other gadgets, which are excellently described in this review. Their utility is discussed as is the usefulness of the operation as far as the clinical outcome is concerned.
Even the most sceptical reader will appreciate knowledge the availability and experience hitherto gained with this novel technique. For the final evaluation of its value for clinical practice, it seems to me that further studies, which include numerous patients, are awaited.
Yavor Enchev, Varna, Bulgaria
Currently, the treatment of spontaneous intracerebral haematomas (ICH) is controversial with respect to indications, timing, surgical techniques, and applied instruments and devices. Neuroendoscopy and neuronavigation have been proved their potential, effectiveness, reliability and advantages in most of the neurosurgical pathologies. Reasonably, similar results could be expected in the treatment of ICH. The authors thoroughly reviewed the published experience in this field. They discuss the rationales of the minimal invasive endoscopic evacuation of ICH, the existed technical directions and nuances, including their own experience, and the achieved outcomes. This rigorous and systematic review outlines the future trends of the pertinent research and the need of controlled clinical trials.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(MPG 46 mb)
Rights and permissions
About this article
Cite this article
Beynon, C., Schiebel, P., Bösel, J. et al. Minimally invasive endoscopic surgery for treatment of spontaneous intracerebral haematomas. Neurosurg Rev 38, 421–428 (2015). https://doi.org/10.1007/s10143-015-0606-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-015-0606-6