Abstract
Purpose
We sought to determine the test characteristics of biliary point-of-care ultrasound (POCUS) and to assess the usefulness of obtaining radiology ultrasound (RUS) or cholescintigraphy (HIDA) after biliary POCUS.
Methods
We conducted a retrospective review of emergency department patients who underwent biliary POCUS between May 4, 2018 and November 28, 2021. To be included, patients had to have at least one of the following confirmatory evaluations (considered in this order): surgery, HIDA, RUS, or abdominal CT scan. When a discrepancy existed between the POCUS and the RUS or HIDA, they were compared to a higher criterion standard (if available).
Results
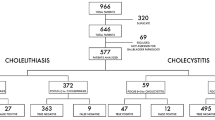
Using 348 patients who had a confirmatory evaluation after biliary POCUS, we found the sensitivity and specificity of biliary POCUS for gallstones to be 97.0% (95% CI 92.6 to 99.2%) and 99.5% (95% CI 97.3 to 100%), respectively. For cholecystitis, the sensitivity and specificity were 83.8% (95% CI 72.9 to 91.6%) and 98.6% (95% CI 96.4 to 99.6%), respectively. RUS and POCUS were concordant in 72 (81.8%) of 88 cases in which the patient had both studies while HIDA and POCUS were concordant in 24 (70.6%) of 34 cases. POCUS was deemed correct in at least 50% of discrepant cases with RUS and at least 30% of discrepant cases with HIDA.
Conclusion
Biliary POCUS has excellent sensitivity and specificity for cholelithiasis; it has lower sensitivity for cholecystitis, but the specificity remains high. Performing a confirmatory RUS or cholescintigraphy after a positive biliary POCUS adds little value, but additional imaging may be useful when POCUS is negative for cholecystitis.


Similar content being viewed by others
References
Everhart JE, Khare M, Hill M, Maurer KR (1999) Prevalence and ethnic differences in gallbladder disease in the United States. Gastroenterology 117:632–639. https://doi.org/10.1016/s0016-5085(99)70456-7
Chatziioannou SN, Moore WH, Ford PV, Dhekne RD (2000) Hepatobiliary scintigraphy is superior to abdominal ultrasonography in suspected acute cholecystitis. Surgery 127:609–613. https://doi.org/10.1067/msy.2000.105868
Kiewiet JJ, Leeuwenburgh MM, Bipat S, Bossuyt PM, Stoker J, Boermeester MA (2012) A systematic review and meta-analysis of diagnostic performance of imaging in acute cholecystitis. Radiology 264(3):708. https://doi.org/10.1148/radiol.12111561
American College of Emergency Physicians (2020) Gallbladder. Sonoguide. Available at https://www.acep.org/sonoguide/basic/gallbladder/ Accessed November 29, 2021.
Expert Panel on Gastrointestinal Imaging: Peterson CM, McNamara MM, Kamel IR, Al-Refaie WB, Arif-Tiwari H et al (2019) ACR appropriateness criteria right upper quadrant pain. J Am Coll Radiol 16(5S):S235–S243. https://doi.org/10.1016/j.jacr.2019.02.013
Pereira J, Bass GA, Mariani D, Dumbrava BD, Casamassima A, da Silva AR et al (2020) Surgeon-performed point-of-care ultrasound for acute cholecystitis: indications and limitations: a European Society for Trauma and Emergency Surgery (ESTES) consensus statement. Eur J Trauma Emerg Surg 46(1):173–183. https://doi.org/10.1007/s00068-019-01197-z
Kendall JL, Shimp RJ (2001) Performance and interpretation of focused right upper quadrant ultrasound by emergency physicians. J Emerg Med 21:7–13. https://doi.org/10.1016/s0736-4679(01)00329-8
Kozaci N, Avci M, Tulubas G, Ararat E, Karakoyun OF, Karaman C et al (2018) Role of emergency physician-performed ultrasound in the differential diagnosis of abdominal pain. Hong Kong J Emerg Med 27:79–86
Miller AH, Pepe PE, Brockman CR, Delaney KA (2006) ED ultrasound in hepatobiliary disease. J Emerg Med 30:69–74. https://doi.org/10.1016/j.jemermed.2005.03.017
Dupriez F, Geukens P, Penaloza A, Vanpee D, Bekkering G, Bobbia X (2021) Agreement of emergency physician-performed ultrasound versus RADiology-performed UltraSound for cholelithiasis or cholecystitis: a systematic review. Eur J Emerg Med 28(5):344–351. https://doi.org/10.1097/MEJ.0000000000000815
Ross M, Brown M, McLaughlin K, Atkinson P, Thompson J, Powelson S et al (2011) Emergency physician-performed ultrasound to diagnose cholelithiasis: a systematic review. Acad Emerg Med 18:227–235. https://doi.org/10.1111/j.1553-2712.2011.01012.x
Summers SM, Scruggs W, Menchine MD, Lahham S, Anderson C, Amr O et al (2010) A prospective evaluation of emergency department bedside ultrasonography for the detection of acute cholecystitis. Ann Emerg Med 56:114–122. https://doi.org/10.1016/j.annemergmed.2010.01.014
Sharif S, Vlahaki D, Skitch S, Truong J, Freeman S, Sidalak D, Healey A (2021) Evaluating the diagnostic accuracy of point-of-care ultrasound for cholelithiasis and cholecystitis in a canadian emergency department. CJEM 23(5):626–630. https://doi.org/10.1007/s43678-020-00068-6
Koichopolos J, Hilsden R, Myslik F, Thompson D, Vandelinde J, Leeper R (2020) Surgeon attitudes toward point of care ultrasound for biliary disease: a nationwide Canadian survey. Can J Surg 63(1):E9–E12. https://doi.org/10.1503/cjs.010218
Ultrasound guidelines: emergency, point-of-care and clinical ultrasound guidelines in medicine. (2017) Ann Emerg Med 69 (5): e27–254.
Harvey RT, Miller WT Jr (1999) Acute biliary disease: initial CT and follow-up US versus initial US and follow-up CT. Radiology 213(3):831–836. https://doi.org/10.1148/radiology.213.3.r99dc17831
Hilsden R, Leeper R, Koichopolos J, Vandelinde JD, Parry N, Thompson D, Myslik F (2018) Point-of-care biliary ultrasound in the emergency department (BUSED): implications for surgical referral and emergency department wait times. Trauma Surg Acute Care Open 3(1):e000164. https://doi.org/10.1136/tsaco-2018-000164.eCollection
Amini R, Adhikari S, Fiorello A (2014) Ultrasound competency assessment in emergency medicine residency programs. Acad Emerg Med 21(7):799–801. https://doi.org/10.1111/acem.12408
Shea JA, Berlin JA, Escarce JJ, Clarke JR, Kinosian BP, Cabana MD et al (1994) Revised estimates of diagnostic test sensitivity and specificity in suspected biliary tract disease. Arch Intern Med 154(22):2573–2581
Kaoutzanis C, Davies E, Leichtle SW, Welch KB, Winter S, Lampman RM, Arneson W (2014) Abdominal ultrasound versus hepato-imino diacetic acid scan in diagnosing acute cholecystitis–what is the real benefit? J Surg Res 188(1):44–52
Hiatt KD, Ou JJ, Childs DD (2020) Role of ultrasound and CT in the workup of right upper quadrant pain in adults in the emergency department: a retrospective review of more than 2800 cases. AJR Am J Roentgenol 214(6):1305–1310
Fagenholz PJ, Fuentes E, Kaafarani H, Cropano C, King D, de Moya M (2015) Computed tomography is more sensitive than ultrasound for the diagnosis of acute cholecystitis. Surg Infect (Larchmt) 16(5):509–512. https://doi.org/10.1089/sur.2015.102
Wertz JR, Lopez JM, Olson D, Thompson WM (2018) Comparing the diagnostic accuracy of ultrasound and CT in evaluating acute cholecystitis. AJR Am J Roentgenol 211(2):W92–W97
Martellotto S, Dohan A, Pocard M (2020) Evaluation of the CT scan as the first examination for the diagnosis and therapeutic strategy for acute cholecystitis. World J Surg 44(6):1779–1789
Chang JH et al (2011) Role of magnetic resonance cholagiopancreatography for choledocholithiasis: analysis of patient with negative MRCP. Scand J Gastroenterol 47(2):217–224
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zitek, T., Fernandez, S., Newberry, M.A. et al. The use of additional imaging studies after biliary point-of-care ultrasound in the emergency department. Emerg Radiol 30, 19–26 (2023). https://doi.org/10.1007/s10140-022-02095-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-022-02095-5