Abstract
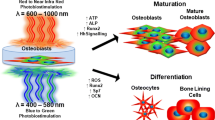
Photobiomodulation (PBM) is a non-invasive treatment that uses laser or led devices making its effects a response to light and not to heat. The possibility of accelerating dental implant osteointegration and orthodontic movements and the need to treat refractory bone lesions, such as bisphosphonate related osteonecrosis of the jaws, has led researchers to consider the effects of PBM on bone for dentistry purposes. The aim of our study was to investigate the effects of 915 nm light supplied with a GaAs diode laser on human osteoblasts in vitro. Osteoblasts were isolated from mandibular cortical bone of a young healthy donor. The irradiation parameters were as follows: doses = 5, 15 and 45 J/cm2; power densities = 0.12 and 1.25 W/cm2; and irradiation times = 41.7, 125 and 375 s. We performed one irradiation per day for 3 and 6 days to study proliferation and differentiation, respectively. Microscopic analysis showed a greater amount of bone nodules in samples treated with 5 J/cm2 and 0.12 W/cm2 compared to controls (56.00 ± 10.44 vs 19.67 ± 7.64, P = 0.0075). Cell growth and quantification of calcium deposition did not show any differences when comparing irradiated and non-irradiated samples. Photobiomodulation, with the parameters investigated in the present study, positively modulated the mineralization process in human osteoblasts, inducing the formation of a greater amount of bone nodules, but did not increase cell proliferation.




Similar content being viewed by others
References
Mester E (1966) The use of the laser beam in therapy. Orv Hetil 107:1012–1016
Karu T (1999) Primary and secondary mechanisms of action of visible to near-IR radiation on cells. J Photochem Photobiol B Biol 49:1–17
Khadra M, Lyngstadaas SP, Haanaes HR, Mustafa K (2005) Effect of laser therapy on attachment, proliferation and differentiation of human osteoblast-like cells cultured on titanium implant material. Biomaterials 26:3503–3509
Walsh LJ (1997) The current status of low level laser therapy in dentistry. Part 1. Soft tissue applications. Aust Dent J 42:247–254
Walsh LJ (1997) The current status of low level laser therapy in dentistry. Part 2. Hard tissue applications. Aust Dent J 42:302–306
Huang YY, Sharma SK, Carroll J, Hamblin MR (2011) Biphasic dose response in low level light therapy—an update. Dose Response 9:602–618
Heymann PGB, Ziebart T, Kammerer PW et al (2016) The enhancing effect of a laser photochemotherapy with cisplatin or zolendronic acid in primary human osteoblasts and osteosarcoma cells in vitro. J Oral Pathol Med 45:803–809
Karoussis IK, Kyriakidou K, Psarros C, Lang NP, Vrotsos IA (2017) Nd:YAG laser radiation (1.064 nm) accelerates differentiation of osteoblasts to osteocytes on smooth and rough titanium surfaces in vitro. Clin Oral Implants Res 28:785–790
Oliveira FA, Matos AA, Santesso MR et al (2016) Low intensity lasers differently induce primary human osteoblast proliferation and differentiation. J Photochem Photobiol B Biol 163:14–21
Crisan L, Soritau O, Baciut M, Baciut G, Crisan BV (2015) The influence of laser radiation on human osteoblasts cultured on nanostructured composite substrates. Clujul Med 88:224–232
Stein A, Benayahu D, Maltz L, Oron U (2005) Low-level laser irradiation promotes proliferation and differentiation of human osteoblasts in vitro. Photomed Laser Surg 23:161–166
Ueda Y, Shimizu N (2003) Effects of pulse frequency of low-level laser therapy (LLLT) on bone nodule formation in rat calvarial cells. J Clin Laser Med Surg 21:271–277
Tschon M, Incerti Parenti S, Cepollaro S, Checchi L, Fini M (2015) Photobiomodulation with low-level diode laser promotes osteoblast migration in an in vitro micro wound model. J Biomed Opt 20:078002–078010
Asai T, Suzuki H, Kitayama M et al (2014) The long-term effects of red light-emitting diode irradiation on the proliferation and differentiation of osteoblast-like MC3T3-E1 cells. Kobe J Med Sci 60:E12–E18
Migliario M, Pittarella P, Fanuli M, Rizzi M, Renò F (2014) Laser-induced osteoblast proliferation is mediated by ROS production. Lasers Med Sci 29:1463–1467
Incerti Parenti S, Checchi L, Fini M, Tschon M (2014) Different doses of low-level laser irradiation modulate the in vitro response of osteoblast-like cells. J Biomed Opt 19:108002–108007
Kanenari M, Zhao J, Abiko Y (2011) Enhancement of microtubule-associated protein-1 alpha gene expression in osteoblasts by low level laser irradiation. Laser Ther 20:47–51
Kiyosaki T, Mitsui N, Suzuki N, Shimizu N (2010) Low-level laser therapy stimulates mineralization via increased Runx2 expression and ERK phosphorylation in osteoblasts. Photomed Laser Surg 28(Suppl 1):S167–S172
Hirata S, Kitamura C, Kukushima H et al (2010) Low-level laser irradiation enhances BMP-induced osteoblast differentiation by stimulating the BMP/Smad signaling pathway. J Cell Biochem 111:1445–1452
Shimizu N, Mayahara K, Kiyosaki T et al (2007) Low-intensity laser irradiation stimulates bone nodule formation via insulin-like growth factor-I expression in rat calvarial cells. Lasers Surg Med 39:551–559
Hamajima S, Hiratsuka K, Kiyama-Kishikawa M et al (2003) Effect of low-level laser irradiation on osteoglycin gene expression in osteoblasts. Lasers Med Sci 18:78–82
Yamamoto M, Tamura K, Hiratsuka K, Abiko Y (2001) Stimulation of MCM3 gene expression in osteoblast by low level laser irradiation. Lasers Med Sci 16:213–217
Huang TH, Lu YC, Kao CT (2012) Low-level diode laser therapy reduces lipopolysaccharide (LPS)-induced bone cell inflammation. Lasers Med Sci 27:621–627
Bayat M, Virdi A, Rezaei F, Chien S (2017) Comparison of the in vitro effects of low-level laser therapy and low-intensity pulsed ultrasound therapy on bony cells and stem cells. Progress Biophys Molec Biol 1–13
Beresford JN, Gallagher JA, Gowen M et al (1984) The effects of monocyte-conditioned medium and interleukin 1 on the synthesis of collagenous and non-collagenous proteins by mouse bone and human bone cells in vitro. Biochim Biophys Acta 801:58–65
Gregory CA, Gunn WG, Peister A, Prockop DJ (2004) An alizarin red-based assay of mineralization by adherent cells in culture: comparison with cetylpyridinium chloride extraction. Anal Biochem 329:77–84
Kaur G, Dufour JM (2012) Cell lines: valuable tools or useless artifacts. Spermatogenesis 2:1–5
Incerti Parenti S, Panseri S, Gracco A et al (2013) Effect of low-level laser irradiation on osteoblast-like cells cultured on porous hydroxyapatite scaffolds. Ann Ist Super Sanita 49:255–260
Stein E, Koehn J, Sutter W et al (2008) Initial effects of low-level laser therapy on growth and differentiation of human osteoblast-like cells. Wien Klin Wochenschr 120:112–117
Renno ACM, McDonnell PA, Parizotto NA, Laakso E-L (2007) The effects of laser irradiation on osteoblast and osteosarcoma cell proliferation and differentiation in vitro. Photomed Laser Surg 25:275–280
Pagin MT, de Oliveira FA, Oliveira RC et al (2014) Laser and light-emitting diode effects on pre-osteoblast growth and differentiation. Lasers Med Sci 29:55–59
Fujihara NA, Hiraki KRN, Marques MM (2006) Irradiation at 780 nm increases proliferation rate of osteoblasts independently of dexamethasone presence. Lasers Surg Med 38:332–336
Ozawa Y, Shimizu N, Kariya G, Abiko Y (1998) Low-energy laser irradiation stimulates bone nodule formation at early stages of cell culture in rat calvarial cells. Bone 22:347–354
Bloise N, Ceccarelli G, Minzioni P et al (2013) Investigation of low-level laser therapy potentiality on proliferation and differentiation of human osteoblast-like cells in the absence/presence of osteogenic factors. J Biomed Opt 18:128006
Tang W, Tian J, Zheng Q et al (2015) Implantable self-powered low-level laser cure system for mouse embryonic osteoblasts’ proliferation and differentiation. ACS Nano 9:7867–7873
Saracino S, Mozzati M, Martinasso G et al (2009) Superpulsed laser irradiation increases osteoblast activity via modulation of bone morphogenetic factors. Lasers Surg Med 41:298–304
Kim IS, Cho TH, Kim K, Weber FE, Hwang SJ (2010) High power-pulsed Nd:YAG laser as a new stimulus to induce BMP-2 expression in MC3T3-E1 osteoblasts. Lasers Surg Med 42:510–518
Belletti S, Uggeri J, Mergoni G et al (2015) Effects of 915 nm GaAs diode laser on mitochondria of human dermal fibroblasts: analysis with confocal microscopy. Lasers Med Sci 30:375–381
Tunér J, Hode L (2004) The laser therapy handbook. Prima Books, Grängesberg
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Mergoni, G., Vescovi, P., Belletti, S. et al. Effects of 915 nm laser irradiation on human osteoblasts: a preliminary in vitro study. Lasers Med Sci 33, 1189–1195 (2018). https://doi.org/10.1007/s10103-018-2453-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-018-2453-5