Abstract
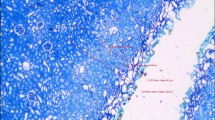
Since the diode laser is a good compromise for the daily use in dental offices, finding usage in numerous dental indications (e.g., surgery, periodontics, and endodontics), the minimization of the collateral damage in laser surgery is important to improve the therapeutical outcome. The aim of this study was to investigate the effect of water/air cooling on the collateral thermal soft tissue damage of 980-nm diode laser incisions. A total of 36 mechanically executed laser cuts in pork liver were made with a 980-nm diode laser in micropulsed mode with three different settings of water/air cooling and examined by histological assessment to determine the area and size of carbonization, necrosis, and reversible tissue damage as well as incision depth and width. In our study, clearly the incision depth increased significantly under water/air cooling (270.9 versus 502.3 μm—test group 3) without significant changes of incision width. In test group 2, the total area of damage was significantly smaller than in the control group (in this group, the incision depth increases by 65 %). In test group 3, the total area of damage was significantly higher (incision depth increased by 85 %), but the bigger part of it represented a reversible tissue alteration leaving the amount of irreversible damage almost the same as in the control group. This first pilot study clearly shows that water/air cooling in vitro has an effect on collateral tissue damage. Further studies will have to verify, if the reduced collateral damage we have proved in this study can lead to accelerated wound healing. Reduction of collateral thermal damage after diode laser incisions is clinically relevant for promoted wound healing.




Similar content being viewed by others
References
Parker S (2007) Lasers and soft tissue: ‘loose’ soft tissue surgery. Br Dent J 202(4):185–191
Sulieman M (2005) An overview of the use of lasers in general dental practice: 1. Laser physics and tissue interactions. Dent Update 32:228–230, 233–4, 236
Scherer H et al (1994) Current status of laser surgery in the area of the soft palate and adjoining regions. Laryngorhinootologie 73(1):14–20
Luciano AA, Frishman GN, Maier DB (1992) A comparative analysis of adhesion reduction, tissue effects, and incising characteristics of electrosurgery, CO2 laser, and Nd:YAG laser at operative laparoscopy: an animal study. J Laparoendosc Surg 2(6):287–292
Jin J-Y, Lee S-H, Yoon H-J (2010) A comparative study of wound healing following incision with a scalpel, diode laser or Er, Cr:YSGG laser in guinea pig oral mucosa: a histological and immunohistochemical analysis. Acta Odontol Scand 68(4):232–238
Tipton WW, Garrick JG, Riggins RS (1975) Healing of electrosurgical and scalpel wounds in rabbits. J Bone Joint Surg Am 57(3):377–379
D’Arcangelo C et al (2007) A preliminary study of healing of diode laser versus scalpel incisions in rat oral tissue: a comparison of clinical, histological, and immunohistochemical results. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103(6):764–773
Burns JA et al (2007) Thermal damage during thulium laser dissection of laryngeal soft tissue is reduced with air cooling: ex vivo calf model study. Ann Otol Rhinol Laryngol 116(11):853–857
Lian HJ, Lan WH, Lin CP (1996) The effects of cooling systems on CO2-lased human enamel. J Clin Laser Med Surg 14(6):381–384
Cercadillo-Ibarguren I et al (2010) Histologic evaluation of thermal damage produced on soft tissues by CO2, Er, Cr:YSGG and diode lasers. Med Oral Patol Oral Cir Bucal 15(6):e912–e918
Hoke JA et al (1990) Erbium:YAG (2.94 mum) laser effects on dental tissues. J Laser Appl 2(3–4):61–65
Moritz A et al (1998) Treatment of periodontal pockets with a diode laser. Lasers Surg Med 22(5):302–311
Moritz A et al (1997) Irradiation of infected root canals with a diode laser in vivo: results of microbiological examinations. Lasers Surg Med 21(3):221–226
Cafaro A et al (2010) Effect of low-level laser irradiation on unresponsive oral lichen planus: early preliminary results in 13 patients. Photomed Laser Surg 28(Suppl 2):S99–S103
Goharkhay K et al (2009) Frequency doubled neodymium:yttrium–aluminum–garnet and diode laser-activated power bleaching—pH, environmental scanning electron microscopy, and colorimetric in vitro evaluations. Lasers Med Sci 24(3):339–346
Romanos G, Nentwig GH (1999) Diode laser (980 nm) in oral and maxillofacial surgical procedures: clinical observations based on clinical applications. J Clin Laser Med Surg 17(5):193–197
Beer F, Passow H (2008) Construction of a standard test assembly for controlled laser studies in tissues: preliminary study on human bone material. Rev Sci Instrum 79(2 Pt 1):024301
Goharkhay K et al (1999) Effects on oral soft tissue produced by a diode laser in vitro. Lasers Surg Med 25(5):401–406
Beer F et al (2011) Reduction of collateral thermal impact of diode laser irradiation on soft tissue due to modified application parameters. Lasers Med Sci 27(5):917–921
Stübinger S et al (2006) Soft tissue surgery with the diode laser–theoretical and clinical aspects. Schweiz Monatsschr Zahnmed 116(8):812–820
Polanyi TG (1983) Laser physics. Otolaryngol Clin North Am 16(4):753–774
Bar-Am A et al (1993) High- and low-power CO2 lasers. Comparison of results for three clinical indications. J Reprod Med 38(6):455–458
Fitzpatrick RE, Ruiz-Esparza J, Goldman MP (1991) The depth of thermal necrosis using the CO2 laser: a comparison of the superpulsed mode and conventional mode. J Dermatol Surg Oncol 17(4):340–344
Iaria G (2008) Clinical, morphological, and ultrastructural aspects with the use of Er:YAG and Er, Cr:YSGG lasers in restorative dentistry. Gen Dent 56(7):636–639
Matcher SJ et al (1995) Performance comparison of several published tissue near-infrared spectroscopy algorithms. Anal Biochem 227(1):54–68
Matcher SJ, Cope M, Delpy DT (1994) Use of the water absorption spectrum to quantify tissue chromophore concentration changes in near-infrared spectroscopy. Phys Med Biol 39(1):177–196
Zwart A et al (1981) A multi-wavelength spectrophotometric method for the simultaneous determination of five haemoglobin derivatives. J Clin Chem Clin Biochem 19(7):457–463
van Assendelft OW (1970) Spectrophotometry of haemoglobin derivatives. Charles C. Thomas, Springfield
Horecker BL (1943) The absorption spectra of hemoglobin and its derivatives in the visible and near infra-red regions. J Biol Behm 148:173–183
Angiero F et al (2012) Diode laser (808 nm) applied to oral soft tissue lesions: a retrospective study to assess histopathological diagnosis and evaluate physical damage. Lasers Med Sci 27(2):383–388
Bohnert M et al (2008) Re-oxygenation of haemoglobin in livores after post-mortem exposure to a cold environment. Int J Legal Med 122(2):91–96
Niemz M (1996) Laser tissue interactions. Springer, Berlin
Conflict of interest
The authors declare that they have no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beer, F., Körpert, W., Buchmair, A.G. et al. The influence of water/air cooling on collateral tissue damage using a diode laser with an innovative pulse design (micropulsed mode)—an in vitro study. Lasers Med Sci 28, 965–971 (2013). https://doi.org/10.1007/s10103-012-1186-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-012-1186-0