Abstract
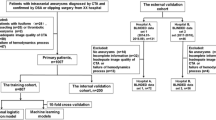
Estimating whether to treat the rupture risk of small intracranial aneurysms (IAs) with size ≤ 7 mm in diameter is difficult but crucial. We aimed to construct and externally validate a convenient machine learning (ML) model for assessing the rupture risk of small IAs. One thousand four patients with small IAs recruited from two hospitals were included in our retrospective research. The patients at hospital 1 were stratified into training (70%) and internal validation set (30%) randomly, and the patients at hospital 2 were used for external validation. We selected predictive features using the least absolute shrinkage and selection operator (LASSO) method and constructed five ML models applying diverse algorithms including random forest classifier (RFC), categorical boosting (CatBoost), support vector machine (SVM) with linear kernel, light gradient boosting machine (LightGBM), and extreme gradient boosting (XGBoost). The Shapley Additive Explanations (SHAP) analysis provided interpretation for the best ML model. The training, internal, and external validation cohorts included 658, 282, and 64 IAs, respectively. The best performance was presented by SVM as AUC of 0.817 in the internal [95% confidence interval (CI), 0.769–0.866] and 0.893 in the external (95% CI, 0.808–0.979) validation cohorts, which overperformed compared with the PHASES score significantly (all P < 0.001). SHAP analysis showed maximum size, location, and irregular shape were the top three important features to predict rupture. Our SVM model based on readily accessible features presented satisfying ability of discrimination in predicting the rupture IAs with small size. Morphological parameters made important contributions to prediction result.



Similar content being viewed by others
References
Wiebers DO, Whisnant JP, Huston J 3rd, Meissner I, Brown RD Jr, Piepgras DG, Forbes GS, Thielen K, Nichols D, O’Fallon WM, Peacock J, Jaeger L, Kassell NF, Kongable-Beckman GL, Torner JC, & International Study of Unruptured Intracranial Aneurysms Investigators (2003) Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet (London, England) 362(9378):103–110. https://doi.org/10.1016/s0140-6736(03)13860-3
Macdonald RL, Schweizer TA (2017) Spontaneous subarachnoid haemorrhage. Lancet (London, England) 389(10069):655–666. https://doi.org/10.1016/S0140-6736(16)30668-7
Malhotra A, Wu X, Forman HP, Grossetta Nardini HK, Matouk CC, Gandhi D, Moore C, Sanelli P (2017) Growth and rupture risk of small unruptured intracranial aneurysms: a systematic review. Ann Intern Med 167(1):26–33. https://doi.org/10.7326/M17-0246
Bender MT, Wendt H, Monarch T, Beaty N, Lin LM, Huang J, Coon A, Tamargo RJ, Colby GP (2018) Small aneurysms account for the majority and increasing percentage of aneurysmal subarachnoid hemorrhage: A 25-year, single institution study. Neurosurg 83(4):692–699. https://doi.org/10.1093/neuros/nyx484
Greving JP, Wermer MJ, Brown RD Jr, Morita A, Juvela S, Yonekura M, Ishibashi T, Torner JC, Nakayama T, Rinkel GJ, Algra A (2014) Development of the PHASES score for prediction of risk of rupture of intracranial aneurysms: a pooled analysis of six prospective cohort studies. Lancet Neurol 13(1):59–66. https://doi.org/10.1016/S1474-4422(13)70263-1
Japan Investigators UCAS, Morita A, Kirino T, Hashi K, Aoki N, Fukuhara S, Hashimoto N, Nakayama T, Sakai M, Teramoto A, Tominari S, Yoshimoto T (2012) The natural course of unruptured cerebral aneurysms in a Japanese cohort. N Engl J Med 366(26):2474–2482. https://doi.org/10.1056/NEJMoa1113260
Kataoka K, Taneda M, Asai T, Yamada Y (2000) Difference in nature of ruptured and unruptured cerebral aneurysms. Lancet (London, England) 355(9199):203. https://doi.org/10.1016/S0140-6736(99)03881-7
Senders JT, Arnaout O, Karhade AV, Dasenbrock HH, Gormley WB, Broekman ML, Smith TR (2018) Natural and artificial intelligence in neurosurgery: a systematic review. Neurosurg 83(2):181–192. https://doi.org/10.1093/neuros/nyx384
Ngiam KY, Khor IW (2019) Big data and machine learning algorithms for health-care delivery. Lancet Oncol 20(5):e262–e273. https://doi.org/10.1016/S1470-2045(19)30149-4
Liu J, Chen Y, Lan L, Lin B, Chen W, Wang M, Li R, Yang Y, Zhao B, Hu Z, Duan Y (2018) Prediction of rupture risk in anterior communicating artery aneurysms with a feed-forward artificial neural network. Eur Radiol 28(8):3268–3275. https://doi.org/10.1007/s00330-017-5300-3
Heo J, Park SJ, Kang SH, Oh CW, Bang JS, Kim T (2020) Prediction of intracranial aneurysm risk using machine learning. Sci Rep 10(1):6921. https://doi.org/10.1038/s41598-020-63906-8
Shalabi LA, Shaaban Z, Kasasbeh B (2006) Data mining: a preprocessing engine. J Comput Sci 2:735–739. https://doi.org/10.3844/jcssp.2006.735.739
Okada S, Ohzeki M, Taguchi S (2019) Efficient partition of integer optimization problems with one-hot encoding. Sci Rep 9(1):13036. https://doi.org/10.1038/s41598-019-49539-6
Tibshirani R (2011) Regression shrinkage and selection via the Lasso: a retrospective. J R Statist Soc B 73:273–282. https://doi.org/10.1111/j.1467-9868.2011.00771.x
Saeys Y, Inza I, Larrañaga P (2007) A review of feature selection techniques in bioinformatics. Bioinformatics (Oxford, England) 23(19):2507–2517. https://doi.org/10.1093/bioinformatics/btm344
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44(3):837–845
Ruopp MD, Perkins NJ, Whitcomb BW, Schisterman EF (2008) Youden Index and optimal cut-point estimated from observations affected by a lower limit of detection. Biometric j Biometrische Zeitschrift 50(3):419–430. https://doi.org/10.1002/bimj.200710415
Rodríguez-Pérez R, Bajorath J (2020) Interpretation of compound activity predictions from complex machine learning models using local approximations and Shapley values. J Med Chem 63(16):8761–8777. https://doi.org/10.1021/acs.jmedchem.9b01101
Liu Q, Jiang P, Jiang Y, Ge H, Li S, Jin H, Li Y (2019) Prediction of aneurysm stability using a machine learning model based on pyradiomics-derived morphological features. Stroke 50(9):2314–2321. https://doi.org/10.1161/STROKEAHA.119.025777
Shi Z, Chen GZ, Mao L, Li XL, Zhou CS, Xia S, Zhang YX, Zhang B, Hu B, Lu GM, Zhang LJ (2021) Machine learning-based prediction of small intracranial aneurysm rupture status using CTA-derived hemodynamics: a multicenter study. AJNR Am J Neuroradiol 42(4):648–654. https://doi.org/10.3174/ajnr.A7034
Kim HC, Rhim JK, Ahn JH, Park JJ, Moon JU, Hong EP, Kim MR, Kim SG, Lee SH, Jeong JH, Choi SW, Jeon JP (2019) Machine learning application for rupture risk assessment in small-sized intracranial aneurysm. J Clin Med 8(5):683. https://doi.org/10.3390/jcm8050683
Ahn JH, Kim HC, Rhim JK, Park JJ, Sigmund D, Park MC, Jeong JH, Jeon JP (2021) Multi-view convolutional neural networks in rupture risk assessment of small, unruptured intracranial aneurysms. J pers med 11(4):239. https://doi.org/10.3390/jpm11040239
Ikawa F, Morita A, Tominari S, Nakayama T, Shiokawa Y, Date I, Nozaki K, Miyamoto S, Kayama T, Arai H, & Japan Neurosurgical Society for UCAS Japan Investigators (2019) Rupture risk of small unruptured cerebral aneurysms. J neurosurg 1–10. Advance online publication. https://doi.org/10.3171/2018.9.JNS181736
Lindgren AE, Koivisto T, Björkman J, von Und Zu, Fraunberg M, Helin K, Jääskeläinen JE, Frösen J (2016) Irregular shape of intracranial aneurysm indicates rupture risk irrespective of size in a population-based cohort. Stroke 47(5):1219–1226. https://doi.org/10.1161/STROKEAHA.115.012404
Rousseau O, Karakachoff M, Gaignard A, Bellanger L, Bijlenga P, Constant DitBeaufils P, L'Allinec V, Levrier O, Aguettaz P, Desilles JP, Michelozzi C, Marnat G, Vion AC, Loirand G, Desal H, Redon R, Gourraud PA, Bourcier R, & ICAN Investigators (2021) Location of intracranial aneurysms is the main factor associated with rupture in the ICAN population. J neurol, neurosurg psychiatry 92(2): 122–128. https://doi.org/10.1136/jnnp-2020-324371
Tada Y, Wada K, Shimada K, Makino H, Liang EI, Murakami S, Kudo M, Kitazato KT, Nagahiro S, Hashimoto T (2014) Roles of hypertension in the rupture of intracranial aneurysms. Stroke 45(2):579–586. https://doi.org/10.1161/STROKEAHA.113.003072
Lindgren AE, Kurki MI, Riihinen A, Koivisto T, Ronkainen A, Rinne J, Hernesniemi J, Eriksson JG, Jääskeläinen JE & von und zu Fraunberg M. (2014) Hypertension predisposes to the formation of saccular intracranial aneurysms in 467 unruptured and 1053 ruptured patients in Eastern Finland. Annals of medicine 46(3): 169–176. https://doi.org/10.3109/07853890.2014.883168
Can A, Castro VM, Yu S, Dligach D, Finan S, Gainer VS, Shadick NA, Savova G, Murphy S, Cai T, Weiss ST, Du R (2018) Antihyperglycemic agents are inversely associated with intracranial aneurysm rupture. Stroke 49(1):34–39. https://doi.org/10.1161/STROKEAHA.117.019249
Song J, Shin YS (2016) Diabetes may affect intracranial aneurysm stabilization in older patients: analysis based on intraoperative findings. Surg Neurol Int 7(Suppl 14):S391–S397. https://doi.org/10.4103/2152-7806.183497
Skodvin TØ, Johnsen LH, Gjertsen Ø, Isaksen JG, Sorteberg A (2017) Cerebral aneurysm morphology before and after rupture: nationwide case series of 29 aneurysms. Stroke 48(4):880–886. https://doi.org/10.1161/STROKEAHA.116.015288
Koffijberg H, Buskens E, Algra A, Wermer MJ, Rinkel GJ (2008) Growth rates of intracranial aneurysms: exploring constancy. J Neurosurg 109(2):176–185. https://doi.org/10.3171/JNS/2008/109/8/0176
Funding
This study was funded by the Special Scientific Research Fund Project of Jiangsu Research Hospital Association — Precisely Drug use — CSPC Pharmaceutical Group Co., Ltd. [grant number JY202001]; Nanjing Pharmaceutical Association — Changzhou Siyao — Hospital Pharmaceutical Research Fund [grant number 2021YX014]; National Natural Science Foundation of China [grant number 82173899].
Author information
Authors and Affiliations
Contributions
JJZ, HWF, and ZZH conceived and designed the study. WGX, TTC, and JL contributed equally to this work. WGX, TTC, and JL conducted the literature review. TTC performed data analysis. WGX drafted the manuscript. LX, CZ, LiX, YBL, and DC collected the data. YZW, QJ, RZQ, and ZYX polished this article. All the authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Ethical approval
The ethics committee of Hunan Provincial People's Hospital has approved this study ([2015]-10) and waived the requirement of written informed consent.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xiong, W., Chen, T., Li, J. et al. Interpretable machine learning model to predict rupture of small intracranial aneurysms and facilitate clinical decision. Neurol Sci 43, 6371–6379 (2022). https://doi.org/10.1007/s10072-022-06351-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-06351-x