Abstract
Background
Activities of daily living (ADL) are fundamental skills required to independently care for oneself and are categorized in basic (BADLs) and instrumental (IADLs) activities of daily living. ADL evaluation is of paramount importance in clinical practice to discriminate between healthy individuals (HC) and patients with mild cognitive impairment (MCI) or Alzheimer’s disease (AD). However, it is unclear whether and to what extent BADL and IADL deficits occur in MCI, when compared with AD. Therefore, the present study aimed at comparing performance on both BADLs and IADLs in HC, MCI, and AD.
Methods
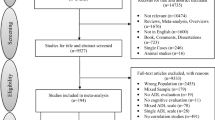
Three electronic databases were consulted for studies comparing total BADLs/IADLs, and single BADLs/IADLs in AD, MCI, and HC (comparisons: AD versus MCI, AD versus HC, MCI versus HC). Ninety-six studies were included in the meta-analysis with random effect models (Hedges’ g). Meta-regression was performed to evaluate the effect of clinical variables on ESs.
Results
AD group had more difficulties in BADLs and IADLs than HC and MCI groups; people with MCI showed more difficulties in both IADLs and BADLs than HC. The meta-regression analysis revealed that the percentage of males in the samples was a significant predictor of the ES in the meta-analysis comparing total BADL scores between MCI and HC; in the comparison between AD and HC, age at evaluation predicted the ES on some single IADLs: preparing food, handling medication, and finances.
Conclusions
In MCI, it should be considered not only a decline of IADLs but also subtle decline of BADL abilities.



Similar content being viewed by others
References
Cornelis E, Gorus E, Van Schelvergem N, De Vriendt P (2019) The relationship between basic, instrumental, and advanced activities of daily living and executive functioning in geriatric patients with neurocognitive disorders. Int J Geriatr Psychiatry 34:889–899. https://doi.org/10.1002/gps.5087
Stuck AE, Walthert JM, Nikolaus T, Büla CJ, Hohmann C, Beck JC (1999) Risk factors for functional status decline in community-living elderly people: a systematic literature review. Soc Sci Med 48:445–469. https://doi.org/10.1016/s0277-9536(98)00370-0
Reisberg B, Finkel S, Overall J, Schmidt-Gollas N, Kanowski S, Lehfeld H, Hulla F, Sclan SG, Wilms HU, Heininger K, Hindmarch I, Stemmler M, Poon L, Kluger A, Cooler C, Bergener M, Hugonot-Diener L, Robert PH, Antipolis S, Erzigkeit H (2001) The Alzheimer’s disease activities of daily living international scale (ADL-IS). Int Psychogeriatr 13:163–181. https://doi.org/10.1017/s1041610201007566
Katz S, Ford AB, Moskowitz RW, Jackson BA, Jaffe MW (1963) Studies of illness in the aged. The index of ADL: a standardized measure of biological and psychosocial function. JAMA 185:914–919. https://doi.org/10.1001/jama.1963.03060120024016
Bucks RS, Ashworth DL, Wilcock GK, Siegfried K (1996) Assessment of activities of daily living in dementia: development of the Bristol Activities of Daily Living Scale. Age Ageing 25:113–120. https://doi.org/10.1093/ageing/25.2.113
Hindmarch I, Lehfeld H, de Jongh P, Erzigkeit H (1998) The Bayer Activities of Daily Living Scale (B-ADL). Dement Geriatr Cogn Disord 9(Suppl 2):20–26. https://doi.org/10.1159/000051195
Wade DT, Collin C (1988) The Barthel ADL Index: a standard measure of physical disability? Int Disabil Stud 10:64–67. https://doi.org/10.3109/09638288809164105
Lawton MP, Brody EM (1969) Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 9:179–186
Ku HM, Kim JH, Lee HS, Ko HJ, Kwon EJ, Jo S, Kim DK (2004) A study on the reliability and validity of Seoul-Activities of Daily Living (S-ADL). Ann Geriatr Med Res 8:206–214
Pfeffer RI, Kurosaki TT, Harrah CHJ, Chance JM, Filos S (1982) Measurement of functional activities in older adults in the community. J Gerontol 37:323–329. https://doi.org/10.1093/geronj/37.3.323
Gauthier S, Gélinas I, Gauthier L (1997) Functional disability in Alzheimer’s disease. Int Psychogeriatr 9(Suppl 1):163–165. https://doi.org/10.1017/s1041610297004857
Galasko D, Bennett DA, Sano M, Marson D, Kaye J, Edland SD (2006) ADCS Prevention Instrument Project: assessment of instrumental activities of daily living for community-dwelling elderly individuals in dementia prevention clinical trials. Alzheimer Dis Assoc Disord 20:S152–S169. https://doi.org/10.1097/01.wad.0000213873.25053.2b
De Paula JJ, Bertola L, de Ávila RT, de O Assis L, Albuquerque M, Bicalho MA, de Moraes EN, Nicolato R, Malloy-Diniz LF (2014) Development, validity, and reliability of the General Activities of Daily Living Scale: a multidimensional measure of activities of daily living for older people. Braz J Psychiatry 36:143–152. https://doi.org/10.1590/1516-4446-2012-1003
McKhann GM, Knopman DS, Chertkow H, Hyman BT, Jack CRJ, Kawas CH, Klunk WE, Koroshetz WJ, Manly JJ, Mayeux R, Mohs RC, Morris JC, Rossor MN, Scheltens P, Carrillo MC, Thies B, Weintraub S, Phelps CH (2011) The diagnosis of dementia due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement 7:263–269. https://doi.org/10.1016/j.jalz.2011.03.005
De Vriendt P, Gorus E, Cornelis E, Bautmans I, Petrovic M, Mets T (2013) The advanced activities of daily living: a tool allowing the evaluation of subtle functional decline in mild cognitive impairment. J Nutr Health Aging 17:64–71. https://doi.org/10.1007/s12603-012-0381-9
Wadley VG, Crowe M, Marsiske M, Cook SE, Unverzagt FW, Rosenberg AL, Rexroth D (2007) Changes in everyday function in individuals with psychometrically defined mild cognitive impairment in the Advanced Cognitive Training for Independent and Vital Elderly Study. J Am Geriatr Soc 55:1192–1198. https://doi.org/10.1111/j.1532-5415.2007.01245.x
Allaire JC, Gamaldo A, Ayotte BJ, Sims R, Whitfield K (2009) Mild cognitive impairment and objective instrumental everyday functioning: the everyday cognition battery memory test. J Am Geriatr Soc 57:120–125. https://doi.org/10.1111/j.1532-5415.2008.02054.x
Malinowsky C, Almkvist O, Nygård L, Kottorp A (2012) Individual variability and environmental characteristics influence older adults’ abilities to manage everyday technology. Int Psychogeriatr 24:484–495. https://doi.org/10.1017/S1041610211002092
Boeve B, McCormick J, Smith G, Ferman T, Rummans T, Carpenter T, Ivnik R, Kokmen E, Tangalos E, Edland S, Knopman D, Petersen R (2003) Mild cognitive impairment in the oldest old. Neurology 60:477–480. https://doi.org/10.1212/wnl.60.3.477
Reppermund S, Brodaty H, Crawford JD, Kochan NA, Draper B, Slavin MJ, Trollor JN, Sachdev PS (2013) Impairment in instrumental activities of daily living with high cognitive demand is an early marker of mild cognitive impairment: the Sydney memory and ageing study. Psychol Med 43:2437–2445. https://doi.org/10.1017/S003329171200308X
Ahn S, Kim J, Koo B, Kim Y (2019) Evaluation of inertial sensor-based pre-impact fall detection algorithms using public dataset. Sensors (Basel) 19. https://doi.org/10.3390/s19040774
Weston A, Barton C, Lesselyong J, Yaffe K (2011) Functional deficits among patients with mild cognitive impairment. Alzheimers Dement 7:611–614. https://doi.org/10.1016/j.jalz.2010.12.011
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Borenstein M, Hedges LV, Higgins JPT, Rothstein HR (2010) A basic introduction to fixed-effect and random-effects models for meta-analysis. Res Synth Methods 1:97–111. https://doi.org/10.1002/jrsm.12
Shi L, Lin L (2019) The trim-and-fill method for publication bias: practical guidelines and recommendations based on a large database of meta-analyses. Medicine (Baltimore) 98:e15987. https://doi.org/10.1097/MD.0000000000015987
Charernboon T, Lerthattasilp T (2016) Characteristic profiles of activities of daily living and relationship with cognitive performance in thai elderly with different stages from normal cognitive function, mild cognitive impairment to dementia. Null 39:307–323. https://doi.org/10.1080/07317115.2016.1162893
Peng G-P, Feng Z, He F-P, Chen Z-Q, Liu X-Y, Liu P, Luo B-Y (2015) Correlation of hippocampal volume and cognitive performances in patients with either mild cognitive impairment or Alzheimer’s disease. CNS Neurosci Ther 21:15–22. https://doi.org/10.1111/cns.12317
Lee M-T, Jang Y, Chang W-Y (2019) How do impairments in cognitive functions affect activities of daily living functions in older adults? PLoS One 14:e0218112. https://doi.org/10.1371/journal.pone.0218112
Pereira FS, Oliveira AM, Diniz BS, Forlenza OV, Yassuda MS (2010) Cross-cultural adaptation, reliability and validity of the DAFS-R in a sample of Brazilian older adults. Arch Clin Neuropsychol 25:335–343. https://doi.org/10.1093/arclin/acq029
Shin K-R, Kang Y, Kim M, Jung D, Kim M (2012) Comparative study between depression in Korean elderly with mild cognitive impairment and normal cognitive function. Nurs Health Sci 14:81–86. https://doi.org/10.1111/j.1442-2018.2011.00666.x
Desai AK, Grossberg GT, Sheth DN (2004) Activities of daily living in patients with dementia: clinical relevance, methods of assessment and effects of treatment. CNS Drugs 18:853–875. https://doi.org/10.2165/00023210-200418130-00003
Petersen RC (2004) Mild cognitive impairment as a diagnostic entity. J Intern Med 256:183–194. https://doi.org/10.1111/j.1365-2796.2004.01388.x
Schmitter-Edgecombe M, Woo E, Greeley DR (2009) Characterizing multiple memory deficits and their relation to everyday functioning in individuals with mild cognitive impairment. Neuropsychology 23:168–177. https://doi.org/10.1037/a0014186
Yeh Y-C, Lin K-N, Chen W-T, Lin C-Y, Chen T-B, Wang P-N (2011) Functional disability profiles in amnestic mild cognitive impairment. Dement Geriatr Cogn Disord 31:225–232. https://doi.org/10.1159/000326910
Rebok GW, Ball K, Guey LT, Jones RN, Kim H-Y, King JW, Marsiske M, Morris JN, Tennstedt SL, Unverzagt FW, Willis SL (2014) Ten-year effects of the advanced cognitive training for independent and vital elderly cognitive training trial on cognition and everyday functioning in older adults. J Am Geriatr Soc 62:16–24. https://doi.org/10.1111/jgs.12607
Alnajjar F, Khalid S, Vogan AA, Shimoda S, Nouchi R, Kawashima R (2019) Emerging cognitive intervention technologies to meet the needs of an aging population: a systematic review. Front Aging Neurosci 11:291. https://doi.org/10.3389/fnagi.2019.00291
Mancioppi G, Fiorini L, Timpano Sportiello M, Cavallo F (2019) Novel technological solutions for assessment, treatment, and assistance in mild cognitive impairment. Front Neuroinform 13:58. https://doi.org/10.3389/fninf.2019.00058
Seelye SA, Smith ASA, Schmitter-Edgecombe M (2010) Cueing technologies for assisting persons with mild cognitive impairment in instrumental activity of daily living completion in an experimenter-assisted smart apartment environment. Arch Clin Neuropsychol 25:481–482
Wu Y-H, Cristancho-Lacroix V, Fassert C, Faucounau V, de Rotrou J, Rigaud A-S (2016) The attitudes and perceptions of older adults with mild cognitive impairment toward an assistive robot. J Appl Gerontol 35:3–17. https://doi.org/10.1177/0733464813515092
Bédard M, Kuzik R, Chambers L, Molloy DW, Dubois S, Lever JA (2005) Understanding burden differences between men and women caregivers: the contribution of care-recipient problem behaviors. Int Psychogeriatr 17:99–118. https://doi.org/10.1017/s1041610204000857
Murman DL (2015) The impact of age on cognition. Semin Hear 36:111–121. https://doi.org/10.1055/s-0035-1555115
Zhang Y, Jia H, Li A, Liu J, Li H (2016) Study on prediction of activities of daily living of the aged people based on longitudinal data. Proc Comput Sci 91:470–477. https://doi.org/10.1016/j.procs.2016.07.122
Marshall GA, Amariglio RE, Sperling RA, Rentz DM (2012) Activities of daily living: where do they fit in the diagnosis of Alzheimer’s disease? Neurogener Dis Manag 2:483–491. https://doi.org/10.2217/nmt.12.55
Acknowledgements
The authors would like to thank Dr. Alessandro Micillo for the graphical elaboration of the study figures.
Author information
Authors and Affiliations
Contributions
Study concept: GS. Study design: MA, FG, and GS. Literature searching and initial records screening: MA and FG. Data extraction and interpretation: MA, FG, and GS. Manuscript preparation: MA, FG, and GS. Critical revision of manuscript: MA, FG, and GS.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The present meta-analytic study is exempt from ethical approval as the study authors collected and synthesized data from primary studies retrieved from public databases.
Informed consent
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Altieri, M., Garramone, F. & Santangelo, G. Functional autonomy in dementia of the Alzheimer’s type, mild cognitive impairment, and healthy aging: a meta-analysis. Neurol Sci 42, 1773–1783 (2021). https://doi.org/10.1007/s10072-021-05142-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05142-0