Abstract
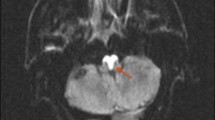
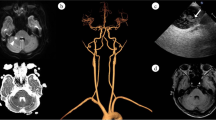
Diaphragmatic palsy after acute stroke is a novel clinical entity and may result in a high incidence of respiratory dysfunction and pneumonia, which especially cause greater morbidity and mortality. Generally, internal capsule and complete middle cerebral artery (MCA) infarctions are major risk-factors for developing diaphragmatic palsy. Herein, we present a case with contralateral diaphragmatic palsy after a subcortical MCA infarction without capsular involvement. Dyspnea occurred after stroke, while a chest X-ray and CT study disclosed an elevated right hemidiaphragm without significant infiltration or patch of pneumonia. A phrenic nerve conduction study showed bilateral mild prolonged onset-latency without any significant right–left difference. This suggested a lesion causing diaphragmatic palsy was not in the phrenic nerve itself, but could possibly originate from an above central location (subcortical MCA infarction). We also discussed the role of transcranial magnetic stimulation study in the survey of central pathway and demonstrated diaphragmatic palsy-related orthopnea.



Similar content being viewed by others
References
Lloyd-Jones D, Adams R, Carnethon M, De Simone G, Ferguson TB, Flegal K et al (2009) Heart disease and stroke statistics–2009 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 119:480–486
Weimar C, Roth MP, Zillessen G, Glahn J, Wimmer ML, Busse O et al (2002) Complications following acute ischemic stroke. Eur Neurol 48:133–140
Tirschwell DL, Kukull WA, Longstreth WT Jr (1999) Medical complications of ischemic stroke and length of hospital stay: experience in Seattle, Washington. J Stroke Cerebrovasc Dis 8:336–343
Santamaria J, Ruiz C (1988) Diaphragmatic elevation in stroke. Eur Neurol 28:81–83
Similowski T, Catala M, Rancurel G, Derenne JP (1996) Impairment of central motor conduction to the diaphragm in stroke. Am J Respir Crit Care Med 154:436–441
Khedr EM, El Shinawy O, Khedr T, Abdel aziz ali Y, Awad EM (2000) Assessment of cortico-diaphragmatic pathway and pulmonary function in acute ischemic stroke patients. Eur J Neurol 7:509–516
Kumar S, Reddy R, Prabhakar S (2009) Contralateral diaphragmatic palsy in acute stroke: An interesting observation. Indian J Crit Care Med 13:28–30
Raichle ME, Plum F (1972) Hyperventilation and cerebral blood flow. Stroke 3:566–575
Elefteriades J, Singh M, Tang P, Siegel MD, Kenney B, Pandey A et al (2008) Unilateral diaphragm paralysis: etiology, impact, and natural history. J Cardiovasc Surg (Torino) 49:289–295
Urban PP, Morgenstern M, Brause K, Wicht S, Vukurevic G, Kessler S et al (2002) Distribution and course of cortico-respiratory projections for voluntary activation in man. A transcranial magnetic stimulation study in healthy subjects and patients with cerebral ischemia. J Neurol 249:735–744
Katzan IL, Cebul RD, Husak SH, Dawson NV, Baker DW (2003) The effect of pneumonia on mortality among patients hospitalized for acute stroke. Neurology 60:620–625
Maskill D, Murphy K, Mier A, Owen M, Guz A (1991) Motor cortical representation of the diaphragm in man. J Physiol 443:105–121
Nakayama T, Fujii Y, Suzuki K, Kanazawa I, Nakada T (2004) The primary motor area for voluntary diaphragmatic motion identified by high field fMRI. J Neurol 251:730–735
Colebatch JG, Adams L, Murphy K, Martin AJ, Lammertsma AA, Tochon-Danguy HJ et al (1991) Regional cerebral blood flow during volitional breathing in man. J Physiol 443:91–103
Khedr EM, Trakhan MN (2001) Localization of diaphragm motor cortical representation and determination of cortico-diaphragmatic latencies by using magnetic stimulation in normal adult human subjects. Eur J Appl Physiol 85:560–566
Swenson MR, Rubenstein RS (1992) Phrenic nerve conduction studies. Muscle Nerve 15:597–603
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wu, MN., Chen, PN., Lai, CL. et al. Contralateral diaphragmatic palsy after subcortical middle cerebral artery infarction without capsular involvement. Neurol Sci 32, 487–490 (2011). https://doi.org/10.1007/s10072-011-0501-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-011-0501-z