Abstract
Background
A better understanding of the epidemiological profile of systemic sclerosis (SSc) in Thais could improve care, human resource deployment, and public health budgeting.
Objectives
We aimed to determine the incidence and prevalence of SSc in Thailand between 2017 and 2020.
Methods
A descriptive epidemiological study was performed using the Information and Communication Technology Center, Ministry of Public Health database, comprising all types of healthcare providers during the study period. Demographic data of patients having a primary diagnosis of M34 systemic sclerosis and over 18 years of age between 2017 and 2020 were reviewed. The incidence and prevalence of SSc were calculated as well as their respective 95% confidence intervals (CIs).
Results
The number of SSc cases in 2017 was 15,920 from a total Thai population of 65,204,797. The prevalence of SSc in 2017 was 24.4 per 100,000 populations (95% CI 24.0–24.8). The prevalence of SSc among women was 2 times greater than among men (32.7 vs. 15.8 per 100,000). The incidence of SSc was stable from 2018 to 2019 but dropped slightly in 2020 (7.2, 7.6, and 6.8 per 100,000 person-years, respectively). Most SSc cases were in northeastern Thailand (11.6, 12.1, and 11.1 per 100,000 person-years from 2018 to 2020, respectively) and the peak was between 60 and 69 years of age (24.6, 23.8, and 20.9 per 100,000 person-years from 2018 to 2020, respectively).
Conclusion
SSc is a rare disease among Thais. The disease was commonly revealed in late middle-aged women with a peak at age 60–69 years, mainly from the northeast regions. The incidence remained stable during the study period, albeit during the emergence of the coronavirus pandemic a slight decline was recorded.
Key Points • The incidence and prevalence of systemic sclerosis (SSc) vary across ethnic populations. • There is a lack of epidemiology research of SSc since the 2013 ACR/EULAR Classification Criteria for Scleroderma was adopted among Thais included Asia-Pacific population as the population has some different clinical features than those reported among Caucasians. • SSc is a rare connective disease among Thais and commonly presents in late middle-aged group of both genders, mainly in Thailand's northern and northeastern regions. • When compare to the epidemiology of SSc in Asia-Pacific, the prevalence of SSc in Thais was higher than among East Asians and the Indian population and the incidence of SSc among Thais was greater than the other Asia-Pacific population including Australian. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Systemic sclerosis (SSc) is a rare disease that typically leads to skin thickness and internal organ fibrosis. The incidence and prevalence of SSc vary across ethnic populations [1]. A review of the incidence from 39 studies and the prevalence from 61 studies revealed that the respective global pooled incidence and prevalence for SSc are 1.4 per 100,000 person-years (95% CI 1.1–1.9) and 17.6 per 100,000 (95% CI 15.1–20.5) [1]. North America has higher estimates of SSc than other continents, and women are 5 times more frequently affected than men [1]. However, the study included the incidence and prevalence before using the 2013 American Rheumatism Association (ACR)/The European Alliance of Associations for Rheumatology (EULAR) Classification Criteria for Scleroderma [2], which is more sensitive and more specific [3] for diagnosing SSc than the previous 1980 American Rheumatism Association classification criteria of SSc [4], LeRoy and Medsger 2011 [5], and the 2011 Preliminary Criteria for the Very Early Diagnosis of Systemic Sclerosis [6]. There has been no study on the incidence and prevalence of SSc since 2013. ACR/EULAR Classification Criteria for Scleroderma was adopted for use in the Thai population. A population-specific study is needed as the Thai population has some different clinical features than those reported among Caucasians and some Asians [7,8,9,10,11,12,13,14,15,16,17]. We thus aimed to determine the incidence, prevalence, and distribution of SSc in Thailand between 2017 and 2020, thereby creating an epidemiological profile of SSc among Thais and helping to plan better care, workforce needs, and public health budgets.
Methods
A descriptive epidemiological study was conducted among adult SSc patients over 18 with a primary diagnosis of M34 systemic sclerosis between 2017 and 2020.
Information resources and statistical analysis
The study was performed using the Information and Communication Technology Center, Ministry of Public Health database, which comprises healthcare paid for by (i) the National Health Security Office (NHSO); (ii) the Civil Servants Benefit System from the Comptroller General’s Department; (iii) the Social Security Office; and (iv) self-payment. The databases are derived from a collection of data submitted by hospitals. Data were gathered from nearly all hospitals in Thailand, including patients who visited private hospitals but not private clinics and some university hospitals in the central region. The diagnosis was coded using the International Classification of Diseases, Tenth Revision (ICD-10). The epidemiologic data of the patients with a primary diagnosis of M34 systemic sclerosis between 2017 and 2020 were extracted and reviewed. The data included age, gender, year of visit, hospital name, Amphoe (municipal district), and province. The duplicated data was removed. The incidence and cumulative incidence of SSc were analyzed, including the respective 95% confidence interval (CI). The data included an overall national and regional perspective (viz., the northern, eastern, northeastern, southern, and central regions). The population data for calculating disease prevalence was from the National Statistical Office of Thailand [18]. The categorical data were presented as numbers and percentages, while the continuous data were presented as means and standard deviations (SDs). All data analyses were performed using STATA version 16.0 (StataCorp., College Station, TX, USA) [19].
Results
According to the Information and Communication Technology Center, Ministry of Public Health database, 30,063 cases had a primary diagnosis of M34 systemic sclerosis between 2017 and 2020. The female-to-male ratio was 2:1. The number of SSc in 2017 was 15,920 cases, and the Thai population was 65,204,797 including 31,966,108 men and 33,238,689 women. Therefore, the prevalence of SSc in 2017 was 24.4 per 100,000 populations (95% CI 24.0–24.8). The respective numbers of SSc in 2017 in Thai women and men were 10,873 and 5047 cases, with prevalences of 32.7 per 100,000 (95% CI 32.1–33.3) and 15.8 per 100,000 (95% CI 15.4–16.2).
The number of new cases of SSc and total Thai population stratified by year is presented in Table 1 and the incidence of SSc stratified by year is presented in Table 2. The incidence of SSc in Thailand trended to be stable between 2018 and 2019 and slightly decreased in 2020. However, the incidence among Thai women was higher than among Thai men. The respective cumulative incidences of SSc in 2019 and 2020 were 14.8 per 100,000 person-years (95% CI 14.5–15.1) and 21.6 per 100,000 person-years (95% CI 21.3–22.0).
The overall mean age of the prevalence cases in 2017 was 59.7 ± 13.3 years which was comparable with the mean age of the incidence case in 2018 to 2020. Of those incidence cases of SSc between 2018 and 2020, the highest cases were revealed in the 60 and 69 age groups. The findings were similar across the 3-year period (Table 1).
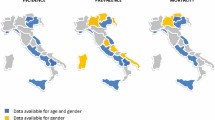
According to the number of SSc per 100,000 based on hospital-based patient visits, the highest number of patients in 2017 was in the northeastern region (8814 cases; 55.4%), followed by the northern region (3252 cases; 20.4%) (Fig. 1A). The new cases of SSc, 2547 cases (54.2%) in 2018 (Fig. 1B), 2650 cases (53.2%) in 2019 (Fig. 1C), and 2435 cases (54.6%) in 2020 (Fig. 1D), were found mainly in the north region, mostly in Prae province, with the incidences of 36.6, 35.5, and 38.0 per 100,000 person-years, respectively. The second highest incidence of SSc in Thailand was in Nan province, with incidences of 34.2, 32.4, and 21.6 per 100,000 person-years in 2018, 2019, and 2020, respectively. While the highest incidence of SSc in the northeastern region was in Ubon Ratchathani province (24.4, 31.0, and 26.6 per 100,000 person-years in 2018, 2019, and 2020, respectively), it was followed by Khon Kaen province (with respective incidences in 2018, 2019, and 2020 of 24.4, 28.5, and 24.9 per 100,000 person-years). Few cases were reported in the western, southern, and eastern regions, albeit new cases were reported in the eastern province of Trat in 2019 (57 cases; 24.8%) and 2020 (51 cases; 22.3%).
Number of SSc per 100,000 population by hospital-based of visit (QGIS software version 3.8.2: an open source and free software of geographic data system information was used for generating the maps; https://www.qgis.org/en/site/). A Number of SSc in 2017 (prevalence cases). B Number of new cases of SSc in 2018 (incidence cases). C Number of new cases of SSc in 2019 (incidence cases). D Number of new cases of SSc in 2020 (incidence cases)
Discussion
This study reported the epidemiology of SSc in Thailand, including the National Information and Communication Technology Center, the Ministry of Public Health database that covers all healthcare providers. Most Thais receive healthcare services at hospitals under the Ministry of Public Health, and their information is recorded during visits to out- and/or in-patient units. The diagnoses between 2017 and 2020 per the ICD code were extracted from the database. Our epidemiologic study explored the prevalence and the incidence of SSc among Thais after the recent adoption of the Classification Criteria for Diagnosis of Early SSc and during the emergence of the COVID-19 pandemic (i.e., early January 2020) [20].
The prevalence of SSc in Thais was 24.4 per 100,000, which was around 3–4 times higher than among East Asians (5.3–7.2 per 100,000) [9, 21, 22] and 2 times higher than in the Indian population (12.0 per 100,000) [23], but comparable to Australian population (20–23 per 100,000) and less than among the Japanese (37 per 100,000) [7, 24]. The incidence of SSc among Thais was 6 times greater than among East Asians [9, 21, 25] (6.8–7.6 per 100,000 person-years vs. 0.7–1.1 per 100,000 person-years) and 3–5 times higher than among the Australian population (1.2–2.3 per 100,000 person-years) [7, 8, 24, 26].
The incidence of SSc was quite similar between the Thais and the Japanese (Table 3) [27]. The findings might be explained by differences in case definitions (ICD coding in ours and the ACR 1980 coding in others), study period, and/or ethnic differences. According to our methods, the study period between 2017 and 2020 was after adoption of the 2013 ACR/EULAR Classification Criteria for diagnosis of early SSc, so that the ICD coding might have been included in the case definition diagnosed in the ACR 1980 or the 2013 ACR/EULAR Classification Criteria for Scleroderma. Notably, the 2013 ACR/EULAR Classification Criteria for Scleroderma has a high sensitivity for the diagnosis of early SSc [3, 28]. The patients with early SSc might have been included in the database, resulting in the high prevalence and incidence of SSc among Thais compared to the studies published before 2013. The epidemiology data among Thais is consistent with Kuwana et al. from Japan [27] and Kim et al. from South Korea, who included patients during the same period [22]. Kim et al. also reported that the prevalence of SSc increased to 34% between 2012 and 2016 in South Korea for a mean annual prevalence change of 0.4 per 100,000 population. The prevalence seemed to gradually increase after adoption of the 2013 ACR/EULAR Classification Criteria for Scleroderma. The findings support our results and help to explain why our prevalence and incidence are higher than the reports from previous decades.
SSc disease affected women more than men. The female-to-male ratio was around 2:1 in Thais, but a higher proportion was revealed in other Asia-Pacific countries (range, 3.5:1–14:1) (Table 3). The higher prevalence of the disease among women was also revealed in other connective tissue diseases (CTD), including systemic lupus erythematosus (SLE) [29, 30], mixed connective tissue disease (MCTD) [29, 31], and primary Sjogren syndrome (SS) in other population [29, 32, 33]. The female-to-male ratio was comparable in patients with systemic vasculitis [29] compared to the overall ratio of female-to-male in SSc, including our data. Unfortunately, there has been no current epidemiologic study of other CTD among Thais; therefore, we cannot conclude whether the proportion of female-to-male Thai SSc patients was comparable to other CTD. We envision a further epidemiological study of Thais vis-à-vis other CTD.
SSc in Thais was commonly found in the late-middle-aged group of both genders (range, 50–69). The number of Thai SSc was highest in those between 60 and 69 years of age (around 27–30% in those 50–59 years of age, and 30–32% in those 60–69 years of age), while < 10% were patients under 40 years of age. The peak age group was comparable to the study of Tamaki et al. from Japan [9], whereas the mean age of SSc among Thais trended higher than among Japanese [9], Taiwanese [21], and Australians [7]. Although the study periods differed from the reports, most SSc patients were still in the late middle-aged group. Interestingly, 15–20% of Thai SSc patients were > 70 years of age. Elderly age is associated with a poor prognosis with shorter median survival than younger persons and adults with SSc [17, 34,35,36,37]. In an aging society, the number of elderly SSc patients may increase, and public health policy and budgets will be needed for complication prevention and close monitoring of disease progression.
We found that there was a higher proportion of SSc in Thai males than in other Asians (Japanese, Chinese, Korean, Iranians, and Indians), Australians, Europeans, and Americans [7, 10,11,12,13,14,15, 38]. The results might be related to the differences in ethnicity and/or genetics among SSc patients, particularly the HLA-gene. HLA-DRB1*1502, DRB5*0102, and DQB1*0501 were genetic susceptibilities for SSc among Thai [39, 40], while HLA-DRB1*0101 and DRB1*0501 were susceptibilities among Japanese, and HLA-DRB1*1104, DQA1*0501, and DQB1*0301 were among Caucasians [41].
SSc was more prevalent, with more incidents in the northeast and northern regions than in the other regions of Thailand. New cases are rarely reported in the western and southern regions of Thailand. When we explored the geographic map and surrounding environment of the area where a high number of new cases of SSc were detected, there are 5 main rivers, including the Yom and Nan Rivers in the northern region and the Nam Phong, Chi, and Mun Rivers in the northeastern region, and in the headwaters of some of the rivers are gold or iron ore mines. Previous data from Foocharoen et al. revealed that air pollution, particularly PM2.5 dust, is associated with hospital mortality among Thai SSc patients [42]. We hypothesize that such pollution might cause pathogenesis among some cases of SSc in Thais. To date, there have been no reports on the quality of water or heavy metal contamination and any association with SSc disease. To test our hypothesis, air pollution evaluation and water quality testing should be conducted.
Genetic susceptibility might be another explanation for the higher number of incidents in the northeast and northern regions. HLA-DRB1*1502 has been identified as a genetic susceptibility to SSc in Thais from both the north and northeast of Thailand. Louthreenoo et al. revealed the association of HLA-DRB1*1502 and DRB5*0102 among Thais with SSc from the northern region of Thailand, [39] while Mahakkanukrauh et al. found that HLA-DRB1*1502 and DQB1*0501 were significantly elevated among SSc from the northeast region of Thailand [40].
Our study had some limitations, including that (a) some university hospitals in the central region were not included in the database; however, we had already included the first visit of all new SSc cases in the analysis from data extracted from local hospitals before referral to a secondary, tertiary center, or university hospitals; (b) we cannot make sure whether all SSc cases in our database were diagnosed by the 2013 ACR/EULAR Classification Criteria or not, despite The 2013 ACR/EULAR Classification Criteria for the diagnosis of SSc is widely used in our countries; (c) the data from literature reviews that reported case definitions using ICD-10 did not mention which criteria were used for the diagnosis of SSc, despite the study period being after the 2013 ACR/EULAR Classification Criteria for SSc was launched. Hence, it was difficult to compare the incidence and prevalence of SSc between our study and the previous database; and (d) the clinical information from the database was limited, and the principal diagnosis in the database was coded according to the ICD-10, which does not provide a specific code for SSc subsets (diffuse cutaneous SSc and limited cutaneous SSc subsets), disease complications, and treatment, so we were not able to provide detailed epidemiology on the SSc subsets, the complication, and the treatment. Notwithstanding, all necessary demographic data were analyzed, and the data were sufficient to complete an overall assessment of the epidemiology of SSc in Thailand. The study strengths were (a) the study was based on an extensive database of SSc patients, thereby ensuring a full suite of epidemiological characteristics of SSc in Thailand, and (b) the results can be generalized to other Southeast Asian and/or Asian-Pacific countries with similar ethnicity and geography.
Conclusions
SSc is a rare connective disease among Thais. The prevalence and incidence are comparable with some Asian populations, particularly the Japanese. The disease commonly presents in Thai women with a peak at age 60–69 years and mainly in Thailand’s northeastern regions. The incidence was steady from 2018 to 2020 but dropped slightly during emergence of coronavirus pandemic.
Data availability
Data and material are available from the corresponding author upon reasonable request.
References
Bairkdar M, Rossides M, Westerlind H et al (2021) Incidence and prevalence of systemic sclerosis globally: a comprehensive systematic review and meta-analysis. Rheumatology (Oxford) 60:3121–3133. https://doi.org/10.1093/rheumatology/keab190
van den Hoogen F, Khanna D, Fransen J et al (2013) Classification criteria for systemic sclerosis: an ACR-EULAR collaborative initiative. Arthritis Rheum 65:2737–2747. https://doi.org/10.1002/art.38098
van den Hoogen F, Khanna D, Fransen J et al (2013) 2013 classification criteria for systemic sclerosis: an American College of Rheumatology/European League against Rheumatism collaborative initiative. Arthritis Rheum 65:2737–2747. https://doi.org/10.1002/art.38098
(1980) Preliminary criteria for the classification of systemic sclerosis (scleroderma). Subcommittee for scleroderma criteria of the American Rheumatism Association Diagnostic and Therapeutic Criteria Committee. Arthritis Rheum 23(5):581–90
LeRoy EC, Medsger TA Jr (2001) Criteria for the classification of early systemic sclerosis. J Rheumatol 28:1573–1576
Avouac J, Fransen J, Walker UA et al (2011) Preliminary criteria for the very early diagnosis of systemic sclerosis: results of a Delphi Consensus Study from EULAR Scleroderma Trials and Research Group. Ann Rheum Dis 70:476–481. https://doi.org/10.1136/ard.2010.136929
Roberts-Thomson PJ, Jones M, Hakendorf P et al (2001) Scleroderma in South Australia: epidemiological observations of possible pathogenic significance. Intern Med J 31:220–229
Englert H, Small-McMahon J, Davis K et al (1999) Systemic sclerosis prevalence and mortality in Sydney 1974-88. Aust N Z J Med 29:42–50
Tamaki T, Mori S, Takehara K (1991) Epidemiological study of patients with systemic sclerosis in Tokyo. Arch Dermatol Res 283:366–371. https://doi.org/10.1007/BF00371817
Geirsson AJ, Steinsson K, Guthmundsson S, Sigurthsson V (1994) Systemic sclerosis in Iceland. A nationwide epidemiological study. Ann Rheum Dis 53:502–505
Hashimoto A, Endo H, Kondo H, Hirohata S (2012) Clinical features of 405 Japanese patients with systemic sclerosis. Mod Rheumatol 22:272–279. https://doi.org/10.1007/s10165-011-0515-7
Poormoghim H, Moghadam AS, Moradi-Lakeh M et al (2013) Systemic sclerosis: demographic, clinical and serological features in 100 Iranian patients. Rheumatol Int 33:1943–1950. https://doi.org/10.1007/s00296-013-2668-5
Ferri C, Valentini G, Cozzi F et al (2002) Systemic sclerosis: demographic, clinical, and serologic features and survival in 1,012 Italian patients. Medicine (Baltimore) 81:139–153
Tyndall A, Mueller-Ladner U, Matucci-Cerinic M (2005) Systemic sclerosis in Europe: first report from the EULAR Scleroderma Trials And Research (EUSTAR) group database. Ann Rheum Dis 64:1107. https://doi.org/10.1136/ard.2005.036038
Delisle VC, Hudson M, Baron M et al (2014) Sex and time to diagnosis in systemic sclerosis: an updated analysis of 1,129 patients from the Canadian scleroderma research group registry. Clin Exp Rheumatol 32 S-10-14
Reveille JD, Fischbach M, McNearney T et al (2001) Systemic sclerosis in 3 US ethnic groups: a comparison of clinical, sociodemographic, serologic, and immunogenetic determinants. Semin Arthritis Rheum 30:332–346. https://doi.org/10.1053/sarh.2001.20268
Foocharoen C, Peansukwech U, Mahakkanukrauh A et al (2020) Clinical characteristics and outcomes of 566 Thais with systemic sclerosis: a cohort study. Int J Rheum Dis 23:945–957. https://doi.org/10.1111/1756-185X.13859
http://statbbi.nso.go.th/staticreport/page/sector/en/01.aspx
StataCorp (2019) Stata Statistical Software: Release 16. StataCorp LLC, College Station, TX
Kuo C-F, See L-C, Yu K-H et al (2011) Epidemiology and mortality of systemic sclerosis: a nationwide population study in Taiwan. Scand J Rheumatol 40:373–378. https://doi.org/10.3109/03009742.2011.553736
Kim H, Cho S-K, Kim JW et al (2020) An increased disease burden of autoimmune inflammatory rheumatic diseases in Korea. Semin Arthritis Rheum 50:526–533. https://doi.org/10.1016/j.semarthrit.2019.11.007
Minz RW, Kumar Y, Anand S et al (2012) Antinuclear antibody positive autoimmune disorders in North India: an appraisal. Rheumatol Int 32:2883–2888. https://doi.org/10.1007/s00296-011-2134-1
Roberts-Thomson PJ, Walker JG, Lu TY-T et al (2006) Scleroderma in South Australia: further epidemiological observations supporting a stochastic explanation. Intern Med J 36:489–497. https://doi.org/10.1111/j.1445-5994.2006.01125.x
Kang GW, Jung KH, Lee YS et al (2018) Incidence, prevalence, mortality and causes of death in systemic sclerosis in Korea: a nationwide population-based study. Br J Dermatol 178:e37–e39. https://doi.org/10.1111/bjd.15838
Chandran G, Smith M, Ahern MJ, Roberts-Thomson PJ (1995) A study of scleroderma in South Australia: prevalence, subset characteristics and nailfold capillaroscopy. Aust N Z J Med 25:688–694
Kuwana M, Saito A, Sakamoto W et al (2022) Incidence rate and prevalence of systemic sclerosis and systemic sclerosis-associated interstitial lung disease in Japan: analysis using Japanese claims databases. Adv Ther 39:2222–2235. https://doi.org/10.1007/s12325-022-02078-5
Araújo FC, Camargo CZ, Kayser C (2017) Validation of the ACR/EULAR classification criteria for systemic sclerosis in patients with early scleroderma. Rheumatol Int 37:1825–1833. https://doi.org/10.1007/s00296-017-3787-1
Yu K-H, See L-C, Kuo C-F et al (2013) Prevalence and incidence in patients with autoimmune rheumatic diseases: a nationwide population-based study in Taiwan. Arthritis Care Res (Hoboken) 65:244–250. https://doi.org/10.1002/acr.21820
EAA C, Banos A, Kosmara D et al (2019) Sexual dimorphism in SLE: above and beyond sex hormones. Lupus 28:3–10. https://doi.org/10.1177/0961203318815768
Ungprasert P, Crowson CS, Chowdhary VR et al (2016) Epidemiology of mixed connective tissue disease, 1985-2014: a population-based study. Arthritis Care Res (Hoboken) 68:1843–1848. https://doi.org/10.1002/acr.22872
Qin B, Wang J, Yang Z et al (2015) Epidemiology of primary Sjögren’s syndrome: a systematic review and meta-analysis. Ann Rheum Dis 74:1983–1989. https://doi.org/10.1136/annrheumdis-2014-205375
Narváez J, Sánchez-Fernández SÁ, Seoane-Mato D et al (2020) Prevalence of Sjögren’s syndrome in the general adult population in Spain: estimating the proportion of undiagnosed cases. Sci Rep 10:10627. https://doi.org/10.1038/s41598-020-67462-z
Apipattarakul R, Foocharoen C, Netwijitpan S et al (2018) Clinical characteristics and mortality rate of Thai elderly-onset systemic sclerosis. Clin Exp Rheumatol 36(Suppl 113):76–81
Foocharoen C, Mahakkanukrauh A, Suwannaroj S, Nanagara R (2014) Clinical characteristics and mortality in systemic sclerosis: a comparison between early- and late-referred diseases. J Med Assoc Thai 97:28–35
Tyndall AJ, Bannert B, Vonk M et al (2010) Causes and risk factors for death in systemic sclerosis: a study from the EULAR Scleroderma Trials and Research (EUSTAR) database. Ann Rheum Dis 69:1809–1815. https://doi.org/10.1136/ard.2009.114264
Rubio-Rivas M, Royo C, Simeón CP et al (2014) Mortality and survival in systemic sclerosis: systematic review and meta-analysis. Semin Arthritis Rheum 44:208–219. https://doi.org/10.1016/j.semarthrit.2014.05.010
Park S-K, Kim T-H, Jun J-B et al (2001) The clinical features and autoantibody profile in progressive systemic sclerosis of Korea. J Korean Rheumatol Assoc 8:243–252
Louthrenoo W, Kasitanon N, Wichainun R et al (2013) Association of HLA-DRB1*15:02 and DRB5*01:02 allele with the susceptibility to systemic sclerosis in Thai patients. Rheumatol Int 33:2069–2077. https://doi.org/10.1007/s00296-013-2686-3
Mahakkanukrauh A, Suwannaroj S, Romphruk A et al (2015) The Association of HLA and Systemic Sclerosis (SSc) in the Northeastern Thais. KKU Res J 20:459–464. https://doi.org/10.14456/kkurj.2015.38
Louthrenoo W, Kasitanon N, Wichainun R et al (2011) Lack of CTGF*-945C/G dimorphism in Thai patients with systemic sclerosis. Open Rheumatol J 5:59–63. https://doi.org/10.2174/1874312901105010059
Foocharoen C, Peansukwech U, Pongkulkiat P et al (2021) Aerosol components associated with hospital mortality in systemic sclerosis: an analysis from a nationwide Thailand healthcare database. Sci Rep 11:7983. https://doi.org/10.1038/s41598-021-87114-0
Li R, Sun J, Ren L-M et al (2012) Epidemiology of eight common rheumatic diseases in China: a large-scale cross-sectional survey in Beijing. Rheumatology (Oxford) 51:721–729. https://doi.org/10.1093/rheumatology/ker370
Acknowledgements
The authors thank (a) the Scleroderma Research Group for research assistance, (b) the Information and Communication Technology Center, Ministry of Public Health for access to database, (c) Mr. Bryan Roderick Hamman—under the aegis of the Publication Clinic Khon Kaen University, Thailand—for assistance with the English-language presentation.
Funding
The study received funding support from Thailand’s National Science, Research, and Innovation Fund.
Author information
Authors and Affiliations
Contributions
Conceptualization: Foocharoen C. and Ngamjarus C. Data curation: Foocharoen C., Suwannaroj S., and Mahakkanukrauh A. Formal analysis: Foocharoen C. Funding acquisition: Foocharoen C. and Mahakkanukrauh A. Methodology: Foocharoen C., Ngamjarus C., and Pattanittum P. Writing—original draft: Foocharoen C. Writing—review and editing: Foocharoen C., Pattanittum P., Ngamjarus C., Suwannaroj S., Ponkulkiat P., Onchan T., Wattanasukchai L., Chaiyarit J., and Mahakkanukrauh A.
Corresponding author
Ethics declarations
Disclosures
None
Ethics approval and consent to participate
The Human Research Ethics Committee of Khon Kaen University reviewed and approved the study per the Helsinki Declaration and the Good Clinical Practice Guidelines (HE651342). The need for informed consent was waived by The Human Research Ethics Committee of Khon Kaen University.
Consent for publication
All authors consent to publication and grant the publisher exclusive license of the full copyright.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Foocharoen, C., Ngamjarus, C., Pattanittum, P. et al. Incidence and prevalence of systemic sclerosis in Thailand in year 2017–2020: a database from the Ministry of Public Health. Clin Rheumatol 42, 1767–1774 (2023). https://doi.org/10.1007/s10067-023-06550-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-023-06550-7