Abstract
Objective
Explore the perspective of patients and professionals regarding non-radiographic axial spondyloarthritis (nr-axSpA) and to define the patient’s journey from diagnosis to treatment in order to identify unmet needs during the process.
Methods
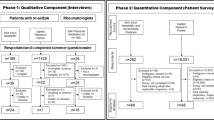
A qualitative study was carried out in two phases. In the first part, five focus groups were held with rheumatologists, orthopaedist, physiotherapists, primary care physicians (PCP), radiologists and six narrative interviews with nr-axSpA patients. In the second part, a nominal group meeting was held to detect which needs were not covered in the nr-axSpA (all of whom had collaborated in the previous phase).
Results
The topics discussed with professional groups and patients were the appropriateness of the term and concept of nr-axSpA, the management of low back pain and inflammatory back pain in routine clinical practice, complementary test and the problem of waiting lists and finally the unmet needs both from a practitioner’s and a patient’s perspective. The final group explored solutions to the problems based on what was discussed in the first part of the project. Some of these solutions were strengthening relations between specialties, implementing high resolution consultations, rethinking the disability scales, offering better information to patients, designing resource maps and using different strategies to promote knowledge of the disease.
Conclusion
Many different perspectives on the same disease have revealed the difficult journey of the patient with suspected nr-axSpA, while identifying problems and solutions.
Key Points • Diagnosis of nr-AxSpA among health professionals outside rheumatology may lead to numerous turns and difficulties in the patient’s journey. • The impact of delays and complications in the journey to diagnosis is not quantified but directly affects the state of well-being and health of patients. • Multidisciplinary care is far from a reality. Primary care (key specialists in any chronic condition), radiologists, orthopaedists, and non-physicians such as physiotherapists and psychologists are generally excluded from dealing with these patients, and often have to do their work outside of physicians, rather than working together in a truly patient-centred medicine. |

Similar content being viewed by others
References
Braun J, Baraliakos X, Kiltz U (2016) Non-radiographic axial spondyloarthritis: a classification or a diagnosis? Clin Exp Rheumatol 34(1 Suppl 95):S5–S6
Fianyo E, Wendling D, Poulain C, Farrenq V, Claudepierre P (2014) Non-radiographic axial spondyloarthritis: what is it? Clin Exp Rheumatol 32(1):1–4
Sieper J, Hu X, Black CM, Grootscholten K, van den Broek RWM, Kachroo S (2017) Systematic review of clinical, humanistic, and economic outcome comparisons between radiographic and non-radiographic axial spondyloarthritis. Semin Arthritis Rheum 46(6):746–753. https://doi.org/10.1016/j.semarthrit.2016.09.002
Baraliakos X, Braun J (2015) Non-radiographic axial spondyloarthritis and ankylosing spondylitis: what are the similarities and differences? RMD Open 1(Suppl 1):e000053. https://doi.org/10.1136/rmdopen-2015-000053
Callhoff J, Sieper J, Weiss A, Zink A, Listing J (2015) Efficacy of TNFalpha blockers in patients with ankylosing spondylitis and non-radiographic axial spondyloarthritis: a meta-analysis. Ann Rheum Dis 74(6):1241–1248. https://doi.org/10.1136/annrheumdis-2014-205322
Kroon FP, van der Burg LR, Ramiro S, Landewe RB, Buchbinder R, Falzon L, van der Heijde D (2015) Non-steroidal anti-inflammatory drugs (NSAIDs) for axial spondyloarthritis (ankylosing spondylitis and non-radiographic axial spondyloarthritis). Cochrane Database Syst Rev 7:CD010952. https://doi.org/10.1002/14651858.CD010952.pub2
van der Heijde D, Ramiro S, Landewe R, Baraliakos X, Van den Bosch F, Sepriano A, Regel A, Ciurea A, Dagfinrud H, Dougados M, van Gaalen F, Geher P, van der Horst-Bruinsma I, Inman RD, Jongkees M, Kiltz U, Kvien TK, Machado PM, Marzo-Ortega H, Molto A, Navarro-Compan V, Ozgocmen S, Pimentel-Santos FM, Reveille J, Rudwaleit M, Sieper J, Sampaio-Barros P, Wiek D, Braun J (2017) 2016 update of the ASAS-EULAR management recommendations for axial spondyloarthritis. Ann Rheum Dis 76(6):978–991. https://doi.org/10.1136/annrheumdis-2016-210770
Ward MM, Deodhar A, Akl EA, Lui A, Ermann J, Gensler LS, Smith JA, Borenstein D, Hiratzka J, Weiss PF, Inman RD, Majithia V, Haroon N, Maksymowych WP, Joyce J, Clark BM, Colbert RA, Figgie MP, Hallegua DS, Prete PE, Rosenbaum JT, Stebulis JA, van den Bosch F, Yu DT, Miller AS, Reveille JD, Caplan L (2016) American College of Rheumatology/Spondylitis Association of America/Spondyloarthritis Research and treatment network 2015 recommendations for the treatment of ankylosing spondylitis and nonradiographic axial spondyloarthritis. Arthritis Rheum 68(2):282–298. https://doi.org/10.1002/art.39298
Deodhar A, Strand V, Kay J, Braun J (2016) The term ‘non-radiographic axial spondyloarthritis’ is much more important to classify than to diagnose patients with axial spondyloarthritis. Ann Rheum Dis 75(5):791–794. https://doi.org/10.1136/annrheumdis-2015-208852
Akkoc N, Khan MA (2016) ASAS classification criteria for axial spondyloarthritis: time to modify. Clin Rheumatol 35(6):1415–1423. https://doi.org/10.1007/s10067-016-3261-6
Fallahi S, Jamshidi AR (2016) Diagnostic delay in ankylosing spondylitis: related factors and prognostic outcomes. Arch Rheumatol 31(1):24–30. https://doi.org/10.5606/ArchRheumatol.2016.5562
Redeker I, Hoffmann F, Callhoff J, Haibel H, Sieper J, Zink A, Poddubnyy D (2018) Determinants of psychological well-being in axial spondyloarthritis: an analysis based on linked claims and patient-reported survey data. Ann Rheum Dis 77(7):1017–1024. https://doi.org/10.1136/annrheumdis-2017-212629
Bair MJ, Robinson RL, Katon W, Kroenke K (2003) Depression and pain comorbidity: a literature review. Arch Intern Med 163(20):2433–2445. https://doi.org/10.1001/archinte.163.20.2433
Zhao S, Thong D, Duffield SJ, Hughes D, Goodson NJ (2018) Alcohol and disease activity in axial spondyloarthritis: a cross-sectional study. Rheumatol Int 38(3):375–381. https://doi.org/10.1007/s00296-018-3927-2
Strand V, Singh JA (2017) Patient burden of axial spondyloarthritis. J Clin Rheumatol 23(7):383–391. https://doi.org/10.1097/RHU.0000000000000589
Robinson PC, Wordsworth BP, Reveille JD, Brown MA (2013) Axial spondyloarthritis: a new disease entity, not necessarily early ankylosing spondylitis. Ann Rheum Dis 72(2):162–164. https://doi.org/10.1136/annrheumdis-2012-202073
Ciurea A, Scherer A, Exer P, Bernhard J, Dudler J, Beyeler B, Kissling R, Stekhoven D, Rufibach K, Tamborrini G, Weiss B, Muller R, Nissen MJ, Michel BA, van der Heijde D, Dougados M, Boonen A, Weber U, Rheumatologists of the Swiss Clinical Quality Management Program for Axial S (2013) Tumor necrosis factor alpha inhibition in radiographic and nonradiographic axial spondyloarthritis: results from a large observational cohort. Arthritis Rheum 65(12):3096–3106. https://doi.org/10.1002/art.38140
Kiltz U, Baraliakos X, Karakostas P, Igelmann M, Kalthoff L, Klink C, Krause D, Schmitz-Bortz E, Florecke M, Bollow M, Braun J (2012) The degree of spinal inflammation is similar in patients with axial spondyloarthritis who report high or low levels of disease activity: a cohort study. Ann Rheum Dis 71(7):1207–1211. https://doi.org/10.1136/annrheumdis-2011-200508
Althoff CE, Sieper J, Song IH, Haibel H, Weiss A, Diekhoff T, Rudwaleit M, Freundlich B, Hamm B, Hermann KG (2013) Active inflammation and structural change in early active axial spondyloarthritis as detected by whole-body MRI. Ann Rheum Dis 72(6):967–973. https://doi.org/10.1136/annrheumdis-2012-201545
Kudrina I, Shir Y, Fitzcharles MA (2015) Multidisciplinary treatment for rheumatic pain. Best Pract Res Clin Rheumatol 29(1):156–163. https://doi.org/10.1016/j.berh.2015.04.029
Wallman JK, Joud A, Olofsson T, Jacobsson LTH, Bliddal H, Kristensen LE (2017) Work disability in non-radiographic axial spondyloarthritis patients before and after start of anti-TNF therapy: a population-based regional cohort study from southern Sweden. Rheumatology (Oxford) 56(5):716–724. https://doi.org/10.1093/rheumatology/kew473
Villaverde V, Carmona L, Lopez Robledillo JC, Serrano S, Gobbo M, Grupo de Estudio E (2013) Motivations and objections to implement a spondyloarthritis integrated care pathway. A qualitative study with primary care physicians. Reumatol Clin 9(2):85–89. https://doi.org/10.1016/j.reuma.2012.06.003
Cooksey R, Brophy S, Husain MJ, Irvine E, Davies H, Siebert S (2012) The information needs of people living with ankylosing spondylitis: a questionnaire survey. BMC Musculoskelet Disord 13:243. https://doi.org/10.1186/1471-2474-13-243
Kjeken I, Dagfinrud H, Mowinckel P, Uhlig T, Kvien TK, Finset A (2006) Rheumatology care: involvement in medical decisions, received information, satisfaction with care, and unmet health care needs in patients with rheumatoid arthritis and ankylosing spondylitis. Arthritis Rheum 55(3):394–401. https://doi.org/10.1002/art.21985
Almodovar R, Gratacos J, Zarco P (2018) Information needs of patients with spondyloarthritis about their disease. Reumatol Clin 14(6):367–371. https://doi.org/10.1016/j.reuma.2017.02.004
Derakhshan MH, Pathak H, Cook D, Dickinson S, Siebert S, Gaffney K, Nass, investigators BR (2018) Services for spondyloarthritis: a survey of patients and rheumatologists. Rheumatology (Oxford) 57(6):987–996. https://doi.org/10.1093/rheumatology/kex518
Jovani V, Blasco-Blasco M, Ruiz-Cantero MT, Pascual E (2017) Understanding how the diagnostic delay of spondyloarthritis differs between women and men: a systematic review and metaanalysis. J Rheumatol 44(2):174–183. https://doi.org/10.3899/jrheum.160825
Rusman T, van Vollenhoven RF, van der Horst-Bruinsma IE (2018) Gender differences in axial spondyloarthritis: women are not so lucky. Curr Rheumatol Rep 20(6):35. https://doi.org/10.1007/s11926-018-0744-2
Acknowledgements
The authors would like to thank the investigators for their contribution in the focus groups and to the patients involved for their collaboration in the interviews.
Funding
This work was supported by Novartis Farmacéutica S.A.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Outside this project, institution (InMusc) has received consultancy honoraria from Abbvie, Astellas, BMS, Gebro Pharma, Lylly, MSD, Pfizer, Roche, Sanofi-Aventis and UCB Pharma. Loreto Carmona and Teresa Oton are full-time employees of InMusc.
Carlos Sastre is a full-time employee of Novartis Farmaceutica S.A.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Otón, T., Sastre, C. & Carmona, L. The journey of the non-radiographic axial spondyloarthritis patient: the perspective of professionals and patients. Clin Rheumatol 40, 591–600 (2021). https://doi.org/10.1007/s10067-020-05269-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05269-z