Abstract
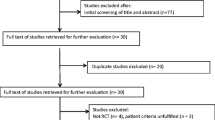
Chronic non-specific widespread pain (CWP) including fibromyalgia (FMS) is characterized by widespread pain, reduced pain threshold, and multiple tender points on examination, causing disability and decreased quality of life. Vitamin D has been proposed as an associated factor in CWP. This meta-analysis aimed to explore the benefit of vitamin D supplementation in the management of CWP. A comprehensive search of the CENTRAL, MEDLINE, and Embase databases was performed from inception through January 2017. The inclusion criterion was the randomized clinical trials’ evaluating the effects of vitamin D treatment in adult subjects with CWP or FMS. CWP was defined as chronic recurrent musculoskeletal pain without secondary causes; FMS patients met the American College of Rheumatology criteria for FMS. Study outcome was assessed using visual analog scale (VAS) of pain intensity. Pooled mean difference (MD) of VAS and 95% confidence interval (CI) were calculated using a random-effect meta-analysis. Meta-regression analysis using a random-effects model was performed to explore the effects of change in vitamin D in the treatment group on difference in the mean of VAS. Sensitivity analysis was performed to evaluate the robustness of results. The between-study heterogeneity of effect size was quantified using the Q statistic and I 2. Data were extracted from four randomized controlled trials involving 287 subjects. Pooled result demonstrated a significantly lower VAS in CWP patients who received vitamin D treatment compared with those who received placebo (MD = 0.46; 95% CI 0.09–0.89, I 2 = 48%). Meta-regression analysis revealed no significant relationship between the changes of vitamin D and VAS (coefficient = 0.04 (95% CI −0.01 to 0.08), p = 0.10). In this meta-analysis, we conclude that vitamin D supplementation is able to decrease pain scores and improve pain despite no significant change in VAS after increasing serum vitamin D level. Further studies need to be conducted in order to explore the improvement of functional status, quality of life, and the pathophysiological change that improves chronic widespread pain.





Similar content being viewed by others
References
Hsiao MY, Hung CY, Chang KV, Han DS, Wang TG (2015) Is serum hypovitaminosis D associated with chronic widespread pain including fibromyalgia? A meta-analysis of observational studies. Pain Physician 18(5):E877–E887
Meeus M, Nijs J (2007) Central sensitization: a biopsychosocial explanation for chronic widespread pain in patients with fibromyalgia and chronic fatigue syndrome. Clin Rheumatol 26(4):465–473
Uceyler N, Valenza R, Stock M, Schedel R, Sprotte G, Sommer C (2006) Reduced levels of antiinflammatory cytokines in patients with chronic widespread pain. Arthritis Rheum 54(8):2656–2664
Schreuder F, Bernsen RM, van der Wouden JC (2012) Vitamin D supplementation for nonspecific musculoskeletal pain in non-Western immigrants: a randomized controlled trial. Ann Fam Med 10(6):547–555
Bischoff HA, Borchers M, Gudat F, Duermueller U, Theiler R, Stahelin HB et al (2001) In situ detection of 1, 25-dihydroxyvitamin D3 receptor in human skeletal muscle tissue. Histochem J 33(1):19–24
Straube S, Andrew Moore R, Derry S, McQuay HJ (2009) Vitamin D and chronic pain. Pain 141(1–2):10–13
Higgins JPT, Green S, Cochrane Collaboration. Cochrane handbook for systematic reviews of interventions. Chichester, England; Hoboken, NJ: Wiley-Blackwell; 2008. xxi, 649 p. p
Wolfe F, Smythe HA, Yunus MB, Bennett RM, Bombardier C, Goldenberg DL et al (1990) The American College of Rheumatology 1990 criteria for the classification of fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum 33(2):160–172
Wolfe F, Clauw DJ, Fitzcharles MA, Goldenberg DL, Katz RS, Mease P et al (2010) The American College of Rheumatology preliminary diagnostic criteria for fibromyalgia and measurement of symptom severity. Arthritis Care Res (Hoboken) 62(5):600–610
Sterne JA, Egger M (2001) Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol 54(10):1046–1055
Warner AE, Arnspiger SA (2008) Diffuse musculoskeletal pain is not associated with low vitamin D levels or improved by treatment with vitamin D. J Clin Rheumatol 14(1):12–16
Sakalli H, Arslan D, Yucel AE (2012) The effect of oral and parenteral vitamin D supplementation in the elderly: a prospective, double-blinded, randomized, placebo-controlled study. Rheumatol Int 32(8):2279–2283
Arvold DS, Odean MJ, Dornfeld MP, Regal RR, Arvold JG, Karwoski GC et al (2009) Correlation of symptoms with vitamin D deficiency and symptom response to cholecalciferol treatment: a randomized controlled trial. Endocr Pract 15(3):203–212
Bjorkman M, Sorva A, Tilvis R (2008) Vitamin D supplementation has no major effect on pain or pain behavior in bedridden geriatric patients with advanced dementia. Aging Clin Exp Res 20(4):316–321
Wepner F, Scheuer R, Schuetz-Wieser B, Machacek P, Pieler-Bruha E, Cross HS et al (2014) Effects of vitamin D on patients with fibromyalgia syndrome: a randomized placebo-controlled trial. Pain 155(2):261–268
Yilmaz R, Salli A, Cingoz HT, Kucuksen S, Ugurlu H (2016) Efficacy of vitamin D replacement therapy on patients with chronic nonspecific widespread musculoskeletal pain with vitamin D deficiency. Int J Rheum Dis
Karras S, Rapti E, Matsoukas S, Kotsa K. Vitamin D in fibromyalgia: a causative or confounding biological interplay? Nutrients. 2016;8(6)
Straube S, Derry S, Straube C, Moore RA (2015) Vitamin D for the treatment of chronic painful conditions in adults. Cochrane Database Syst Rev 5:CD007771
Wu Z, Malihi Z, Stewart AW, Lawes CM, Scragg R (2016) Effect of vitamin D supplementation on pain: a systematic review and meta-analysis. Pain Physician. 19(7):415–427
Shipton EE, Shipton EA (2015) Vitamin D deficiency and pain: clinical evidence of low levels of vitamin D and supplementation in chronic pain states. Pain Ther 4(1):67–87
Atef SH (2017) Vitamin D assays in clinical laboratory: past, present and future challenges. J Steroid Biochem Mol Biol
Farrell CJ, Martin S, McWhinney B, Straub I, Williams P, Herrmann M (2012) State-of-the-art vitamin D assays: a comparison of automated immunoassays with liquid chromatography-tandem mass spectrometry methods. Clin Chem 58(3):531–542
Jafri L, Khan AH, Siddiqui AA, Mushtaq S, Iqbal R, Ghani F et al (2011) Comparison of high performance liquid chromatography, radio immunoassay and electrochemiluminescence immunoassay for quantification of serum 25 hydroxy vitamin D. Clin Biochem 44(10–11):864–868
Abokrysha NT (2012) Vitamin D deficiency in women with fibromyalgia in Saudi Arabia. Pain Med 13(3):452–458
Badsha H, Daher M, Ooi KK (2009) Myalgias or non-specific muscle pain in Arab or Indo-Pakistani patients may indicate vitamin D deficiency. Clin Rheumatol 28(8):971–973
Matthana MH (2011) The relation between vitamin D deficiency and fibromyalgia syndrome in women. Saudi Med J 32(9):925–929
Harari M, Dramsdahl E, Shany S, Baumfeld Y, Ingber A, Novack V et al (2011) Increased vitamin D serum levels correlate with clinical improvement of rheumatic diseases after Dead Sea climatotherapy. Isr Med Assoc J 13(4):212–215
Grant WB, Karras SN, Bischoff-Ferrari HA, Annweiler C, Boucher BJ, Juzeniene A et al (2016) Do studies reporting ‘U’-shaped serum 25-hydroxyvitamin D-health outcome relationships reflect adverse effects? Dermatoendocrinol 8(1):e1187349
Acknowledgements
We thank Matthew Roslund for language editing and proofreading our article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Funding sources
None
Rights and permissions
About this article
Cite this article
Yong, W.C., Sanguankeo, A. & Upala, S. Effect of vitamin D supplementation in chronic widespread pain: a systematic review and meta-analysis. Clin Rheumatol 36, 2825–2833 (2017). https://doi.org/10.1007/s10067-017-3754-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-017-3754-y