Abstract
Introduction
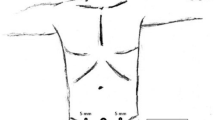
Diastasis recti represents a midline contour abnormality of the anterior abdominal wall that is secondary to attenuation of the linea alba. Severe diastasis recti is defined as attenuation of the linea alba as well as the linea semilunaris. Treatment options are variable and include conditioning exercises and surgical repair with or without mesh. This manuscript will review the indications and technique of onlay mesh for correction of severe diastasis recti.
Methods
Abdominoplasty with diastasis repair has been performed in 63 women from January 2010 to January 2020. Of these, 4 had repair for severe diastasis that included plication and onlay mesh. The mesh was polypropylene in 3 patients and silk in 1 patient. Indications for onlay mesh included severe diastasis as a means of further reinforcing the strength of the anterior rectus sheath.
Results
Of the 4 patients, all tolerated the operation well without morbidity. Natural contour was established in all. There were no infections, seromas, delayed healing or mesh removals. All drains were removed by 7 days.
Conclusion
The use of an onlay mesh has demonstrated success and should be considered in select patients for the surgical management of severe diastasis.























Similar content being viewed by others
References
Batchvarova Z, Leymarie N, Lepage C, Leyder P (2008) Use of a submuscular resorbable mesh for correction of severe post-pregnancy musculoaponeurotic laxity: an 11-year retrospective study. Plast Reconstr Surg 121:1240
Cheesborough JE, Dumanian GA (2015) Simultaneous prosthetic mesh abdominal wall reconstruction with abdominoplasty for ventral hernia and severe rectus diastasis repairs. Plast Reconstr Surg 135:268
Nahabedian MY (2017) Diastasis recti. In: Cobb W, Hope W (eds) Textbook of hernia. Springer, New York
Nahabedian MY (2016) Diagnosis and management of diastasis recti. In: Novitsky Y, Heniford T (eds) Current principles in surgery of the abdominal wall. Springer, New York
Nahabedian MY (2018) Management strategies for diastasis recti. Semin Plastic Surg 32(3):147–153
Van Kerckhoven L, Nevens T, Van De Winkel N, Miserez M, Vranckx JJ, Segers K (2021) Treatment of rectus diastasis: should the midline always be reinforced with mesh? A systematic review. J Plast Reconstr Aesthet Surg S1748–6815(21):00047–00054
Ferreira LM, Castilho HT, Hochberg J et al (2001) Triangular mattress suture in abdominal diastasis to prevent epigastric bulging. Ann Plast Surg 46:130
Nahas FX, Augusto SM, Ghelfond C (2001) Nylon versus polydioxanone in the correction of rectus diastasis. Plast Reconstr Surg 107:700
Al-Qattan MM (1997) Abdominoplasty in multiparous women with severe musculoaponeurotic laxity. Br J Plast Surg 50:450
Bucaria V, Boccuzz A (2021) Autologous dermal mesh in severe postpregnancy recti muscles diastasis. Aesth Plast Surg 45:198–211
Emanuelsson P, Gunnarsson U, Strigard K, Stark B (2014) Early complications, pain, and quality of life after reconstructive surgery for abdominal rectus muscle diastasis: a 3-month follow-up. J Plast Reconstr Aesthet Surg 67:1082–1088
Wormer BA, Clavin NW, Lefaivre J-F et al (2017) Reducing postoperative abdominal bulge following deep inferior epigastric perforator flap breast reconstruction with onlay monofilament poly-4-hydroxybutyrate biosynthetic mesh. J Reconstr Microsurg. 33(1):8–18
Emanuelsson P, Gunnarsson U, Dahlstrand U, Strig K, Stark B (2016) Operative correction of abdominal rectus diastasis (ARD) reduces pain and improves abdominal wall muscle strength: a randomized, prospective trial comparing retromuscular mesh repair to double-row, self-retaining sutures. Surgery 160:1367–1375
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Nahabedian is a consultant for Allergan and Stryker. No support was obtained in preparation of this manuscript.
Ethical approval
This manuscript was prpeared in complicance with the Helsinki doctrine.
Human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained for the surgical procedure prior to their participation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nahabedian, M.Y. Diastasis recti repair with onlay mesh. Hernia 25, 855–862 (2021). https://doi.org/10.1007/s10029-021-02464-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-021-02464-y