Abstract
Purpose
Local anaesthesia (LA) has proven effective for inguinal hernia repair in developed countries. Hernias in low to middle income countries represent a different issue. The aim of this study was to analyse the feasibility of LA for African hernia repairs in a limited resource environment.
Methods
Data from patients who underwent herniorrhaphy under LA or spinal anaesthesia (SA) by the 6th and 7th Forward Surgical Team were prospectively collected. All of the patients benefited from a transversus abdominis plane (TAP) block for postoperative analgesia. Primary endpoints concerned the pain response and conversion to general anaesthesia. Secondary endpoints concerned the complication and recurrence rates. Predictors of LA failure were then identified.
Results
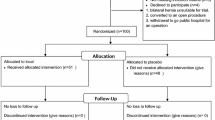
In all, 189 inguinal hernias were operated during the study period, and 119 patients fulfilled the inclusion criteria: 57 LA and 62 SA. Forty-eight percent of patients presented with inguinoscrotal hernias. Local anaesthesia led to more pain during surgery and necessitated more administration of analgesics but resulted in fewer micturition difficulties and better postoperative pain control. Conversion rates were not different. Inguinoscrotal hernia and a time interval <50 min between the TAP block and skin incision were predictors of LA failure. Forty-four patients were followed-up at one month. No recurrence was noted.
Conclusions
Local anaesthesia is a safe alternative to SA. Small or medium hernias can easily be performed under LA in rural centres, but inguinoscrotal hernias required an ultrasound-guided TAP block performed 50 min before surgery to achieve optimal analgesia, and should be managed only in centres equipped with ultrasonography.


Similar content being viewed by others
References
Prakash D, Heskin L, Doherty S, Galvin R (2017) Local anaesthesia versus spinal anaesthesia in inguinal hernia repair: a systematic review and meta-analysis. Surgeon 15:47–57. doi:10.1016/j.surge.2016.01.001
Nordin P, Zetterstrom H, Gunnarsson U, Nilsson E (2003) Local, regional, or general anaesthesia in groin hernia repair: multicentre randomised trial. Lancet 362:853–858. doi:10.1016/S0140-6736(03)14339-5
O’Dwyer PJ, Serpell MG, Millar K, Paterson C, Young D, Hair A, Courtney CA, Horgan P, Kumar S, Walker A, Ford I (2003) Local or general anesthesia for open hernia repair: a randomized trial. Ann Surg 237:574–579. doi:10.1097/01.SLA.0000059992.76731.64
Nordin P, Hernell H, Unosson M, Gunnarsson U, Nilsson E (2004) Type of anaesthesia and patient acceptance in groin hernia repair: a multicentre randomised trial. Hernia 8:220–225. doi:10.1007/s10029-004-0234-5
Gultekin FA, Kurukahvecioglu O, Karamercan A, Ege B, Ersoy E, Tatlicioglu E (2007) A prospective comparison of local and spinal anesthesia for inguinal hernia repair. Hernia 11:153–156. doi:10.1007/s10029-006-0166-3
Nordin P, Zetterstrom H, Carlsson P, Nilsson E (2007) Cost-effectiveness analysis of local, regional and general anaesthesia for inguinal hernia repair using data from a randomized clinical trial. Br J Surg 94:500–505. doi:10.1002/bjs.5543
van Veen RN, Mahabier C, Dawson I, Hop WC, Kok NF, Lange JF, Jeekel J (2008) Spinal or local anesthesia in lichtenstein hernia repair: a randomized controlled trial. Ann Surg 247:428–433. doi:10.1097/SLA.0b013e318165b0ff
Reece-Smith AM, Maggio AQ, Tang TY, Walsh SR (2009) Local anaesthetic vs. general anaesthetic for inguinal hernia repair: systematic review and meta-analysis. Int J Clin Pract 63:1739–1742. doi:10.1111/j.1742-1241.2009.02131.x
Joshi GP, Rawal N, Kehlet H, Bonnet F, Camu F, Fischer HB, Neugebauer EA, Schug SA, Simanski CJ (2012) Evidence-based management of postoperative pain in adults undergoing open inguinal hernia surgery. Br J Surg 99:168–185. doi:10.1002/bjs.7660
Lundstrom KJ, Sandblom G, Smedberg S, Nordin P (2012) Risk factors for complications in groin hernia surgery: a national register study. Ann Surg 255:784–788. doi:10.1097/SLA.0b013e31824b7cb3
Bourgon AL, Fox JP, Saxe JM, Woods RJ (2015) Outcomes and charges associated with outpatient inguinal hernia repair according to method of anesthesia and surgical approach. Am J Surg 209:468–472. doi:10.1016/j.amjsurg.2014.09.021
Nordberg EM (1984) Incidence and estimated need of caesarean section, inguinal hernia repair, and operation for strangulated hernia in rural Africa. Br Med J (Clin Res Ed) 289:92–93
Gil J, Rodriguez JM, Hernandez Q, Gil E, Balsalobre MD, Gonzalez M, Torregrosa N, Verdu T, Alcaraz M, Parrilla P (2012) Do hernia operations in african international cooperation programmes provide good quality? World J Surg 36:2795–2801. doi:10.1007/s00268-012-1768-9
Kulacoglu H, Ozyaylali I, Yazicioglu D (2009) Factors determining the doses of local anesthetic agents in unilateral inguinal hernia repair. Hernia 13:511–516. doi:10.1007/s10029-009-0513-2
Mabula JB, Chalya PL (2012) Surgical management of inguinal hernias at Bugando Medical Centre in northwestern Tanzania: our experiences in a resource-limited setting. BMC Res Notes 5:585. doi:10.1186/1756-0500-5-585
Mitura K, Koziel S, Pasierbek M (2015) Groin hernia surgery in northern Ghana—humanitarian mission of Polish surgeons in Tamale. Pol Przegl Chir 87:16–21. doi:10.1515/pjs-2015-0012
Sanders DL, Porter CS, Mitchell KC, Kingsnorth AN (2008) A prospective cohort study comparing the African and European hernia. Hernia 12:527–529. doi:10.1007/s10029-008-0369-x
Ohene-Yeboah M (2003) Strangulated external hernias in Kumasi. West Afr J Med 22:310–313
Shillcutt SD, Clarke MG, Kingsnorth AN (2010) Cost-effectiveness of groin hernia surgery in the Western Region of Ghana. Arch Surg 145:954–961. doi:10.1001/archsurg.2010.208
Miserez M, Alexandre JH, Campanelli G, Corcione F, Cuccurullo D, Pascual MH, Hoeferlin A, Kingsnorth AN, Mandala V, Palot JP, Schumpelick V, Simmermacher RK, Stoppa R, Flament JB (2007) The European hernia society groin hernia classification: simple and easy to remember. Hernia 11:113–116. doi:10.1007/s10029-007-0198-3
Kingsnorth A, LeBlanc K (2003) Hernias: inguinal and incisional. Lancet 362:1561–1571. doi:10.1016/S0140-6736(03)14746-0
Ozgun H, Kurt MN, Kurt I, Cevikel MH (2002) Comparison of local, spinal, and general anaesthesia for inguinal herniorrhaphy. Eur J Surg 168:455–459. doi:10.1080/110241502321116442
Narita M, Sakano S, Okamoto S, Uemoto S, Yamamoto M (2009) Tumescent local anesthesia in inguinal herniorrhaphy with a PROLENE hernia system: original technique and results. Am J Surg 198:e27–e31. doi:10.1016/j.amjsurg.2008.11.045
Ban LJ, Lei WZ, Liu Y, Gong YP, Zeng Y, Yang L, Zhang W (2011) Comparison of three concentrations of simplex lidocaine in local anesthesia for inguinal hernia mesh-repairs. Hernia 15:517–520. doi:10.1007/s10029-011-0813-1
Milone M, Di Minno MN, Musella M, Maietta P, Salvatore G, Iacovazzo C, Milone F (2013) Outpatient inguinal hernia repair under local anaesthesia: feasibility and efficacy of ultrasound-guided transversus abdominis plane block. Hernia 17:749–755. doi:10.1007/s10029-012-1022-2
Young MJ, Gorlin AW, Modest VE, Quraishi SA (2012) Clinical implications of the transversus abdominis plane block in adults. Anesthesiol Res Pract 2012:731645. doi:10.1155/2012/731645
Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, de Lange D, Fortelny R, Heikkinen T, Kingsnorth A, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Miserez M (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13:343–403. doi:10.1007/s10029-009-0529-7
Gurleyik E, Gurleyik G, Cetinkaya F, Unalmiser S (1998) The inflammatory response to open tension-free inguinal hernioplasty versus conventional repairs. Am J Surg 175:179–182
Nilsson H, Angeras U, Sandblom G, Nordin P (2016) Serious adverse events within 30 days of groin hernia surgery. Hernia 20:377–385. doi:10.1007/s10029-016-1476-8
Vatansev C, Belviranli M, Aksoy F, Tuncer S, Sahin M, Karahan O (2002) The effects of different hernia repair methods on postoperative pain medication and CRP levels. Surg Laparosc Endosc Percutan Tech 12:243–246
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
S. Bourgouin, Y. Goudard, A. Montcriol, J. Bordes, A. Nau and P. Balandraud have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Human and animal rights
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Bourgouin, S., Goudard, Y., Montcriol, A. et al. Feasibility and limits of inguinal hernia repair under local anaesthesia in a limited resource environment: a prospective controlled study. Hernia 21, 749–757 (2017). https://doi.org/10.1007/s10029-017-1631-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-017-1631-x