Abstract
Background
Inguinal hernia repairs are one of the most commonly performed procedures in the UK. This study examined the adequacy of the consent process for inguinal hernia repair focusing on the patients’ understanding of the relative risks and benefits of laparoscopic versus open repair.
Methods
The study consisted of a retrospective postal questionnaire poll of 200 patients (162 males and 38 females) aged between 42 and 85 who had been assessed in the surgical outpatients (within the last 12 months) and received counselling regarding their inguinal hernia repair. Patient perception regarding the risks and merit of laparoscopic versus open repair was surveyed using a multiple-choice questionnaire.
Results
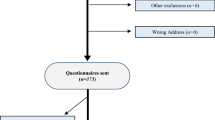
One hundred and twenty patients (60 %) returned their questionnaires, after excluding recurrent and bilateral hernias; 97 patients were entered into the study. The majority of patients reported a perception that a laparoscopic repair was safer and quicker than open (61.5 and 75.4 %, respectively); 29.2 % of patients felt that the recurrence rate was lower with a laparoscopic repair with 50.8 % of patients expressing that open repair had a higher complication rate than laparoscopic treatment; 81.5 % of patients correctly appreciated that laparoscopic repair had a quicker return to work; and 76.9 % of patients felt that laparoscopic repair was the only method, which could be undertaken as a day case procedure.
Conclusion
The results show that many patients have an incorrect perception of laparoscopic inguinal hernia repair, which may reflect an inadequate consent and counselling process. No definitive evidence exists regarding the superior safety and efficacy of one method over another, but it would appear that a significant number of patients are unaware of this.



Similar content being viewed by others
References
Laparoscopic surgery for inguinal hernia repair. National Institute for Clinical Excellence. http://www.nice.org.uk/nicemedia/live/11542/32934.pdf
Simons MP, Aufenacker T, Bay-Nielsen M et al (2009) European hernia society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13(4):343–403
McCormack K, Scott NW, Go PM, Ross S, Grant AM (2003) Collaboration EU hernia trialists. Laparoscopic techniques versus open techniques for inguinal hernia repair. Cochrane Database of Systematic Reviews 2003: CD001785
Bright E, Reddy VM, Wallace D, Garcea G, Dennison AR (2010) The incidence and success of treatment of severe chronic groin pain after open, transabdominal preperitoneal and totally extraperitoneal hernia repair. World J Surg 34(4):692–696
Alkhaffaf B, Decadt B (2010) Litigation following groin hernia repair in England. Hernia 14(2):181–186
Williams N, Scott A (1999) Conventional or laparoscopic inguinal hernia repair? The surgeon’s choice. Ann R Coll Surg Engl 81:56–57
General Medical Council (2008) Consent: patients and doctors making decisions together. GMC, London
Ashraff S, Malawa G, Dolan T, Khanduja V (2006) Prospective randomised controlled trial on the role of patient information leaflets in obtaining informed consent. ANZ J Surg 76(3):139–141
Lavelle-Jones C, Byrne DJ, Rice P, Cushieri A (1993) Factors affecting quality of informed consent. Brit Med J 306:885–890
Sugarman J, McCrory DC, Hubal RC (1998) Getting meaningful informed consent from older adults: a structured literature review of empirical research. J Am Geriatr Soc 46:517–524
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Patel, M., Garcea, G., Fairhurst, K. et al. Patient perception of laparoscopic versus open mesh repair of inguinal hernia, the hard sell. Hernia 16, 411–415 (2012). https://doi.org/10.1007/s10029-012-0933-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-012-0933-2