Abstract
Objective
This study aimed to determine the prevalence of ADHD and co-morbid conditions in a sample of primary school children aged 7–12 years in Nigeria.
Method
A two-staged procedure in which primary school pupils aged 6–12 years (n = 1112) were assessed for DSM-IV criteria of attention deficit hyperactivity disorder (ADHD) by their teachers in the first stage and their parents in the second stage. A flexible criterion was used for estimating the prevalence.
Results
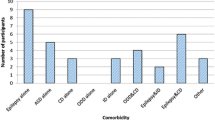
The prevalence of ADHD was 8.7%. The prevalence of the subtypes were: predominantly Inattentive 4.9%, predominantly hyperactive/impulsive 1.2% and combined 2.6%. The male to female ratio was 2:1 for all the subtypes of ADHD except hyperactive/impulsive which was 3.2:1. The co-morbid conditions include oppositional defiant disorder (ODD – 25.8%), conduct disorder (CD – 9.3%) and anxiety/depression (20.6%). While ODD and CD were associated with the hyperactive/impulsive subtype, anxiety/depression was associated with inattentive subtype.
Conclusion
Our findings support the notion that ADHD occurs across cultures. Given the prevalent rate, efforts should be made to map out strategies for early identification and referral of these children for proper evaluation and treatment. This study can serve as a platform for future analytical studies about this challenging research issue in sub-Saharan Africa.
Similar content being viewed by others
References
American Psychiatric Association (1994). Diagnostic and statistical manual of mental disorders, (4th ed). American Psychiatric Association, Washington, DC
Ashenafi Y, Kebede D, Desta M, Alem A (2000) Socio-demographic correlates of mental and behavioural disorders of children in southern Ethiopia. East Afr Med J 77:565–569
Ashenafi Y, Kebede D, Desta M, Alem A (2001) Prevalence of mental and behavioural disorders in Ethiopian children. East Afr Med J 78:308–311
Biederman J, Faraone SV, Monuteaux M, Spencer T, Wilens T, Bober M (2004) Gender effects of attention deficit hyperactivity disorder in adults, revisited. Biol Psychiatry 55:692–700
Brook U, Boaz M (2005) Attention deficit and learning disabilities (ADHD/LD) among high school pupils in Holon (Israel). Patient Educational Counselling 58:164–167
Cornejo JW, Osio O, Sanchez Y, Carrizosa J, Sanchez G, Grisales H, Castillo-Parra H, Holguin J (2005), [Prevalence of attention deficit hyperactivity disorder in Colombian children and teenagers]. Rev Neurol 40:716–722
Dwivedi KN, Banhatti RG (2005) Attention deficit/hyperactivity disorder and ethnicity. Arch Dis Child 2005 1:i10–2
Ersan EE, Dogan O, Dogan S, Sumer H (2004) The distribution of symptoms of attention-deficit/hyperactivity disorder and oppositional defiant disorder in school age children in Turkey. Euro Child Adolesc Psychiatry 13:354–361
Faraone SV, Sergeant J, Gillberg C, Biderman J (2003) The worldwide prevalence of ADHD: Is it an American condition? World Psychiatry 2:104–113
Graetz BW, Sawyer MG, Hazell P, Arney F, Baghurst P (2001) Validity of DSM-IV ADHD subtypes in a nationally representative sample of Australian children and adolescents. J Am Acad Child Adolesc Psychiatry 40:1410–1417
Levy F, Hay DA, Bennett KS, McStephen M (2005) Gender differences in ADHD subtype comorbidity. J Am Acad Child Adolesc Psychiatry 44:368–376
Lindgren S, Koeppl GG (1987) Assesing child behaviour problems in a medical setting: development of the Pediatric Behaviour Scale. In: Prinz RJ (ed) Advances in behavioural assesment of children and families, vol 3. JAI Press, Greenwich, CT, pp 57–90
Livingston R (1999) Cultural issues in diagnosis and treatment of ADHD. J Am Acad Child Adolesc Psychiatry 38:1591–1594
National Institute of Health (1998) Diagnosis and Treatment of Attention-Deficit/Hyperactivity Disorder. US Government Printing Office; NIH Consensus Statement 16(2), Washington DC
Newcorn J, Halperin J, Jensen P, et al. (2001) Symptoms profiles in children with ADHD: effects of comorbidity and gender. J Am Acad Child Adolesc Psychiatry 40:137–146
Perin JM, Stein MT, Amler RW, et al. (2000) Diagnosis and evaluation of the child with attention deficit/hyperactivity disorder. Paediatrics 105:1158–1170
Rohde LA (2002) ADHD in Brazil: The DSM-IV criteria in a culturally different population. J Am Acad Child Adolesc Psychiatry 41:1131–1133
Rohde LA, Szobot C, Polanczyk G, Schmitz M, Martins S, Tramontina S (2005) Attention-deficit/hyperactivity disorder in a diverse culture: do research and clinical findings support the notion of a cultural construct for the disorder? Biol Psychiatry 57:1436–1441
Scahill I, Schwab-Stone M (2000) Epidemiology of ADHD in school-age children. Child Adolesc Psychiatr Clin North America 9:541–555
Schaffer D, Fisher P, Lucas CP, Dulcan MK, Schwab-Stone ME (2000) NIMH Diagnostic Interview Schedule for Children version IV (NIMH DISC-IV): description differences from the previous versions, and reliability of some common diagnosis. J Am Acad Child Adolesc Psychiatry 39:28–38
Timimi S, Taylor E (2004) ADHD is best understood as a cultural construct. Br J Psychiatry 184:8–9
Wolraich ML, Hannah JN, Baumgaertal A, Feurer ID (1998) Examination of the DSM-IV criteria for attention-deficit/hyperactivity disorder in a countrywide sample. J Dev Behav Paediatr 19:162–168
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Adewuya, A.O., Famuyiwa, O.O. Attention deficit hyperactivity disorder among Nigerian primary school children Prevalence and co-morbid conditions. Eur Child Adolesc Psychiatry 16, 10–15 (2007). https://doi.org/10.1007/s00787-006-0569-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-006-0569-9