Abstract
Objectives
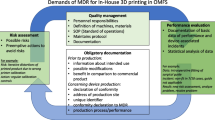
Oral and maxillofacial surgery (OMFS) has undergone pioneering progress through the development of three-dimensional (3D) printing technologies. The aim of this study was to evaluate the use of 3D printing at OMFS university and non-university hospitals and private practices in Germany.
Materials and methods
For explorative assessment, a dynamic online questionnaire containing 10–22 questions about the current use of 3D printing and the reasons behind it was sent to OMFS university and non-university hospitals and private practices in Germany by the study group from the German Association of Oral and Maxillofacial Surgery (DGMKG).
Results
In total, 156 participants responded from university (23 [14.7%]) and non-university hospitals (19 [12.2%]) and private practices without (85 [50.5%]) and with 29 (18.6%) inpatient treatment facility. Highest applications of 3D printing were in implantology (57%), microvascular bone reconstructions (25.6%), and orthognathics (21.1%). Among the participants, 37.8% reportedly were not using 3D printing. Among the hospitals and private practices, 21.1% had their own 3D printer, and 2.5% shared it with other departments. The major reason for not having a 3D printer was poor cost efficiency (37.6%). Possessing a 3D printer was motivated by independence from external providers (91.3%) and rapid template production (82.6%). The preferred printing methods were stereolithography (69.4 %) and filament printing (44.4%).
Conclusions
OMFS 3D printing is established in Germany with a wide range of applications.
Clinical relevance
The prevalence of 3D printing in hospitals and private practices is moderate. This may be enhanced by future innovations including improved cost efficiency.


Similar content being viewed by others
References
(1987) 4665492 Computer automated manufacturing process and system: William E Masters. Robot Comput Integr Manuf 3:i–ii. https://doi.org/10.1016/0736-5845(87)90060-3
Hull CW (1984) Apparatus for production of three-dimensional objects by stereolithography Patent US4575330A United States
Andre JC, Le Mehaute A, De Witte O (1984) Device for producing a model of an industrial part. French Patent FR 2:567–668
Tack P, Victor J, Gemmel P, Annemans L (2016) 3D-printing techniques in a medical setting: a systematic literature review. Biomed Eng Online 15:115. https://doi.org/10.1186/s12938-016-0236-4
Schubert C, van Langeveld MC, Donoso LA (2014) Innovations in 3D printing: a 3D overview from optics to organs. Br J Ophthalmol 98:159–161. https://doi.org/10.1136/bjophthalmol-2013-304446
Wren K (2013) Science and society. Experts warn against bans on 3D printing. Science 342(6157):439
Mertz L (2013) New world of 3-D printing offers “completely new ways of thinking”: Q&A with author, engineer, and 3-D printing expert Hod Lipson. IEEE Pulse 4:12–14. https://doi.org/10.1109/MPUL.2013.2279615
Marschall JS, Dutra V, Flint RL, Kushner GM, Alpert B, Azevedo B (2019) Expedited in-house virtual reduction, 3-D printing, and custom reconstruction plate adaptation for the management of acute mandible fractures. Int J Oral Maxillofac Surg 48:39. https://doi.org/10.1016/j.ijom.2019.03.119
Zeller AN, Neuhaus MT, Fresenborg S, Zimmerer RM, Jehn P, Spalthoff S, Gellrich NC, Dittmann JA (2020) Accurate and cost-effective mandibular biomodels: a standardized evaluation of 3D-printing via fused layer deposition modeling on soluble support structures. J Stomatol Oral Maxillofac Surg. https://doi.org/10.1016/j.jormas.2020.09.018
Ventola CL (2014) Medical applications for 3D printing: current and projected uses. P T 39:704–711
Andersson JL, Marcus M, Nomikos GG, Svensson TH (1994) Prazosin modulates the changes in firing pattern and transmitter release induced by raclopride in the mesolimbic, but not in the nigrostriatal dopaminergic system. Naunyn Schmiedeberg’s Arch Pharmacol 349:236–243. https://doi.org/10.1007/BF00169289
Abeliansky AL, Martínez-Zarzoso I, Prettner K (2020) 3D printing, international trade, and FDI. Econ Model 85:288–306. https://doi.org/10.1016/j.econmod.2019.10.014
Ganguli A, Pagan-Diaz GJ, Grant L, Cvetkovic C, Bramlet M, Vozenilek J, Kesavadas T, Bashir R (2018) 3D printing for preoperative planning and surgical training: a review. Biomed Microdevices 20:65. https://doi.org/10.1007/s10544-018-0301-9
Waran V, Narayanan V, Karuppiah R, Pancharatnam D, Chandran H, Raman R, Rahman ZA, Owen SL, Aziz TZ (2014) Injecting realism in surgical training-initial simulation experience with custom 3D models. J Surg Educ 71:193–197. https://doi.org/10.1016/j.jsurg.2013.08.010
Watson RA (2014) A low-cost surgical application of additive fabrication. J Surg Educ 71:14–17. https://doi.org/10.1016/j.jsurg.2013.10.012
Werz SM, Zeichner SJ, Berg BI, Zeilhofer HF, Thieringer F (2018) 3D printed surgical simulation models as educational tool by maxillofacial surgeons. Eur J Dent Educ 22:e500–e505. https://doi.org/10.1111/eje.12332
Lichtenstein JT, Zeller AN, Lemound J, Lichtenstein TE, Rana M, Gellrich NC, Wagner ME (2017) 3D-printed simulation device for orbital surgery. J Surg Educ 74:2–8. https://doi.org/10.1016/j.jsurg.2016.07.005
Petzold R, Zeilhofer HF, Kalender WA (1999) Rapid protyping technology in medicine--basics and applications. Comput Med Imaging Graph 23:277–284. https://doi.org/10.1016/s0895-6111(99)00025-7
Webb PA (2000) A review of rapid prototyping (RP) techniques in the medical and biomedical sector. J Med Eng Technol 24:149–153. https://doi.org/10.1080/03091900050163427
Winder J, Bibb R (2005) Medical rapid prototyping technologies: state of the art and current limitations for application in oral and maxillofacial surgery. J Oral Maxillofac Surg 63:1006–1015. https://doi.org/10.1016/j.joms.2005.03.016
Kamio T, Hayashi K, Onda T, Takaki T, Shibahara T, Yakushiji T, Shibui T, Kato H (2018) Utilizing a low-cost desktop 3D printer to develop a “one-stop 3D printing lab” for oral and maxillofacial surgery and dentistry fields. 3D Print Med 4:6. https://doi.org/10.1186/s41205-018-0028-5
Marschall JS, Dutra V, Flint RL, Kushner GM, Alpert B, Scarfe W, Azevedo B (2019) In-house digital workflow for the management of acute mandible fractures. J Oral Maxillofac Surg 77:2084 e1–2084 e9. https://doi.org/10.1016/j.joms.2019.05.027
Zeller AN, Neuhaus MT, Gessler N, Skade S, Korn P, Jehn P, Gellrich NC, Zimmerer RM (2020) Self-centering second-generation patient-specific functionalized implants for deep orbital reconstruction. J Stomatol Oral Maxillofac Surg. https://doi.org/10.1016/j.jormas.2020.12.007
Jehn P, Spalthoff S, Korn P, Zeller AN, Dittmann J, Zimmerer R, Tavassol F, Gellrich NC (2020) Patient-specific implant modification for alloplastic bridging of mandibular segmental defects in head and neck surgery. J Craniomaxillofac Surg 48:315–322. https://doi.org/10.1016/j.jcms.2020.01.018
Zeller AN, Neuhaus MT, Weissbach LVM, Rana M, Dhawan A, Eckstein FM, Gellrich NC, Zimmerer RM (2020) Patient-specific mandibular reconstruction plates increase accuracy and long-term stability in immediate alloplastic reconstruction of segmental mandibular defects. J Maxillofac Oral Surg 19:609–615. https://doi.org/10.1007/s12663-019-01323-9
Honigmann P, Sharma N, Okolo B, Popp U, Msallem B, Thieringer FM (2018) Patient-specific surgical implants made of 3D printed PEEK: material, technology, and scope of surgical application. Biomed Res Int 2018:4520636–4520638. https://doi.org/10.1155/2018/4520636
Rohner D, Guijarro-Martinez R, Bucher P, Hammer B (2013) Importance of patient-specific intraoperative guides in complex maxillofacial reconstruction. J Craniomaxillofac Surg 41:382–390. https://doi.org/10.1016/j.jcms.2012.10.021
De Mori A, Pena Fernandez M, Blunn G, Tozzi G, Roldo M (2018) 3D printing and electrospinning of composite hydrogels for cartilage and bone tissue engineering. Polymers (Basel) 10. https://doi.org/10.3390/polym10030285
Norman J, Madurawe RD, Moore CM, Khan MA, Khairuzzaman A (2017) A new chapter in pharmaceutical manufacturing: 3D-printed drug products. Adv Drug Deliv Rev 108:39–50. https://doi.org/10.1016/j.addr.2016.03.001
Pai D (2017) 3D-Printing skin is real: here’s what you need to know. Allure News. [Online]. Available https://www.allure.com/story/3d-printing-skin. Accessed 2020
Jacobs CA, Lin AY (2017) A new classification of three-dimensional printing technologies: systematic review of three-dimensional printing for patient-specific craniomaxillofacial surgery. Plast Reconstr Surg 139:1211–1220. https://doi.org/10.1097/PRS.0000000000003232
Lin AY, Yarholar LM (2020) Plastic surgery innovation with 3D printing for craniomaxillofacial operations. Mo Med 117:136–142
Pabst A, Thiem DGE, Goetze E, Bartella AK, Neuhaus MT, Hoffmann J, Zeller AN (2021) How is neck dissection performed in oral and maxillofacial surgery? Results of a representative nationwide survey among university and non-university hospitals in Germany. Clin Oral Investig 25:3007–3019. https://doi.org/10.1007/s00784-020-03622-9
Derksen W, Wismeijer D, Flugge T, Hassan B, Tahmaseb A (2019) The accuracy of computer-guided implant surgery with tooth-supported, digitally designed drill guides based on CBCT and intraoral scanning. A prospective cohort study. Clin Oral Implants Res 30:1005–1015. https://doi.org/10.1111/clr.13514
Mahendru S, Jain R, Aggarwal A, Aulakh HS, Jain A, Khazanchi RK, Sarin D (2020) CAD-CAM vs conventional technique for mandibular reconstruction with free fibula flap: a comparison of outcomes. Surg Oncol 34:284–291. https://doi.org/10.1016/j.suronc.2020.04.012
Geusens J, Sun Y, Luebbers HT, Bila M, Darche V, Politis C (2019) Accuracy of computer-aided design/computer-aided manufacturing-assisted mandibular reconstruction with a fibula free flap. J Craniofac Surg 30:2319–2323. https://doi.org/10.1097/SCS.0000000000005704
Tabakovic SZ, Konstantinovic VS, Radosavljevic R, Movrin D, Hadzistevic M, Hatab N (2015) Application of computer-aided designing and rapid prototyping technologies in reconstruction of blowout fractures of the orbital floor. J Craniofac Surg 26:1558–1563. https://doi.org/10.1097/SCS.0000000000001883
Krause M, Kamal M, Kruber D, Halama D, Hierl T, Lethaus B, Bartella AK (2021) Improved access in minimally invasive temporomandibular joint surgery through a novel endaural template. BMC Surg 21:93. https://doi.org/10.1186/s12893-021-01098-2
Park JH, Lee YB, Kim SY, Kim HJ, Jung YS, Jung HD (2019) Accuracy of modified CAD/CAM generated wafer for orthognathic surgery. PLoS One 14:e0216945. https://doi.org/10.1371/journal.pone.0216945
Oth O, Mestrallet P, Glineur R (2020) Clinical study on the minimally invasive-guided genioplasty using piezosurgery and 3D printed surgical guide. Ann Maxillofac Surg 10:91–95. https://doi.org/10.4103/ams.ams_79_19
Merema BJ, Kraeima J, Witjes MJH, van Bakelen NB, Spijkervet FKL (2021) Accuracy of fit analysis of the patient-specific Groningen temporomandibular joint prosthesis. Int J Oral Maxillofac Surg 50:538–545. https://doi.org/10.1016/j.ijom.2020.08.012
Zweifel DF, Simon C, Hoarau R, Pasche P, Broome M (2015) Are virtual planning and guided surgery for head and neck reconstruction economically viable? J Oral Maxillofac Surg 73:170–175. https://doi.org/10.1016/j.joms.2014.07.038
van Baar GJC, Forouzanfar T, Liberton N, Winters HAH, Leusink FKJ (2018) Accuracy of computer-assisted surgery in mandibular reconstruction: a systematic review. Oral Oncol 84:52–60. https://doi.org/10.1016/j.oraloncology.2018.07.004
Shilo D, Emodi O, Blanc O, Noy D, Rachmiel A (2018) Printing the future-updates in 3D printing for surgical applications. Rambam Maimonides Med J 9:e0020. https://doi.org/10.5041/RMMJ.10343
Hoang D, Perrault D, Stevanovic M, Ghiassi A (2016) Surgical applications of three-dimensional printing: a review of the current literature & how to get started. Ann Transl Med 4:456. https://doi.org/10.21037/atm.2016.12.18
Seifert LB, Schnurr B, Herrera-Vizcaino C, Begic A, Thieringer F, Schwarz F, Sader R (2020) 3D-printed patient individualised models vs cadaveric models in an undergraduate oral and maxillofacial surgery curriculum: comparison of student's perceptions. Eur J Dent Educ 24:799–806. https://doi.org/10.1111/eje.12522
Zheng YX, Yu DF, Zhao JG, Wu YL, Zheng B (2016) 3D printout models vs. 3D-rendered images: which is better for preoperative planning? J Surg Educ 73:518–523. https://doi.org/10.1016/j.jsurg.2016.01.003
Heller M, Bauer HK, Goetze E, Gielisch M, Ozbolat IT, Moncal KK, Rizk E, Seitz H, Gelinsky M, Schroder HC, Wang XH, Muller WE, Al-Nawas B (2016) Materials and scaffolds in medical 3D printing and bioprinting in the context of bone regeneration. Int J Comput Dent 19:301–321
Honigmann P, Sharma N, Schumacher R, Rueegg J, Haefeli M, Thieringer F (2021) In-Hospital 3D Printed scaphoid prosthesis using medical-grade polyetheretherketone (PEEK) biomaterial. Biomed Res Int 2021:1301028–1301027. https://doi.org/10.1155/2021/1301028
van de Vijfeijken S, Schreurs R, Dubois L, Becking AG (2019) The use of cranial resection templates with 3D virtual planning and PEEK patient-specific implants: a 3 year follow-up. J Craniomaxillofac Surg 47:542–547. https://doi.org/10.1016/j.jcms.2018.07.012
Haleem A, Javaid M, Vaish A, Vaishya R (2019) Three-dimensional-printed polyether ether ketone implants for orthopedics. Indian J Orthop 53:377–379. https://doi.org/10.4103/ortho.IJOrtho_499_18
Legocki AT, Duffy-Peter A, Scott AR (2017) Benefits and limitations of entry-level 3-dimensional printing of maxillofacial skeletal models. JAMA Otolaryngol Head Neck Surg 143:389–394. https://doi.org/10.1001/jamaoto.2016.3673
Meglioli M, Naveau A, Macaluso GM, Catros S (2020) 3D printed bone models in oral and cranio-maxillofacial surgery: a systematic review. 3D Print Med 6:30. https://doi.org/10.1186/s41205-020-00082-5
Zhuang YD, Zhou MC, Liu SC, Wu JF, Wang R, Chen CM (2019) Effectiveness of personalized 3D printed models for patient education in degenerative lumbar disease. Patient Educ Couns 102:1875–1881. https://doi.org/10.1016/j.pec.2019.05.006
Nicot R, Couly G, Ferri J, Levaillant JM (2018) Three-dimensional printed haptic model from a prenatal surface-rendered oropalatal sonographic view: a new tool in the surgical planning of cleft lip/palate. Int J Oral Maxillofac Surg 47:44–47. https://doi.org/10.1016/j.ijom.2017.06.005
Grall P, Ferri J, Nicot R (2021) Surgical training 2.0: A systematic approach reviewing the literature focusing on oral maxillofacial surgery - Part I. J Stomatol Oral Maxillofac Surg. https://doi.org/10.1016/j.jormas.2021.01.006
Cameron JL (1997) William Stewart Halsted. Our surgical heritage. Ann Surg 225:445–458. https://doi.org/10.1097/00000658-199705000-00002
Hanisch M, Kroeger E, Dekiff M, Timme M, Kleinheinz J, Dirksen D (2020) 3D-printed surgical training model based on real patient situations for dental education. Int J Environ Res Public Health 17. https://doi.org/10.3390/ijerph17082901
Murphy SV, Atala A (2014) 3D bioprinting of tissues and organs. Nat Biotechnol 32:773–785. https://doi.org/10.1038/nbt.2958
Ashammakhi N, Hasan A, Kaarela O, Byambaa B, Sheikhi A, Gaharwar AK, Khademhosseini A (2019) Advancing frontiers in bone bioprinting. Adv Healthc Mater 8:e1801048. https://doi.org/10.1002/adhm.201801048
Acknowledgements
We would like to thank all participants of the survey, the board, the academy, the scientific working group (AKWi), the professional organization of oral and maxillofacial surgeons, and all members and colleagues of the German Association of Oral and Maxillofacial Surgery (DGMKG). We owe a huge debt of gratitude to Professor and Dr. Max Heiland, the study administration, and the steering committee of the study administration of DGMKG for approving and supporting this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The study was conducted according to the principles of the Declaration of Helsinki. The study was approved by the study administration and the steering committee of the study administration of DGMKG. This study contains data from a survey that exclusively included oral and maxillofacial surgeons in Germany. Participation in this study was voluntary. None of the patients was included in the study. This article does not contain any studies on animals performed by any of the authors.
Consent to participate
Formal consent is not required for this type of study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pabst, A., Goetze, E., Thiem, D.G.E. et al. 3D printing in oral and maxillofacial surgery: a nationwide survey among university and non-university hospitals and private practices in Germany. Clin Oral Invest 26, 911–919 (2022). https://doi.org/10.1007/s00784-021-04073-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04073-6