Abstract
Background
Oral cancer progression is a multi-step process in which adhesion molecules play a pivotal role in the development of recurrent, invasive, and distant metastasis. The aim of this study was to adopt prognostic biomarkers to assess the lymph node metastasis of OSCC that will facilitate in deciding the treatment modality by the surgeons.
Objectives
The objectives of the study were to assess the biological behaviour of OSCC by correlating the expression levels of P-Cadherin and WNT5A immunohistochemically.
Methods
A total of 60 selected OSCCs cases (lymph node metastasis n = 30, non-metastatic n = 30) and 10 normal healthy controls were quantitatively and qualitatively analysed by immunohistochemistry for P-Cadherin and WNT5A. A survival analysis was also performed.
Results
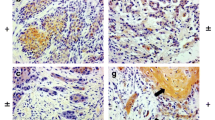
The expression levels of P-Cadherin and WNT5A in OSCC groups were statistically significant between metastatic and non-metastatic groups (p < 0.001). P-Cadherin and WNT5A expression in metastatic (lymph node metastasis) and non-metastatic cases showed a significant correlation coefficient of 0.753 at (p < 0.01). The present study also found that the aberrant expression (high) of P-Cadherin was associated with diminished survival of patients with metastatic OSCC.
Conclusion
The present study demonstrated the aberrant expression of P-Cadherin and WNT5A could serve as important prognosticator in OSCC.
Clinical relevance
P-Cadherin and WNT5A could be used as significant predictors of disease outcome.








Similar content being viewed by others
Abbreviations
- OSCC :
-
Oral squamous cell carcinoma
- WNT5A :
-
Wingless-Type 5A
- HNSCC :
-
Head and neck squamous cell carcinoma
- FFPE :
-
Formalin-fixed paraffin-embedded
- UICC :
-
Union for International Cancer Control
- EDTA :
-
Ethylene diamine tetra-acetic acid
- NOM :
-
Normal mucosa
- DAB :
-
Diamine-benzidine
References
Sathiyasekar AC, Chandrasekar P, Pakash A, Kumar KG, Jaishlal MS (2016) Overview of immunology of oral squamous cell carcinoma. J Pharm Bioallied Sci 8(Suppl 1):S8
Sklenicka S, Gardiner S, Dierks EJ, Potter BE, Bell RB (2010) Survival analysis and risk factors for recurrence in oral squamous cell carcinoma: does surgical salvage affect outcome? J Oral Maxillofac Surg 68(6):1270–1275
Kim MM, Califano JA (2004) Molecular pathology of head-and-neck cancer. Int J Cancer 112(4):545–553
Nguyen PT, Kudo Y, Yoshida M, Kamata N, Ogawa I, Takata T (2011) N-cadherin expression is involved in malignant behaviour of head and neck cancer in relation to epithelial-mesenchymal transition. Histol Histopathol 26(1):147
Kupferman ME, Patel V, Sriuranpong V, Amornphimoltham P, Jasser SA, Mandal M, Zhou G, Wang J, Coombes K, Multani A, Pathak S (2007) Molecular analysis of anoikis resistance in oral cavity squamous cell carcinoma. Oral Oncol 43(5):440–454
Muñoz-Guerra MF, Marazuela EG, Fernández-Contreras ME, Gamallo C (2005) P-cadherin expression reduced in squamous cell carcinoma of the oral cavity: An indicator of poor prognosis. Cancer 103(5):960–9
Yamamoto E, Miyakawa A, Kohama GI (1984) Mode of invasion and lymph node metastasis in squamous cell carcinoma of the oral cavity. Head Neck Surg 6(5):938–947
Mohammad DN, Garib BT, Khudeir HH, Abdul–Majeed BA. Immunohistochemical expression of P-cadherin and cortactin in oral squamous cell carcinomas
Meng W, Takeichi M (2009) Adherens junction: molecular architecture and regulation. Cold Spring Harb Perspect Biol 5:a002899
Nelson WJ, Nusse R (2004) Convergence of Wnt, ß-catenin, and cadherin pathways. Science 303(5663):1483–1487
Jiang WG, Sanders AJ, Katoh M, Ungefroren H, Gieseler F, Prince M, Thompson SK, Zollo M, Spano D, Dhawan P, Sliva D. Tissue invasion and metastasis: Molecular, biological and clinical perspectives. In Seminars in cancer biology 2015 Dec 1 (Vol. 35, pp. S244-S275). Academic Press
Vieira AF, Paredes J (2015) P-cadherin and the journey to cancer metastasis. Mol Cancer 14(1):178
McDonald SL, Silver A (2009) The opposing roles of Wnt-5a in cancer. Br J Cancer 101(2):209
Prgomet Z, Andersson T, Lindberg P (2017) Higher expression of WNT 5A protein in oral squamous cell carcinoma compared with dysplasia and oral mucosa with a normal appearance. Eur J Oral Sci 125(4):237–246
Qin L, Yin YT, Zheng FJ, Peng LX, Yang CF, Bao YN, Liang YY, Li XJ, Xiang YQ, Sun R, Li AH (2015) WNT5A promotes stemness characteristics in nasopharyngeal carcinoma cells leading to metastasis and tumorigenesis. Oncotarget 6(12):10239
Sun L, Hu H, Peng L, Zhou Z, Zhao X, Pan J, Sun L, Yang Z, Ran Y (2011) P-cadherin promotes liver metastasis and is associated with poor prognosis in colon cancer. Am J Pathol 179(1):380–390
Rasbridge SA, Gillett CE, Sampson SA, Walsh FS, Millis RR (1993) Epithelial (E-) and placentae (P-) cadherin cell adhesion molecule expression in breast carcinoma. J Pathol 169(2):245–250
Palacios J, Benito N, Pizarro A, Suárez A, Espada J, Cano A, Gamallo C (1995) Anomalous expression of P-cadherin in breast carcinoma. Correlation with E-cadherin expression and pathological features. The American journal of pathology 146(3):605
Zhu N, Qin L, Luo Z, Guo Q, Yang L, Liao D (2014) Challenging role of Wnt5a and its signaling pathway in cancer metastasis. Exp Ther Med 8(1):3–8
Bo H, Zhang S, Gao L, Chen Y, Zhang J, Chang X, Zhu M (2013) Upregulation of Wnt5a promotes epithelial-to-mesenchymal transition and metastasis of pancreatic cancer cells. BMC Cancer 13(1):496
Shimoyama Y, Hirohashi S (1991) Expression of E-and P-cadherin in gastric carcinomas. Can Res 51(8):2185–2192
Paredes J, Albergaria A, Oliveira JT, Jerónimo C, Milanezi F, Schmitt FC (2005) P-cadherin overexpression is an indicator of clinical outcome in invasive breast carcinomas and is associated with CDH3 promoter hypomethylation. Clin Cancer Res 11(16):5869–5877
Muzio LL, Campisi G, Farina A, Rubini C, Pannone G, Serpico R, Laino G, De Lillo A, Carinci F (2005) P-cadherin expression and survival rate in oral squamous cell carcinoma: an immunohistochemical study. BMC Cancer 5(1):63
Bauer K, Gosau M, Reinders J, Oefner P, Reichert TE, Bauer R (2013) Presenilin 1/γ-secretase modulates P-cadherin processing and influences cell adhesion in oral squamous cell carcinoma cell lines. Carcinogenesis 34(11):2622–2628
Mandeville JA, Neto BS, Vanni AJ, Smith GL, Rieger-Christ KM, Zeheb R, Loda M, Libertino JA, Summerhayes IC (2008) P-cadherin as a prognostic indicator and a modulator of migratory behaviour in bladder carcinoma cells. BJU Int 102(11):1707–1714
Paredes J, Correia AL, Ribeiro AS, Milanezi F, Cameselle-Teijeiro J, Schmitt FC (2008) Breast carcinomas that co-express E-and P-cadherin are associated with p120-catenin cytoplasmic localization and poor patient survival. J Clin Pathol
Noguti J, De Moura CF, De Jesus GP, Da Silva VH, Hossaka TA, Oshima CT, Ribeiro DA (2012) Metastasis from oral cancer: an overview. Cancer Genomics-Proteomics 9(5):329–335
Bauer R, Dowejko A, Driemel O, Boberhoff AK, Reichert TE (2008) Truncated P-cadherin is produced in oral squamous cell carcinoma. FEBS J 275(16):4198–4210
Peixoto TS, Gomes MC, de Castro Gomes DQ, Lima KC, Granville-Garcia AF, de Brito Costa EM (2017) Analysis of survival rates and prognostic factors among patients with oral squamous cell carcinoma. J Public Health 25(4):433–441
Janot F, Klijanienko J, Russo A, Mamet JP, De Braud F, El-Naggar AK, Pignon JP, Luboinski B, Cvitkovic E (1996) Prognostic value of clinicopathological parameters in head and neck squamous cell carcinoma: a prospective analysis. Br J Cancer 73(4):531
Pires FR, Ramos AB, Oliveira JB, Tavares AS, Luz PS, Santos TC (2013) Oral squamous cell carcinoma: clinicopathological features from 346 cases from a single oral pathology service during an 8-year period. J Appl Oral Sci 21(5):460–467
Hutchins LF, Unger JM, Crowley JJ, Coltman CA Jr, Albain KS (1999) Underrepresentation of patients 65 years of age or older in cancer-treatment trials. N Engl J Med 341(27):2061–2067
Feller LL, Khammissa RR, Kramer BB, Lemmer JJ (2013) Oral squamous cell carcinoma in relation to field precancerisation: pathobiology. Cancer Cell Int 13(1):31
Abraham M, Sowmya SV, Rao RS, Haragannavar VC, Patil S, Augustine D, Nambiar S (2018) Stearoyl coenzyme A desaturase: A diagnostic and prognostic biomarker in patients with oral epithelial dysplasia and oral squamous cell carcinoma. Translational Research in Oral Oncology 3:2057178X18782512
Bundgaard T, Bentzen SM, Wildt J, Sorensen FB, Søgaard H, Nielsen JE (1996) Histopathologic, stereologic, epidemiologic, and clinical parameters in the prognostic evaluation of squamous cell carcinoma of the oral cavity. Head Neck 18(2):142–152
Mehta V, Yu GP, Schantz SP (2010) Population-based analysis of oral and oropharyngeal carcinoma: changing trends of histopathologic differentiation, survival and patient demographics. Laryngoscope 120(11):2203–2212
Kantola S, Parikka M, Jokinen K, Hyrynkangs K, Soini Y, Alho OP, Salo T (2000) Prognostic factors in tongue cancer–relative importance of demographic, clinical and histopathological factors. Br J Cancer 83(5):614
Gravdal K, Halverson OJ, Haukaas SA, Akslen LA (2007) A switch from E-cadherin to N-cadherin expression indicates epithelial to mesenchymal transition and is of strong and independent importance for the progress of prostate cancer. Clin Cancer Res 13(23):7003–7011
Yi S, Yang ZL, Miao X, Zou Q, Li J, Liang L, Zeng G, Chen S (2014) N-cadherin and P-cadherin are biomarkers for invasion, metastasis, and poor prognosis of gallbladder carcinomas. Pathology-Research and Practice 210(6):363–368
Adamczyk A, Niemiec J, Ambicka A, Małecki K, Wysocki WH, Mitus J, Rys J (2012) Expression of ER/PR/HER2, basal markers and adhesion molecules in primary breast cancer and in lymph nodes metastases: a comparative immunohistochemical analysis. Pol J Pathol 63(4):228–234
Acknowledgements
The authors thank Dr. Saman Warnakulasuriya, Professor, Department of Oral Medicine, King’s College London, UK, for his valuable suggestions. The authors thank Dr. Puneet Gupta for performing the statistical analysis
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Khan, W., Haragannavar, V.C., Rao, R.S. et al. P-Cadherin and WNT5A expression in assessment of lymph node metastasis in oral squamous cell carcinoma. Clin Oral Invest 26, 259–273 (2022). https://doi.org/10.1007/s00784-021-03996-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-03996-4