Abstract
Objectives
Stable and appropriate condyle positioning is necessary for maintaining temporomandibular joint function. It is unclear if this position remains stable in patients after free fibular flap (FFF) condylar reconstruction. We investigated whether condylar position deviated after reconstruction, and whether this affected functional recovery.
Materials and methods
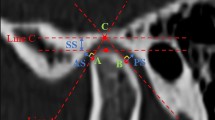
We retrospectively reviewed 43 patients who underwent conventional FFF condylar reconstruction, and 5 patients who underwent reconstruction by computer-assisted three-dimensional (3D) printing methods. Three-dimensional models were built from cone-beam computed tomography images obtained immediately postoperatively and 1-year postoperatively. The glenoid fossa and fibular condyle centers were used to measure the fibular condyle position in the models. Clinical examination indices, including maximum mouth opening (MMO), pain during chewing/mouth opening, and patient satisfaction with mastication and 1-year outcomes were assessed.
Results
Fibular condyle position changed significantly over 1 year in both groups (P < 0.05). Clinical examination at 1 year after the surgery showed that in the conventional group, the MMO range was ≥ 35 mm in 76.7% of patients and < 35 mm in 23.3% of patients; 4.7% experienced pain during chewing/mouth opening, and 7% were dissatisfied with treatment outcomes. In the 3D printing group, all patients had an MMO range exceeding 35 mm, none had pain, and all were satisfied with functional outcomes.
Conclusions
The position of the fibular condyle deviates after reconstructive surgery, but it is unlikely to affect functional recovery.
Clinical relevance
These findings can form the basis for evaluation of functional outcomes of patients who have previously undergone condylar reconstruction by FFF.



Similar content being viewed by others
References
Weinberg LA (1979) An evaluation of occlusal factors in TMJ dysfunction-pain syndrome. J Prosthet Dent 41(2):198–208
Blaschke DD, Solberg WK, Sanders B (1980) Arthrography of the temporomandibular joint: review of current status. J Am Dent Assoc 100(3):388–395
Shokri T, Stahl LE, Kanekar SG, Goyal N (2019) Osseous changes over time in free fibular flap reconstruction. Laryngoscope 129(5):1113–1116
Shen Y, Guo XH, Sun J, Li J, Shi J, Huang W, Ow A (2013) Double-barrel vascularised fibula graft in mandibular reconstruction: a 10-year experience with an algorithm. J Plast Reconstr Aesthet Surg 66(3):364–371
Kim J-W, Hwang J-H, Ahn K-M (2016) Fibular flap for mandible reconstruction in osteoradionecrosis of the jaw: selection criteria of fibula flap. Maxillofac Plast Reconstr Surg 38(1):46
Gravvanis A, Anterriotis D, Kakagia D (2017) Mandibular condyle reconstruction with fibula free-tissue transfer: the role of the masseter muscle. J Craniofac Surg 28(8):1955–1959
Wilson KM, Rizk NM, Armstrong SL, Gluckman JL (1998) Effects of hemimandibulectomy on quality of life. Laryngoscope 108(10):1574–1577
Schliephake H, Neukam FW, Schmelzeisen R, Varoga B, Schneller H (1995) Long-term quality of life after ablative intraoral tumour surgery. J Cranio-Maxillofac Surg 23(4):243–249
Colletti G, Autelitano L, Rabbiosi D, Biglioli F, Chiapasco M, Mandalà M, Allevi F (2014) Technical refinements in mandibular reconstruction with free fibula flaps: outcome-oriented retrospective review of 99 cases. Acta Otorhinolaryngol Ital 34(5):342–348
Chao JW et al (2014) Oral rehabilitation outcomes after free fibula reconstruction of the mandible without condylar restoration. J Craniofac Surg 25(2):415–417
Obregon F et al (2015) Three-dimensional bioprinting for regenerative dentistry and craniofacial tissue engineering. J Dental Res 94(9_suppl):143S–152S
Derby B (2012) Printing and prototyping of tissues and scaffolds. Science 338(6109):921–926
Avraham T et al (2014) Functional outcomes of virtually planned free fibula flap reconstruction of the mandible. Plastic Reconstr Surg 134(4):628e–634e
Yoshimura H, Matsuda S, Ohba S, Minegishi Y, Nakai K, Fujieda S, Sano K (2017) Stereolithographic model-assisted reconstruction of the mandibular condyle with a vascularized fibular flap following hemimandibulectomy: evaluation of morphological and functional outcomes. Oncol Lett 14(5):5471–5483
Modabber A, Legros C, Rana M, Gerressen M, Riediger D, Ghassemi A (2012) Evaluation of computer-assisted jaw reconstruction with free vascularized fibular flap compared to conventional surgery: a clinical pilot study. Int J Med Robot Comput Assisted Surg 8(2):215–220
Li KK, Cheney ML, Teknos TN (1996) The importance of mandibular position in microvascular mandibular reconstruction. Laryngoscope 106(7):903–907
Yu Y et al (2016) Three-dimensional accuracy of virtual planning and surgical navigation for mandibular reconstruction with free fibula flap. J Oral Maxillofac Surg 74(7):1503 e1–1503 e10
Nahabedian MY, Tufaro A, Manson PN (2001) Improved mandible function after hemimandibulectomy, condylar head preservation, and vascularized fibular reconstruction. Ann Plast Surg 46(5):506–510
Taylor G et al (1975) The free vascularized bone graft. A clinical extension of microvascular techniques. Plast Reconstr Surg 55(5):533–544
Hidalgo DA (1989) Fibula free flap: a new method of mandible reconstruction. Plast Reconstr Surg 84(1):71–79
González-García R et al (2008) Vascularized fibular flap for reconstruction of the condyle after mandibular ablation. J Oral Maxillofac Surg 66(6):1133–1137
Yoshimura H et al (2017) Stereolithographic model-assisted reconstruction of the mandibular condyle with a vascularized fibular flap following hemimandibulectomy: evaluation of morphological and functional outcomes. Oncol Lett 14(5):5471–5483
Tecco S, Saccucci M, Nucera R, Polimeni A, Pagnoni M, Cordasco G, Festa F, Iannetti G (2010) Condylar volume and surface in Caucasian young adult subjects. BMC Med Imaging 10(1):28
Gerbino G, Boffano P, Tosco P, Berrone S (2009) Long-term clinical and radiological outcomes for the surgical treatment of mandibular condylar fractures. J Oral Maxillofac Surg 67(5):1009–1014
Walker RV (1994) Condylar fractures: nonsurgical management. J Oral Maxillofac Surg 52(11):1185–1188
Casanova-Rosado JF, Medina-Solís CE, Casanova-Rosado AJ, Vallejos-Sánchez AA, Patiño-Marín N, Maupome G, Gomez-Gomez V (2012) Clinical characterization of mouth opening among Mexican adolescents and young adults. J Dent Sci 7(1):81–84
Sefidroodi M, Lobekk OK, Løes S, Schilbred Eriksen E (2019) Temporomandibular joint function 10-15 years after mandibular setback surgery and six weeks of intermaxillary fixation. J Appl Oral Sci 27
Kaur S, Datta K (2018) An in vitro study to evaluate the accuracy of orthopantomograph as an aid to determine condylar guidance. J Indian Prosthodont Soc 18(1):35–41
van Vlijmen OJ et al (2009) Comparison of cephalometric radiographs obtained from cone-beam computed tomography scans and conventional radiographs. J Oral Maxillofac Surg 67(1):92–97
Li X-Y, Jia C, Zhang Z-C (2017) The normal range of maximum mouth opening and its correlation with height or weight in the young adult Chinese population. J Dent Sci 12(1):56–59
Wang W et al (2013) Three-dimensional virtual technology in reconstruction of mandibular defect including condyle using double-barrel vascularized fibula flap. J Cranio-Maxillofac Surg 41(5):417–422
Perrott DH, Umeda H, Kaban LB (1994) Costochondral graft construction/reconstruction of the ramus/condyle unit: long-term follow-up. Int J Oral Maxillofac Surg 23(6):321–328
Ko EW-C, Huang C-S, Chen Y-R (1999) Temporomandibular joint reconstruction in children using costochondral grafts. J Oral Maxillofac Surg 57(7):789–798
González-García R, Naval-Gías L, Rodríguez-Campo FJ, Martínez-Chacón JL, Gil-Díez Usandizaga JL (2008) Vascularized fibular flap for reconstruction of the condyle after mandibular ablation. J Oral Maxillofac Surg 66(6):1133–1137
Hanasono MM, Militsakh ON, Richmon JD, Rosenthal EL, Wax MK (2013) Mandibulectomy and free flap reconstruction for bisphosphonate-related osteonecrosis of the jaws. JAMA Otolaryngol Head Neck Surg 139(11):1135–1142
Deganello A, Gitti G, Struijs B, Paiar F, Gallo O (2013) Palliative combined treatment for unresectable cutaneous basosquamous cell carcinoma of the head and neck. Acta Otorhinolaryngol Ital 33(5):353–356
Yu Y et al (2016) Three-dimensional accuracy of virtual planning and surgical navigation for mandibular reconstruction with free fibula flap. J Oral Maxillofac Surg 74(7):1503. e1–1503. e10
Makiguchi T, Yokoo S, Hashikawa K, Miyazaki H, Terashi H (2015) Evaluation of bone height of the free fibula flap in mandible reconstruction. J Craniofac Surg 26(3):673–676
Hidalgo DA, Pusic AL (2002) Free-flap mandibular reconstruction: a 10-year follow-up study. Plast Reconstr Surg 110(2):438–449 discussion 450-1
Wilkman T, Apajalahti S, Wilkman E, Törnwall J, Lassus P (2017) A comparison of bone resorption over time: an analysis of the free scapular, iliac crest, and fibular microvascular flaps in mandibular reconstruction. J Oral Maxillofac Surg 75(3):616–621
Beumer J III, Marunick MT, Esposito SJ (2011) Maxillofacial rehabilitation: prosthodontic and surgical management of cancer-related, acquired, and congenital defects of the head and neck. 276
Bolzoni A, Mapelli A, Baj A, Sidequersky FV, Giannì AB, Sforza C (2015) Evaluation of three-dimensional mandibular movements after reconstruction with free fibula flap. Acta Otorhinolaryngol Ital 35(6):371–378
Engroff SL (2005) Fibula flap reconstruction of the condyle in disarticulation resections of the mandible: a case report and review of the technique. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol 100(6):661–665
Funding
This work was supported by the National Natural Science Foundation of China (81360403), the Medical and Health Appropriate Technology Development and Promotion Project of Guangxi Province (S2018067), and Guangxi Nature Science Foundation (2019GXNSFAA185054).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The research was approved by the Ethics Committee of Guangxi Medical University (20130305-12). Informed consent was provided by all patients.
Patient consent for publication
Informed permission for publication was acquired from all patients.
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Table S1
(DOCX 14 kb)
Rights and permissions
About this article
Cite this article
Tang, Q., Li, Y., Yu, T. et al. Association between condylar position changes and functional outcomes after condylar reconstruction by free fibular flap. Clin Oral Invest 25, 95–103 (2021). https://doi.org/10.1007/s00784-020-03338-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03338-w