Abstract
Objectives
Suppression of periodontal pathogens in the oral cavity of periodontally healthy individuals may lower the risk for periodontal or periimplant diseases. Therefore, the present study aimed to analyze the effect of supragingival debridement (SD) with adjunctive full mouth glycine powder air polishing (FM-GPAP) on the prevalence of periodontal pathogens in periodontally healthy individuals.
Materials and Methods
Eighty-seven systemically and periodontally healthy intraoral carriers of red complex bacteria, i.e., Porphyromonas gingivalis, Tannerella forsythia, and Treponema denticola or other periodontal pathogens including Aggregatibacter actinomycetemcomitans, Prevotella intermedia, and Eikenella corrodens were enrolled into the study and randomly assigned to receive SD with adjunctive FM-GPAP (test, n = 42) or SD alone (control, n = 45). In the first observation period, microbiological samples were obtained prior to, and 2, 5, and 9 days following intervention. If one of these periodontal pathogens could still not be identified, additional microbial sampling was performed after 6 and 12 weeks.
Results
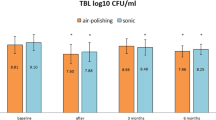
The prevalence of red complex bacteria was significantly reduced in the test compared to the control group following treatment (p = 0.004) and at day 9 (p = 0.031). Intragroup comparison showed a significant (test, p < 0.001; control, p ≤ 0.01) reduction in the mean prevalence in both groups from BL through day 9 with an additional significant intergroup difference (p = 0.048) at day 9. However, the initial strong reduction returned to baseline values after 6 and 12 weeks.
Conclusion
In periodontally healthy carriers of periodontal pathogens, FM-GPAP as an adjunct to SD transiently enhances the suppression of red complex bacteria.
Clinical relevance
Whether the enhanced suppression of red complex bacteria by adjunctive FM-GPAP prevents the development of periodontitis in periodontally healthy carriers requires further investigations.





Similar content being viewed by others
References
Zee KY (2009) Smoking and periodontal disease. Aust Dent J 54(Suppl 1):S44–S50. https://doi.org/10.1111/j.1834-7819.2009.01142.x
Genco RJ, Borgnakke WS (2013) Risk factors for periodontal disease. Periodontol 2000 62:59–94. https://doi.org/10.1111/j.1600-0757.2012.00457.x
Clark WB, Loe H (1993) Mechanisms of initiation and progression of periodontal disease. Periodontol 2000 2:72–82
Darveau RP, Tanner A, Page RC (1997) The microbial challenge in periodontitis. Periodontol 2000 14:12–32
Flemmig TF, Beikler T (2011) Control of oral biofilms. Periodontol 2000 55:9–15. https://doi.org/10.1111/j.1600-0757.2010.00383.x
Pozhitkov AE, Leroux BG, Randolph TW, Beikler T, Flemmig TF, Noble PA (2015) Towards microbiome transplant as a therapy for periodontitis: an exploratory study of periodontitis microbial signature contrasted by oral health, caries and edentulism. BMC Oral Health 15:125
Rafiei M, Kiani F, Sayehmiri K, Sayehmiri F, Tavirani M, Dousti M, Sheikhi A (2018) Prevalence of anaerobic bacteria (P.gingivalis) as major microbial agent in the incidence periodontal diseases by meta-analysis. J Dent (Shiraz) 19:232–242
Nadkarni MA, Chhour KL, Browne GV, Byun R, Nguyen KA, Chapple CC, Jacques NA, Hunter N (2015) Age-dependent changes in Porphyromonas gingivalis and Prevotella species/phylotypes in healthy gingiva and inflamed/diseased sub-gingival sites. Clin Oral Investig 19:911–919. https://doi.org/10.1007/s00784-014-1301-7
Aruni AW, Dou Y, Mishra A, Fletcher HM (2015) The Biofilm Community-Rebels with a Cause. Curr Oral Health Rep 2:48–56
Kinane DF, Galicia JC, Gorr SU, Stathopoulou PG, Benakanakere M (2008) P. gingivalis interactions with epithelial cells. Front Biosci 13:966–984
Lamont RJ, Hajishengallis G (2015) Polymicrobial synergy and dysbiosis in inflammatory disease. Trends Mol Med 21:172–183
Aas JA, Paster BJ, Stokes LN, Olsen I, Dewhirst FE (2005) Defining the normal bacterial flora of the oral cavity. J Clin Microbiol 43:5721–5732
Duran-Pinedo AE, Baker VD, Frias-Lopez J (2014) The periodontal pathogen Porphyromonas gingivalis induces expression of transposases and cell death of Streptococcus mitis in a biofilm model. Infect Immun 82:3374–3382
Bosshardt DD (2018) The periodontal pocket: pathogenesis, histopathology and consequences. Periodontol 2000 76:43–50. https://doi.org/10.1111/prd.12153
Mineoka T, Awano S, Rikimaru T, Kurata H, Yoshida A, Ansai T, Takehara T (2008) Site-specific development of periodontal disease is associated with increased levels of Porphyromonas gingivalis, Treponema denticola, and Tannerella forsythia in subgingival plaque. J Periodontol 79:670–676. https://doi.org/10.1902/jop.2008.070398
Yao ES, Lamont RJ, Leu SP, Weinberg A (1996) Interbacterial binding among strains of pathogenic and commensal oral bacterial species. Oral Microbiol Immunol 11:35–41
Kolenbrander PE, Andersen RN (1989) Inhibition of coaggregation between Fusobacterium nucleatum and Porphyromonas (Bacteroides) gingivalis by lactose and related sugars. Infect Immun 57:3204–3209
Kolenbrander PE, Palmer RJ Jr, Rickard AH, Jakubovics NS, Chalmers NI, Diaz PI (2006) Bacterial interactions and successions during plaque development. Periodontol 2000 42:47–79. https://doi.org/10.1111/j.1600-0757.2006.00187.x
Abusleme L, Dupuy AK, Dutzan N, Silva N, Burleson JA, Strausbaugh LD, Gamonal J, Diaz PI (2013) The subgingival microbiome in health and periodontitis and its relationship with community biomass and inflammation. ISME J 7:1016–1025
Riep B, Edesi-Neuss L, Claessen F, Skarabis H, Ehmke B, Flemmig TF, Bernimoulin JP, Gobel UB, Moter A (2009) Are putative periodontal pathogens reliable diagnostic markers? J Clin Microbiol 47:1705–1711
Beikler T, Abdeen G, Schnitzer S, Salzer S, Ehmke B, Heinecke A, Flemmig TF (2004) Microbiological shifts in intra- and extraoral habitats following mechanical periodontal therapy. J Clin Periodontol 31:777–783. https://doi.org/10.1111/j.1600-051X.2004.00557.x
Beikler T, Schnitzer S, Abdeen G, Ehmke B, Eisenacher M, Flemmig TF (2006) Sampling strategy for intraoral detection of periodontal pathogens before and following periodontal therapy. J Periodontol 77:1323–1332. https://doi.org/10.1902/jop.2006.050204
Ximenez-Fyvie LA, Haffajee AD, Socransky SS (2000) Comparison of the microbiota of supra- and subgingival plaque in health and periodontitis. J Clin Periodontol 27:648–657
Carrouel F, Viennot S, Santamaria J, Veber P, Bourgeois D (2016) Quantitative molecular detection of 19 major pathogens in the interdental biofilm of periodontally healthy young adults. Front Microbiol 7:840
Tallarico M, Canullo L, Caneva M, Ozcan M (2017) Microbial colonization at the implant-abutment interface and its possible influence on periimplantitis: a systematic review and meta-analysis. J Prosthodont Res 61:233–241. https://doi.org/10.1016/j.jpor.2017.03.001
Jervoe-Storm PM, Jepsen S, Johren P, Mericske-Stern R, Enkling N (2015) Internal bacterial colonization of implants: association with peri-implant bone loss. Clin Oral Implants Res 26:957–963. https://doi.org/10.1111/clr.12421
Keller W, Bragger U, Mombelli A (1998) Peri-implant microflora of implants with cemented and screw retained suprastructures. Clin Oral Implants Res 9:209–217
Leonhardt A, Dahlen G, Renvert S (2003) Five-year clinical, microbiological, and radiological outcome following treatment of peri-implantitis in man. J Periodontol 74:1415–1422. https://doi.org/10.1902/jop.2003.74.10.1415
Flemmig TF, Hetzel M, Topoll H, Gerss J, Haeberlein I, Petersilka G (2007) Subgingival debridement efficacy of glycine powder air polishing. J Periodontol 78:1002–1010. https://doi.org/10.1902/jop.2007.060420
Pelka MA, Altmaier K, Petschelt A, Lohbauer U (2010) The effect of air-polishing abrasives on wear of direct restoration materials and sealants. J Am Dent Assoc 141:63–70
Petersilka G, Faggion CM Jr, Stratmann U, Gerss J, Ehmke B, Haeberlein I, Flemmig TF (2008) Effect of glycine powder air-polishing on the gingiva. J Clin Periodontol 35:324–332. https://doi.org/10.1111/j.1600-051X.2007.01195.x
Petersilka GJ (2011) Subgingival air-polishing in the treatment of periodontal biofilm infections. Periodontol 2000 55:124–142. https://doi.org/10.1111/j.1600-0757.2010.00342.x
Charles CJ, Charles AH (1994) Periodontal screening and recording. J Calif Dent Assoc 22:43–46
Ainamo J, Barmes D, Beagrie G, Cutress T, Martin J, Sardo-Infirri J (1982) Development of the World Health Organization (WHO) community periodontal index of treatment needs (CPITN). Int Dent J 32:281–291
Saxer UPM, R H (1975) Motivation and education. SSO Schweiz Monatsschr Zahnheilkd 85:905–919
Lange DEP, C H, Eenboom A, Promesberger A (1977) Clinical methods for the objective evaluation of oral hygiene. Dtsch Zahnarztl Z 32:44–47
Ashimoto A, Chen C, Bakker I, Slots J (1996) Polymerase chain reaction detection of 8 putative periodontal pathogens in subgingival plaque of gingivitis and advanced periodontitis lesions. Oral Microbiol Immunol 11:266–273
Stubbs SL, Brazier JS, O'Neill GL, Duerden BI (1999) PCR targeted to the 16S-23S rRNA gene intergenic spacer region of Clostridium difficile and construction of a library consisting of 116 different PCR ribotypes. J Clin Microbiol 37:461–463
Quirynen M, De Soete M, Dierickx K, van Steenberghe D (2001) The intra-oral translocation of periodontopathogens jeopardises the outcome of periodontal therapy. A review of the literature. J Clin Periodontol 28:499–507
Leblebicioglu B, Kulekci G, Ciftci S, Keskin F, Badur S (2009) Salivary detection of periodontopathic bacteria and periodontal health status in dental students. Anaerobe 15:82–86. https://doi.org/10.1016/j.anaerobe.2008.12.005
Socransky SS, Haffajee AD, Cugini MA, Smith C, Kent RL Jr (1998) Microbial complexes in subgingival plaque. J Clin Periodontol 25:134–144
Tan KH, Seers CA, Dashper SG, Mitchell HL, Pyke JS, Meuric V, Slakeski N, Cleal SM, Chambers JL, McConville MJ, Reynolds EC (2014) Porphyromonas gingivalis and Treponema denticola exhibit metabolic symbioses. PLoS Pathog 10:e1003955
Tanner A, Maiden MF, Macuch PJ, Murray LL, Kent RL Jr (1998) Microbiota of health, gingivitis, and initial periodontitis. J Clin Periodontol 25:85–98
Thurnheer T, Belibasakis GN, Bostanci N (2014) Colonisation of gingival epithelia by subgingival biofilms in vitro: role of “red complex” bacteria. Arch Oral Biol 59:977–986. https://doi.org/10.1016/j.archoralbio.2014.05.023
Hajishengallis G, Liang S, Payne MA, Hashim A, Jotwani R, Eskan MA, McIntosh ML, Alsam A, Kirkwood KL, Lambris JD, Darveau RP, Curtis MA (2011) Low-abundance biofilm species orchestrates inflammatory periodontal disease through the commensal microbiota and complement. Cell Host Microbe 10:497–506
Nussbaum G, Shapira L (2011) How has neutrophil research improved our understanding of periodontal pathogenesis? J Clin Periodontol 38(Suppl 11):49–59. https://doi.org/10.1111/j.1600-051X.2010.01678.x
van Winkelhoff AJ, Rams TE, Slots J (1996) Systemic antibiotic therapy in periodontics. Periodontol 2000 10:45–78
Jepsen K, Jepsen S (2016) Antibiotics/antimicrobials: systemic and local administration in the therapy of mild to moderately advanced periodontitis. Periodontol 2000 71:82–112. https://doi.org/10.1111/prd.12121
Badersten A, Nilveus R, Egelberg J (1981) Effect of nonsurgical periodontal therapy. I. Moderately advanced periodontitis. J Clin Periodontol 8:57–72
Wilder-Smith P, Arrastia AM, Schell MJ, Liaw LH, Grill G, Berns MW (1995) Effect of ND:YAG laser irradiation and root planing on the root surface: structural and thermal effects. J Periodontol 66:1032–1039. https://doi.org/10.1902/jop.1995.66.12.1032
Flemmig TF, Arushanov D, Daubert D, Rothen M, Mueller G, Leroux BG (2012) Randomized controlled trial assessing efficacy and safety of glycine powder air polishing in moderate-to-deep periodontal pockets. J Periodontol 83:444–452. https://doi.org/10.1902/jop.2011.110367
Mussano F, Rovasio S, Schierano G, Baldi I, Carossa S (2013) The effect of glycine-powder airflow and hand instrumentation on peri-implant soft tissues: a split-mouth pilot study. Int J Prosthodont 26:42–44
Eick S, Pfister W (2004) Efficacy of antibiotics against periodontopathogenic bacteria within epithelial cells: an in vitro study. J Periodontol 75:1327–1334. https://doi.org/10.1902/jop.2004.75.10.1327
Matsunaga T, Nakayuki A, Saito Y, Kato A, Noiri Y, Ebisu S, Azakami H (2011) Genomic recombination through plasmid-encoded recombinase enhances hemolytic activity and adherence to epithelial cells in the periodontopathogenic bacterium Eikenella corrodens. Biosci Biotechnol Biochem 75:748–751. https://doi.org/10.1271/bbb.100866
Longo PL, Nunes AC, Umeda JE, Mayer MP (2013) Gene expression and phenotypic traits of Aggregatibacter actinomycetemcomitans in response to environmental changes. J Periodontal Res 48:766–772. https://doi.org/10.1111/jre.12067
Ebersole JL, Dawson DR 3rd, Morford LA, Peyyala R, Miller CS, Gonzalez OA (2013) Periodontal disease immunology: ‘double indemnity’ in protecting the host. Periodontol 2000 62:163–202
Periasamy S, Kolenbrander PE (2009) Mutualistic biofilm communities develop with Porphyromonas gingivalis and initial, early, and late colonizers of enamel. J Bacteriol 191:6804–6811
Bollen CM, Quirynen M (1996) Microbiological response to mechanical treatment in combination with adjunctive therapy: a review of the literature. J Periodontol 67:1143–1158. https://doi.org/10.1902/jop.1996.67.11.1143
Fang H, Han M, Li QL, Cao CY, Xia R, Zhang ZH (2016) Comparison of full-mouth disinfection and quadrant-wise scaling in the treatment of adult chronic periodontitis: a systematic review and meta-analysis. J Periodontal Res 51:417–430. https://doi.org/10.1111/jre.12326
Eberhard J, Jepsen S, Jervoe-Storm PM, Needleman I, Worthington HV (2015) Full-mouth treatment modalities (within 24 hours) for chronic periodontitis in adults. Cochrane Database Syst Rev:CD004622. https://doi.org/10.1002/14651858.CD004622.pub3
Funding
The follow-up was funded by the authors own departments.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Thomas Flemmig is an inventor with patents covering the fine-grain, low-abrasive glycine powder used in the present study. To safeguard against the conduct and outcomes of the clinical trial being influenced by a potential conflict of interest, Thomas Flemmig refrained from any sensitive elements of the clinical trial, including patient consent, direct data scoring, statistical analysis of data, and adverse event evaluation and reporting.
No other investigators had any conflicts of interest related to this study.
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional review board of the Heinrich-Heine-University, Germany (protocol number 3519).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Belinda Reinhardt and Astrid Klocke are co-first authors
Rights and permissions
About this article
Cite this article
Reinhardt, B., Klocke, A., Neering, S.H. et al. Microbiological dynamics of red complex bacteria following full-mouth air polishing in periodontally healthy subjects—a randomized clinical pilot study. Clin Oral Invest 23, 3905–3914 (2019). https://doi.org/10.1007/s00784-019-02821-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02821-3