Abstract
Objective
To evaluate the clinical performance of posterior resin composite restorations regarding experimental and regular adhesive protocols in caries affected-dentin (CAD).
Material and methods
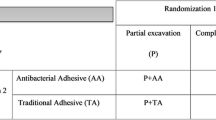
A total of 92 class I and class II cavities with carious lesions were selected and randomly assigned to the following groups: (1) bioactive glass-ceramic powder/two-step etch and rinse system, (2) control/two-step etch and rinse system, (3) bioactive glass-ceramic powder/two-step self-etching system, and (4) control/two-step self-etching system. Two operators carried out the adhesive protocols and restored the cavities with a nano-hybrid resin composite. Participants were followed up at 1 week and 6, 12, and 18 months for clinical evaluation performed by two blinded examiners and calibrated according to FDI criteria. Data were analyzed using Kruskal-Wallis and Dunn tests with a confidence of 95%.
Results
The clinical performance of resin composite restoration was not affected by the experimental use of an adhesive protocol including a bioactive glass-ceramic powder for 18 months post-procedure. However, there was a significant difference between group 2 and group 4 (p < 0.05) for marginal adaptation (18 months). Group 2 was significantly different from group 3 (p < 0.05) for fracture of material/retention (18 months) and marginal adaptation (1 week); group 2 showed a better performance.
Conclusion
Adhesive protocols can alter the clinical performance of posterior restorations in terms of marginal adaptation and the fracture of material/retention in CAD. Clinical significance: Adhesive protocols may influence the success of resin composite restorations in CAD; this is important because failure can lead to caries, re-incidence, and/or clinical re-work.

Similar content being viewed by others
References
Tyas MJ, Anusavice KJ, Frencken JE, Mount GJ (2000) Minimal intervention dentistry--a review. FDI Commission Project 1-97. Int Dent J 50:1–12. https://doi.org/10.1111/j.1875-595X.2000.tb00540.x
FDI policy statement on Minimal Intervention Dentistry (MID) for managing dental caries: Adopted by the general assembly: September 2016, Poznan, Poland (2017). Int Dent J 67:6–7. https://doi.org/10.1111/idj.12308
Nakajima M, Kunawarote S, Prasansuttiporn T, Tagami J (2011) Bonding to caries-affected dentin. Jpn Dent Sci Rev 47:102–114. https://doi.org/10.1016/j.jdsr.2011.03.002
Pinna R, Maioli M, Eramo S, Mura I, Milia E (2015) Carious affected dentine: its behaviour in adhesive bonding. Aust Dent J 60:276–293. https://doi.org/10.1111/adj.12309
Ekambaram M, Yiu CKY, Matinlinna JP (2015) Bonding of resin adhesives to caries-affected dentin – a systematic review. Int J Adhes Adhes 61:23–34. https://doi.org/10.1016/j.ijadhadh.2015.04.011
Perdigão J, Reis A, Loguercio AD (2013) Dentin adhesion and MMPs: a comprehensive review. J Esthet Restor Dent 25:219–241. https://doi.org/10.1111/jerd.12016
Erhardt MC, Toledano M, Osorio R, Pimenta LA (2008) Histomorphologic characterization and bond strength evaluation of caries-affected dentin/resin interfaces: effects of long-term water exposure. Dent Mater 24:786–798. https://doi.org/10.1016/j.dental.2007.09.007
Armstrong SR, Vargas MA, Chung I, Pashley DH, Campbell JA, Laffoon JE, Qian F (2004) Resin-dentin interfacial ultrastructure and microtensile dentin bond strength after five-year water storage. Oper Dent 29:705–712. https://doi.org/10.3290/j.jad.a17543
Hashimoto M, Fujita S, Nagano F, Ohno H, Endo K (2010) Ten-years degradation of resin-dentin bonds. Eur J Oral Sci 118:404–410. https://doi.org/10.1111/j.1600-0722.2010.00744.x
Anchieta RB, Machado LS, Martini AP, Santos PH, Giannini M, Janal M et al (2015) Effect of long-term storage on nanomechanical and morphological properties of dentin-adhesive interfaces. Dent Mater 31:141–153. https://doi.org/10.1016/j.dental.2014.11.010
Hashimoto M, Ohno H, Kaga M, Endo K, Sano H, Oguchi H (2000) In vivo degradation of resin-dentin bonds in humans over 1 to 3 years. J Dent Res 79:1385–1391. https://doi.org/10.1177/00220345000790060601
Tam L, Jokstad A (2010) The bond between resin composite restorations and dentin may degrade in the mouth over time. J Evid Based Dent Pract 10:21–22. https://doi.org/10.1016/j.jebdp.2009.11.011
Opdam NJ, van de Sande FH, Bronkhorst E, Cenci MS, Bottenberg P, Pallesen U et al (2014) Longevity of posterior composite restorations: a systematic review and meta-analysis. J Dent Res 93:943–949. https://doi.org/10.1177/0022034514544217
Ástvaldsdóttir Á, Dagerhamn J, van Dijken JW, Naimi-Akbar A, Sandborgh-Englund G, Tranæus S et al (2015) Longevity of posterior resin composite restorations in adults – a systematic review. J Dent 43:934–954. https://doi.org/10.1016/j.jdent.2015.05.001
Reis A, Carrilho M, Breschi L, Loguercio AD (2013) Overview of clinical alternatives to minimize the degradation of the resin-dentin bonds. Oper Dent 38:E1–E25. https://doi.org/10.2341/12-258-LIT
Stanislawczuk R, Pereira F, Munoz MA, Luque I, Farago PV, Reis A et al (2014) Effects of chlorhexidine-containing adhesives on the durability of resin-dentine interfaces. J Dent 42:39–47. https://doi.org/10.1016/j.jdent.2013.11.002
Loguercio AD, Hass V, Gutierrez MF, Luque-Martinez IV, Szezs A, Stanislawczuk R, Bandeca MC, Reis A (2016) Five-year effects of chlorhexidine on the in vitro durability of resin/dentin interfaces. J Adhes Dent 18:35–42. https://doi.org/10.3290/j.jad.a35514
Zheng P, Zaruba M, Attin T, Wiegand A (2015) Effect of different matrix metalloproteinase inhibitors on microtensile bond strength of an etch-and-rinse and a self-etching adhesive to dentin. Oper Dent 40:80–86. https://doi.org/10.2341/13-162-L
Macedo GV, Yamauchi M, Bedran-Russo AK (2009) Effects of chemical cross-linkers on caries-affected dentin bonding. J Dent Res 88:1096–1100. https://doi.org/10.1177/0022034509351001
Chiang YS, Chen YL, Chuang SF, Wu CM, Wei PJ, Han CF, Lin JC, Chang HT (2013) Riboflavin-ultraviolet-A-induced collagen cross-linking treatments in improving dentin bonding. Dent Mater 29:682–692. https://doi.org/10.1016/j.dental.2013.03.015
Hernández M, Cobb D, Swift EJ (2014) Current strategies in dentin remineralization. J Esthet Restor Dent 26:139–145. https://doi.org/10.1111/jerd.12095
Zhong B, Peng C, Wang G, Tian L, Cai Q, Cui F (2015) Contemporary research findings on dentine remineralization. J Tissue Eng Regen Med 9:1004–1016. https://doi.org/10.1002/term.1814
Sauro S, Pashley DH (2016) Strategies to stabilise dentine-bonded interfaces through remineralising operative approaches – state of the art. Int J Adhes Adhes 69:39–57. https://doi.org/10.1016/j.ijadhadh.2016.03.014
Sauro S, Osorio R, Watson TF, Toledano M (2012) Therapeutic effects of novel resin bonding systems containing bioactive glasses on mineral-depleted areas within the bonded-dentine interface. J Mater Sci Mater Med 23:1521–1532. https://doi.org/10.1007/s10856-012-4606-6
Profeta AC, Mannocci F, Foxton RM, Thompson I, Watson TF, Sauro S (2012) Bioactive effects of a calcium/sodium phosphosilicate on the resin-dentine interface: a microtensile bond strength, scanning electron microscopy, and confocal microscopy study. Eur J Oral Sci 120:353–362. https://doi.org/10.1111/j.1600-0722.2012.00974.x
Sauro S, Watson TF, Thompson I, Banerjee A (2012) One-bottle self-etching adhesives applied to dentine air-abraded using bioactive glasses containing polyacrylic acid: an in vitro microtensile bond strength and confocal microscopy study. J Dent 40:896–905. https://doi.org/10.1016/j.jdent.2012.07.004
Crovace MC, Souza MT, Chinaglia CR, Peitl O, Zanotto ED (2016) Biosilicate® — a multipurpose, highly bioactive glass-ceramic. In vitro, in vivo and clinical trials. J Non-Crys Solids 432 Part A 432:90–110. https://doi.org/10.1016/j.jnoncrysol.2015.03.022
Renno AC, Bossini PS, Crovace MC, Rodrigues AC, Zanotto ED, Parizotto NA (2013) Characterization and in vivo biological performance of biosilicate. Biomed Res Int 2013:141427–141427. https://doi.org/10.1155/2013/141427
Martins CH, Carvalho TC, Souza MG, Ravagnani C, Peitl O, Zanotto ED et al (2011) Assessment of antimicrobial effect of Biosilicate® against anaerobic, microaerophilic and facultative anaerobic microorganisms. J Mater Sci Mater Med 22:1439–1446. https://doi.org/10.1007/s10856-011-4330-7
Tirapelli C, Panzeri H, Soares RG, Peitl O, Zanotto ED (2010) A novel bioactive glass-ceramic for treating dentin hypersensitivity. Braz Oral Res 24:381–387. https://doi.org/10.1590/S1806-83242010000400002
Tirapelli C, Panzeri H, Lara EH, Soares RG, Peitl O, Zanotto ED (2011) The effect of a novel crystallised bioactive glass-ceramic powder on dentine hypersensitivity: a long-term clinical study. J Oral Rehabil 38:253–262. https://doi.org/10.1111/j.1365-2842.2010.02157.x
Pinheiro H, Lopes B, Klautau E, Cardoso J, Silva B, Cardoso P (2010) Influence of bioactive materials used on the dentin surface whitened with carbamide peroxide 16%. Mat Res 13:273–278. https://doi.org/10.1590/S1516-14392010000200024
Pintado-Palomino K, Tirapelli C (2015) The effect of home-use and in-office bleaching treatments combined with experimental desensitizing agents on enamel and dentin. Eur J Dent 9:66–73. https://doi.org/10.4103/1305-7456.149645
Rastelli A, Nicolodelli G, Romano R, Milori D, Perazzoli I, Ferreira E et al (2016) After bleaching enamel remineralization using a bioactive glass-ceramic (BioSilicate®). Biomed glasses 2:1–9. https://doi.org/10.1515/bglass-2016-0001
de Morais RC, Silveira RE, Chinelatti MA, Pires-de-Souza FCP (2016) Biosilicate as a dentin pretreatment for total-etch and self-etch adhesives: in vitro study. Int J Adhes Adhes 70:271–276. https://doi.org/10.1016/j.ijadhadh.2016.07.007
Hickel R, Roulet JF, Bayne S, Heintze SD, Mjör IA, Peters M et al (2007) Recommendations for conducting controlled clinical studies of dental restorative materials. Science committee project 2/98--FDI world dental federation study design (part I) and criteria for evaluation (part II) of direct and indirect restorations including onlays and partial crowns. J Adhes Dent 9 Suppl 1:121–147. https://doi.org/10.3290/j.jad.a19262
Innes NP, Frencken JE, Bjørndal L, Maltz M, Manton DJ, Ricketts D et al (2016) Managing carious lesions: consensus recommendations on terminology. Adv Dent Res 28:49–57. https://doi.org/10.1177/0022034516639276
Massara ML, Alves JB, Brandão PR (2002) Atraumatic restorative treatment: clinical, ultrastructural and chemical analysis. Caries Res 36:430–436. https://doi.org/10.1159/000066534
Hickel R, Peschke A, Tyas M, Mjör I, Bayne S, Peters M, Hiller KA, Randall R, Vanherle G, Heintze SD (2010) FDI World Dental Federation: clinical criteria for the evaluation of direct and indirect restorations-update and clinical examples. Clin Oral Investig 14:349–366. https://doi.org/10.1007/s00784-010-0432-8
Profeta AC, Mannocci F, Foxton R, Watson TF, Feitosa VP, De Carlo B et al (2013) Experimental etch-and-rinse adhesives doped with bioactive calcium silicate-based micro-fillers to generate therapeutic resin-dentin interfaces. Dent Mater 29:729–741. https://doi.org/10.1016/j.dental.2013.04.001
Sauro S, Watson TF, Thompson I, Toledano M, Nucci C, Banerjee A (2012) Influence of air-abrasion executed with polyacrylic acid-Bioglass 45S5 on the bonding performance of a resin-modified glass ionomer cement. Eur J Oral Sci 120:168–177. https://doi.org/10.1111/j.1600-0722.2012.00939.x
Pires-de-Souza FC, de Marco FF, Casemiro LA, Panzeri H (2007) Desensitizing bioactive agents improves bond strength of indirect resin-cemented restorations: preliminary results. J Appl Oral Sci 15:120–126. https://doi.org/10.1590/S1678-77572007000200009
Osorio E, Fagundes T, Navarro MF, Zanotto ED, Peitl O, Osorio R, Toledano-Osorio M, Toledano M (2015) A novel bioactive agent improves adhesion of resin-modified glass-ionomer to dentin. J Adhes Sci Technol 29:1543–1552. https://doi.org/10.1080/01694243.2015.1030897
Boeckler A, Boeckler L, Eppendorf K, Schaller HG, Gernhardt CR (2012) A prospective, randomized clinical trial of a two-step self-etching vs two-step etch-and-rinse adhesive and SEM margin analysis: four-year results. J Adhes Dent 14:585–592. https://doi.org/10.3290/j.jad.a27796
Sundfeld RH, Scatolin RS, Oliveira FG, Machado LS, Alexandre RS, Sundefeld ML (2012) One-year clinical evaluation of composite restorations in posterior teeth: effect of adhesive systems. Oper Dent 37:E1–E8. https://doi.org/10.2341/10-375-C
Sundfeld RH, Machado LS, Pita DS, Franco LM, Sundfeld D, Sundefeld ML et al (2016) Three-year clinical evaluation of class I restorations in posterior teeth. Effects of two adhesive systems. Compend Contin Educ Dent 37:e1–e4
Boeckler A, Schaller HG, Gernhardt CR (2012) A prospective, double-blind, randomized clinical trial of a one-step, self-etch adhesive with and without an intermediary layer of a flowable composite: a 2-year evaluation. Quintessence Int 43:279–286
Wattanawongpitak N, Yoshikawa T, Burrow MF, Tagami J (2006) The effect of bonding system and composite type on adaptation of different C-factor restorations. Dent Mater J 25:45–50. https://doi.org/10.4012/dmj.25.45
Wattanawongpitak N, Yoshikawa T, Burrow MF, Tagami J (2007) The effect of thermal stress on bonding durability of resin composite adaptation to the cavity wall. Dent Mater J 26:445–450. https://doi.org/10.4012/dmj.25.45
Sideridou ID, Karabela MM, Vouvoudi E (2011) Physical properties of current dental nanohybrid and nanofill light-cured resin composites. Dent Mater 27:598–607. https://doi.org/10.1016/j.dental.2011.02.015
Krithikadatta J (2010) Clinical effectiveness of contemporary dentin bonding agents. J Conserv Dent 13:173–183. https://doi.org/10.4103/0972-0707.73376
Manchorova-Veleva NA, Vladimirov SB, Keskinova Dcapital AC (2015) Clinical effect of dental adhesive on marginal integrity in class I and class II resin-composite restorations. Folia Med (Plovdiv) 57:250–256. https://doi.org/10.1515/folmed-2015-0046
Boushell LW, Heymann HO, Ritter AV, Sturdevant JR, Swift EJ Jr, Wilder AD Jr et al (2016) Six-year clinical performance of etch-and-rinse and self-etch adhesives. Dent Mater 32:1065–1072. https://doi.org/10.1016/j.dental.2016.06.003
Mena-Serrano A, Kose C, De Paula EA, Tay LY, Reis A, Loguercio AD et al (2013) A new universal simplified adhesive: 6-month clinical evaluation. J Esthet Restor Dent 25:55–69. https://doi.org/10.1111/jerd.12005
Perdigao J, Kose C, Mena-Serrano AP, De Paula EA, Tay LY, Reis A et al (2014) A new universal simplified adhesive: 18-month clinical evaluation. Oper Dent 39:113–127. https://doi.org/10.2341/13-045-C
Funding
This study was funded by the São Paulo Research Foundation - FAPESP (grant number 2010/12032-6) and Center for Research, Teaching and Innovation in Glass (CeRTEV)/CEPID grant number 2013/07793-6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were conducted in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Pintado-Palomino, K., de Almeida, C.V.V.B., da Motta, R.J.G. et al. Clinical, double blind, randomized controlled trial of experimental adhesive protocols in caries-affected dentin. Clin Oral Invest 23, 1855–1864 (2019). https://doi.org/10.1007/s00784-018-2615-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2615-7