Abstract
Objectives
To synthesize a silver-doped bioactive glass/mesoporous silica nanoparticle (Ag-BGN@MSN), as well as to investigate its effects on dentinal tubule occlusion, microtensile bond strength (MTBS), and antibacterial activity.
Materials and methods
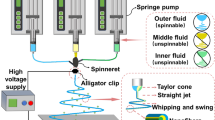
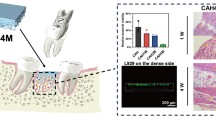
Ag-BGN@MSN was synthesized using a modified “quick alkali-mediated sol-gel” method. Demineralized tooth disc models were made and divided into four groups; the following treatments were then applied: group 1—no treatment, group 2—bioglass, group 3—MSN, group 4—Ag-BGN@MSN. Next, four discs were selected from each group and soaked into 6 wt% citric acid to test acid-resistant stability. Dentinal tubule occlusion, as well as the occlusion ratio, was observed using field-emission scanning electron microscopy. The MTBS was also measured to evaluate the desensitizing effect of the treatments. Cytotoxicity was examined using the MTT assay. Antibacterial activity was detected against Lactobacillus casei, and ion dissolution was evaluated using inductively coupled plasma optical emission spectrometry.
Results
Ag-BGN@MSN effectively occluded the dentinal tubule and formed a membrane-like layer. After the acid challenge, Ag-BGN@MSN had the highest rate of dentinal tubule occlusion. There were no significant differences in MTBS among the four groups (P > 0.05). All concentrations of Ag-BGN@MSN used had a relative cell viability above 72%.
Conclusions
Ag-BGN@MSN was successfully fabricated using a modified sol-gel method. The Ag-BGN@MSN biocomposite effectively occluded dentinal with acid-resistant stability, did not decrease bond strength in self-etch adhesive system, had low cytotoxicity, and antibacterial effect.
Clininal relevance
Dentinal tubule sealing induced by Ag-BGN@MSN biocomposite with antibacterial effect is likely to increase long-term stability in DH.












Similar content being viewed by others
Reference
Sanjay M, Vivek A, Bhoomika A (2010) Dentin hypersensitivity: recent trends in management. J Conserv Dent 13:218–224. https://doi.org/10.4103/0972-0707.73385
Holland GR, Narhi MN, Addy M, Gangarosa L, Orchardson R (1997) Guidelines for the design and conduct of clinical trials on dentine hypersensitivity. J Clin Periodontol 24:808–813. https://doi.org/10.1111/j.1600-051X.1997.tb01194.x
Brannstrom M (1963) Dentin sensitivity and aspiration of odontoblasts. J Am Dent Assoc 66:366–370. https://doi.org/10.14219/jada.archive.1963.0104
Rees JS, Jin U, Lam S, Kudanowska I, Vowles R (2003) The prevalence of dentine hypersensitivity in a hospital clinic population in Hong Kong. J Dent 31:453–461. https://doi.org/10.1016/S0300-5712(03)00092-7
Flynn J, Galloway R, Orchardson R (1985) The incidence of ‘hypersensitive’ teeth in the West of Scotland. J Dent 13:230–236. https://doi.org/10.1016/0300-5712(85)90004-1
Fischer C, Fischer RG, Wennberg A (1992) Prevalence and distribution of cervical dentine hypersensitivity in a population in Rio de Janeiro, Brazil. J Dent 20:272–276. https://doi.org/10.1016/0300-5712(92)90043-C
Wang Y, Que K, Lin L, Hu D, Li X (2012) Prevalence of dentine hypersensitivity in the general population in China. J Oral Rehabil 39:812–820. https://doi.org/10.1111/j.1365-2842.2012.02334.x
Liu HC, Lan WH, Hsieh CC (1998) Prevalence and distribution of cervical dentin hypersensitivity in a population in Taipei, Taiwan. J Endod 24:45–47. https://doi.org/10.1016/S0099-2399(98)80213-6
Absi EG, Addy M, Adams D (1987) Dentine hypersensitivity: a study of the patency of dentinal tubules in sensitive and non-sensitive cervical dentine. J Clin Periodontol 14:280–284. https://doi.org/10.1111/j.1600-051X.1987.tb01533.x
Schmidlin PR, Sahrmann P (2013) Current management of dentin hypersensitivity. Clin Oral Investig 17:55–59. https://doi.org/10.1007/s00784-012-0912-0
Pashley DH (1994) Dentin permeability and its role in the pathobiology of dentin sensitivity. Arch Oral Biol 39:73–80. https://doi.org/10.1016/0003-9969(94)90191-0
Wang Z, Sa Y, Sauro S, Chen H, Xing W, Ma X (2010) Effect of desensitising toothpastes on dentinal tubule occlusion: a dentine permeability measurement and SEM in vitro study. J Dent 38:400–410. https://doi.org/10.1016/j.jdent.2010.01.007
Canali GD, Rached RN, Mazur RF, Souza EM (2017) Effect of erosion/abrasion challenge on the dentin tubule occlusion using different desensitizing agents. Braz Dent J 28:216–224. https://doi.org/10.1590/0103-6440201700811
Reis C, De-Deus G, Leal F, Azevedo E, Coutinho-Filho T, Paciornik S (2008) Strong effect on dentin after the use of high concentrations of citric acid: an assessment with co-site optical microscopy and ESEM. Dent Mater 24:1608–1615. https://doi.org/10.1016/j.dental.2008.03.027
Wiegand A, Stock A, Attin R, Werner C, Attin T (2007) Impact of the acid flow rate on dentin erosion. J Dent 35:21–27. https://doi.org/10.1016/j.jdent.2006.04.002
Pei D, Liu S, Huang C, Du X, Yang H, Wang WY (2013) Effect of pretreatment with calcium-containing desensitizer on the dentine bonding of mild self-etch adhesives. Eur J Oral Sci 121:204–210. https://doi.org/10.1111/eos.12047
Tang F, Li L, Chen D (2012) Mesoporous silica nanoparticles: synthesis, biocompatibility and drug delivery. Adv Mater 24:1504–1534. https://doi.org/10.1002/adma.201104763
Huang X, Young NP, Townley HE (2014) Characterisation and comparison of mesoporous silica particles for optimised drug delivery. Nanomater Nanotechnol 4:2–15. https://doi.org/10.5772/58290
Tian L, Peng C, Shi Y, Guo X, Zhong B, Qi J et al (2014) Effect of mesoporous silica nanoparticles on dentinal tubule occlusion: an in vitro study using SEM and image analysis. Dent Mater J 33:125–132. https://doi.org/10.4012/dmj.2013-215
Prabhakar AR, Paul MJ, Basappa N (2010) Comparative evaluation of the remineralizing effects and surface micro hardness of glass ionomer cements containing bioactive glass (S53P4): an in vitro study. Int J Clin Pediatr Dent 3:69–77. https://doi.org/10.5005/jp-journals-10005-1057
Erol-Taygun M, Zheng K, Boccaccini AR (2013) Nanoscale bioactive glasses in medical applications. Int J Appl Glas Sci 4:136–148. https://doi.org/10.1111/ijag.12029
Webster TJ, Ergun C, Doremus RH, Siegel RW, Bizios R (2000) Enhanced functions of osteoblasts on nanophase ceramics. Biomaterials 21:1803–1810. https://doi.org/10.1016/S0142-9612(00)00075-2
Miguez-Pacheco V, Hench LL, Boccaccini AR (2015) Bioactive glasses beyond bone and teeth: emerging applications in contact with soft tissues. Acta Biomater 13:1–15. https://doi.org/10.1016/j.actbio.2014.11.004
Hoppe A, Güldal NS, Boccaccini AR (2011) A review of the biological response to ionic dissolution products from bioactive glasses and glass-ceramics. Biomaterials 32:2757–2774. https://doi.org/10.1016/j.biomaterials.2011.01.004
Ruparelia JP, Chatterjee AK, Duttagupta SP, Mukherji S (2008) Strain specificity in antimicrobial activity of silver and copper nanoparticles. Acta Biomater 4:707–716. https://doi.org/10.1016/j.actbio.2007.11.006
El-Kady AM, Ali AF, Rizk RA, Ahmed MM (2012) Synthesis, characterization and microbiological response of silver-doped bioactive glass nanoparticles. Ceram Int 38:177–188. https://doi.org/10.1016/j.ceramint.2011.05.158
Shi X, Wang Y, Wei K, Ren L, Lai C (2008) Self-assembly of nanohydroxyapatite in mesoporous silica. J Mater Sci Mater Med 19:2933–2940. https://doi.org/10.1007/s10856-008-3424-3
Xia W, Chang J (2007) Preparation and characterization of nano-bioactive-glasses (NBG) by a quick alkali-mediated sol–gel method. Mater Lett 61:3251–3253. https://doi.org/10.1016/j.matlet.2006.11.048
Wang Y, Zhao Q, Han N, Bai L, Li J, Liu J, Che E, Hu L, Zhang Q, Jiang T, Wang S (2015) Mesoporous silica nanoparticles in drug delivery and biomedical applications. Nanomedicine 11:313–327. https://doi.org/10.1016/j.nano.2014.09.014
Horcajada P, Rámila A, Boulahya K, González-Calbet J, Vallet-Regí M (2004) Bioactivity in ordered mesoporous materials. Solid State Sci 6:1295–1300. https://doi.org/10.1016/j.solidstatesciences.2004.07.026
Lee BS, Chang CW, Chen WP, Lan WH, Lin CP (2005) In vitro study of dentin hypersensitivity treated by Nd:YAP laser and bioglass. Dent Mater 21:511–519. https://doi.org/10.1016/j.dental.2004.08.002
Chiang YC, Chen HJ, Liu HC, Kang SH, Lee BS, Lin FH (2010) A novel mesoporous biomaterial for treating dentin hypersensitivity. J Dent Res 89:236–240. https://doi.org/10.1177/0022034509357148
Yu J, Yang H, Li K, Lei J, Zhou L, Huang C (2016) A novel application of nanohydroxyapatite/mesoporous silica biocomposite on treating dentin hypersensitivity: an in vitro study. J Dent 50:21–29. https://doi.org/10.1016/j.jdent.2016.04.005
Xu Z, Neoh KG, Kishen A (2008) Monitoring acid-demineralization of human dentine by electrochemical impedance spectroscopy (EIS). J Dent 36(12):1005–1012. https://doi.org/10.1016/j.jdent.2008.08.007
Izquierdo-Barba I, Ruiz-González L, Doadrio JC, González-Calbet JM, Vallet-Regí M (2005) Tissue regeneration: a new property of mesoporous materials. Solid State Sci 7:983–989. https://doi.org/10.1016/j.solidstatesciences.2005.04.003
Vollenweider M, Brunner TJ, Knecht S, Grass RN, Zehnder M, Imfeld T, Stark WJ (2007) Remineralization of human dentin using ultrafine bioactive glass particles. Acta Biomater 3:936–943. https://doi.org/10.1016/j.actbio.2007.04.003
Vallet-Regí M, Izquierdo-Barba I, Rámila A, Pérez-Pariente J, Babonneau F, González-Calbet JM (2005) Phosphorous-doped MCM-41 as bioactive material. Solid State Sci 7:233–237. https://doi.org/10.1016/j.solidstatesciences.2004.10.038
Adebayo OA, Burrow MF, Tyas MJ (2008) Dentine bonding after CPP-ACP paste treatment with and without conditioning. J Dent 36:1013–1024. https://doi.org/10.1016/j.jdent.2008.08.011
Bergamin AC, Bridi EC, Amaral FL, Turssi CP, Basting RT, Aguiar FH, França FM (2016) Influence of an arginine-containing toothpaste on bond strength of different adhesive systems to eroded dentin. Gen Dent 64:67–73
Marshall SJ, Bayne SC, Baier R, Tomsia AP, Marshall GW (2010) A review of adhesion science. Dent Mater 26:11–16. https://doi.org/10.1016/j.dental.2009.11.157
Yang H, Pei D, Liu S, Wang Y, Zhou L, Deng D (2013) Effect of a functional desensitizing paste containing 8% arginine and calcium carbonate on the microtensile bond strength of etch-and-rinse adhesives to human dentin. Am J Dent 26:137–142. https://doi.org/10.1186/s40563-014-0024-y
Karpiński TM, Szkaradkiewicz AK (2013) Microbiology of dental caries. J Biol Earth Sci 3:21–24. https://doi.org/10.1007/978-1-349-16547-6_3
Jung WK, Koo HC, Kim KW, Shin S, Kim SH, Park YH (2008) Antibacterial activity and mechanism of action of the silver ion in Staphylococcus aureus and Escherichia coli. Appl Environ Microbiol 74:2171–2178. https://doi.org/10.1128/AEM.02001-07
Brown ML, Davis HB, Tufekci E, Crowe JJ, Covelle DA, Mitchell JC (2011) Ion release from a novel orthodontic resin bonding agent for the reduction and/or prevention of white spot lesions: an in vitro study. Angle Orthod 81:1014–1020. https://doi.org/10.2319/120710-708.1
Funding
This study was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIP) (NRF-2015R1C1A1A01051832).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
YI Kim has received research grants from the National Research Foundation of Korea (NRF) for this study. All authors declare that they have no competing interest.
Ethical approval
The study was approved by the Ethics Committee of Pusan National University Dental Hospital (PNUDH-2016-033).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Jung, JH., Kim, DH., Yoo, KH. et al. Dentin sealing and antibacterial effects of silver-doped bioactive glass/mesoporous silica nanocomposite: an in vitro study. Clin Oral Invest 23, 253–266 (2019). https://doi.org/10.1007/s00784-018-2432-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2432-z