Abstract
Objectives
Research has been ongoing on achieving optimum bone healing in the reconstruction of bone loss. Clinically, soft tissue migration into the already existing bone defects is the leading cause of unfavourable bone healing. Platelet-rich fibrin, a recent material that is used to promote bone healing, was compared with single- and double-layered resorbable collagen membranes to determine whether a healing protocol which increases patient comfort is possible.
Materials and methods
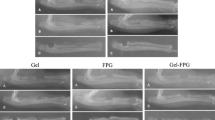
Sixty adult female Sprague-Dawley rats were used. The rats were divided into five main groups as a sacrification group, a control group, and three experimental groups. The bone defects experimental group 1 were covered with a single-layer collagen membrane, and experimental group 2 were covered with the double-layered collagen membrane. Defects on the experimental group 3 were covered with platelet-rich fibrin membranes which were derived from the sacrification group. The animals in the main groups were also divided into eight subgroups arranged by sacrification periods on day 7 and day 28.
Results
Statistical analysis of our study revealed that new bone formation in experimental group 3 was significantly higher than in other groups. Fibrosis was found to be lower in experimental group 3 than in any other group. No significant differences were found between experimental group 1 and the control group.
Conclusion
Platelet-rich fibrin, which can be used as an autologous membrane which promotes bone healing, yields better clinical result compared to collagen membranes.
Clinical relevance
Histopathologic evaluation has been carried out regarding the effect of platelet-rich fibrin and collagen membranes applied on bone recovery. Our objective is to contribute to barrier membrane studies that continue to guide and accelerate bone recovery.

Similar content being viewed by others
References
Tatullo M, Marrelli M, Cassetta M, Pacifici A, Stefanelli LV, Scacco S, Dipalma G, Pacifici L, Inchingolo F (2012) Platelet rich fibrin (PRF) in reconstructive surgery of atrophied maxillary bones: clinical and histological evaluations. Int J Med Sci 9(10):872–880
Dahlin C, Alberius P, Linde A (1991) Osteopromotion for cranioplasty: an experimental study in rats using a membrane technique. J Neurosurg 74:487–491
Cafesse RG, Qumones CR (1991) Guided tissue regeneration: biologic rationale, surgical technique, and clinical results. Compend Contin Educ Dent 3:166–178
Dohan DM, Choukroun J, Diss A, Dohan SL, Dohan AJ, Mouhyı J, Gogly B (2006) Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part II: platelet-related biologic features. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 101:E45–E50
Choukroun J, Diss A, Simonpieri A, Girard MO, Schoeffler C, Dohan SL, Dohan AJ, Mouhyi J, Dohan DM (2006) Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part IV: clinical effects on tissue healing. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 101:E56–E60
Ghanaati S, Booms P, Orlowska A, Kubesch A, Lorenz J, Rutkowski J, Landes C, Sader R, Kirkpatrick CJ, Choukroun J (2014) Advanced platelet-rich fibrin: a new concept for cell-based tissue engineering by means of inflammatory cells. J Oral Implantol 40:679–689
Kobayashi E, Flückiger L, Fujioka-Kobayashi M et al (2016) Comparative release of growth factors from PRP, PRF, and advanced-PRF. Clin Oral Investig 20:2353
Buser D, Dula K, Belser U, Hirt HP, Berthold H (1992) Localized ridge augmentation using guided bone regeneration. 1. Surgical procedure in the maxilla. Int J Periodontics Restorative Dent 13:29–45
Schmitz JP, Schwartz Z, Hollinger JO, Boyan BD (1990) Characterization of rat calvarial nonunion defects. Acta Anat (Basel) 138:185–192
Ogiso B, Hughes FJ, Melcher AH, McCulloch CA (1991) Fibroblasts inhibit mineralized bone nodule formation by rat bone marrow stromal cells in vitro. J Cell Physiol 146:442–450
Hardwick R, Dahlin C (1994) Healing pattern of bone regeneration in membrane-protected defects: a histologic study in the canine mandible. Int J Oral Maxillofac Implants 9:13–29
Schenk RK, Buser D, Hardwick WR, Dahlin C (1994) Healing pattern of bone regeneration in membrane-protected defects: a histologic study in the canine mandible. Int J Oral Maxillofac Implants 9(1):13–29
Simion M, Scarano A, Gionso L, Piattelli A (1996) Guided bone regeneration using resorbable and nonresorbable membranes: a comparative histologic study in humans. Int J Oral Maxillofac Implants 11(6):735–742
Chung CP, Kim DK, Park YJ, Nam KH, Lee SJ (1997) Biological effects of drug loaded biodegradable membranes for guided bone regeneration. J Periodontal Res 32:172–175
Tuskan C, Yaltırık M (2002) Oral ve Maksillofasiyal Cerrahide Kullanılan Biyomateryaller. İ.Ü. Basım ve Yayınevi Müdürlüğü, İstanbul, pp 19–26
Dohan DM, Choukroun J, Diss A, Dohan SL, Dohan AJ, Mouhyı J, Gogly B (2006) Platelet-rich fibrin (PRF); a second generation platelet concentrate. Part I: technological concepts and evolution. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 101:E37–E44
Yang YG, Sykes M (2007) Xenotransplantation: current status and a perspective on the future. Nat Rev Immunol 7(7):519–531
DelRossi AJ, Cernaianu AC, Vertrees RA, Wacker CJ, Fuller SJ, Cilley JH Jr, Baldino WA (1990) Platelet-rich plasma reduces postoperative blood loss after cardiopulmonary bypass. J Thorac Cardiovasc Surg 100(2):281–286
Fijnheer R, Pietersz RN, Korte DD, Gouwerok CW, Dekker WJ, Reesink HW, Roos D (1990) Platelet activation during the preparation of platelet concentrates; a comparison of the platelet-rich plasma and the buffy coat methods. Transfusion 30(7):634–638
Schlegel KA, Donath K, Rupprecht S, Falk S, Zimmermann R, Felszeghy E, Wiltfang J (2004) De novo bone formation using bovine collagen and platelet-rich plasma. Biomaterials 25(23):5387–5393
Thorwarth M, Schultze-Mosgau S, Kessler P, Wiltfang J, Schlegel KA (2005) Bone regeneration in osseous defects using a resorbable nanoparticular hydroxyapatite. J Oral Maxillofac Surg 63(11):1626–1633
Tsay RC, Vo J, Burke A, Eisig SB, Lu HH, Landesberg R (2005) Differential growth factor retention by platelet-rich plasma composites. J Oral Maxillofac Surg 63(4):521–528
Lacoste E, Martineau I, Gagnon G (2003) Platelet concentrates; effects of calcium and thrombin on endothelial cell proliferation and growth factor release. J Periodontol 74(10):1498–1507
Misch CE (2007) Contemporary implant dentistry. Elsevier Health Sciences
Lucarelli E, Beretta R, Dozza B, Tazzari PL, O’ Connell SM, Ricci F, Pierini M, Squarzoni S, Pagliaro PP, Oprita EI, Donati D (2010) A recently developed bifacial platelet-rich fibrin matrix. Eur Cell Mater 20:13–23
Raja SV, Naidu ME (2008) Platelet-rich fibrin: evolution of a second-generation platelet concentrate. Indian J Dent Res 19:42–46
Gentile P, Bottini DJ, Spallone D, Curcio BC, Cervelli V (2010) Application of platelet-rich plasma in maxillofacial surgery: clinical evaluation. J Craniofac Surg 21(3):900–904
Gassling VL, Açil Y, Springer IN, Hubert N, Wiltfang J (2009) Platelet-rich plasma and platelet-rich fibrin in human cell culture. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol 108(1):48–55
Vence BS, Mandelaris GA, Forbes DP (2009) Management of dentoalveolar ridge defects for implant site development: an interdisciplinary approach. Dent 30(5):250–262
Thorat M, Pradeep AR, Pallavi B (2011) Clinical effect of autologous platelet-rich fibrin in the treatment of intra-bony defects: a controlled clinical trial. J Clin Periodontol 38(10):925–932
Mooren RE, Dankers AC, Merkx MA, Bronkhorst EM, Jansen JA, Stoelinga PJ (2010) The effect of platelet-rich plasma on early and late bone healing using a mixture of particulate autogenous cancellous bone and Bio-Oss: an experimental study in goats. Int J Oral Maxillofac Surg 39(4):371–378
Funding
The present work was supported by the Research Fund of Istanbul University, Istanbul, Turkey.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and institutional guidelines for the care and use of animals were followed.
Informed consent
For this type of study, formal consent is not required.
The present work has the approval of the Animal Rights Committee of Istanbul University.
Rights and permissions
About this article
Cite this article
Tayşi, M., Atalay, B., Çankaya, B. et al. Effects of single- and double-layered resorbable membranes and platelet-rich fibrin on bone healing. Clin Oral Invest 22, 1689–1695 (2018). https://doi.org/10.1007/s00784-017-2259-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-017-2259-z