Abstract
Objectives
The aim of this study is to improve the understanding of interleukin mechanisms during osseointegration to enhance the monitoring of implant failure and success. Clinical parameters, implant stability, and cytokine levels in peri-implant crevicular fluid (PICF) during early bone healing after implant placement were investigated.
Material and methods
Sixty narrow implants were placed in mandible anterior region of 30 edentulous patients (67.23 ± 7.66 years). Bone type, insertion torque, and primary stability were registered during surgery. Clinical measurements of peri-implant health and the secondary implant stability quotient (ISQ) were recorded. Samples from the PICF were collected 1, 2, 4, 8, and 12 weeks after surgery and analyzed for IL-1β, IL-6, IL-10, and TNF-α levels using ELISAs.
Results
The gingival index increased significantly during the first week (p = 0.05), while the plaque index increased significantly between 4 to 8 and 8 to 12 weeks (p < 0.05). The probing depth and the ISQ also reduced significantly (p < 0.05) over time. The TNF-α release increased significantly after the 2nd week for non-atrophic patients and 4th week for atrophic patients (p < 0.05). The IL-1β concentrations showed a short-lived peak after 1st week (p = 0.003), specially in atrophic patients and sites with bone type I (p = 0.034; p = 0.007). The IL-6 concentrations peaked during the 1st and 2nd weeks (p < 0.05; p = 0.005) in atrophic patients and in bone type II (p = 0.023; p = 0.003). The IL-10 concentrations increased gradually over time, showing the highest concentrations at the 12th week (p < 0.005). A total of 12 implants failed at different periods.
Conclusion
While the clinical measurements presented differences between the evaluation periods, these were not indicative of early dental implant failure or peri-implant diseases. Smoking, bone atrophy, and bone type can greatly influence the cytokines concentrations during the healing time.




Similar content being viewed by others
Change history
04 September 2017
An erratum to this article has been published.
References
Papaspyridakos P, Chen CJ, Singh M, Weber HP, Gallucci GO (2012) Success criteria in implant dentistry: a systematic review. J Dent Res 91(3):242–248
Duarte PM, de Mendonca AC, Maximo MB, Santos VR, Bastos MF, Nociti FH (2009) Effect of anti-infective mechanical therapy on clinical parameters and cytokine levels in human peri-implant diseases. J Periodontol 80(2):234–243
Trindade R, Albrektsson T, Tengvall P, Wennerberg A (2016) Foreign body reaction to biomaterials: on mechanisms for buildup and breakdown of osseointegration. Clin Implant Dent Relat Res 18(1):192–203
Shanbhag S, Shanbhag V, Stavropoulos A (2015) Genomic analyses of early peri-implant bone healing in humans: a systematic review. Int J Implant Dent 1(1):5
Javed F, Al-Hezaimi K, Salameh Z, Almas K, Romanos GE (2011) Proinflammatory cytokines in the crevicular fluid of patients with peri-implantitis. Cytokine 53(1):8–12
Mosmman T, Sad S (1996) The expanding universe of T-cell subset: Th1, Th2 and more. Immunol Today 17(3):138–146
Hall J, Pehrson N-G, Ekestubbe A, Jemt T, Friberg B (2015) A controlled, cross-sectional exploratory study on markers for the plasminogen system and inflammation in crevicular fluid samples from healthy, mucositis and peri-implantitis sites. Eur J Oral Implantol 8(2):153–166
Mundy GR (1991) Inflammatory mediators and the destruction of bone. J Periodontal Res 26(3 Pt 2):213–217
Li JY, Wang HL (2014) Biomarkers associated with periimplant diseases. Implant Dent 23(5):607–611
Boynuegri AD, Yalim M, Nemli SK, Erguder BI, Gokalp P (2012) Effect of different localizations of microgap on clinical parameters and inflammatory cytokines in peri-implant crevicular fluid: a prospective comparative study. Clin Oral Investig 16(2):353–361
Ataoglu H, Alptekin NO, Haliloglu S, Gursel M, Ataoglu T, Serpek B, Durmus E (2002) Interleukin-Iβ, tumor necrosis factor-α levels and neutrophil elastase activity in peri-implant crevicular fluid: correlation with clinical parameters and effect of smoking. Clin Oral Implants Res 13(5):470–476
Duarte PM, Serrao CR, Miranda TS, Zanatta LC, Bastos MF, Faveri M, Figueiredo LC, Feres M (2016) Could cytokine levels in the peri-implant crevicular fluid be used to distinguish between healthy implants and implants with peri-implantitis? A systematic review. J Periodontal Res 51(6):689–698
Faot F, Nascimento GG, Bielemann AM, Campao TD, Leite FR, Quirynen M (2015) Can peri-implant crevicular fluid assist in the diagnosis of peri-implantitis? A systematic review and meta-analysis. J Periodontol 86(5):631–645
Wu Y, Zhang C, Squarize CH, Zou D (2015) Oral rehabilitation of adult edentulous siblings severely lacking alveolar bone due to ectodermal dysplasia: a report of 2 clinical cases and a literature review. J Oral Maxillofac Surg 73(9):1733):e1–12
Zhang Q, Chen B, Yan F, Guo J, Zhu X, Ma S and Yang W (2014) Interleukin-10 inhibits bone resorption: a potential therapeutic strategy in periodontitis and other bone loss diseases. Biomed Res Int 2014 (284836)
Stow JL, Murray RZ (2013) Intracellular trafficking and secretion of inflammatory cytokines. Cytokine Growth Factor Rev 24(3):227–239
Stow JL, Low PC, Offenhauser C, Sangermani D (2009) Cytokine secretion in macrophages and other cells: pathways and mediators. Immunobiology 214(7):601–612
Kishimoto T (2010) IL-6: from its discovery to clinical applications. Int Immunol 22(5):347–352
Shrum JP (1996) Cytokines. Clin Dermatol 14:331–336
Guncu GN, Akman AC, Gunday S, Yamalik N, Berker E (2012) Effect of inflammation on cytokine levels and bone remodelling markers in peri-implant sulcus fluid: a preliminary report. Cytokine 59(2):313–316
Javed F, Ahmed HB, Crespi R, Romanos GE (2013) Role of primary stability for successful osseointegration of dental implants: factors of influence and evaluation. Interv Med Appl Sci 5(4):162–167
Cavallaro J, Greenstein B, Greenstein G (2009) Clinical methodologies for achieving primary dental implant stability. J Am Dent Assoc 140(11):1366–1372
Oates TW, Valderrama P, Bischof M, Nedir R, Jones A, Simpson J, Toutenburg H, Cochran DL (2007) Enhanced implant stability with a chemically modified SLA surface a randomized pilot study. Int J Oral Maxillofac Implants 22(5):755–760
Xie Q, Wolf J, Ainamo A (1997) Quantitative assessment of vertical heights of maxillary and mandibular bones in panoramic radiographs of elderly dentate and edentulous subjects. Acta Odontol Scand 55(3):155–161
Cawood JL, Howell RA (1988) A classification of the edentulous jaws. Int J Oral Maxillofac Surg 17(4):232–236
Molly L (2006) Bone density and primary stability in implant therapy. Clin Oral Implants Res 17(Suppl 2):124–135
Mombelli A, van Oosten MA, Schurch E Jr, Land NP (1987) The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 2(4):145–151
Al-Nawas B, Bragger U, Meijer HJ, Naert I, Persson R, Perucchi A, Quirynen M, Raghoebar GM, Reichert TE, Romeo E, Santing HJ, Schimmel M, Storelli S, ten Bruggenkate C, Vandekerckhove B, Wagner W, Wismeijer D, Muller F (2012) A double-blind randomized controlled trial (RCT) of titanium-13Zirconium versus titanium grade IV small-diameter bone level implants in edentulous mandibles—results from a 1-year observation period. Clin Implant Dent Relat Res 14(6):896–904
Emecen-Huja P, Eubank TD, Shapiro V, Yildiz V, Tatakis DN, Leblebicioglu B (2013) Peri-implant versus periodontal wound healing. J Clin Periodontol 40(8):816–824
Onuma T, Aquiar K, Duarte PM, Feres M, Giro G, Coelho PG, Cassoni A, Shibli JA (2015) Levels of osteodastogenesis-related factors in the peri-implant crevicular fluid and clinical parameters of immediately loaded implants in patients with osteopenia: a short-term report. Int J Oral Maxillofac Implants 30(6):1431–1436
Dogan SB, Kurtis MB, Tuter G, Serdar M, Watanabe K, Karakis S (2015) Evaluation of clinical parameters and levels of proinflammatory cytokines in the crevicular fluid around dental implants in patients with type 2 diabetes mellitus. Int J Oral Maxillofac Implants 30(5):1119–1127
Tsoukaki M, Kalpidis CD, Sakellari D, Tsalikis L, Mikrogiorgis G, Konstantinidis A (2013) Clinical, radiographic, microbiological, and immunological outcomes of flapped vs. flapless dental implants: a prospective randomized controlled clinical trial. Clin Oral Implants Res 24(9):969–976
Taxel P, Ortiz D, Shafer D, Pendrys D, Reisine S, Rengasamy K, Freilich M (2014) The relationship between implant stability and bone health markers in post-menopausal women with bisphosphonate exposure. Clin Oral Investig 18(1):49–57
Güncü GN, Tözüm TF, Güncü MB, Yamalik N (2008) Relationships between implant stability, image-based measures and nitric oxide levels. J Oral Rehabil 35(10):745–753
Prati AJ, Casati MZ, Ribeiro FV, Cirano FR, Pastore GP, Pimentel SP, Casarin RCV, Author A, Division of Maxillofacial Surgery P, University SPB, Division of Periodontics PUS, Paulo B, Correspondence A, R.C.V. Casarin DoPPUSP and Brazil. Email cycb (2013) Release of bone markers in immediately loaded and nonloaded dental implants: a randomized clinical trial. J Dental Res 92(12):161S–167S
Basegmez C, Yalcin S, Yalcin F, Ersanli S, Mijiritsky E (2012) Evaluation of periimplant crevicular fluid prostaglandin E2 and matrix metalloproteinase-8 levels from health to periimplant disease status: a prospective study. Implant Dent 21(4):306–310
Raggatt LJ, Partridge NC (2010) Cellular and molecular mechanisms of bone remodeling. J Biol Chem 285(33):25103–25108
Gokmenoglu C, Ozmeric N, Erguder I, Elgun S (2014) The effect of light-emitting diode photobiomodulation on implant stability and biochemical markers in peri-implant crevicular fluid. Photomed Laser Surg 32(3):138–145
Slotte C, Lenneras M, Gothberg C, Suska F, Zoric N, Thomsen P, Nannmark U (2012) Gene expression of inflammation and bone healing in peri-implant crevicular fluid after placement and loading of dental implants. A kinetic clinical pilot study using quantitative real-time PCR. Clin Implant Dent Relat Res 14(5):723–736
Güncü MB, Aslan Y, Tümer C, Güncü GN, Uysal S (2008) In-patient comparison of immediate and conventional loaded implants in mandibular molar sites within 12 months. Clin Oral Implants Res 19(4):335–341
Tozum TF, Turkyilmaz I, Yamalik N, Tumer C, Kilinc A, Kilinc K, Karabulut E, Eratalay K (2005) Analysis of thte possible impact of inflammation severity and early and delayed loading on nitric oxide metabolism around dental implants. Int J Oral Maxillofac Implants 20(4):547–556
Gruber R, Nadir J, Haas R (2010) Neutrophil elastase activity and concentrations of interleukin 1-beta in crevicular fluid after immediate replacement and immediate loading of implants. Br J Oral Maxillofac Surg 48(3):228–231
Khoury SB, Thomas L, Walters JD, Sheridan JF, Leblebicioglu B (2008) Early wound healing following one-stage dental implant placement with and without antibiotic prophylaxis: a pilot study. J Periodontol 79(10):1904–1912
Nogueira-Filho G, Pesun I, Isaak-Ploegman C, Wijegunasinghe M, Wierzbicki T, McCulloch CA (2014) Longitudinal comparison of cytokines in peri-implant fluid and gingival crevicular fluid in healthy mouths. J Periodontol 85(11):1582–1588
Nowzari H, Botero JE, DeGiacomo M, Villacres MC, Rich SK (2008) Microbiology and cytokine levels around healthy dental implants and teeth. Clin Implant Dent Relat Res 10(3):166–173
Gurol C, Kazazoglu E, Dabakoglu B, Korachi M (2011) A comparative study of the role of cytokine polymorphisms interleukin-10 and tumor necrosis factor alpha in susceptibility to implant failure and chronic periodontitis. Int J Oral Maxillofac Implants 26(5):955–960
Dimitriou R, Tsiridis E, Giannoudis PV (2005) Current concepts of molecular aspects of bone healing. Injury 36(12):1392–1404
Wei L, Sun Y, Kong XF, Zhang C, Yue T, Zhu Q, He DY, Jiang LD (2016) The effects of dopamine receptor 2 expression on B cells on bone metabolism and TNF-alpha levels in rheumatoid arthritis. BMC Musculoskelet Disord 19(17):352
Lim HS, Park YH, Kim SK (2016) Relationship between serum inflammatory marker and bone mineral density in healthy adults. J Bone Metab 23(1):27–33
Lang NP, Salvi GE, Huynh-Ba G, Ivanovski S, Donos N, Bosshardt DD (2011) Early osseointegration to hydrophilic and hydrophobic implant surfaces in humans. Clin Oral Implants Res 22(4):349–356
Graves DT, Nooh N, Gillen T, Davey M, Patel S, Cottrell D, Amar S (2001) IL-1 plays a critical role in oral, but not dermal, wound healing. J Immunol 167(9):5316–5320
Carta S, Tassi S, Semino C, Fossati G, Mascagni P, Dinarello CA, Rubartelli A (2006) Histone deacetylase inhibitors prevent exocytosis of interleukin-1beta-containing secretory lysosomes: role of microtubules. Blood 108(5):1618–1626
Petkovic AB, Matic SM, Stamatovic NV, Vojvodic DV, Todorovic TM, Lazic ZR, Kozomara RJ (2010) Proinflammatory cytokines (IL-1beta and TNF-alpha) and chemokines (IL-8 and MIP-1alpha) as markers of peri-implant tissue condition. Int J Oral Maxillofac Surg 39(5):478–485
Jawa RS, Anillo S, Huntoon K, Baumann H, Kulaylat M (2011) Analytic review: interleukin-6 in surgery, trauma, and critical care: part I: basic science. J Intensive Care Med 26(1):3–12
Jawa RS, Anillo S, Huntoon K, Baumann H, Kulaylat M (2011) Interleukin-6 in surgery, trauma, and critical care part II: clinical implications. J Intensive Care Med 26(2):73–87
Tatli U, Damlar I, Erdogan O, Esen E (2013) Effects of smoking on periimplant health status and IL-1beta, TNF-alpha, and PGE2 levels in periimplant crevicular fluid: a cross-sectional study on well-maintained implant recall patients. Implant Dent 22(5):519–524
Rioux N, Castonguay A (2001) 4-(Methylnitrosamino)-1-(3-pyridyl)-1-butanone modulation of cytokine release in U937 human macrophages. Cancer Immunol Immunother 49(12):663–670
Takanashi S, Hasegawa Y, Kanehira Y, Yamamoto K, Fujimoto K, Satoh K, Okamura K (1999) Interleukin-10 level in sputum is reduced in bronchial asthma, COPD and in smokers. Eur Respir J 4:309–314
Zweers J, van Doornik A, Hogendorf EA, Quirynen M, Van der Weijden GA (2015) Clinical and radiographic evaluation of narrow- vs. regular-diameter dental implants: a 3-year follow-up. A retrospective study. Clin Oral Implants Res 26(2):149–156
Preoteasa E, Imre M, Preoteasa CT (2014) A 3-year follow-up study of overdentures retained by mini-dental implants. Int J Oral Maxillofac Implants 29(5):1170–1176
de Souza RF, Ribeiro AB, Della Vecchia MP, Costa L, Cunha TR, Reis AC, Albuquerque RF Jr (2015) Mini vs. standard implants for mandibular overdentures: a randomized trial. J Dental Res 94(10):1376–1384
Catalan A, Martinez A, Marchesani F, Gonzalez U (2016) Mandibular overdentures retained by two mini-implants: a seven-year retention and satisfaction study. J Prosthodont 25(5):364–370
Emami E, Cerutti-Kopplin D, Menassa M, Audy N, Kodama N, Durand R, Rompre P, de Grandmont P (2016) Does immediate loading affect clinical and patient-centered outcomes of mandibular 2-unsplinted-implant overdenture? A 2-year within-case analysis. J Dent 50:30–36
Gomes FI, Aragao MG, de Paulo Teixeira Pinto V, Gondim DV, Barroso FC, Silva AA, Bezerra MM, Chaves HV (2015) Effects of nonsteroidal anti-inflammatory drugs on osseointegration: a review. J Oral Implantol 41(2):219–230
Acknowledgments
The authors thank Neodent for supplying the dental implants used in the study. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
There was no grant support or funding for this study.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The research protocol was approved by the Ethics Committee of School of Dentistry (Number 1.267.086/2015), Federal University of Pelotas. Patients and their families or legal representatives provided signed written informed consent.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
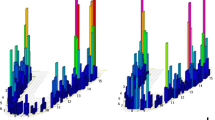
The original version of this article was revised: the results of the cytokine analyses (page 5 and Table 3) should be referred to as “median” instead of “means”. In addition, the significant differences between the categorized groups in the Figs. 1–4 were indicated by asterisks, but these asterisks disappeared during the conversion of the figures’ source files.
An erratum to this article is available at https://doi.org/10.1007/s00784-017-2191-2.
Rights and permissions
About this article
Cite this article
Bielemann, A.M., Marcello-Machado, R.M., Leite, F.R.M. et al. Comparison between inflammation-related markers in peri-implant crevicular fluid and clinical parameters during osseointegration in edentulous jaws. Clin Oral Invest 22, 531–543 (2018). https://doi.org/10.1007/s00784-017-2169-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-017-2169-0