Abstract
Objectives
The purposes of this study were to fabricate biodegradable polydioxanone (PDS II®) electrospun periodontal drug delivery systems (hereafter referred to as matrices) containing either metronidazole (MET) or ciprofloxacin (CIP) and to investigate the effects of antibiotic incorporation on both periodontopathogens and commensal oral bacteria.
Materials and methods
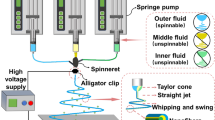
Fibrous matrices were processed from PDS polymer solution by electrospinning. Antibiotic-containing PDS solutions were prepared to obtain four distinct groups: 5 wt.% MET, 25 wt.% MET, 5 wt.% CIP, and 25 wt.% CIP. Pure PDS was used as a control. High-performance liquid chromatography (HPLC) was done to evaluate MET and CIP release. Dual-species biofilms formed by Lactobacillus casei (Lc) and Streptococcus salivarius (Ss) were grown on the surface of all electrospun matrices. After 4 days of biofilm growth, the viability of bacteria on biofilms was assessed. Additionally, antimicrobial properties were evaluated against periodontopathogens Fusobacterium nucleatum (Fn) and Aggregatibacter actinomycetemcomitans (Aa) using agar diffusion assay.
Results
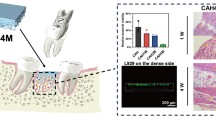
A three-dimensional interconnected porous network was observed in the different fabricated matrices. Pure PDS showed the highest fiber diameter mean (1,158 ± 402 nm) followed in a descending order by groups 5 wt.% MET (1,108 ± 383 nm), 25 wt.% MET (944 ± 392 nm), 5 wt.% CIP (871 ± 309 nm), and 25 wt.% CIP (765 ± 288 nm). HPLC demonstrated that groups containing higher amounts (25 wt.%) of incorporated drugs released more over time, while those with lower levels (5 wt.%) the least. No inhibitory effect of the tested antibiotics was detected on biofilm formation by the tested commensal oral bacteria. Meanwhile, CIP-containing matrices inhibited growth of Fn and Aa.
Conclusion
CIP-containing matrices led to a significant inhibition of periodontopathogens without negatively impairing the growth of periodontal beneficial bacteria.
Clinical relevance
Based on the proven in vitro inhibition of periodontitis-related bacteria, future in vivo research using relevant animal models is needed to confirm the effectiveness of these drug delivery systems.




Similar content being viewed by others
References
Walker CB, Karpinia K (2002) Rationale for use of antibiotics in periodontics. J Periodontol 73:1188–1196
Xajigeorgiou C, Sakellari D, Slini T, Baka A, Konstantinidis A (2006) Clinical and microbiological effects of different antimicrobials on generalized aggressive periodontitis. J Clin Periodontol 33:254–264
Serrano C, Torres N, Valdivieso C, Castano C, Barrera M, Cabrales A (2009) Antibiotic resistance of periodontal pathogens obtained from frequent antibiotics users. Acta Odontol Latinoam 22:99–104
Ardila CM, Granada MI, Guzman IC (2010) Antibiotic resistance of subgingival species in chronic periodontitis patients. J Periodontol Res 45:557–563
Aminov RI (2009) The role of antibiotics and antibiotic resistance in nature. Environ Microbiol 11:2970–2988
Sullivan A, Edlund C, Nord CE (2001) Effect of antimicrobial agents on the ecological balance of human microflora. Lancet Infect Dis 1:101–114
Koll-Klais P, Mandar R, Leibur E, Marcotte H, Hammarstrom L, Mikelsaar M (2005) Oral lactobacilli in chronic periodontitis and periodontal health: species composition and antimicrobial activity. Oral Microbiol Immunol 20:354–361
van Hoogmoed CG, Geertsema-doornbusch GI, Teughels W, Quirynen M, Busscher HJ, van der Mei HC (2008) Reduction in periodontal pathogens adhesion by antagonistic strains. Oral Microbiol Immunol 23:43–48
Bottino MC, Thomas V, Schmidt G, Vohra YK, Chu TM, Kowolik MJ, Janowski GM (2012) Recent advances in the development of GTR/GBR membranes for periodontal regeneration—a materials perspective. Dent Mater 28:703–721
Bottino MC, Thomas V, Janowski GM (2011) A novel spatially designed and functionally graded electrospun membrane for periodontal regeneration. Acta Biomater 7:216–224
Rodrigues RMJ, Goncalves C, Souto R, Feres-Filho EJ, Uzeda M, Colombo APV (2004) Antibiotics resistance profile of the subgingival microbiota following systemic or local tetracycline therapy. J Clin Periodontol 31:420–427
Killoy WJ (1999) Local delivery of antimicrobials: a new era in the treatment of adult periodontitis. Compend Contin Educ Dent 20:13–18
Killoy WJ (2002) The clinical significance of local chemotherapies. J Clin Periodontol 29:22–29
Rams TE, Slots J (1996) Local delivery of antimicrobial agents in the periodontal pocket. Periodontol 10:139–159, 2000
Thomas V, Zhang X, Vohra YK (2009) A biomimetic tubular scaffold with spatially designed nanofibers of protein/PDS bio-blends. Biotechnol Bioeng 104:1025–1033
Cui W, Li X, Zhu X, Yu G, Zhou S, Weng J (2006) Investigation of drug release and matrix degradation of electrospun poly(DL-lactide) fibers with paracetanol inoculation. Biomacromolecules 7(5):1623–1629
Guggenheim B, Giertsen E, Schupbach P, Shapiro S (2001) Validation of an in vitro biofilm model of supragingival plaque. J Dent Res 80:363–370
Stookey GK, Stahlman DB (1976) Enhanced fluoride uptake in enamel with a fluoride-impregnated prophylactic cup. J Dent Res 55:333–341
Bottino MC, Kamocki K, Yassen GH, Platt JA, Vail MM, Ehrlich Y, Spolnik KJ, Gregory RL (2013) Bioactive nanofibrous scaffolds for regenerative endodontics. J Dent Res 92(11):963–969
Reise M, Wyrwa R, Müller U, Zylinski M, Völpel A, Schnabelrauch M, Berg A, Jandt KD, Watts DC, Sigusch BW (2012) Release of metronidazole from electrospun poly(L-lactide-co-D/L-lactide) fibers for local periodontitis treatment. Dent Mater 28(2):179–188
Aas JA, Paster BJ, Stokes LN, Olsen I, Dewhirst FE (2009) Defining the normal bacterial flora of the oral cavity. J Clin Microbiol 43:5721–5732
Duan K, Sibley CD, Davidson CJ, Surette MG (2009) Chemical interactions between organisms in microbial communities. Contrib Microbiol 16:1–17
Socransky SS, Haffajee AD (1992) The bacterial etiology of destructive periodontal disease: current concepts. J Periodontol 63:322–331
Teughels W, Kinder Haake S, Sliepen I, Pauwels M, van Eldere J, Cassiman J, Quirynen M (2007) Bacteria interfere with A. actinomycetemcomitans colonization. J Dent Res 86:611–617
Sliepen I, Hofkens J, van Essche M, Quirynen M, Teughels W (2008) Aggregatibacter actinomycetemcomitans adhesion inhibited in a flow cell. Oral Microbiol Immunol 23:520–524
Suci P, Young M (2011) Selective killing of Aggregatibacter actinomycetemcomitans by ciprofloxacin during development of a dual species biofilm with Streptococcus sanguinis. Arch Oral Biol 56:1055–1063
Elyzol® Colgate. http://colgate-sensitive-pro-relief.colgateprofessional.ro/products/Colgate-Elyzol-25-Dental-Gel/faqs. Accessed 21 January 2014
Chow AW, Patten V, Guze LB (1975) Susceptibility of anaerobic bacteria to metronidazole: relative resistance of non-spore-forming gram-positive baccilli. J Infect Dis 131(2):182–185
Shaddox LM, Walker C (2009) Microbial testing in periodontics: value, limitations and future directions. Periodontol 2000(50):25–38
Kalsi R, Vandana K, Prakash S (2011) Effect of local drug delivery in chronic periodontitis patients: a meta-analysis. J Indian Soc Periodontol 15(4):304–309
Riep B, Purucker P, Bernimoulin J (1999) Repeated local metronidazole-therapy as adjunct to scaling and root planing in maintenance patients. J Clin Periodontol 26(11):710–715
Salvi G, Mombelli A, Mayfield L, Rutar A, Suvan J, Garrett S, Lang N (2002) Local antimicrobial therapy after initial periodontal treatment. J Clin Periodontol 29(6):540–550
Boland ED, Coleman BD, Barnes CP, Simpson DG, Wnek GE, Bowlin GL (2005) Electrospinning polydioxanone for biomedical applications. Acta Biomater 1(1):115–123
Acknowledgments
This work was supported in part by the Research Support Funds Grant (RSFG) at Indiana University-Purdue University Indianapolis (IUPUI), by start-up funds from the IU School of Dentistry, and the NIH-NIDCR (Grant # DE023552) (all to M.C.B.).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Marco C. Bottino and Rodrigo A. Arthur contributed equally to this manuscript
Rights and permissions
About this article
Cite this article
Bottino, M.C., Arthur, R.A., Waeiss, R.A. et al. Biodegradable nanofibrous drug delivery systems: effects of metronidazole and ciprofloxacin on periodontopathogens and commensal oral bacteria. Clin Oral Invest 18, 2151–2158 (2014). https://doi.org/10.1007/s00784-014-1201-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-014-1201-x