Abstract
Objectives
Topical hemostatic agents are used in all surgical disciplines. Most of these hemostats are based on animal-derived products like collagen and gelatin. They carry the potential risk of pathogen transmission. A newly developed biodegradable, fully synthetic hemostatic agent based on polyurethane foam (PU) with 55 % polyethylene glycol (PEG) would prevent these potential risks.
Materials and methods
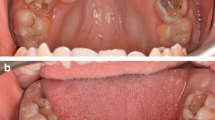
The hemostatic efficacy of this new agent was compared to gelatin and collagen in humans who underwent extraction of an upper and lower molar (split-mouth model). After extraction of a molar in the maxilla and mandible, a PU foam and collagen or gelatin were inserted in the extraction socket for 2 min. Hereafter, the agents were removed and stored in ethylenediaminetetraacetic acid to stop coagulation. Then, the concentration of coagulation parameters thrombin–antithrombin III (TAT) complexes, fibrinogen, and thromboxane B2 (TxB2) in blood extracts from the agents was measured. The concentrations were also determined in baseline blood samples which were collected from the extraction socket.
Results
The concentrations of TAT and TxB2 were significantly increased, and fibrinogen concentration was significantly reduced compared to baseline wound blood concentrations indicating enhanced hemostasis. No significant differences were seen in the concentrations of these coagulation parameters in the three different hemostatic agents.
Conclusions
These results show that PU combined with 55 % PEG is a promising alternative for the animal-derived hemostatic agents.
Clinical relevance
The synthetic hemostatic agent could replace the animal-derived products like collagen and gelatin and therewith prevent the potential risk of pathogen transmission.



Similar content being viewed by others
References
Nemoto T, Horiuchi M, Ishiguro N, Shinagawa M (1999) Detection methods of possible prion contaminants in collagen and gelatin. Arch Virol 144(1):177–84
Lutolf MP, Hubbell JA (2005) Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat Biotechnol 23(1):47–55
van Minnen B, van Leeuwen MB, Kors G, Zuidema J, van Kooten TG, Bos RR (2008) In vivo resorption of a biodegradable polyurethane foam, based on 1,4-butanediisocyanate: a three-year subcutaneous implantation study. J Biomed Mater Res A 85(4):972–82
Visscher SH, van Minnen B, van Leeuwen MB, van Kooten TG, Bos RR (2009) Closure of oroantral communications using biodegradable polyurethane foam: a long term study in rabbits. J Biomed Mater Res B 91(2):957–63
Gorbet MB, Sefton MV (2004) Biomaterial-associated thrombosis: roles of coagulation factors, complement, platelets and leukocytes. Biomaterials 25(26):5681–703
Broekema FI, van Oeveren W, Zuidema J, Visscher SH, Bos RR (2011) In vitro analysis of polyurethane foam as a topical hemostatic agent. J Mater Sci Mater Med 22(4):1081–6
Furie B, Furie BC (2007) In vivo thrombus formation. J Thromb Haemost 1:12–17
Pelzer H, Schwarz A, Heimburger N (1988) Determination of human thrombin-antithrombin III complex in plasma with an enzyme-linked immunosorbent assay. Thromb Haemost 59(1):101–6
Davie EW, Fujikawa K, Kisiel W (1991) The coagulation cascade: initiation, maintenance, and regulation. Biochemistry 30(43):10363–70
Kamath S, Blann AD, Lip GY (2001) Platelet activation: assessment and quantification. Eur Heart J 22(17):1561–71
Monroe DM, Hoffman M, Oliver JA, Roberts HR (1997) Platelet activity of high-dose factor VIIa is independent of tissue factor. Br J Haematol 99(3):542–7
Skarja GA, Brash JL (1997) Physicochemical properties and platelet interactions of segmented polyurethanes containing sulfonate groups in the hard segment. J Biomed Mater Res 34(4):439–55
Elwing H (1998) Protein absorption and ellipsometry in biomaterial research. Biomaterials 19(4–5):397–406
Thatte HS, Zagarins SE, Amiji M, Khuri SF (2004) Poly-N-acetyl glucosamine-mediated red blood cell interactions. J Trauma 57(1 Suppl):S7–12
Kanko M, Liman T, Topcu S (2006) A low-cost and simple method to stop intraoperative leakage-type bleeding: use of the vancomycin-oxidized regenerated cellulose (ORC) sandwich. J Invest Surg 19(5):323–7
Schonauer C, Tessitore E, Barbagallo G, Albanese V, Moraci A (2004) The use of local agents: bone wax, gelatin, collagen, oxidized cellulose. Eur Spine J 13(1):S89–96
Palm MD, Altman JS (2008) Topical hemostatic agents: a review. Dermatol Surg 34(4):431–45
Hong YM, Loughlin KR (2006) The use of hemostatic agents and sealants in urology. J Urol 176(6 Pt 1):2367–74
Msezane LP, Katz MH, Gofrit ON, Shalhav AL, Zorn KC (2008) Hemostatic agents and instruments in laparoscopic renal surgery. J Endourol 22(3):403–8
Alexander JM, Rabinowitz JL (1978) Microfibrillar collagen (avitene) as a hemostatic agent in experimental oral wounds. J Oral Surg 36(3):202–5
Wagner WR, Pachence JM, Ristich J, Johnson PC (1996) Comparative in vitro analysis of topical hemostatic agents. J Surg Res 66(2):100–8
Jorgensen LN, Lind B, Hauch O, Leffers A, Albrecht-Beste E, Konradsen LA (1990) Thrombin-antithrombin III-complex & fibrin degradation products in plasma: surgery and postoperative deep venous thrombosis. Thromb Res 59(1):69–76
Kannel WB, Wolf PA, Castelli WP, D'Agostino RB (1987) Fibrinogen and risk of cardiovascular disease: the Framingham study. JAMA 258(9):1183–6
Patrono C, Ciabattoni G, Pugliese F, Pierucci A, Blair IA, FitzGerald GA (1986) Estimated rate of thromboxane secretion into the circulation of normal humans. J Clin Invest 77(2):590–4
Albrechtsen OK, Thaysen JH (1955) Fibrinolytic activity in human saliva. Acta Physiol Scand 35(2):138–45
Acknowledgments
The authors gratefully acknowledge R. de Graaf, J. Jankie, and B.C. Bhat for the development and production of the PU sponges. We thank Dr. J.J.R. Huddleston Slater for his contribution to the study design.
Conflict of interest
This study was financially supported by Polyganics BV and the University Medical Center Groningen, The Netherlands.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Broekema, F.I., van Oeveren, W., Selten, M.H.A. et al. In vivo hemostatic efficacy of polyurethane foam compared to collagen and gelatin. Clin Oral Invest 17, 1273–1278 (2013). https://doi.org/10.1007/s00784-012-0809-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-012-0809-y