Abstract
Background
Techniques of cemented total hip arthroplasty have developed over time. We present the outcomes of Charnley total hip arthroplasty performed using improved second- and third-generation cementing techniques.
Methods
We reviewed the radiologic results of 91 Charnley total hip arthroplasties performed using second- and third-generation cementing techniques. Second-generation techniques involved making multiple anchor holes, a double-cementing method on the acetabular side and an intramedullary plug, and retrograde filling with a cement gun on the femoral side in 57 hips. Third-generation techniques involved additional vacuum mixing and cement pressurization in 34 hips.
Results
Joint survival rates at 20 years when using second-generation techniques were 89% for the socket and 94% for the stem with aseptic loosening as the end point; the survival rates at 10 years when using third-generation techniques were 97 and 100%, respectively. According to our radiographic evaluation system for the clear zone at 5 years, there was less clear zone in the acetabular side with the third-generation techniques than with second-generation techniques. In the femoral side, there was very little development of the clear zone, but the difference between generations was not significant.
Conclusions
Second- and third-generation cementing techniques showed excellent survivorship. The clear zone scores at 5 years indicated that third-generation techniques were effective, especially in the acetabular side, and may produce better long-term results than second-generation techniques.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Charnley low-friction arthroplasty is the gold standard for cemented hip replacement [1]. Several authors have reported favorable long-term results of Charnley total hip arthroplasty over 30 years of follow-up [2–4]. The quality of the cementing is as essential to the success of the procedure as the principle of implant design. Cementing techniques have evolved with time, and so the purpose of this study was to review the radiologic outcome of Charnley total hip arthroplasty using improved cementing techniques and to confirm the effects of modified third-generation techniques.
Materials and methods
We reviewed the outcomes of 91 primary total hip arthroplasties in which the Charnley prosthesis and improved cementing techniques were used in 87 patients with a diagnosis of hip osteoarthritis. The total hip arthroplasties were performed by multiple surgeons, and details of the surgical procedures and implants were identified in the surgical records. From among 132 Charnley total hip arthroplasties performed between July 1983 and March 1995, the surgical techniques could not be identified for 27 hips, and 6 patients (6 hips) died before 10 years follow-up, and another 42 hips were lost to follow-up at 10 years. Thus, 57 hips were selected on the basis of the requirements that so-called second-generation techniques were used and there was a minimum follow-up duration of 10 years. The average age of the patients at surgery was 64.9 years (range 52–78 years), and the average duration of follow-up was 14.5 years (range 10–21 years). Among 45 Charnley total hip arthroplasties performed between December 1998 and March 2001, 11 hips were lost to follow-up at 5 years. Thus, 34 hips were selected on the basis of the requirements that modified third-generation techniques were used and there was a minimum follow-up duration of 5 years. The average age of the patients at surgery was 66.8 years (range 51–85 years), and the average duration of follow-up was 8.4 years (range 5–11 years).
Operative techniques
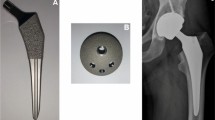
In all patients, Charnley prostheses (22 mm metal head, ultra-high molecular weight polyethylene) were implanted using Simplex P cement via a posterior approach. Our second-generation techniques included the preparation of multiple anchor holes, the use of a rotary brush, jet lavage, the double-cementing method, and placement of a Charnley unflanged socket in the acetabular side. The acetabulum was usually reamed through the subchondral bone plate, and the preserved subchondral bone at the periphery and/or eburnated bone at the roof were treated to be as rough as possible. The double-cementing method meant that 50% less cement in a relatively low viscosity stage could be finger-packed into the acetabulum with multiple anchor holes, mainly in the peripheral area for cement penetration as the first step. Then in the second step, the remaining 50% of the cement in a relatively high viscosity stage was placed on top as the filler just before socket insertion. For the femoral side, the preparation involved a rotary reamer, rotary brush, jet lavage, an intramedullary plug, and retrograde filling with a cement gun, and a Charnley flanged stem was used (Fig. 1a). Our third-generation techniques included preparation with an H2O2-impregnated sponge and improvements such as cement pressurization and vacuum mixing as additions to the second-generation techniques. Third-generation techniques included use of the Exeter-type balloon pressurizer after the first step of the double-cementing method, and the Charnley flanged socket in the acetabular side. The femoral seal was placed over the proximal opening during pressurization after retrograde filling in the femoral side. The Charnley flanged stem was used in 6 hips while the Charnley Elite Plus stem was used in 28 hips (Fig. 1b).
Radiographic method
Kaplan–Meier survival analysis was performed with aseptic loosening and revision for aseptic loosening as end points. Loosening was defined as the migration or presence of a continuous clear zone at the bone–cement interface, using the modified criteria of Hodgkinson et al. [5] for the socket and Harris et al. [6] for the stem. The clear zone referred to radiolucency with the reactive line of the bone sclerosis. We devised a clear zone scoring system (CZ score) in 1993 and have used it to evaluate the quality of the cement–bone interface. To score the cement–bone interface, the acetabulum was divided into 12 areas and the femur was divided into 18 areas. The CZ score represents the sum of points according to the width of the clear zone in each area. For example, a continuous clear zone of width 1 mm showed 24 points in the acetabular side and 36 points in the femoral side (Fig. 2).
Statistical analysis was performed using the Mann–Whitney U test (StatView version 5.0 software), and the survival rates were compared using the logrank test (SPSS 15.0J software). Differences with a P value <0.05 were considered significantly significant.
This study was approved by the Institutional Review Board of Aichi Medical University.
Results
Seven acetabular components and three femoral components were judged to have undergone aseptic loosening in the second-generation group. The survival rates at 20 years were 88.7 ± 4.4% of the acetabular component and 94.0 ± 3.5% of the femoral component with aseptic loosening as the end point (Fig. 3); the survival rates at 10 years were 90.8 ± 3.9 and 96.5 ± 2.4%, respectively, in the second-generation group. Only one acetabular component was judged to have undergone aseptic loosening in the third-generation group, and the survival rates at 10 years were 97.1 ± 2.9% of the acetabular component and 100% of the femoral component with aseptic loosening as the end point (Fig. 4). There was no significant difference in survival rates at 10 years between the two generation groups.
Two acetabular components and one femoral component required revision for aseptic loosening, and one stable stem was exchanged at the time of acetabular revision using a cement-within-cement technique with ultrasonic tools [7, 8] in the second-generation group. The survival rates at 20 years were 93.0 ± 5.3% of the acetabular component and 98.2 ± 1.8% of the femoral component, with revision for aseptic loosening as the end point (Fig. 5). None of the components required revision because of aseptic loosening in the third-generation group.
The average CZ scores at 5 years were 9.3 ± 5.6 points for loosened sockets and 2.4 ± 2.2 points for stable sockets, and 11.7 ± 16.9 for loosened stems and 0.4 ± 1.3 points for stable stems, revealing a significant difference between loosened sockets and stable sockets (Fig. 6). The average CZ scores at 5 years were 3.9 ± 3.3 points for sockets with second-generation techniques and 1.4 ± 2.4 points for sockets with third-generation techniques, and 1.2 ± 4.3 points for stems with second-generation techniques and 0.03 ± 0.2 points for stems with third-generation techniques. The CZ scores showed a significant difference between the generations for the sockets. The CZ score was very low when using stems with the third-generation techniques, but the difference between generations was not significant (Fig. 7).
Discussion
The evolution of femoral cementing techniques is conventionally described in terms of generations [9, 10]. First-generation techniques involved finger-packing cement into an unplugged canal. Second-generation techniques involved plugging the medullary canal, cleaning the canal with pulsatile lavage, and using a retrograde cement gun. Third-generation techniques involved reduction of cement porosity and pressurization of cement as additions to the second-generation techniques. In contrast to these femoral cementing techniques, the techniques for acetabular cementing have not been clearly classified into generations.
Clinical results have been described in the literature for improved cementing techniques. Smith et al. [11] reported a survival rate of 88% at 18 years, and Buckwalter et al. [12] reported a survival rate of 80% over 25 years with revision of the femoral component for aseptic loosening defined as the end point in second-generation techniques. Williams et al. [13] reported a survival rate of 100% at 12 years with revision of the femoral component for aseptic loosening as the end point with the use of a polished tapered stem and so-called contemporary cementing techniques. Rasquinha et al. [14] reported a survival rate of 100% at 15 years with revision of the femoral component for aseptic loosening as the end point in the third-generation techniques. de Jong et al. [15] reported a survival rate of 99% at 20 years using revision of the acetabular component for aseptic loosening as the end point, with reaming to the depth of the subchondral layer, making 6–8 multiple anchorage holes, and impaction of cancellous bone into the holes as second-generation techniques. In our series, the survival rates of second- and third-generation groups were comparable to those of the abovementioned studies.
Our study has two limitations. First, although it would have been preferable for comparative purposes to use the same stem in all cases, 6 Charnley flanged stems and 28 Charnley Elite Plus stems were used in the third-generation techniques. The Charnley Elite Plus stem was developed by preserving the major features of the Charnley flanged stem [16], and Kalairajah et al. [16] and Kim et al. [17] found outcomes with the Charnley Elite Plus stem to be similar to those with the conventional Charnley stem. With this in mind, we decided to adopt the Charnley Elite Plus stem as the main prosthesis in this series.
Second, the follow-up period was too different for the two generation groups in the present study to allow a comparison of long-term outcome. Hence, we adopted the CZ score to predict the prognosis. Ranawat et al. [18] and Flivik et al. [19] have shown that early findings of a radiolucent line on the cement–bone interface can predict the longevity of a cemented cup with high accuracy. Our study also showed that the CZ scores of the loosened cups were significantly greater than those of the stable cups at 5 years. In addition, the CZ scores at 5 years decreased significantly for the cup and showed very few points for the stem in the third-generation group. Accordingly, we consider that the third-generation techniques will provide excellent long-term outcome, and the long-term effects of third-generation techniques in the acetabular side especially may surpass those of second-generation techniques.
While the mid-term results for the third-generation group improved substantially with better cementing, a continuous clear zone at the cement–bone interface was seen in only one cup with the third-generation techniques. A reason for this may be poor cement penetration into the bone because of retention of the subchondral bone plate. The radiographs showed that the clear zone had progressed to all areas at 4 years after surgery in case (a) with wide retention of the subchondral bone plate, and no clear zone was apparent at 4 years postoperatively in case (b) with the removal of the subchondral bone plate (Fig. 8). Both patients underwent our third-generation technique, and in the acetabulum side, case (a) had wide retention of the subchondral bone plate which was treated to be rough after reaming according to the surgical records. The radiographs showed that cement had penetrated into the cancellous bone as the initial interlock in case (b), whereas the cement–bone interface was relatively clear in case (a) immediately after surgery (Fig. 8). Eftekher and Tzitzikalakis [20] and Kobayashi et al. [21, 22] reported that retention of the subchondral bone plate with multiple holes drilled in it was important during acetabular preparation. However, Flivik et al. [23] demonstrated that removing the subchondral bone plate improved the cement–bone interface without jeopardizing the initial stability and implied better long-term cup survival. We theoretically agree with removing the subchondral bone plate; however, in reality, it appears that perfect removal is impossible without degradation of the bone bed. Therefore, we perforate the thick and sclerotic bone plate to get anchoring holes [24] and additionally try to use the interface bioactive bone cement technique to achieve an enduring physicochemical bond by interposing osteoconductive crystal hydroxyapatite granules at the cement–bone interface [25, 26] for cases with wide retention of the subchondral bone plate after reaming.
In conclusion, second- and third-generation techniques showed excellent outcomes for the femoral components. The CZ scores at 5 years indicated that third-generation techniques were effective in the acetabular side and may produce better long-term results than second-generation techniques, but further improvements are required in the preparation of the bone bed.
References
Nerssian OA, Martin G, Joshi RP, Su BW, Eftekhar NS. A 15- to 25-year follow-up study primary Charnley low-friction arthroplasty. A single surgeon series. J Arthroplast. 2005;20:162–7.
Callaghan JJ, Bracha P, Liu SS, Piyaworakhun S, Goetz DD, Johnston RC. Survivorship of a Charnley total hip arthroplasty. A concise follow-up, at a minimum of thirty-five years, of previous reports. J Bone Jt Surg Am. 2009;91:2617–21.
Mullins MM, Norbury W, Dowell JK, Heywood-Waddington M. Thirty-year results of a prospective study of Charnley total hip arthroplasty by the posterior approach. J Arthroplast. 2007;22:833–9.
Wroblewski BM, Siney PD, Fleming PA. Charnley low-frictional torque arthroplasty. Follow-up for 30 to 40 years. J Bone Jt Surg Br. 2009;91:447–50.
Hodgkinson JP, Maskell AP, Paul A, Wroblewski BM. Flanged acetabular components in cemented Charnley hip arthroplasty. Ten-year follow-up of 350 patients. J Bone Jt Surg Br. 1993;75:464–7.
Harris WH, Mccarthy JC Jr, O’neill DA. Femoral component loosening using contemporary techniques of femoral cement fixation. J Bone Jt Surg Am. 1982;64:1063–7.
Lieberman JR, Moeckel BH, Evans BG, Salvati EA, Ranawat CS. Cement-within-cement revision hip arthroplasty. J Bone Jt Surg Br. 1993;75:869–71.
McCallum JD III, Hozack WJ. Recementing a femoral component into a stable cement mantle using ultrasonic tools. Clin Orthop. 1995;319:232–7.
Dalury DF. The technique of cemented total hip replacement. Orthopedics. 2005;28(Suppl):s853–6.
Maloney WJ, Kang MN, Hartfort JM. The cemented femoral component. In: Callaghan JJ, Rosenberg AG, Rubash HE, editors. The adult hip, vol. 2. 2nd ed. Philadelphia: Lippincott Williams & Wilkins; 2007. p. 917–39.
Smith SW, Estok DM, Harris WH. Total hip arthroplasty with use of second-generation cementing techniques. An eighteen-year-average follow-up study. J Bone Jt Surg Am. 1998;80:1632–40.
Buckwalter AE, Callaghan JJ, Liu SS, Pedersen DR, Goetz DD, Sullivan PM, Leinen JA, Johnston RC. Results of Charnley total hip arthroplasty with use of improved femoral cementing techniques. A concise follow-up, at minimum of twenty-five years, of a previous report. J Bone Jt Surg Am. 2006;88:1481–5.
Williams HDW, Browne G, Gie GA, Ling RSM, Timperley AJ, Wendover NA. The Exeter universal cemented femoral component at 8 to 12 years. A study of the first 325 hips. J Bone Jt Surg Br. 2002;84:324–34.
Rasquinha VJ, Dua V, Rodriguez JA, Ranawat CS. Fifteen-year survivorship of a collarless, cemented, normalized femoral stem in primary hybrid total hip arthroplasty with a modified third-generation cement technique. J Arthroplast. 2003;18(Suppl 1):86–94.
de Jong PT, de Man FHR, Haverkamp D, Marti RK. The long-term outcome of the cemented Weber acetabular component in total hip replacement using a second-generation cementing technique. J Bone Jt Surg Br. 2009;91:31–6.
Kalairajah Y, Azurza K, Molloy S, Hulme C, Cronin M, Drabu KJ. Is Charnley evolution working? A five-year outcome study. Acta Orthop Belg. 2004;70:315–21.
Kim YH, Kim JS, Yoon SH. Long-term survivalship of the Charnley Elite Plus femoral component in young patients. J Bone Jt Surg Br. 2007;89:449–54.
Ranawat CS, Deshmukh RG, Peters LE, Umlas ME. Prediction of the long-term durability of all-polyethylene cemented socket. Clin Orthop. 1995;317:89–105.
Flivik G, Sanfridsson J, Ӧnnerfält R, Kesteris U, Ryd L. Migration of the acetabular component: effect of cement pressurization and significance of early radiolucency. Acta Orthop. 2005;76:159–68.
Eftekher NS, Tzitzikalakis GI. Failures and reoperations following low-friction arthroplasty of the hip. A five- to fifteen-year follow-up study. Clin Orthop. 1986;211:65–77.
Kobayashi S, Terayama K. Radiology of low-friction arthroplasty of the hip. A comparison of socket fixation techniques. J Bone Jt Surg Br. 1990;72:439–43.
Kobayashi S, Eftekhar NS, Terayama K, Iorio R. Risk factors affecting radiological failure of the socket in primary Charnley low friction arthroplasty. A 10- to 20-year follow-up study. Clin Orthop. 1994;306:84–96.
Flivik G, Kristiansson I, Kesteris U, Ryd L. Is removal of subchondral bone plate advantageous in cemented cup fixation? A randomized RSA study. Clin Orthop. 2006;448:164–72.
Crites BM, Berend ME, Ritter MA. Technical consideration of cemented acetabular components. A 30-year evaluation. Clin Orthop. 2000;381:114–9.
Oonishi H, Kadoya Y, Iwaki H, Kin N. Total hip arthroplasty with a modified cementing technique using hydroxyapatite granules. J Arthroplast. 2001;16:784–9.
Oonishi H, Ohashi H, Oonishi H, Kim SC. THA with hydroxyapatite granules at cement–bone interface. 15- to 20-year results. Clin Orthop. 2008;466:373–9.
Conflict of interest
No benefits or funds were received in support of this study.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Hirose, S., Otsuka, H., Morishima, T. et al. Outcomes of Charnley total hip arthroplasty using improved cementing with so-called second- and third-generation techniques. J Orthop Sci 17, 118–123 (2012). https://doi.org/10.1007/s00776-011-0180-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-011-0180-x