Abstract
Background
Aggressive vertebral hemangiomas causing spinal compression are rare, and there is controversy with regard to treatment. The purpose of this study was to evaluate the clinical results of patients with aggressive vertebral hemangiomas at a mean follow-up of more than 10 years after total excision and discuss the treatment options for the tumors.
Methods
We performed a retrospective review of patients with aggressive vertebral hemangiomas who were treated with total excision. The surgeries were carried out on five patients (average age 47 years). In all five patients, the tumor was in the thoracic spine and was causing myelopathy with extraosseous extension. There were three tumors of type 5 and two of type 6 according to Tomita’s surgical classification of spinal tumors. The tumors were assessed using magnetic resonance imaging (MRI), and the clinical results were evaluated.
Results
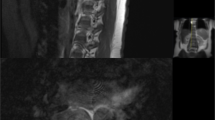
All of the tumors showed low-intensity or low-isointensity signal on T1-weighted MRI. All five patients had a combination of preoperative transarterial embolization and total excision including tumor margin. Total en bloc excisions were performed in two patients. En bloc and piecemeal combined total excisions were performed in two patients. Piecemeal total excision was performed in one patient. Intraoperative blood loss ranged from 1580 to 3400 ml (mean 2424 ml). There were no perioperative complications. According to the Japanese Orthopaedic Association score, the myelopathy improved after the surgery from 5.3 ± 2.9 to 9.8 ± 1.7 (total of 11 points). None of the patients have had a recurrence at a mean followup of 135.2 months (range 92–163 months).
Conclusions
We performed a combination of preoperative transarterial embolization and total excision for aggressive vertebral hemangiomas with extraosseous extension that were causing spinal cord compression in all five cases. The results in the long-term follow-up have proved satisfactory.
Similar content being viewed by others
References
Hemmy DC. Vertebral hemangiomas. In: Neurosurgery. Wilkins RH, Rengachary SS, editors. New York: McGraw-Hill; 1996. p. 1827–1829.
Dagi TF, Schmidek HH. Vascular tumors of the spine. In: Sundaresan N, Schmidek HH, Schiller AL, Rosenthal DI, editors. Tumors of the spine: diagnosis and clinical management. Philadelphia: Saunders; 1990. p. 181–191.
Reizine D, Laredo JD, Riche MC. Vertebral hemangiomas. In: Jeanmart L, editor. Radiology of the spine: tumours. Berlin: Springer-Verlag; 1986. p. 73–80.
Healy M, Herz DA, Pearl L. Spinal hemangiomas. Neurosurgery 1983;13:689–691.
Nguyen JP, Djindjian M, Gaston A. Vertebral hemangiomas presenting with neurologic symptoms. Surg Neurol 1987;27:391–397.
Tomita K, Kawahara N, Baba H, Tsuchiya H, Fujita T, Toribatake Y. Total en bloc spondylectomy: a new surgical technique for primary malignant vertebral tumors. Spine 1997;22:324–333.
Japanese Orthopaedic Association. Scoring system for cervical myelopathy. J Jpn Assoc 1994;68:490–503.
Laredo JD, Assouline EA, Gelbert F, Wybier M, Merland JJ, Tubiana JM. Vertebral hemangiomas: fat content as a sign of aggressiveness. Radiology 1990;177:467–472.
Fujita T, Kawahara K, Tomita K, Ueda Y. Analysis on the MRI and histologic findings of symptomatic vertebral hemangioma. J Cent Jpn Orthop Traum 1999;42:571–572 (in Japanese).
Bas T, Aparisi F, Bas JL. Efficacy and safety of ethanol injections in 18 cases of vertebral hemangioma: a mean follow-up of 2 years. Spine 2001;26:1577–1582.
Doppman JL, Oldfield EH, Heiss JD. Symptomatic vertebral hemangiomas: treatment by means of direct intralesional injection of ethanol. Radiology 2000;214:341–348.
Niemeyer T, McClellan J, Webb J, Jaspan T, Ramli N. Brown-Sequard syndrome after management of vertebral hemangioma with intralesional alcohol: a case report. Spine 1999;24:1845–1847.
Goyal M, Mishra NK, Sharma A, Gaikwad SB, Mohanty BK, Sharma S. Alcohol ablation of symptomatic vertebral hemangiomas. AJNR Am J Neuroradiol 1999;20:1091–1096.
Miszczyk L, Ficek K, Trela K, Spindel J. The efficacy of radiotherapy for vertebral hemangiomas. Neoplasma 2001;48:82–84.
Brankrock S, Krull A, Schwarz R, Alberti W. Results of radiotherapy for vertebral hemangioma. Strahlenther Onkol 1999;175:405–408.
Fox MW, Onofrio BM. The natural history and management of symptomatic and asymptomatic vertebral hemangiomas. J Neurosurg 1993;78:36–45.
Acosta FL, Sanai N, Chi JH, Dowd CF, Chin C, Tihan T. Comprehensive management of symptomatic and aggressive vertebral hemangiomas. Neurosurg Clin N Am 2008;19:17–29.
Murugan L, Samson RS, Chandy MJ. Management of symptomatic vertebral hemangiomas: review of 13 patients. Neurol India 2002;50:301–305.
Rudnick J, Stern M. Symptomatic thoracic vertebral hemangioma: a case report and literature review. Arch Phys Med Rehabil 2004;85:1544–1547.
Kawahara N, Tomita K, Murakami H, Demura S. Total en bloc spondylectomy for spinal tumors: surgical techniques and related basic background. Orthop Clin North Am 2009;40:47–63.
Lee S, Hadlow AT. Extraosseous extension of vertebral hemangioma, a rare cause of spinal cord compression. Spine 1999;24:2111–114.
Ng VW, Clifton A, Moore AJ. Preoperative endovascular embolization of a vertebral haemangioma. J Bone Joint Surg Br 1997;79:808–811.
Shah KC, Chacho AG. Extensive vertebral haemangioma with cord compression in two patients: review of the literature. Br J Neurosurg 2004;18:250–252.
Gellad FE, Sadato N, Numaguchi Y, Levine AM. Vascular metastatic lesion of the spine: preoperative embolization. Radiology 1990;176:683–686.
Roscoe MW, McBroom RJ, Louis EST, Grossman H, Perrin R. Preoperative embolization in the treatment of osseous metastases from renal cell carcinoma. Clin Orthop 1989;238:302–307.
Baloch KG, Grimer RJ, Carter SR, Tillman RM. Radical surgery for the solitary bony metastasis from renal-cell carcinoma. J Bone Joint Surg Br 2000;82:62–67.
Author information
Authors and Affiliations
About this article
Cite this article
Kato, S., Kawahara, N., Murakami, H. et al. Surgical management of aggressive vertebral hemangiomas causing spinal cord compression: long-term clinical follow-up of five cases. J Orthop Sci 15, 350–356 (2010). https://doi.org/10.1007/s00776-010-1483-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-010-1483-z