Abstract
Vaccination is a cost-effective way to control the influenza epidemic. Vaccines based on highly conserved antigens can provide protection against different influenza A strains and subtypes. In this study, the recombinant nucleoprotein (rNP) of the A/PR/8/34 (H1N1) influenza virus strain was effectively expressed using a prokaryotic expression system and then purified with a nickel-charged Sepharose affinity column as a candidate component for an influenza vaccine. The rNP was administered intranasally three times at 3-week intervals to female BALB/c mice in combination with an adjuvant (cholera toxin B subunit containing 0.2% of the whole toxin). Twenty-one days after the last immunization, the mice were challenged with homologous or heterologous influenza viruses at a lethal dose. The results showed that intranasal immunization of 10 μg rNP with adjuvant completely protected the immunized mice against the homologous influenza virus, and immunization with 100 μg rNP in combination with adjuvant provided good cross-protection against heterologous H5N1 and H9N2 avian influenza viruses. The results indicate that such a vaccine administered intranasally can induce mucosal and cell-mediated immunity, thus having the potential to control epidemics caused by new emerging influenza viruses.
Similar content being viewed by others
Introduction
Influenza is a highly contagious and acute respiratory disease caused by infection of the host respiratory tract mucosa by influenza virus. Vaccination is the most effective way to control influenza epidemic sand pandemics. The current strategy for vaccine development focuses on inducing antibodies against the surface glycoproteins hemagglutinin (HA) and neuraminidase (NA). However, HA and NA are prone to antigenic drift, and the World Health Organization has to reformulate the vaccine strains every year. Even so, it is difficult to ensure that the vaccine strains match those that will be circulating in the next season. Highly pathogenic H5N1 avian influenza emerged in 1997, followed by several waves of infection from 2002 until now [1]. Once it breaks the species barrier and becomes capable of efficient person-to-person transmission, a very severe epidemic may occur. The new H1N1 influenza virus, which first appeared in Mexico in 2009, can be transmitted effectively from person to person and has spread rapidly across the globe. Therefore, developing a universal vaccine against influenza viruses with new pandemic potential based on an internal protein is a sensible solution. This kind of vaccine could at least reduce mortality in a new epidemic or pandemic before an antigenically matched vaccine is ready.
The highly conserved internal protein NP of influenza A virus is an attractive candidate as a component of a “universal” influenza vaccine [2]. Previous studies have revealed that NP-based DNA vaccines and viral vector vaccines are not only protective against matched challenge viruses but also partially protective against mismatched viruses [3–8]. This protective immunity is generally mediated by an NP-specific cytotoxic T lymphocyte (CTL) immune response [9]. However, the heterosubtypic immune response that offers some protection against different influenza A subtypes is limited. Attempts to enhance the protective effect have been made, including combination of NP with other conserved proteins such as M1 and NS1 [10, 11]. At the same time, several studies have confirmed that inactivated whole virus vaccines administered intranasally can induce more effective cross-protection against heterologous viruses than those administered via any other parenteral immunizing routes [12, 13]. Bright et al. [14] indicated that intranasal delivery of influenza VLPs could elicit broader immune responses than the same vaccine delivered intramuscularly, and that stronger cellular immune responses, in particular, were induced in the lung mucosa in mice vaccinated intranasally compared to those vaccinated intramuscularly. This confirmed that vaccines delivered intranasally not only effectively confer mucosal immunity in the respiratory tract, but also elicit systemic immunity. The respiratory mucosa is the first line of defense against influenza infection. Therefore, it has been of interest to develop intranasally administered vaccines for influenza. In addition, intranasal administration is easy to carry out, even by the recipient himself, without the need for needles and specially trained healthcare specialists, which may greatly extend vaccination coverage [15].
In this study, we prepared rNP expressed in E. coli and tested its efficacy in protecting intranasally immunized mice against the homologous and heterologous viruses. The most effective mucosal adjuvant, cholera toxin B (CTB) subunits containing a trace amount of the holotoxin (named CTB★) [16], was coadministered to enhance the immunogenicity of the rNP vaccine. We confirmed that the vaccine delivered intranasally could induce a broad spectrum of protective immunity against diverse influenza A viruses, including a highly pathogenic H5N1 strain of avian influenza.
Materials and methods
Viruses and mice
Influenza viruses used in this study included a mouse-adapted A/PR/8/34 (H1N1) virus, an H9N2 influenza virus A/Chicken/Jiangsu/7/2002 (H9N2), and an H5N1 influenza virus A/Chicken/Henan/12/2004(H5N1). The H9N2 and H5N1 influenza viruses were isolated by our group in 2002 and 2004, respectively. After being passaged and adapted in mice as described in our previous studies [17, 18], the viruses were frozen at −70°C until use.
Both of the H9N2 and H5N1 influenza viruses were fully sequenced, and the corresponding accession numbers of the eight segments of A/Chicken/Jiangsu/7/2002 (H9N2) in the DDBJ/ENBL/GenBank databases are as follows: FJ384756 for segment 1, FJ384757 for segment 2, FJ384758 for segment 3, FJ384759 for segment 4, FJ384744 for segment 5, FJ384745 for segment 6, FJ384746 for segment 7, FJ384747 for segment 8. The accession numbers of A/Chicken/Henan/12/2004(H5N1) are: AY950281 for segment 1, AY950274 for segment 2, AY950267 for segment 3, AY950232 for segment 4, AY950253 for segment 5, AY950246 for segment 6, AY950239 for segment 7, AY950260 for segment 8. The NP present in the H9N2 strain A/Chicken/Jiangsu/7/2002 and the H5N1 strain A/Chicken/Henan/12/2004 have gene sequence identities of 84.9 and 84.7%, respectively, with the H1N1 strain A/PR/8/34, and all three strains include the immunodominant class I epitope NP147–155 (TYQRTRALV) and class II antigen epitopes (FWRGENGRKTRSAYERMCNILKGK, RLIQNSLTIERMVLSAFDERNK, and AVKGVGTMVMELIRMIKRGINDRN).
All experiments with live H5N1 and H9N2 viruses were performed in a biosafety level 3 containment facility at the Wuhan Institute of Virology, Chinese Academy of Sciences.
Specific-pathogen-free female BALB/c mice (6–8 weeks old) were purchased from Shanghai Laboratory Animal Center, China. All mice were bred in the Animal Resource Center at the Shanghai Institute of Biological Products and maintained under specific-pathogen-free conditions. All experiments involving animals were approved by the Animal Care Committee of the Shanghai Institute of Biological Products.
Preparation of rNP and adjuvant
Plasmid pET28a/NP was constructed by cloning the PCR products of the NP gene from the A/PR/8/34 (H1N1) influenza virus strain into the plasmid expression vector pET28a. The plasmid was then used to transform Escherichia coli (E. coli) BL21 (DE3) bacteria for expression. Briefly, bacteria were grown to log phase, and protein expression was induced by adding isopropyl-β-d-thiogalactopyranoside to a final concentration of 0.1 mM. After 6 h of further incubation at 28°C, the cells were pelleted and resuspended in a suitable volume of 50 mM NaH2PO4, 300 mM NaCl, 10 mM imidazole (pH 8.0) with 1 mg/ml lysozyme and 1 mM PMSF. Lysates were rocked at 4°C for 30 min and then sonicated on ice. DNase I was added to a final concentration of 5 μg/ml, and the lysates were rocked an additional hour at 4°C. Lysates were clarified by centrifugation at 10,000×g for 30 min. The soluble recombinant NP protein was absorbed onto a nickel-charged Sepharose affinity column (Qiagen) and then eluted from the column using 250 mM imidazole. The recombinant proteins were dialyzed against PBS and sterile filtered before use.
CT and CTB were purchased from Sigma (USA). One microgram of CTB supplemented with 2 ng of CT (0.2% of CTB), designated as CTB★, was used as adjuvant [19].
SDS-PAGE and western blotting
The expressed protein was analyzed for size and purity by SDS-PAGE and western blotting. For SDS-PAGE analysis, the expressed rNP was lysed in SDS-PAGE sample loading buffer and then separated by SDS-PAGE, followed by staining with Coomassie brilliant blue R-250. For immunoblot analysis, the expressed rNP protein separated by SDS-PAGE was transferred to a polyvinylidene difluoride (PVDF) membrane (Millipore). The membrane was blocked and then incubated first with anti-His monoclonal antibody (Novagen), and subsequently with horseradish peroxidase (HRP)-conjugated secondary anti-mouse antibody (KPL). Binding signals were visualized with 3,3′,5,5′-tetramethylbenzidine (TMB) substrate.
Immunization and challenge
Female BALB/c mice were anesthetized and immunized three times (3 weeks apart) intranasally or intraperitoneally with PBS containing different doses of rNP alone or in combination with 1 μg CTB★. The CTB★-immunized group was taken as an adjuvant control, and the unimmunized group served as negative control. Three weeks after the last immunization, mice were anesthetized and challenged intranasally with 20 μl of the viral suspension containing 10 × LD50 (104 EID50) of A/PR/8/34 (H1N1), 5 × LD50 (104 EID50) of A/Chicken/Jiangsu/7/2002 (H9N2), or 5 × LD50 (102.5 EID50) of A/Chicken/Henan/12/2004 (H5N1). Survival and weight loss were monitored for 21 days.
Specimens
Three days after the challenge, five mice from each group were randomly chosen for sample collection. The mice were anaesthetized with chloroform and then bled from the heart with a syringe. The sera were collected from the blood and used for IgG Ab assays. After bleeding, the mice were incised ventrally along the median line from the xiphoid process to the point of the chin. The trachea and lungs were taken out and washed three times by injecting with a total of 2 ml of PBS containing 0.1% BSA. The bronchoalveolar wash was used for virus titration after removing cellular debris by centrifugation. The head of the mouse was removed, and the lower jaw was cut off. A syringe needle was inserted into the posterior opening of the nasopharynx, and a total of 1 ml of PBS containing 0.1% BSA was injected three times to collect the outflow as nasal wash. The nasal wash was centrifuged to remove cellular debris and used for IgA Ab assays [20].
Antibody (Ab) assays
The concentrations of IgG and IgA Abs against the NP were measured by ELISA. ELISA was performed using a series of reagents consisting of the following: first, inactivated split influenza virus PR8 vaccine prepared by the Shanghai Institute of Biological Products; second, serial twofold dilutions of sera or nasal wash from each group of immunized or control mice; third, goat anti-mouse IgG Ab (γ-chain specific) (KPL) or goat anti-mouse IgA (α-chain specific) (KPL) conjugated with horseradish peroxidase (HRP); and finally, the substrate TMB. The optical density was read at 450 nm. Ab-positive cutoff values were set as means + 2 × SD of preimmune sera. An ELISA Ab titer was expressed as the highest serum dilution giving a positive reaction [21].
Passive serum transfer
Naive mice were given an intraperitoneal injection of pooled serum, 1 ml per mouse, from mice that had been immunized three times (3 weeks apart) with 100 μg rNP in combination with CTB★ or from unimmunized control mice. Mice were challenged with a lethal dose of A/PR/8/34 virus within 24 h after serum transfer.
Gamma interferon (IFN-γ) ELISPOT assay
Spleen cells were isolated from mice for IFN-γ ELISPOT assays 2 weeks after the last immunization, as described in our previous study [22]. The cell suspensions were stimulated in the presence of 2 μg/ml NP peptide stimulants. The H-2d-restricted NP class I peptide (TYQRTRALV) and a pool of three H-2d-restricted class II peptides (FWRGENGRKTRSAYERMCNILKGK, RLIQNSLTIERMVLSAFDERNK, and AVKGVGTMVMELIRMIKRGINDRN) were used as stimulants [23, 24]. Spots were counted with an ELISpot reader system (Bioreader 4000; Bio-sys, Germany). The number of peptide-reactive cells was represented as spot-forming cells (SFCs) per 106 splenocytes and was calculated by subtracting spot numbers in medium-only wells from spot numbers in peptide-containing wells.
Virus titration
The bronchoalveolar wash was serially diluted tenfold, starting from a dilution of 1:10, inoculated onto Madin Darby canine kidney (MDCK) cells, incubated at 37°C and examined for cytopathic effect 2 days later. The virus titer of each specimen, expressed as the 50% tissue culture infection dose (TCID50), was calculated by the Reed–Muench method. The virus titer in each experimental group was represented by the mean ± SD of the virus titer per ml of specimens from five mice in each group [25, 26].
Statistics
The results of test groups were evaluated by Student’s t test; if the P value was less than 0.05, the difference was considered significant. The survival rates of the mice in the test and control groups were compared by using Fisher’s exact test.
Results
Expression, purification, and characterization of rNP protein
To evaluate the efficacy of rNP protein as a potential vaccine candidate, the NP gene of influenza A/PR/8/34 (PR8) was cloned into the pET28a plasmid for expression in E. coli BL21 (DE3) bacteria. The soluble 6× His-tagged rNP protein was affinity-purified using a QIAGEN purification kit (Ni–NTA Agarose). This protein ran as a single band on a reducing SDS-PAGE gel (Fig. 1a), and as much as 30 mg highly purified protein could be obtained per liter of culture. The purified rNP was further confirmed by western blotting analysis with anti-His monoclonal antibody (Fig. 1b).
Protection of mice by intranasal administration of rNP against a lethal influenza H1N1 virus challenge
One hundred thirty-five BALB/c mice were divided randomly into nine groups of 15 mice each (Groups A–I, Table 1). The mice in Group A were immunized intraperitoneally, and the mice in Groups B–H were immunized intranasally. Group I was the unimmunized control. The intranasally immunized mice received 10, 30, 100 μg rNP alone (Group G, Group E and Group C, respectively) or in combination with 1 μg of CTB★ (Group F, Group D and Group B, respectively). The mice immunized with CTB★ alone served as the adjuvant control (Group H). All seven groups (Group B–H) were immunized three times intranasally at an interval of 3 weeks with 20 μl PBS containing different amounts of rNP with or without CTB★. For intraperitoneal immunization, each mouse was injected with 200 μl PBS containing 100 μg rNP in combination with 1 μg CTB★, and the regimen was the same as for the intranasal immunization described above. Twenty-one days after the last immunization, all of the mice were challenged with an A/PR/8/34 (H1N1) virus suspension at a lethal dose of 10 × LD50, and bronchoalveolar washes were collected 3 days postinfection from five mice of each group for titration of lung virus, as described in "Materials and methods". The remaining 10 mice in each group were observed for 21 days to evaluate the potential of the vaccine to protect mice against the homologous virus infection, by monitoring survival rate and weight loss.
The results showed that the protection provided by rNP vaccine against the homologous virus depended on the administered dosage and the adjuvant. As shown in Fig. 2a, the survival rates of the mice immunized with rNP alone at dosages of 10 μg (Group G), 30 μg (Group E) and 100 μg (Group C) against virus challenge were 10% (1/10), 30% (3/10) and 40% (4/10), respectively, and the survival rates with the same dosage of rNP in combination with adjuvant were all 100% (10/10). The mice immunized intraperitoneally with 100 μg rNP in combination with adjuvant and the mice in two control groups all succumbed to the challenge, and none survived. The survival data of Groups C, E, and G demonstrated that a stronger protective effect was achieved by the higher immunizing dose. At the same time, the survival rate of the mice immunized with 10 μg rNP in combination with the adjuvant CTB★ (Group F) was higher than that of the mice immunized with 100 μg rNP alone (Group C), which suggested that CTB★ effectively enhanced protective immunity induced by rNP. Although the mice could not be protected from death by intraperitoneal immunization with rNP, several of them survived to the tenth day after challenge. This indicates that the immunization was able to delay death slightly, as the mice in the unimmunized group all died within 8 days post-challenge.
Protection of mice against lethal challenge with homologous virus. One hundred thirty-five BALB/c mice were randomly divided into nine groups. Six groups of mice were immunized intranasally with various doses of rNP alone or in combination with CTB★. The CTB★-immunized group and the unimmunized group served as adjuvant control and negative control, respectively. Another group was immunized intraperitoneally with rNP vaccine in combination with CTB★. Three weeks after the last immunization, mice were challenged with a lethal dose (10 × LD50) of influenza PR8 virus. Survival (a) and weight loss (b) were monitored for 21 days
Immediately after viral infection, a marked body weight reduction was observed in all groups. As shown in Fig. 2b, weight reduction was dramatic in both the control group and the intraperitoneal immunization group, but it was less dramatic in the intranasal-rNP-immunized groups. Group B (100 μg rNP + CTB★) had the lowest weight loss. Body weight reduction in both Group B and Group D (30 μg rNP + CTB★) was slower and body weight started to increase 7 days after virus challenge, while the remaining groups (Groups C, E, F, G) began to recover their body weight 9 days after challenge.
Three days after challenge, the residual lung virus titers of all of the mice that were immunized intranasally with rNP were significantly lower than those of mice in the unimmunized control group (P < 0.05), as shown in Table 1. In the intranasally immunized groups, the lung viral titers declined with increased rNP dose, regardless of the absence or presence of adjuvant. Moreover, virus titers of the mice immunized with rNP plus adjuvant were lower than those of the mice immunized with the same dosage of rNP alone.
All of these results suggest that rNP, as a candidate vaccine, is capable of protecting mice against homologous influenza virus challenge and that the adjuvant CTB★ can significantly enhance the protective effect of the rNP vaccine.
Antibody responses in mice immunized with rNP
Mice in Groups A–I were immunized according to procedures described above. Three days after the challenge, five mice in each group were sacrificed to obtain the sera and nasal washes for detection of specific IgG and IgA Abs, respectively, by ELISA.
As shown in Table 2, except for the group receiving adjuvant alone and the unimmunized group, the serum IgG titers of all of the mice immunized with rNP were very high, with little difference between them. Group A, which was immunized intraperitoneally, also had a high IgG antibody level, comparable to the group that was immunized mucosally with a similar dosage. However, the IgG level did not correlate with the protection (Table 1), indicating that the high level of IgG in the serum did not play a major role in protecting mice against challenge.
IgA Ab was detected in nasal washes of mice of all groups (Groups B–G) that were immunized intranasally with rNP. The IgA titer increased with increasing dosage of rNP. The adjuvanted groups had generally higher IgA titers than the corresponding non-adjuvanted groups. Even Group F (10 μg rNP + CTB★) had higher IgA level than Group C (100 μg rNP). The three adjuvanted groups all achieved a high level of IgA antibody, with no significant difference between them. IgA antibody specific for NP was undetected in the nasal washes of the mice immunized intraperitoneally as well as of the adjuvant-immunized mice and the unimmunized mice.
These data indicate that intranasal immunization of mice with rNP can effectively induce not only systemic immunity, but also mucosal immunity, producing a high level of mucosal IgA.
Passive immunization
To test the role of the serum antibodies specific to NP, we used a passive immunization approach. Serum specimens of the mice receiving 100 μg rNP plus CTB★ three times intranasally with at an interval of 3 weeks (named rNP + CTB★), which had the best protective effect, were collected 3 weeks after the last immunization. Serum specimens from mice in the unimmunized control group (named control) were also collected. The specimens were transferred to naive mice (named P rNP + CTB★ or P control), and the mice were challenged within 24 h. Mice in both the P rNP + CTB★ group and the P control group died within 10 days, and their body weight decreased rapidly (Fig. 3). This revealed that the passively transferred serum antibody was unable to protect mice against virus infection, which was consistent with the above results. Tables 1 and 2 showed that Group A, which had been immunized intraperitoneally three times with 100 μg rNP plus adjuvant CTB★, also produced high level of antibody in the serum but failed to cope with the virus challenge. In summary, a high level of anti-NP antibody in serum is not a major factor in the protection of mice against influenza virus challenge.
Protection of mice against lethal challenge with homologous virus after pretreatment with anti-NP serum. Serum collected from mice immunized with rNP together with CTB★ (designated as rNP + CTB★ group) or from unimmunized mice (designated as control group) was passively transferred intraperitoneally to naive BALB/c mice (10 per group). The recipients (designated as P rNP + CTB★ group or P control group) were challenged with 10 × LD50 of A/PR/8/34 and monitored for survival (a) and weight loss (b)
Cell-mediated immunity
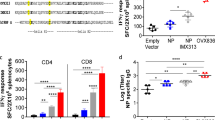
Cellular immune responses were assessed by measuring IFN-γ secretion in mouse splenocytes. BALB/c mice were randomly divided into three groups (at least three mice per group). Two of the groups were immunized with 100 μg rNP and adjuvanted rNP, respectively, as described above. The remaining group was an unimmunized control. Spleen cells were isolated from mice for IFN-γ ELISPOT assays at 2 weeks after the last immunization. The NP has been shown to be highly conserved, especially its T-cell epitopes that are recognized by C57BL/6 H-2b or BALB/c H-2d mice. These epitopes are completely conserved or differ only by individual amino acids but are still recognized by the same T cells [27]. We used the H-2d-restricted NP class I peptide (TYQRTRALV) recognized by CD8+ T cells and a pool of three H-2d-restricted class II peptides (FWRGENGRKTRSAYERMCNILKGK, RLIQNSLTIERMVLSAFDERNK, and AVKGVGTMVMELIRMIKRGINDRN) recognized by CD4+ T cells as stimuli for detection of peptide-specific IFN-γ-secreting T cells.
As indicated in Fig. 4, compared with the unimmunized control group, a significant number of NP-specific IFN-γ-secreting splenocytes were detected in both immunized groups. Mice immunized intranasally with adjuvanted rNP induced more NP-specific IFN-γ-secreting splenocytes, including CD4+ and CD8+ T cells, than the mice immunized with rNP alone, and the difference between their CD8+ T cell responses was significant (P < 0.05). Only a few non-specific spots were detected in the control group (less than 10 spots/106), and the number of positive non-specific spots (concanavalin-stimulated) was up to 2,000/106 cells (data not shown).
Detection of IFN-γ secreted by CD4+ or CD8+ T cells. Mice were immunized intranasally three times at 3-week intervals with 100 μg rNP alone or in combination with CTB★. Two weeks after the last immunization, splenocytes were harvested and stimulated with peptides recognized by CD4+ or CD8+ T cells. *Significant difference (P < 0.05)
These results indicate that rNP delivered by mucosal routes can effectively induce cell-mediated immunity with strong NP-specific CD4+ and CD8+ T cell responses. In addition, the combined use of the adjuvant can induce more IFN-γ-secreting T cells, and specific CD8+ T cells in particular.
Protection of mice by intranasal administration of rNP with CTB★ against lethal challenge with heterologous influenza viruses
To test the cross-protective immunity provided by rNP plus CTB★, two challenge experiments using either A/Chicken/Henan/12/2004 (H5N1) or A/Chicken/Jiangsu/7/2002 (H9N2) avian influenza strains were carried out. Sixty BALB/c mice were randomly divided into four groups. Two groups of mice were immunized with 100 μg rNP in combination with CTB★ as described above, and the remaining two groups served as unimmunized controls. Three weeks after the last immunization, all of the mice were challenged intranasally with 5 × LD50 of the appropriate avian influenza virus. Compared to the unimmunized control mice, the survival rates of mice in the immunized group increased dramatically, 100% (10/10) for H5N1 and 90% (9/10) for H9N2, respectively (Fig. 5a).
Protection of mice against lethal challenge with heterologous virus. Sixty BALB/c mice were randomly divided into four groups. Two groups of mice were immunized three times with 100 μg rNP plus CTB★ at an interval of 3 weeks. The remaining two groups were unimmunized controls. Three weeks after the last immunization, mice were challenged with a lethal dose (5 × LD50) of A/Chicken/Jiangsu/7/2002 (H9N2) or A/Chicken/Henan/12/2004 (H5N1). Survival (a) and weight loss (b) were monitored for 21 days
Three days after challenge, the residual lung virus titers of the immunized mice were lower than those of the corresponding unimmunized mice (Table 3). Weight loss was observed 21 days after challenge, as shown in Fig. 5b. Although mice in all groups experienced a reduction in body weight, mice in the immunized groups lost body weight more slowly. These results indicate that the highly conserved internal protein NP is not only able to protect mice against homologous virus but also confers cross-protection against heterosubtypic virus, confirming its potential for use as a component of a universal influenza vaccine.
Discussion
New influenza vaccination strategies are urgently needed, due to uncertainties about drift and shift in viral strains. NP is an important internal protein of influenza virus. Several attempts have been made to develop a vaccine with NP to confer broad protection. However, some NP-based vaccines delivered using recombinant vaccinia virus [6, 28], fowlpox virus [29], vesicular stomatitis virus [30], adenovirus vector [7, 8, 31] and DNA plasmid [3–5, 32] have not been found to provide adequate protection. Viral vectors are easy to manipulate genetically and easy to produce in large-scale operations. However, some of them have the potential to cause pathogenicity in humans. A major problem is that many people have been exposed to these viral strains. Pre-existing immunity would therefore interfere with the induction of an immune response to a foreign protein expressed from the virus. Tamura et al. [19] showed that intranasal immunization of mice with rNP from A/PR/8/34 expressed in insect cells could accelerate the clearing of the homologous virus in the nasal site of the mice, promoting recovery from infection. In this study, we successfully constructed a prokaryotic expression vector for the NP gene of A/PR/8/34 (H1N1) influenza virus and obtained the rNP from the E. coli BL21 (DE3). The efficacy of the rNP to elicit protective immunity against diverse influenza A viruses was evaluated in a mouse model.
The results showed that intranasal immunization with 10 μg rNP plus CTB★ 3 times at an interval of 3 weeks could completely protect mice against lethal homologous virus challenge. Compared to mice in the unimmunized control, the mice that were immunized intranasally with rNP could accelerate clearance of virus in the respiratory tract. However, intraperitoneal immunization could not confer effective protection against challenge. Intranasal immunization was more effective than immunization by the parenteral route for clearing the virus, which might be due to the fact that recruitment of immune lymphocytes to the infection site in mice immunized intranasally occurred more quickly than in mice immunized parenterally [33]. At the same time, intranasal immunization could induce a high level of local IgA Ab, which was critical for mucosal immunity. Our study confirmed that the survival rate of mice was associated with the level of anti-NP IgA. Protection might be provided by secretory IgA, which could neutralize virus infectivity during transcytosis in the infected epithelial cells. It is possible that IgA antibodies inhibit intracellular replication or assembly of the virus by interfering with a function of the newly synthesized viral protein NP [34–39]. Previous research has shown that serum antibodies to NP do not contribute to protective immunity because these antibodies do not have neutralizing activity [40, 41], and this was confirmed by our study. Although some studies have revealed that non-neutralizing antibodies against NP might play a role in fighting against virus challenge at a sublethal dose [42, 43], the mice that had undergone passive immunization in our present study did not survive challenge with a lethal dose of homologous influenza virus, indicating that rNP-induced humoral immunity was not a major factor in conferring protection.
Several research groups have confirmed that all NP-based vaccines, including those inducing cell-mediated immunity, are capable of providing partial cross-protection against influenza A heterosubtypic challenge [3–8]. In this study, cellular immune responses were assessed by measuring IFN-γ secretion in splenocytes, using the reported epitopes of NP recognized by CD4+ or CD8+ T cells as stimuli [23, 24]. All mice immunized intranasally with 100 μg rNP alone or in combination with adjuvant were able to induce specific IFN-γ-secreting CD4+ and CD8+ T cells, but the mice in the unimmunized control group could not. The number of IFN-γ-secreting cells in mice immunized with 100 μg rNP plus CTB★ was more than that in mice with 100 μg rNP alone, and the difference in IFN-γ-secreting CD8+ T cells between the two groups, which might be related to the survival rate, was significant (P < 0.05) (Fig. 4). These data indicate that cell-mediated immunity, particularly the specific CD8+ T cells, may have played an important role in protection of mice against the virus. In summary, the coadministration of CTB★ and rNP can induce stronger mucosal immunity and cell-mediated immunity, significantly enhancing the efficacy of the rNP-based vaccine.
The highly pathogenic avian influenza H5N1 virus emerged in 1997 and has caused human illness and death, indicating the possibility of a new pandemic due to the lack of pre-existing immunity in humans. In this study, we showed that intranasal immunization of mice with 100 μg rNP in combination with CTB★ could effectively provide cross-protection against challenge with H5N1 and H9N2 virus strains, reaching a protective rate of 100 and 90%, respectively. It may be cell-mediated immunity or the high level of IgA Ab located in the respiratory tract mucosa induced by the highly conserved NP that contributes to heterosubtypic protection. Since the NP is highly conserved among all influenza A viruses, this vaccine might provide protection against all influenza A viruses, such as the pandemic (H1N1) 2009 influenza virus, which has NP gene sequence identity of 85.8% with the H1N1 A/PR/8/34.
Our initial investigation of this rNP-based vaccine in the mouse model is intended as a proof-of-concept study, not as a final choice of vaccine. BALB/c mice have no functional Mx system to mediate innate resistance to some RNA viruses, so influenza virus infection is highly lethal to mice, unlike most human influenza virus infections [44, 45]. In this study, we used the mouse model to test the efficacy of the vaccine to some degree, and in the future, we will use a better animal model system such as non-human primates, which more closely model influenza virus infection in humans, before we proceed to clinical research.
Our study has confirmed the feasibility of using NP as a candidate for developing a universal vaccine. It would also be interesting to determine whether this protection can be improved by adding other protein components of influenza virus, such as M1 and M2e, which are also known to be less susceptible to sequence drift. The NP-based subunit vaccine would be low-cost due to the high yield of production in bacteria in fermentors, and additionally, it does not require annual updating and manufacturing. A vaccine based on NP may be a good choice for reducing the number of deaths and the severity of disease during influenza epidemics and pandemics while strain-matched vaccines are being prepared.
References
Horimoto T, Kawaoka Y (2005) Influenza: lessons from past pandemics, warnings from current incidents. Nat Rev Microbiol 3:591–600
Kaiser J (2006) A one-size-fits-all flu vaccine? Science 312:380–382
Luo M, Tao P, Li J et al (2008) Immunization with plasmid DNA encoding influenza A virus nucleoprotein fused to a tissue plasminogen activator signal sequence elicits strong immune responses and protection against H5N1 challenge in mice. J Virol Methods 154:121–127
Epstein SL, Tumpey TM, Misplon JA et al (2002) DNA vaccine expressing conserved influenza virus proteins protective against H5N1 challenge infection in mice. Emerg Infect Dis 8:796–801
Ulmer JB, Donnelly JJ, Parker SE et al (1993) Heterologous protection against influenza by injection of DNA encoding a viral protein. Science 259:1745–1749
Altstein AD, Gitelman AK, Smirnov YA et al (2006) Immunization with influenza A NP-expressing vaccinia virus recombinant protects mice against experimental infection with human and avian influenza viruses. Arch Virol 151:921–931
Epstein SL, Kong WP, Misplon JA et al (2005) Protection against multiple influenza A subtypes by vaccination with highly conserved nucleoprotein. Vaccine 23:5404–5410
Roy S, Kobinger GP, Lin J et al (2007) Partial protection against H5N1 influenza in mice with a single dose of a chimpanzee adenovirus vector expressing nucleoprotein. Vaccine 25:6845–6851
Thomas PG, Keating R, Hulse-Post DJ et al (2006) Cell-mediated protection in influenza infection. Emerg Infect Dis 12:48–54
Adar Y, Singer Y, Levi P et al (2009) A universal epitope-based influenza vaccine and its efficacy against H5N1. Vaccine 27:2099–2107
Zhirnov OP, Isaeva EI, Konakova TE et al (2007) Protection against mouse and avian influenza A strains via vaccination with a combination of conserved proteins NP, M1 and NS1. Influenza Other Respi Viruses 1:71–79
Tumpey TM, Renshaw M, Clements JD et al (2001) Mucosal delivery of inactivated influenza vaccine induces B-cell-dependent heterosubtypic cross-Protection against lethal influenza A H5N1 virus infection. J Virol 75:5141–5150
Takada A, Matsushita S, Ninomiya A et al (2003) Intranasal immunization with formalin-inactivated virus vaccine induces a broad spectrum of heterosubtypic immunity against influenza A virus infection in mice. Vaccine 21:3212–3218
Bright RA, Carter DM, Crevar CJ et al (2008) Cross-clade protective immune responses to influenza viruses with H5N1 HA and NA elicited by an influenza virus-like particle. PLoS ONE 3:1501–1512
Freytag LC, Clements JD (2005) Mucosal adjuvants. Vaccine 23:1804–1813
Tamura S-I, Yamanaka A, Shimohara M et al (1994) Synergistic action of cholera toxin B subunit (and Escherichia coli heat-labile toxin B subunit) and a trace amount of cholera whole toxin as an adjuvant for nasal influenza vaccine. Vaccine 12:419–426
Qiu M, Fang F, Chen Y et al (2006) Protection against avian influenza H9N2 virus challenge by immunization with hemagglutinin- or neuraminidase-expressing DNA in BALB/c mice. Biochem Biophys Res Commun 343:1124–1131
Zheng L, Wang F, Yang Z et al (2009) A single immunization with HA DNA vaccine by electroporation induces early protection against H5N1 avian influenza virus challenge in mice. BMC Infect Dis 9:17
Tamura S-I, Miyata K, Matwo K et al (1996) Acceleration of influenza virus clearance by Thl cells in the nasal site of mice immunized intranasally with adjuvant-combined recombinant nucleoprotein. J Immunol 156:3892–3900
Chen Z, Sahashi Y, Matsuo K et al (1998) Comparison of the ability of viral protein-expressing plasmid DNAs to protect against influenza. Vaccine 16:1544–1549
Zhu Q, Chang H, Chen Y et al (2005) Protection of inactivated influenza virus vaccine against lethal influenza virus infection in diabetic mice. Biochem Biophys Res Commun 329:87–94
Chen Q, Kuang H, Wang H et al (2009) Comparing the ability of a series of viral protein-expressing plasmid DNAs to protect against H5N1 influenza virus. Virus Genes 38:30–38
Deng YJ, Yewdell W, Eisenlohr LC et al (1997) MHC affinity, peptide liberation, T cell repertoire, and immunodominance all contribute to the paucity of MHC class I-restricted peptides recognized by antiviral CTL. J Immunol 158:1507–1515
Gao XM, Liew FY, Tite JP (1989) Identification and characterization of T helper epitopes in the nucleoprotein of influenza A virus. J Immunol 143:3007–3014
Chen J, Zhang F, Fang F et al (2007) Vaccination with hemagglutinin or neuraminidase DNA protects BALB/c mice against influenza virus infection in presence of maternal antibody. BMC Infect Dis 7:118
Zhang F, Chen J, Fang F et al (2005) Maternal immunization with both hemagglutinin- and neuraminidase-expressing DNAs provides an enhanced protection against a lethal influenza virus challenge in infant and adult mice. DNA Cell Biol 24:758–765
Powell TJ, Strutt T, Reome J et al (2007) Priming with cold-adapted influenza A does not prevent infection but elicits long-lived protection against supralethal challenge with heterosubtypic virus. J Immunol 178:1030–1038
Andrew ME, Coupar BE, Boyle DB et al (1987) The roles of influenza virus haemagglutinin and nucleoprotein in protection: analysis using vaccinia virus recombinants. Scand J Immunol 25:21–28
Webster RG, Kawaoka Y, Taylor J et al (1991) Efficacy of nucleoprotein and haemagglutinin antigens expressed in fowlpox virus as vaccine for influenza in chickens. Vaccine 9:303–308
Barefoot BE, Sample CJ, Ramsburg EA (2009) Recombinant vesicular stomatitis virus expressing influenza nucleoprotein induces CD8 T-cell responses that enhance antibody-mediated protection after lethal challenge with influenza virus. Clin Vaccine Immunol 16:488–498
Wesley RD, Tang M, Lager KM (2004) Protection of weaned pigs by vaccination with human adenovirus 5 recombinant viruses expressing the hemagglutinin and the nucleoprotein of H3N2 swine influenza virus. Vaccine 22:3427–3434
Macklin MD, McCabe D, McGregor MW et al (1998) Immunization of pigs with a particle-mediated DNA vaccine to influenza A virus protects against challenge with homologous virus. J Virol 72:1491–1496
Tite JP, Hughes-Jenkins C, O’Callaghan D et al (1990) Antiviral immunity induced by recombinant nucleoprotein of influenza A virus II Protection from influenza infection and mechanism of protection. Immunology 71:202–207
Mazanec MB, Kaetzel CS, Lamm ME et al (1992) Intracellular neutralization of virus by immunoglobulin A antibodies. Proc Natl Acad Sci 89:6901–6905
Mazanec MB, Coudret CL, Fletcher DR (1995) Intracellular neutralization of influenza virus by immunoglobulin A anti-hemagglutinin monoclonal antibodies. J Virol 69:1339–1343
Yan H, Lamm ME, Bjorling E et al (2002) Multiple functions of immunoglobulin A in mucosal defense against viruses: an in vitro measles virus model. J Virol 76:10972–10979
Huang YT, Wright A, Gao X et al (2005) Intraepithelial cell neutralization of HIV-1 replication by IgA. J Immunol 174:4828–4835
Corthesy B, Benureau Y, Perrier C et al (2006) Rotavirus anti-VP6 secretory immunoglobulin A contributes to protection via intracellular neutralization but not via immune exclusion. J Virol 80:10692–10699
Wright A, Yan H, Lamm ME et al (2006) Immunoglobulin A antibodies against internal HIV-1 proteins neutralize HIV-1 replication inside epithelial cells. Virology 356:165–170
Epstein SL, Lo CY, Misplon JA et al (1998) Mechanism of protective immunity against influenza virus infection in mice without antibodies. J Immunol 160:322–327
Epstein SL, Lo CY, Misplon JA et al (1997) Mechanisms of heterosubtypic immunity to lethal influenza A virus infection in fully immunocompetent, T cell-depleted, β2-microglobulin-deficient, and J chain-deficient mice. J Immunol 158:1222–1230
Zheng B, Zhang Y, He H et al (2007) Rectification of age-associated deficiency in cytotoxic T cell response to influenza a virus by immunization with immune complexes. J Immunol 179:6153–6159
Carragher DM, Kaminski DA, Moquin A et al (2008) A novel role for non-neutralizing antibodies against nucleoprotein in facilitating resistance to influenza virus. J Immunol 181:4168–4176
Haller O, Staeheli P, Kochs G (2007) Interferon-induced Mx proteins in antiviral host defense. Biochimie 89:812–818
Tumpey TM, Szretter KJ, Van Hoeven N et al (2007) The Mx1 gene protects mice against the pandemic 1918 and highly lethal human H5N1 influenza viruses. J Virol 81:10818–10821
Acknowledgments
This study was supported by the following research funds: National 973 Project (2010CB530301); National Natural Science Foundation of China (30972623); National Key Technology R&D Program of China (2006BAD06A03); Science and Technology Commission of Shanghai Municipality (09DZ1908600; 10XD1422200); Chinese Academy of Sciences (KSCX1-YW-R-14).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guo, L., Zheng, M., Ding, Y. et al. Protection against multiple influenza A virus subtypes by intranasal administration of recombinant nucleoprotein. Arch Virol 155, 1765–1775 (2010). https://doi.org/10.1007/s00705-010-0756-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00705-010-0756-3