Abstract
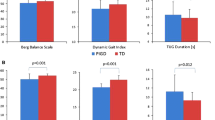
Patients with early Parkinson’s disease (PD) may not complain of gait difficulties but subtle gait abnormalities may be revealed as part of a “preclinical gait syndrome” when they are challenged by dual tasks. 21 early PD patients (n = 21, mean age 63.5 years, H&Y 1.62, disease duration <5 years, mean UPDRS-III 7.7) who did not have gait complaints were as compared to age- and gender-matched healthy controls (n = 21). Memory function was not different between the two groups. Under normal walking conditions, there were no significant differences in gait parameters between the patients and the control group. In both groups, normalized gait velocity decreased in response to dual tasking in a parallel fashion (p < 0.001). Similarly, gait variability increased in both groups with dual tasking although not statistically significant. In PD patients, the performance of an additional task resulted in an increased number of cadences (p = 0.04), a reduction in swing time (p = 0.02) and cycle time (p = 0.04) compared with the control group but there was no significant reduction in normalized velocity. Stride width also increased in the PD patients. The addition of a cognitive task may affect certain aspects of gait and is able to elicit subclinical deficits in early PD patients. In an attempt to maintain velocity, early PD patients develop compensatory mechanisms by increasing cadence and decreasing swing time and cycle time. Increased step width helps support balance, and prevents going beyond the base-of-support which may predispose to unsteadiness and falls. We propose that these findings occur as part of a spectrum of a “preclinical gait syndrome” and longitudinal studies are needed to assess the predictive values of these early markers of gait deficits.



Similar content being viewed by others
References
Baltadjieva R, Giladi N, Gruendlinger L, Peretz C, Hausdorff JM (2006) Marked alterations in the gait timing and rhythmicity of patients with de novo Parkinson’s disease. Eur J Neurosci 24(6):1815–1820
Bhidayasiri R, Truong DD (2012) Therapeutic strategies for nonmotor symptoms in early Parkinson’s disease: the case for a higher priority and stronger evidence. Parkinsonism Relat Disord 18(Suppl 1):S110–S113
Bloem BR, Grimbergen YA, van Dijk JG, Munneke M (2006) The “posture second” strategy: a review of wrong priorities in Parkinson’s disease. J Neurol Sci 248(1–2):196–204
Carpinella I, Crenna P, Calabrese E, Rabuffetti M, Mazzoleni P, Nemni R et al (2007) Locomotor function in the early stage of Parkinson’s disease. IEEE Trans Neural Syst Rehabil Eng 15(4):543–551
Chastan N, Debono B, Maltete D, Weber J (2008) Discordance between measured postural instability and absence of clinical symptoms in Parkinson’s disease patients in the early stages of the disease. Mov Disord 23(3):366–372
Chee R, Murphy A, Danoudis M, Georgiou-Karistianis N, Iansek R (2009) Gait freezing in Parkinson’s disease and the stride length sequence effect interaction. Brain 132(Pt 8):2151–2160
Donner A, Eliasziw M (1987) Sample size requirements for reliability studies. Stat Med 6(4):441–448
Evans JR, Mason SL, Williams-Gray CH, Foltynie T, Brayne C, Robbins TW et al (2011) The natural history of treated Parkinson’s disease in an incident, community based cohort. J Neurol Neurosurg Psychiatry 82(10):1112–1118
Fearnley JM, Lees AJ (1991) Ageing and Parkinson’s disease: substantia nigra regional selectivity. Brain 114(Pt 5):2283–2301
Ferrarin M, Carpinella I, Rabuffetti M, Calabrese E, Mazzoleni P, Nemni R (2006) Locomotor disorders in patients at early stages of Parkinson’s disease: a quantitative analysis. Conf Proc IEEE Eng Med Biol Soc 1:1224–1227
Fioretti S, Guidi M, Ladislao L, Ghetti G (2004) Analysis and reliability of posturographic parameters in Parkinson patients at an early stage. Conf Proc IEEE Eng Med Biol Soc 1:651–654
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12(3):189–198
Frenkel-Toledo S, Giladi N, Peretz C, Herman T, Gruendlinger L, Hausdorff JM (2005) Effect of gait speed on gait rhythmicity in Parkinson’s disease: variability of stride time and swing time respond differently. J Neuroeng Rehabil 2:23
Ganguli M, Ratcliff G, Huff FJ, Belle S, Kancel MJ, Fischer L et al (1990) Serial sevens versus world backwards: a comparison of the two measures of attention from the MMSE. J Geriatr Psychiatry Neurol 3(4):203–207
Geurts AC, Boonstra TA, Voermans NC, Diender MG, Weerdesteyn V, Bloem BR (2011) Assessment of postural asymmetry in mild to moderate Parkinson’s disease. Gait Posture 33(1):143–145
Gibb WR, Lees AJ (1988) The relevance of the Lewy body to the pathogenesis of idiopathic Parkinson’s disease. J Neurol Neurosurg Psychiatry 51(6):745–752
Gilman S, Wenning GK, Low PA, Brooks DJ, Mathias CJ, Trojanowski JQ et al (2008) Second consensus statement on the diagnosis of multiple system atrophy. Neurology 71(9):670–676
Goetz CG, Poewe W, Rascol O, Sampaio C, Stebbins GT, Counsell C et al (2004) Movement Disorder Society Task Force report on the Hoehn and Yahr staging scale: status and recommendations. Mov Disord 19(9):1020–1028
Hausdorff JM (2005) Gait variability: methods, modeling and meaning. J Neuroeng Rehabil 2:19
Hausdorff JM (2007) Gait dynamics, fractals and falls: finding meaning in the stride-to-stride fluctuations of human walking. Hum Mov Sci 26(4):555–589
Hoehn MM, Yahr MD (1967) Parkinsonism: onset, progression and mortality. Neurology 17(5):427–442
Karzmark P (2000) Validity of the serial seven procedure. Int J Geriatr Psychiatry 15(8):677–679
Kressig RW, Beauchet O (2006) Guidelines for clinical applications of spatio-temporal gait analysis in older adults. Aging Clin Exp Res 18(2):174–176
Lang AE (2011) A critical appraisal of the premotor symptoms of Parkinson’s disease: potential usefulness in early diagnosis and design of neuroprotective trials. Mov Disord 26(5):775–783
Lee CS, Samii A, Sossi V, Ruth TJ, Schulzer M, Holden JE et al (2000) In vivo positron emission tomographic evidence for compensatory changes in presynaptic dopaminergic nerve terminals in Parkinson’s disease. Ann Neurol 47(4):493–503
Lewek MD, Poole R, Johnson J, Halawa O, Huang X (2010) Arm swing magnitude and asymmetry during gait in the early stages of Parkinson’s disease. Gait Posture 31(2):256–260
Litvan I, Agid Y, Calne D, Campbell G, Dubois B, Duvoisin RC et al (1996) Clinical research criteria for the diagnosis of progressive supranuclear palsy (Steele–Richardson–Olszewski syndrome): report of the NINDS-SPSP international workshop. Neurology 47(1):1–9
Morris ME, Iansek R, Matyas TA, Summers JJ (1994) Ability to modulate walking cadence remains intact in Parkinson’s disease. J Neurol Neurosurg Psychiatry 57(12):1532–1534
Nandhagopal R, Kuramoto L, Schulzer M, Mak E, Cragg J, McKenzie J et al (2011) Longitudinal evolution of compensatory changes in striatal dopamine processing in Parkinson’s disease. Brain 134(Pt 11):3290–3298
Nelson AJ (1974) Functional ambulation profile. Phys Ther 54(10):1059–1065
Nelson AJ, Zwick D, Brody S, Doran C, Pulver L, Rooz G et al (2002) The validity of the GaitRite and the Functional Ambulation Performance scoring system in the analysis of Parkinson gait. NeuroRehabilitation 17(3):255–262
Pickering RM, Grimbergen YA, Rigney U, Ashburn A, Mazibrada G, Wood B et al (2007) A meta-analysis of six prospective studies of falling in Parkinson’s disease. Mov Disord 22(13):1892–1900
Plotnik M, Giladi N, Hausdorff JM (2009) Bilateral coordination of gait and Parkinson’s disease: the effects of dual tasking. J Neurol Neurosurg Psychiatry 80(3):347–350
Rocchi L, Chiari L, Mancini M, Carlson-Kuhta P, Gross A, Horak FB (2006) Step initiation in Parkinson’s disease: influence of initial stance conditions. Neurosci Lett 406(1–2):128–132
Rochester L, Hetherington V, Jones D, Nieuwboer A, Willems AM, Kwakkel G et al (2004) Attending to the task: interference effects of functional tasks on walking in Parkinson’s disease and the roles of cognition, depression, fatigue, and balance. Arch Phys Med Rehabil 85(10):1578–1585
van Nuenen BF, Helmich RC, Ferraye M, Thaler A, Hendler T, Orr-Urtreger A et al (2012) Cerebral pathological and compensatory mechanisms in the premotor phase of leucine-rich repeat kinase 2 parkinsonism. Brain 135(Pt 12):3687–3698
Yang YR, Lee YY, Cheng SJ, Lin PY, Wang RY (2008) Relationships between gait and dynamic balance in early Parkinson’s disease. Gait Posture 27(4):611–615
Yogev G, Giladi N, Peretz C, Springer S, Simon ES, Hausdorff JM (2005) Dual tasking, gait rhythmicity, and Parkinson’s disease: which aspects of gait are attention demanding? Eur J Neurosci 22(5):1248–1256
Yogev-Seligmann G, Hausdorff JM, Giladi N (2008) The role of executive function and attention in gait. Mov Disord 23(3):329–342 (quiz 472)
Acknowledgments
The study was supported by the Rachadaphiseksomphot Endowment Fund Part of the “Strengthen CU’s Researcher’s Project” and research unit (RU) grant number GRU 52-026-30-005 of Chulalongkorn University, Bangkok, Thailand. We would like to thank Wannipat Buated for her assistance in patients recruitment and the data assortment.
Conflict of interest
The authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Panyakaew, P., Bhidayasiri, R. The spectrum of preclinical gait disorders in early Parkinson’s disease: subclinical gait abnormalities and compensatory mechanisms revealed with dual tasking. J Neural Transm 120, 1665–1672 (2013). https://doi.org/10.1007/s00702-013-1051-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-013-1051-8