Abstract
Study design
This is a retrospective study.
Objective
Implant nonfusion is an important prognostic factor for patients after anterior cervical discectomy and fusion (ACDF). This study aimed to investigate endplate-specific pseudarthrosis after ACDF, to determine if the rate of fusion is inferior in the lower endplate, and to identify any differences in clinical and radiological results.
Summary of background data
Research comparing each endplate on which the endplate affects nonfusion is limited.
Methods
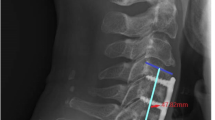
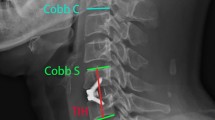
We analyzed 71 patients with 142 total spinal levels who underwent double-level ACDF (C4-5-6 and C5-6-7) with an allograft and plate at our hospital between January 2012 and December 2018. Fusion grades were assessed using computed tomography and the Bridwell fusion grade system at 1 year postoperatively. Radiological parameters were obtained from lateral cervical radiographs collected preoperatively and at 1 month and 1 year after surgery.
Results
There was no difference in fusion between the C4-5-6 and C5-6-7 ACDF procedures, but the fusion rate and Bridwell fusion grade at the caudal surgery level were lower than those at the cranial surgery level (93 vs. 79%, p < 0.001). The lower endplate of the caudal fusion level showed the most common pseudarthrosis (18 of 71 [25%]). There was no difference in radiological parameters and clinical outcomes between the fusion and pseudarthrosis groups.
Conclusion
In double-level ACDF procedures, the nonfusion rate was higher at the caudal fusion levels, especially at the lower endplates of the caudal fusion levels.





Similar content being viewed by others
References
Barsa P, Suchomel P (2007) Factors affecting sagittal malalignment due to cage subsidence in standalone cage assisted anterior cervical fusion. Eur Spine J 16(9):1395
Bridwell KH, Lenke LG, McEnery KW et al (1995) Anterior fresh frozen structural allografts in the thoracic and lumbar spine. Do they work if combined with posterior fusion and instrumentation in adult patients with kyphosis or anterior column defects? Spine (Phila Pa 1976) 20(12):1410–1418
Cannada LK, Scherping SC, Yoo JU et al (2003) Pseudoarthrosis of the cervical spine: a comparison of radiographic diagnostic measures. Spine 28(1):46–51
Crawford CH III, Carreon LY, Mummaneni P et al (2020) Asymptomatic ACDF nonunions underestimate the true prevalence of radiographic pseudarthrosis. Spine 45(13):E776–E780
Ezra D, Masharawi Y, Salame K et al (2017) Demographic aspects in cervical vertebral bodies’ size and shape (C3–C7): a skeletal study. Spine J 17(1):135–142
Fraser JF, Härtl R (2007) Anterior approaches to fusion of the cervical spine: a metaanalysis of fusion rates. J Neurosurg Spine 6(4):298–303
Goh JC, Wong H-k, Thambyah A et al (2000) Influence of PLIF cage size on lumbar spine stability. Spine 25(1):35
Jiang S-D, Jiang L-S, Dai L-Y (2012) Anterior cervical discectomy and fusion versus anterior cervical corpectomy and fusion for multilevel cervical spondylosis: a systematic review. Arch Orthop Trauma Surg 132(2):155–161
Lapsiwala S, Benzel E (2006) Surgical management of cervical myelopathy dealing with the cervical–thoracic junction. Spine J 6(6, Supplement):S268–S273
Lee D-H, Cho JH, Hwang CJ et al (2018) What is the fate of pseudarthrosis detected 1 year after anterior cervical discectomy and fusion? Spine 43(1):E23–E28
Lee NJ, Vulapalli M, Park P et al (2020) Does screw length for primary two-level ACDF influence pseudarthrosis risk? Spine J 20(11):1752–1760
Leven D, Cho SK (2016) Pseudarthrosis of the cervical spine: risk factors, diagnosis and management. Asian Spine J 10(4):776–786
Lin W, Ha A, Boddapati V et al (2018) Diagnosing pseudoarthrosis after anterior cervical discectomy and fusion. Neurospine 15(3):194–205
Marrache M, Bronheim R, Harris AB et al (2020) Synthetic cages associated with increased rates of revision surgery and higher costs compared to allograft in ACDF in the nonelderly patient. Neurospine 17(4):896–901
McAnany SJ, Baird EO, Overley SC et al (2015) A meta-analysis of the clinical and fusion results following treatment of symptomatic cervical pseudarthrosis. Global Spine J 5(2):148–155
Nichols NM, Jamieson A, Wang M et al (2020) Characterizing the fusion order and level-specific rates of arthrodesis in 3-level anterior cervical discectomy and fusion: a radiographic study. J Clin Neurosci 81:328–333
Odom GL, Finney W, Woodhall B (1958) Cervical disk lesions. J Am Med Assoc 166(1):23–28
Oshina M, Oshima Y, Tanaka S, Riew KD (2018) Radiological fusion criteria of postoperative anterior cervical discectomy and fusion: a systematic review. Global Spine J 8(7):739–750
Phillips FM, Carlson G, Emery SE et al (1997) Anterior cervical pseudarthrosis: natural history and treatment. Spine 22(14):1585–1589
Raizman NM, O’Brien JR, Poehling-Monaghan KL et al (2009) Pseudarthrosis of the spine. J Am Acad Orthop Surg 17(8):494–503
Robinson R (1955) Anterolateral disc removal and interbody fusion for cervical disc syndrome. Bull Johns Hopkins Hosp 96:223–224
Shriver MF, Lewis DJ, Kshettry VR et al (2015) Pseudoarthrosis rates in anterior cervical discectomy and fusion: a meta-analysis. Spine J 15(9):2016–2027
Wang JC, McDonough PW, Endow KK et al (2000) Increased fusion rates with cervical plating for two-level anterior cervical discectomy and fusion. Spine 25(1):41
Wang JC, McDonough PW, Kanim LE et al (2001) Increased fusion rates with cervical plating for three-level anterior cervical discectomy and fusion. Spine 26(6):643–646
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the Institutional Review Board of Gangnam Severance Hospital (IRB No. 3–2021-0008).
Consent to participate
Not required because this study was a retrospective study.
Consent for publication
Not required because this study was a retrospective study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Spine degenerative
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jang, H.J., Kim, K.H., Park, J.Y. et al. Endplate-specific fusion rate 1 year after surgery for two-level anterior cervical discectomy and fusion(ACDF). Acta Neurochir 164, 3173–3180 (2022). https://doi.org/10.1007/s00701-022-05377-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05377-6