Abstract
Background
There is wide variation in the reported size of ruptured intracranial aneurysms and methods of size estimation. There is widespread belief that small aneurysms < 7 mm do not rupture. Therefore, we performed a systematic review and meta-analysis of the literature to determine the size of ruptured aneurysms according to aneurysm locations and methods of size estimation.
Methods
We searched PubMed, Cochrane, CINAHL, and EMBASE databases using a combination of Medical Subject Headings (MeSH) terms. We included articles that reported mean aneurysm size in consecutive series of ruptured intracranial. We excluded studies limited to a specific aneurysm location or type. The random-effects model was used to calculate overall mean size and location-specific mean size. We performed meta-regression to explain observed heterogeneity and variation in reported size.
Results
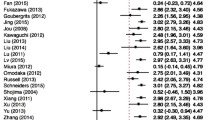
The systematic review included 36 studies and 12,609 ruptured intracranial aneurysms. Overall mean aneurysm size was 7.0 mm (95% confidence interval [CI 6.2–7.4]). Pooled mean size varied with location. Overall mean size of 2145 ruptured anterior circulation aneurysms was 6.0 mm (95% CI 5.6–6.4, residual I2 = 86%). Overall mean size of 743 ruptured posterior circulation aneurysms was 6.2 mm (95% CI 5.3–7.0, residual I2 = 93%). Meta-regression identified aneurysm location and definition of size (i.e., maximum dimension vs. aneurysm height) as significant determinants of aneurysm size reported in the studies.
Conclusions
The mean size of ruptured aneurysms in most studies was approximately 7 mm. The general wisdom that aneurysms of this size do not rupture is incorrect. Location and size definition were significant determinants of aneurysm size.




Similar content being viewed by others
References
AlMatter M, Bhogal P, Aguilar Perez M, Schob S, Hellstern V, Bazner H, Ganslandt O, Henkes H (2019) The size of ruptured intracranial aneurysms: a 10-year series from a single center. Clin Neuroradiol 29:125–133. https://doi.org/10.1007/s00062-017-0632-6
Baharoglu MI, Lauric A, Gao BL, Malek AM (2012) Identification of a dichotomy in morphological predictors of rupture status between sidewall- and bifurcation-type intracranial aneurysms. J Neurosurg 116:871–881. https://doi.org/10.3171/2011.11.JNS11311
Beck J, Rohde S, Berkefeld J, Seifert V, Raabe A (2006) Size and location of ruptured and unruptured intracranial aneurysms measured by 3-dimensional rotational angiography. Surg Neurol 65:18–25; discussion 25-17. https://doi.org/10.1016/j.surneu.2005.05.019
Bhogal P, AlMatter M, Hellstern V, Ganslandt O, Bazner H, Henkes H, Perez MA (2018) Difference in aneurysm characteristics between ruptured and unruptured aneurysms in patients with multiple intracranial aneurysms. Surg Neurol Int 9:1. https://doi.org/10.4103/sni.sni_339_17
Bijlenga P, Ebeling C, Jaegersberg M, Summers P, Rogers A, Waterworth A, Iavindrasana J, Macho J, Pereira VM, Bukovics P, Vivas E, Sturkenboom MC, Wright J, Friedrich CM, Frangi A, Byrne J, Schaller K, Rufenacht D (2013) Risk of rupture of small anterior communicating artery aneurysms is similar to posterior circulation aneurysms. Stroke 44:3018–3026. https://doi.org/10.1161/strokeaha.113.001667
Brinjikji W, Zhu YQ, Lanzino G, Cloft HJ, Murad MH, Wang Z, Kallmes DF (2016) Risk factors for growth of intracranial aneurysms: a systematic review and meta-analysis. AJNR Am J Neuroradiol 37:615–620. https://doi.org/10.3174/ajnr.A4575
Detmer FJ, Chung BJ, Jimenez C, Hamzei-Sichani F, Kallmes D, Putman C, Cebral JR (2019) Associations of hemodynamics, morphology, and patient characteristics with aneurysm rupture stratified by aneurysm location. Neuroradiology 61:275–284. https://doi.org/10.1007/s00234-018-2135-9
Dhar S, Tremmel M, Mocco J, Kim M, Yamamoto J, Siddiqui AH, Hopkins LN, Meng H (2008) Morphology parameters for intracranial aneurysm rupture risk assessment. Neurosurgery 63:185–196; discussion 196-187. https://doi.org/10.1227/01.Neu.0000316847.64140.81
Duan Z, Li Y, Guan S, Ma C, Han Y, Ren X, Wei L, Li W, Lou J, Yang Z (2018) Morphological parameters and anatomical locations associated with rupture status of small intracranial aneurysms. Sci Rep 8:6440. https://doi.org/10.1038/s41598-018-24732-1
Feng X, Zhang B, Guo E, Wang L, Qian Z, Liu P, Wen X, Xu W, Jiang C, Li Y, Wu Z, Liu A (2017) Bifurcation location and growth of aneurysm size are significantly associated with an irregular shape of unruptured intracranial aneurysms. World Neurosurg 107:255–262. https://doi.org/10.1016/j.wneu.2017.07.063
Froelich JJ, Neilson S, Peters-Wilke J, Dubey A, Thani N, Erasmus A, Carr MW, Hunn AW (2016) Size and location of ruptured intracranial aneurysms: a 5-year clinical survey. World Neurosurg 91:260–265. https://doi.org/10.1016/j.wneu.2016.04.044
Greving JP, Wermer MJ, Brown RD Jr, Morita A, Juvela S, Yonekura M, Ishibashi T, Torner JC, Nakayama T, Rinkel GJ, Algra A (2014) Development of the PHASES score for prediction of risk of rupture of intracranial aneurysms: a pooled analysis of six prospective cohort studies. Lancet Neurol 13:59–66. https://doi.org/10.1016/s1474-4422(13)70263-1
Hilditch CA, Brinjikji W, Tsang AC, Nicholson P, Kostynskyy A, Tymianski M, Krings T, Radovanovic I, Pereira VM (2018) Application of PHASES and ELAPSS scores to ruptured cerebral aneurysms: how many would have been conservatively managed? J Neurosurg Sci epub May 28. https://doi.org/10.23736/S0390-5616.18.04498-3
Ho A, Lin N, Charoenvimolphan N, Stanley M, Frerichs KU, Day AL, Du R (2014) Morphological parameters associated with ruptured posterior communicating aneurysms. PLoS One 9:e94837. https://doi.org/10.1371/journal.pone.0094837
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13. https://doi.org/10.1186/1471-2288-5-13
Huttunen T, von und zu Fraunberg M, Frosen J, Lehecka M, Tromp G, Helin K, Koivisto T, Rinne J, Ronkainen A, Hernesniemi J, Jaaskelainen JE (2010) Saccular intracranial aneurysm disease: distribution of site, size, and age suggests different etiologies for aneurysm formation and rupture in 316 familial and 1454 sporadic eastern Finnish patients. Neurosurgery 66:631–638; discussion 638. https://doi.org/10.1227/01.Neu.0000367634.89384.4b
Jagadeesan BD, Delgado Almandoz JE, Kadkhodayan Y, Derdeyn CP, Cross DT 3rd, Chicoine MR, Rich KM, Zipfel GJ, Dacey RG, Moran CJ (2014) Size and anatomic location of ruptured intracranial aneurysms in patients with single and multiple aneurysms: a retrospective study from a single center. J Neurointerv Surg 6:169–174. https://doi.org/10.1136/neurintsurg-2012-010623
Jeon HJ, Lee JW, Kim SY, Park KY, Huh SK (2014) Morphological parameters related to ruptured aneurysm in the patient with multiple cerebral aneurysms (clinical investigation). Neurol Res 36:1056–1062. https://doi.org/10.1179/1743132814y.0000000393
Jeong YG, Jung YT, Kim MS, Eun CK, Jang SH (2009) Size and location of ruptured intracranial aneurysms. J Korean Neurosurg Soc 45:11–15. https://doi.org/10.3340/jkns.2009.45.1.11
Jiang Y, Lan Q, Wang Q, Lu H, Ge F, Wang Y (2014) Correlation between the rupture risk and 3D geometric parameters of saccular intracranial aneurysms. Cell Biochem Biophys 70:1417–1420. https://doi.org/10.1007/s12013-014-0074-6
Joo SW, Lee SI, Noh SJ, Jeong YG, Kim MS, Jeong YT (2009) What is the significance of a large number of ruptured aneurysms smaller than 7 mm in diameter? J Korean Neurosurg Soc 45:85–89. https://doi.org/10.3340/jkns.2009.45.2.85
Kashiwazaki D, Kuroda S (2013) Size ratio can highly predict rupture risk in intracranial small (<5 mm) aneurysms. Stroke 44:2169–2173. https://doi.org/10.1161/strokeaha.113.001138
Kleinloog R, van 't Hof FN, Wolters FJ, Rasing I, van der Schaaf IC, Rinkel GJ, Ruigrok YM (2013) The association between genetic risk factors and the size of intracranial aneurysms at time of rupture. Neurosurgery 73:705–708. https://doi.org/10.1227/neu.0000000000000078
Korja M, Kivisaari R, Rezai Jahromi B, Lehto H (2018) Size of ruptured intracranial aneurysms is decreasing: twenty-year long consecutive series of hospitalized patients. Stroke 49:746–749. https://doi.org/10.1161/STROKEAHA.117.019235
Lauric A, Baharoglu MI, Gao BL, Malek AM (2012) Incremental contribution of size ratio as a discriminant for rupture status in cerebral aneurysms: comparison with size, height, and vessel diameter. Neurosurgery 70:944–951; discussion 951-942. https://doi.org/10.1227/NEU.0b013e31823bcda7
Lauric A, Baharoglu MI, Malek AM (2012) Ruptured status discrimination performance of aspect ratio, height/width, and bottleneck factor is highly dependent on aneurysm sizing methodology. Neurosurgery 71:38–45. https://doi.org/10.1227/NEU.0b013e3182503bf9
Lee GJ, Eom KS, Lee C, Kim DW, Kang SD (2015) Rupture of very small intracranial aneurysms: incidence and clinical characteristics. J Cerebrovasc Endovasc Neurosurg 17:217–222. https://doi.org/10.7461/jcen.2015.17.3.217
Ma D, Tremmel M, Paluch RA, Levy EI, Meng H, Mocco J (2010) Size ratio for clinical assessment of intracranial aneurysm rupture risk. Neurol Res 32:482–486. https://doi.org/10.1179/016164109x12581096796558
Meng H, Tutino VM, Xiang J, Siddiqui A (2014) High WSS or low WSS? Complex interactions of hemodynamics with intracranial aneurysm initiation, growth, and rupture: toward a unifying hypothesis. AJNR Am J Neuroradiol 35:1254–1262. https://doi.org/10.3174/ajnr.A3558
Nabaweesi-Batuka J, Kitunguu PK, Kiboi JG (2016) Pattern of cerebral aneurysms in a Kenyan population as seen at an Urban Hospital. World Neurosurg 87:255–265. https://doi.org/10.1016/j.wneu.2015.09.061
Nikolic I, Tasic G, Bogosavljevic V, Nestorovic B, Jovanovic V, Kojic Z, Djoric I, Djurovic B (2012) Predictable morphometric parameters for rupture of intracranial aneurysms - a series of 142 operated aneurysms. Turk Neurosurg 22:420–426. https://doi.org/10.5137/1019-5149.Jtn.4698-11.1
Ohashi Y, Horikoshi T, Sugita M, Yagishita T, Nukui H (2004) Size of cerebral aneurysms and related factors in patients with subarachnoid hemorrhage. Surg Neurol 61:239–245; discussion 245-237. https://doi.org/10.1016/s0090-3019(03)00427-0
Qiu T, Jin G, Bao W (2014) The interrelated effects of 2D angiographic morphological variables and aneurysm rupture. Neurosciences (Riyadh) 19:210–217
Rahman M, Smietana J, Hauck E, Hoh B, Hopkins N, Siddiqui A, Levy EI, Meng H, Mocco J (2010) Size ratio correlates with intracranial aneurysm rupture status: a prospective study. Stroke 41:916–920. https://doi.org/10.1161/strokeaha.109.574244
Rajabzadeh-Oghaz H, Varble N, Davies JM, Mowla A, Shakir HJ, Sonig A, Shallwani H, Snyder KV, Levy EI, Siddiqui AH, Meng H (2017) Computer-assisted adjuncts for aneurysmal morphologic assessment: toward more precise and accurate approaches. Proc SPIE Int Soc Opt Eng:10134. https://doi.org/10.1117/12.2255553
Roessler K, Cejna M, Zachenhofer I (2011) Aneurysmatic subarachnoidal haemorrhage: incidence and location of small ruptured cerebral aneurysms - a retrospective population-based study. Wien Klin Wochenschr 123:444–449. https://doi.org/10.1007/s00508-011-1598-z
Russell SM, Lin K, Hahn SA, Jafar JJ (2003) Smaller cerebral aneurysms producing more extensive subarachnoid hemorrhage following rupture: a radiological investigation and discussion of theoretical determinants. J Neurosurg 99:248–253. https://doi.org/10.3171/jns.2003.99.2.0248
Ujiie H, Tamano Y, Sasaki K, Hori T (2001) Is the aspect ratio a reliable index for predicting the rupture of a saccular aneurysm? Neurosurgery 48:495–502; discussion 502-493
Varble N, Kono K, Rajabzadeh-Oghaz H, Meng H (2018) Rupture resemblance models may correlate to growth rates of intracranial aneurysms: preliminary results. World Neurosurg 110:e794–e805. https://doi.org/10.1016/j.wneu.2017.11.093
Varble N, Tutino VM, Yu J, Sonig A, Siddiqui AH, Davies JM, Meng H (2018) Shared and distinct rupture discriminants of small and large intracranial aneurysms. Stroke 49:856–864. https://doi.org/10.1161/STROKEAHA.117.019929
Wang GX, Wen L, Yang L, Zhang QC, Yin JB, Duan CM, Zhang D (2018) Risk factors for the rupture of intracranial aneurysms using computed tomography angiography. World Neurosurg 110:e333–e338. https://doi.org/10.1016/j.wneu.2017.10.174
Wang GX, Zhang D, Wang ZP, Yang LQ, Yang H, Li W (2018) Risk factors for ruptured intracranial aneurysms. Indian J Med Res 147:51–57. https://doi.org/10.4103/ijmr.IJMR_1665_15
Waqas M, Rajabzadeh-Oghaz H, Tutino VM, Vakharia K, Poppenberg KE, Mowla A, Meng H, Siddiqui AH (2019) Morphologic parameters and location associated with rupture status of intracranial aneurysms in elderly patients. World Neurosurg 129:e831–e837. https://doi.org/10.1016/j.wneu.2019.06.045
Weir B, Disney L, Karrison T (2002) Sizes of ruptured and unruptured aneurysms in relation to their sites and the ages of patients. J Neurosurg 96:64–70. https://doi.org/10.3171/jns.2002.96.1.0064
Wiebers DO, Whisnant JP, Huston J, 3rd, Meissner I, Brown RD, Jr., Piepgras DG, Forbes GS, Thielen K, Nichols D, O'Fallon WM, Peacock J, Jaeger L, Kassell NF, Kongable-Beckman GL, Torner JC, International Study of Unruptured Intracranial Aneurysms I (2003) Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet 362:103–110. https://doi.org/10.1016/s0140-6736(03)13860-3
Xiang J, Natarajan SK, Tremmel M, Ma D, Mocco J, Hopkins LN, Siddiqui AH, Levy EI, Meng H (2011) Hemodynamic-morphologic discriminants for intracranial aneurysm rupture. Stroke 42:144–152. https://doi.org/10.1161/STROKEAHA.110.592923
Yasuda R, Strother CM, Taki W, Shinki K, Royalty K, Pulfer K, Karmonik C (2011) Aneurysm volume-to-ostium area ratio: a parameter useful for discriminating the rupture status of intracranial aneurysms. Neurosurgery 68:310–317; discussion 317-318. https://doi.org/10.1227/NEU.0b013e3182010ed0
You SH, Kong DS, Kim JS, Jeon P, Kim KH, Roh HK, Kim GM, Lee KH, Hong SC (2010) Characteristic features of unruptured intracranial aneurysms: predictive risk factors for aneurysm rupture. J Neurol Neurosurg Psychiatry 81:479–484. https://doi.org/10.1136/jnnp.2008.169573
Yu J, Wu Q, Ma FQ, Xu J, Zhang JM (2010) Assessment of the risk of rupture of intracranial aneurysms using three-dimensional cerebral digital subtraction angiography. J Int Med Res 38:1785–1794. https://doi.org/10.1177/147323001003800525
Zhao L, Zhang L, Zhang X, Li Z, Tian L, Wang YX (2014) An analysis of 1256 cases of sporadic ruptured cerebral aneurysm in a single Chinese institution. PLoS One 9:e85668. https://doi.org/10.1371/journal.pone.0085668
Zheng Y, Xu F, Ren J, Xu Q, Liu Y, Tian Y, Leng B (2016) Assessment of intracranial aneurysm rupture based on morphology parameters and anatomical locations. J Neurointerv Surg 8:1240–1246. https://doi.org/10.1136/neurintsurg-2015-012112
Acknowledgments
The authors thank Paul H. Dressel BFA for formatting the illustrations and Debra J. Zimmer for editorial assistance.
Funding
No funding was received in conjunction with this work.
Author information
Authors and Affiliations
Contributions
Conception and design: MW, AHS; acquisition of data: ADG, FC, HHR, MW; analysis and interpretation of data: all authors; drafting the manuscript: MW; critically revising the manuscript: all authors; reviewed submitted version of manuscript: all authors.
Corresponding author
Ethics declarations
Conflict of interest
JMD: Research grant: National Center for Advancing Translational Sciences of the National Institutes of Health under award number KL2TR001413 to the University at Buffalo. Consulting: Medtronic; Honoraria: Neurotrauma Science, LLC; shareholder/ownership interests: Cerebrotech, RIST Neurovascular.
EIL: Shareholder/Ownership interests: NeXtGen Biologics, RAPID Medical, Claret Medical, Cognition Medical, Imperative Care (formerly the Stroke Project), Rebound Therapeutics, StimMed, Three Rivers Medical; National Principal Investigator/Steering Committees: Medtronic (merged with Covidien Neurovascular) SWIFT Prime and SWIFT Direct Trials; Honoraria: Medtronic (training and lectures); Consultant: Claret Medical, GLG Consulting, Guidepoint Global, Imperative Care, Medtronic, Rebound, StimMed; Advisory Board: Stryker (AIS Clinical Advisory Board), NeXtGen Biologics, MEDX, Cognition Medical, Endostream Medical; Site Principal Investigator: CONFIDENCE study (MicroVention), STRATIS Study—Sub I (Medtronic).
HM: Principal investigator of NIH grant 1R01NS091075, R03NS090193, and Canon Medical Systems Corporation grant [no grant number]. Co-founder, Neurovascular Diagnostics, Inc.
MM: Ownership/stock: Serenity medical, Synchron, VICIS; Consultant: Canon Medical, Medtronic; NIH grant support R21NS109575 (Principal Investigator).
AHS: Co-investigator of NIH/NINDS 1R01NS091075; Financial interest/investor/stock options/ownership: Adona Medical, Inc., Amnis Therapeutics, (Purchased by Boston Scientific October 2017), Blink TBI Inc., Buffalo Technology Partners Inc., Cerebrotech Medical Systems, Inc., Cognition Medical, Endostream Medical Ltd., Imperative Care, International Medical Distribution Partners, Neurovascular Diagnostics Inc., Q’Apel Medical Inc., Rebound Therapeutics Corp. (Purchased 2019 by Integra Lifesciences, Corp), Rist Neurovascular Inc., Sense Diagnostics, Inc., Serenity Medical Inc., Silk Road Medical, Spinnaker Medical, Inc., StimMed, Synchron, Three Rivers Medical Inc., Vastrax, LLC, VICIS, Inc., Viseon Inc.; Consultant/advisory board: Amnis Therapeutics, Boston Scientific, Canon Medical Systems USA Inc., Cerebrotech Medical Systems Inc., Cerenovus, Corindus Inc., Endostream Medical Ltd., Imperative Care, Inc. Integra LifeSciences Corp., Medtronic, MicroVention, Minnetronix Neuro, Inc., Northwest University–DSMB Chair for HEAT Trial, Penumbra, Q’Apel Medical Inc., Rapid Medical, Rebound Therapeutics Corp.(Purchased by Integra LifeSciences Corp.), Serenity Medical Inc., Silk Road Medical, StimMed, Stryker, Three Rivers Medical, Inc., VasSol, W.L. Gore & Associates; Principal investigator/steering comment of the following trials: Cerenovus NAPA and ARISE II; Medtronic SWIFT PRIME and SWIFT DIRECT; MicroVention FRED & CONFIDENCE; MUSC POSITIVE; and Penumbra 3D Separator, COMPASS, and INVEST.
KVS: Consulting and teaching for Canon Medical Systems Corporation, Penumbra Inc., Medtronic, and Jacobs Institute. Co-Founder: Neurovascular Diagnostics, Inc.
The remaining authors report no disclosures.
Ethical approval
Institutional review board approval was deemed unnecessary. This submission does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Previous Presentation
Oral Presentation, Congress of Neurological Surgeons Annual Meeting, San Francisco CA, October 19-23, 2019
This article is part of the Topical Collection on Vascular Neurosurgery - Aneurysm
Electronic supplementary material
ESM 1
(DOCX 124 kb)
Rights and permissions
About this article
Cite this article
Waqas, M., Chin, F., Rajabzadeh-Oghaz, H. et al. Size of ruptured intracranial aneurysms: a systematic review and meta-analysis. Acta Neurochir 162, 1353–1362 (2020). https://doi.org/10.1007/s00701-020-04291-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-020-04291-z