Abstract
Background
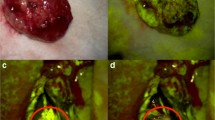
Surgical resection is a key element of the multidisciplinary treatment of cerebral metastases (CMs). Recent studies have highlighted the importance of complete resection of CMs for improving recurrence-free and overall survival rates. This study presents the first data on the use of fluorescein sodium (FL) under the dedicated surgical microscope filter YELLOW 560 nm (Zeiss Meditec, Germany) in patients with CM.
Methods
Thirty patients with CMs of different primary cancers were included (15 females, 15 males; mean age 61.1 years); 200 mg of FL was intravenously injected directly before CM resection. A YELLOW 560 nm filter was used for microsurgical tumor resection and resection control. Surgical reports were evaluated regarding the degree of fluorescent staining, postoperative MRIs regarding the extent of resection [gadolinium (Gd)-enhanced T1-weighted sequence] and the postoperative courses regarding any adverse effects.
Results
Most patients (90.0 %, n = 27) showed bright fluorescent staining, which markedly enhanced tumor visibility. Three patients (10.0 %) (two with adenocarcinoma of the lung and one with melanoma of the skin) showed no or only insufficient FL staining. Another three patients (10.0 %) showed residual tumor tissue in the postoperative MRI examination. In two other patients, radiographic examination could not exclude the possibility of very small areas of residual tumor tissue. Thus, gross-total resection was achieved in 83.3 % (n = 25) of patients. No adverse effects were registered over the postoperative course.
Conclusions
FL and the YELLOW 560 nm filter are safe and practical tools for the resection of CM, but further prospective research is needed to confirm that this advanced technique will improve the quality of CM resection.

Similar content being viewed by others
References
Acerbi F, Broggi M, Eoli M, Anghileri E, Cavallo C, Boffano C, Cordella R, Cuppini L, Pollo B, Schiariti M, Visintini S, Orsi C, La Corte E, Broggi G, Ferroli P (2014) Is fluorescein-guided technique able to help in resection of high-grade gliomas? Neurosurg Focus 36:E5
Alexandru D, Bota DA, Linskey ME (2012) Epidemiology of central nervous system metastases. Prog Neurol Surg 25:13–29
Barone DG, Lawrie TA, Hart MG (2014) Image guided surgery for the resection of brain tumours. Cochrane Database Syst Rev 1:CD009685
Baumert BG, Rutten I, Dehing-Oberije C, Twijnstra A, Dirx MJ, Debougnoux-Huppertz RM, Lambin P, Kubat B (2006) A pathology-based substrate for target definition in radiosurgery of brain metastases. Int J Radiat Oncol Biol Phys 66:187–194
Berger MS (2014) The fluorescein-guided technique. Neurosurg Focus 36:E6
Berghoff AS, Rajky O, Winkler F, Bartsch R, Furtner J, Hainfellner JA, Goodman SL, Weller M, Schittenhelm J, Preusser M (2013) Invasion patterns in brain metastases of solid cancers. Neuro Oncol 15:1664–1672
DeAngelis LM, Currie VE, Kim JH, Krol G, O’Hehir MA, Farag FM, Young CW, Posner JB (1989) The combined use of radiation therapy and lonidamine in the treatment of brain metastases. J Neurooncol 7:241–247
Gates M, Alsaidi M, Kalkanis S (2012) Surgical treatment of solitary brain metastases. Prog Neurol Surg 25:74–81
Kamp MA, Dibue M, Niemann L, Reichelt DC, Felsberg J, Steiger HJ, Szelenyi A, Rapp M, Sabel M (2012) Proof of principle: supramarginal resection of cerebral metastases in eloquent brain areas. Acta Neurochir (Wien) 154:1981–1986
Kamp MA, Dibue M, Santacroce A, Zella SM, Niemann L, Steiger HJ, Rapp M, Sabel M (2013) The tumour is not enough or is it? problems and new concepts in the surgery of cerebral metastases. Ecancermedicalscience 7:306
Kamp MA, Grosser P, Felsberg J, Slotty PJ, Steiger HJ, Reifenberger G, Sabel M (2012) 5-aminolevulinic acid (5-ALA)-induced fluorescence in intracerebral metastases: a retrospective study. Acta Neurochir (Wien) 154:223–228, discussion 228
Lee CH, Kim DG, Kim JW, Han JH, Kim YH, Park CK, Kim CY, Paek SH, Jung HW (2013) The role of surgical resection in the management of brain metastasis: a 17-year longitudinal study. Acta Neurochir (Wien) 155:389–397
Lee J, Baird A, Eliceiri BP (2011) In vivo measurement of glioma-induced vascular permeability. Methods Mol Biol 763:417–422
Li Y, Rey-Dios R, Roberts DW, Valdes PA, Cohen-Gadol AA (2014) Intraoperative fluorescence-guided resection of high-grade gliomas: a comparison of the present techniques and evolution of future strategies. World Neurosurg 82:175–185
Marbacher S, Klinger E, Schwyzer L, Fischer I, Nevzati E, Diepers M, Roelcke U, Fathi AR, Coluccia D, Fandino J (2014) Use of fluorescence to guide resection or biopsy of primary brain tumors and brain metastases. Neurosurg Focus 36:E10
Moore GE (1947) Fluorescein as an agent in the differentiation of normal and malignant tissues. Science 106:130–131
Nduom EK, Yang C, Merrill MJ, Zhuang Z, Lonser RR (2013) Characterization of the blood–brain barrier of metastatic and primary malignant neoplasms. J Neurosurg 119:427–433
Nieder C, Spanne O, Mehta MP, Grosu AL, Geinitz H (2011) Presentation, patterns of care, and survival in patients with brain metastases: what has changed in the last 20 years? Cancer 117:2505–2512
Okuda T, Kataoka K, Yabuuchi T, Yugami H, Kato A (2010) Fluorescence-guided surgery of metastatic brain tumors using fluorescein sodium. J Clin Neurosci 17:118–121
Patchell RA, Tibbs PA, Regine WF, Dempsey RJ, Mohiuddin M, Kryscio RJ, Markesbery WR, Foon KA, Young B (1998) Postoperative radiotherapy in the treatment of single metastases to the brain: a randomized trial. JAMA 280:1485–1489
Patchell RA, Tibbs PA, Walsh JW, Dempsey RJ, Maruyama Y, Kryscio RJ, Markesbery WR, Macdonald JS, Young B (1990) A randomized trial of surgery in the treatment of single metastases to the brain. N Engl J Med 322:494–500
Rabb MF, Burton TC, Schatz H, Yannuzzi LA (1978) Fluorescein angiography of the fundus: a schematic approach to interpretation. Surv Ophthalmol 22:387–403
Rey-Dios R, Cohen-Gadol AA (2013) Technical principles and neurosurgical applications of fluorescein fluorescence using a microscope-integrated fluorescence module. Acta Neurochir (Wien) 155:701–706
Schackert G, Steinmetz A, Meier U, Sobottka SB (2001) Surgical management of single and multiple brain metastases: results of a retrospective study. Onkologie 24:246–255
Schebesch KM, Proescholdt M, Hohne J, Hohenberger C, Hansen E, Riemenschneider MJ, Ullrich W, Doenitz C, Schlaier J, Lange M, Brawanski A (2013) Sodium fluorescein-guided resection under the YELLOW 560 nm surgical microscope filter in malignant brain tumor surgery–a feasibility study. Acta Neurochir (Wien) 155:693–699
Schodel P, Schebesch KM, Brawanski A, Proescholdt MA (2013) Surgical resection of brain metastases-impact on neurological outcome. Int J Mol Sci 14:8708–8718
Stark AM, Tscheslog H, Buhl R, Held-Feindt J, Mehdorn HM (2005) Surgical treatment for brain metastases: prognostic factors and survival in 177 patients. Neurosurg Rev 28:115–119
Stummer W, Pichlmeier U, Meinel T, Wiestler OD, Zanella F, Reulen HJ, Group AL-GS (2006) Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. Lancet Oncol 7:392–401
Vecht CJ, Haaxma-Reiche H, Noordijk EM, Padberg GW, Voormolen JH, Hoekstra FH, Tans JT, Lambooij N, Metsaars JA, Wattendorff AR (1993) Treatment of single brain metastasis: radiotherapy alone or combined with neurosurgery? Ann Neurol 33:583–590
Wen PY, Loeffler JS (2000) Brain metastases. Curr Treat Opt Oncol 1:447–458
Yoo H, Kim YZ, Nam BH, Shin SH, Yang HS, Lee JS, Zo JI, Lee SH (2009) Reduced local recurrence of a single brain metastasis through microscopic total resection. J Neurosurg 110:730–736
Conflicts of interest
All authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript. Schebesch: financial support (training for physicians)-Carl Zeiss Meditec AG, Honoraria-Carl Zeiss Meditec AG.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schebesch, KM., Hoehne, J., Hohenberger, C. et al. Fluorescein sodium-guided resection of cerebral metastases—experience with the first 30 patients. Acta Neurochir 157, 899–904 (2015). https://doi.org/10.1007/s00701-015-2395-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-015-2395-7