Abstract
Background
Resection is recommended for low-grade gliomas, but often it is not performed if the tumor is suspected of invading the primary motor cortex. The study aim is to assess what influence preoperative navigated transcranial magnetic stimulation (nTMS) has on the treatment strategy and clinical outcome for suspected low-grade gliomas in presumed motor eloquent location.
Methods
This paper reports on all our patients with gliomas in the primary motor cortex that were non-enhancing on MRI, since we began using nTMS (n = 11). For the comparison group, we identified the 11 most recent such patients just before we started using nTMS.
Results
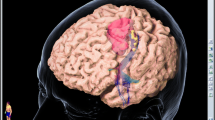
Exact delineation of motor functional versus non-functional cortical tissue was provided by nTMS in all cases, also within the area of altered FLAIR signal. In 6 out of 11 cases, the nTMS mapping result changed the treatment plan towards early and more extensive resection. Only one nTMS patient had another seizure within the follow-up period, whereas four patients in the comparison group had further seizures. In the nTMS group, 1 of 4 patients with pre-op neurological deficits improved by one year; whereas the comparison group had increased neurological deficits in 3 of the 8 patients not having surgery. The median (range) change of tumor volume from baseline to 1 year was −83 % (−67 % to −100 %) in the nTMS group, but +12 % (+40 % to −56 %) in the comparison group (p < 0.001).
Conclusions
nTMS provides accurate motor mapping results also in infiltrative gliomas and enables more frequent and more extensive surgical resection of non-enhancing gliomas in or near the primary motor cortex. The substantial differences observed here in neurological and oncological outcomes suggest that further comparative research is warranted.





Similar content being viewed by others
References
Ashby LS (2010) Low-grade glioma: no longer to treat or not to treat, but why to treat. World Neurosurg 73:e5
Cairncross JG, Laperriere NJ (1989) Low-Grade Glioma: To Treat or Not to Treat? Arch Neurol 46:1238–1239
Cavaliere R, Lopers MBS, Schiff D (2005) Low-grade gliomas: an update on pathology and therapy. Lancet Neurol 4:760–770
Chang EF, Clark A, Smith JS, Polley M-Y, Chang SM, Barbaro NM, Parsa AT, McDermott MW, Berger MS (2011) Functional mapping–guided resection of low-grade gliomas in eloquent areas of the brain: improvement of long-term survival. J Neurosurg 114:566–573
Duffau H, Capelle L, Denvil D, Sichez N, Gatignol P, Taillandier L, Lopes M, Mitchell MC, Roche S, Muller JC, Bitar A, Sichez JP, van Effenterre R (2003) Usefulness of intraoperative electrical subcortical mapping during surgery for low-grade gliomas located within eloquent brain regions: functional results in a consecutive series of 103 patients. J Neurosurg 98:764–778
Duffau H (2006) New concepts in surgery of WHO grade II gliomas: functional brain mapping, connectionism and plasticity – a review. J Neurooncol 79:77–115
Duffau H (2012) The challenge to remove diffuse low-grade gliomas while preserving brain functions. Acta Neurochir 154:569–574
Ginsberg LE, Fuller GN, Hashmi M, Leeds NE, Schomer DF (1998) The Significance of Lack of MR Contrast Enhancement of Supratentorial Brain Tumors in Adults: Histopathological Evaluation of a Series. Surg Neurol 49:436–440
Grier JT, Batchelor T (2006) Low-Grade Gliomas In Adults. Oncologist 11:681–692
Jackson RJ, Fuller GN, Abi-Said D, Lang FF, Gokaslan ZL, Shi WM, Wildrick DM, Sawaya R (2001) Limitations of stereotactic biopsy in the initial management of gliomas. Neuro Oncol 3:193–200
Jakola AS, Myrmel KS, Kloster R, Torp SH, Lindal S, Unsgård G, Solheim O (2012) Comparison of a Strategy Favoring Early Surgical Resection vs a Strategy Favoring Watchful Waiting in Low-Grade Gliomas. JAMA 308:1881–1888
Jakola AS, Unsgård G, Myrmel KS, Kloster R, Torp SH, Lindal S, Solheim O (2012) Low grade gliomas in eloquent locations - implications for surgical strategy, survival and long term quality of life. PLoS One 7:e51450
Kleihues P, Louis DN, Scheithauer BW, Rorke LB, Reifenberger G, Burger PC, Cavenee WK (2002) The WHO Classification of Tumors of the Nervous System. J Neuropathol Exp Neurol 61:215–225
Kombos T, Suess O, Ciklatekerlio O, Brock M (2001) Monitoring of Intraoperative Motor Evoked Potentials to Increase the Safety of Surgery in and around the Motor Cortex. J Neurosurg 95:608–614
Kombos T, Kopetsch O, Suess O, Brock M (2003) Does Preoperative Paresis Influence Intraoperative Monitoring of the Motor Cortex? J Clin Neurophysiol 20:129–134
Kombos T, Picht T, Suess O (2008) Electrical Excitability of the Angular Gyrus. J Clin Neurophysiol 25:340–345
Kombos T, Picht T, Derdilopoulos A, Suess O (2009) Impact of Intraoperative Neurophysiological Monitoring on Surgery of High-Grade Gliomas. J Clin Neurophysiol 26:422–425
Kondziolka D, Lunsford LD, Martinez AJ (1993) Unreliability of contemporary neurodiagnostic imaging in evaluating suspected adult supratentorial (low-grade) astrocytoma. J Neurosurg 79:533–536
Krieg SM, Shiban E, Buchmann N, Gempt J, Foerschler A, Meyer B, Ringel F (2012) Utility of presurgical navigated transcranial magnetic brain stimulation for the resection of tumors in eloquent motor areas. J Neurosurg 116:994–1001
Kros JM (2011) Grading of Gliomas: The Road from Eminence to Evidence. J Neuropathol Exp Neurol 70:101–109
Lang FF, Gilbert MR (2006) Diffusely Infiltrative Low-Grade Gliomas in Adults. J Clin Oncol 24:1236–1245
Picht T, Wachter D, Mularski S, Kuehn B, Brock M, Kombos T, Suess O (2008) Functional Magnetic Resonance Imaging and Cortical Mapping in Motor Cortex Tumor Surgery: Complementary Methods. Zentralbl Neurochir 69:1–6
Picht P, Schmidt S, Brandt S, Frey D, Hannula H, Neuvonen T, Karhu J, Vajkoczy P, Suess O (2011) Preoperative Functional Mapping for Rolandic Brain Tumor Surgery: Comparison of Navigated Transcranial Magnetic Stimulation to Direct Cortical Stimulation. Neurosurgery 69:581–589
Picht T, Schulz J, Hanna M, Schmidt S, Suess O, Vajkoczy P (2012) Assessment of the Influence of Navigated Transcranial Magnetic Stimulation on Surgical Planning for Tumors in or Near the Motor Cortex. Neurosurgery 70:1248–1257
Piepmeier JM (2009) Current concepts in the evaluation and management of WHO grade II gliomas. J Neurooncol 92:253–259
Pouratian N, Asthagiri A, Jagannathan J, Shaffey ME, Schiff D (2007) Surgery Insight: the role of surgery in the management of low-grade gliomas. Nat Clin Pract Neurol 3:628–639
Recht LD, Lew R, Smith TW (1992) Suspected Low-grade Glioma: Is Deferring Treatment Safe? Ann Neurol 31:431–436
Sanai N, Berger MS (2008) Glioma Extent of Resection and Its Impact on Patient Outcome. Neurosurgery 62:753–762
Scott JN, Brasher PMA, Sevick RJ, Rewcastle NB, Forsyth PA (2002) How often are nonenhancing supratentorial gliomas malignant? A population study. Neurology 59:947–949
Seiz M, Freyschlag CF, Schenkel S, Weiss C, Thomé C, Schmieder K, Stummer W, Tuettenberg J (2011) Management of Patients With Low-Grade Gliomas – A Survey Among German Neurosurgical Departments. Cent Eur Neurosurg 72:186–191
Soffietti R, Baumert BG, Bello L, von Deimling A, Duffau H, Frénay M, Grisold W, Grant R, Graus F, Hoang-Xuan K, Klein M, Melin B, Rees J, Siegal T, Smits A, Stupp R, Wick W (2010) Guidelines on management of low-grade gliomas: report of an EFNS-EANO Task Force. Eur J Neurol 17:1124–1133
Suess O, Suess S, Brock M, Kombos T (2006) Intraoperative Electrocortical Stimulation of Brodman Area 4: A 10-Year Analysis of 255 Cases. Head Face Med 2:20
Warnke PC (2010) A 31-Year-Old Woman With a Transformed Low-grade Glioma. JAMA 303:967–976
Whittle IR (2004) The Dilemma of Low Grade Glioma. J Neurol Neurosurg Psychiatry 75(Suppl II):ii31–ii36
Acknowledgments
We would like to thank Michael Hanna, PhD, (Mercury Medical Research & Writing) for providing publication consulting, statistical analysis, and medical writing services. We would also like to thank Adela Castelló, MSc, DPH, (Mercury Medical Research & Writing) for some recommendations on statistics and publishing.
Conflicts of interest
The research reported in this article was supported in part by a grant from the Berlin Cancer Society. Dr. Picht has served as a speaker for Nexstim OY, the manufacturer of the device used in this study. Dr Picht and Dr. Schulz had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
Comment
Picht et al. present a study were they assessed the usefulness of preoperative navigated transcranial magnetic stimulation for the surgery of presumed low grade astrocytomas. This topic is interesting as nTMS is a relatively new tool, is not part of the standard armamentarium of most neurosurgical centers and therefore its use is limited and its usefulness still uncertain.
The goal of the study is to define the impact of this technology on the surgical results and on the overall clinical course of patients with presumed WHOII gliomas in or invading the motor cortex. The authors describe their experience with 11 patients and show convincingly good results in terms of extent of resection and low postoperative deficits. Every neurosurgeon knows from experience that lesions in the primary motor cortex are challenging and prone to postoperative motor deficits. Therefore we can appreciate the good results shown by the authors and reasonably deduct that nTMS probably provided an advantage, be it solely the confidence to offer surgery and attempt an extensive resection.
The comparison with an historical group can be useful for the assessment of new technology that is not easily subjected to randomized control trials and the number of patients is low. However, this requires homogenous groups which is not the case here and this is the main flaw of this study. Scientifically, the historical groups are not comparable. The study assesses what the availability of TMS changes in the overall management of these patients. However, this study does not compare surgery with or without TMS nor does it provide comparative data on observation vs Surgery (with or without TMS). Therefore any conclusion about the safety of surgery or the specific contribution of TMS to surgical outcomes cannot be drawn. Furthermore heterogeneity between groups is introduced by the fact that there were grade II and III tumors in both groups but some historical cases do not have a definitive diagnosis.
After all it could well be that surgery with DES alone is equal to nTMS and that the number of patients undergoing surgery in the nTMS group are the result of a change in the surgical philosophy for these lesions overtime.
Ivan Radovanovic
Toronto, Canada
Thomas Picht and Juliane Schulz contributed equally to this paper.
Rights and permissions
About this article
Cite this article
Picht, T., Schulz, J. & Vajkoczy, P. The preoperative use of navigated transcranial magnetic stimulation facilitates early resection of suspected low-grade gliomas in the motor cortex. Acta Neurochir 155, 1813–1821 (2013). https://doi.org/10.1007/s00701-013-1839-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-013-1839-1