Abstract
Rationale
Arterial vasospasm has rarely been reported following temporal lobectomy for intractable epilepsy.
Case presentation
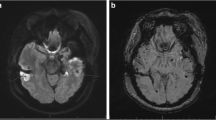
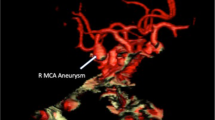
A 31-year-old patient presented with a global aphasia 2 days after a left dominant anteromesial temporal lobectomy for intractable epilepsy. Magnetic resonance imaging on 5th post-operative day revealed severe narrowing of M1 segment of the left middle cerebral artery (MCA) and Transcranial Doppler (TCD) ultrasonography an increased velocity of the MCA that suggested a severe vasospasm. The patient received continuous intravenous hyperhydratation and nimodipine; aphasia improved within 24 h and resolved completely within 6 weeks, associated with velocity reduction on control TCD.
Conclusion
Transient vasospasm is a likely underestimated cause of focal deficit following temporomesial resection that deserves appropriate treatment.

Similar content being viewed by others
References
Aoki N, Origitano TC, al-Mefty O (1995) Vasospasm after resection of skull base tumours. Acta Neurochir (Wien) 132:53–58. doi:10.1007/BF01404848
Bejjani GK, Duong DH, Kalamarides M, Ziyal I, Sullivan BJ (1997) Cerebral vasospasm after tumour resection. A case report. Neurochirurgie 43:164–168
Bejjani GK, Sekhar LN, Yost AM, Bank WO, Wright DC (1999) Vasospasm after cranial base tumour resection: pathogenesis, diagnosis, and therapy. Surg Neurol 52:577–583. doi:10.1016/S0090-3019(99)00108-1 discussion 583-574
Desmurget M, Bonnetblanc F, Duffau H (2007) Contrasting acute and slow-growing lesions: a new door to brain plasticity. Brain 130:898–914. doi:10.1093/brain/awl300
Duffau H, Capelle L, Sichez N, Denvil D, Lopes M, Sichez JP, Bitar A, Fohanno D (2002) Intra-operative mapping of the sub-cortical language pathways using direct stimulations. An anatomo-functional study. Brain 125:199–214. doi:10.1093/brain/awf016
Dull C, Torbey MT (2005) Cerebral vasospasm associated with intra-ventricular haemorrhage. Neurocrit Care 3:150–152. doi:10.1385/NCC:3:2:150
Garcia-Morales I, Garcia MT, Galan-Davila L, Gomez-Escalonilla C, Saiz-Diaz R, Martinez-Salio A, de la Pena P, Tejerina JA (2002) Periodic lateralised epileptiform discharges: aetiology, clinical aspects, seizures, and evolution in 130 patients. J Clin Neurophysiol 19:172–177. doi:10.1097/00004691-200203000-00009
Hansen-Schwartz J (2004) Cerebral vasospasm: a consideration of the various cellular mechanisms involved in the pathophysiology. Neurocrit Care 1:235–246. doi:10.1385/NCC:1:2:235
Kobayashi M, Takayama H, Mihara B, Kawase T (2002) Severe vasospasm caused by repeated intra-ventricular haemorrhage from small arterio-venous malformation. Acta Neurochir (Wien) 144:405–406. doi:10.1007/s007010200059
Kothbauer K, Schroth G, Seiler RW, Do DD (1995) Severe symptomatic vasospasm after rupture of an arterio-venous malformation. AJNR Am J Neuroradiol 16:1073–1075
Maeda K, Kurita H, Nakamura T, Usui M, Tsutsumi K, Morimoto T, Kirino T (1997) Occurrence of severe vasospasm following intra-ventricular haemorrhage from an arterio-venous malformation. Report of two cases. J Neurosurg 87:436–439
Oertel M, Boscardin WJ, Obrist WD, Glenn TC, McArthur DL, Gravori T, Lee JH, Martin NA (2005) Post-traumatic vasospasm: the epidemiology, severity, and time course of an underestimated phenomenon: a prospective study performed in 299 patients. J Neurosurg 103:812–824
Schaller C, Jung A, Clusmann H, Schramm J, Meyer B (2004) Rate of vasospasm following the trans-sylvian versus trans-cortical approach for selective amygdalo-hippocampectomy. Neurol Res 26:666–670. doi:10.1179/016164104225015921
Schaller C, Klemm E, Haun D, Schramm J, Meyer B (2002) The trans-sylvian approach is “minimally invasive” but not “atraumatic”. Neurosurgery 51:971–976. doi:10.1097/00006123-200210000-00022 discussion 976-977
Schaller C, Zentner J (1998) Vasospastic reactions in response to the trans-sylvian approach. Surg Neurol 49:170–175. doi:10.1016/S0090-3019(97)00283-8
Yanaka K, Hyodo A, Tsuchida Y, Yoshii Y, Nose T (1992) Symptomatic cerebral vasospasm after intra-ventricular haemorrhage from ruptured arterio-venous malformation. Surg Neurol 38:63–67. doi:10.1016/0090-3019(92)90214-8
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
This interesting case report reminds us that even the most uneventful surgical procedure can lead to a postoperative complication. A point of interest is that TCD should be part of the work up in case of unexpected postoperative neurological deficits.
Mario Zuccarello
Mayfield Clinic, USA
Rights and permissions
About this article
Cite this article
Mandonnet, E., Chassoux, F., Naggara, O. et al. Transient symptomatic vasospasm following antero-mesial temporal lobectomy for refractory epilepsy. Acta Neurochir 151, 1723–1726 (2009). https://doi.org/10.1007/s00701-009-0314-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-009-0314-5