Summary.
Lesions ventral to the brainstem in the retrosellar and interpeduncular region are major challenges to the surgeon because of their location at great depth in the centre of the cranial base. We report the operative management of a patient with a meningioma in an unusual location, extending from the upper clivus, retrosellar and interpeduncular region into the suprasellar area up to the level of the foramen of Monro.
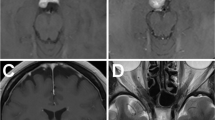
A 41-year-old man presented with a 3-month history of progressive visual disturbance, episodic headache and signs and symptoms of endocrinological disturbance. Magnetic resonance imaging (MRI) studies showed a homogeneously enhancing tumour ventral to the brainstem with large cranio-caudal extension from the upper clivus to the suprasellar area.
Operative removal was planned in two stages. First, through a right lateral suboccipital retrosigmoid craniectomy the caudal portion of the tumour at the upper clivus and prepontine region was removed. Second, the residual suprasellar part of the tumour was removed totally through a fronto-lateral craniotomy on the right side one week later.
When a tumour is very large or involves different areas of the skull base, it is necessary to decide between removal in one stage, which requires a complex and time consuming skull base approach, or in multiple stages. Our case demonstrates how a retrosellar meningioma extending to the suprasellar region can be totally removed using two simple skull base approaches without the risk of compromise to venous drainage and without the need for extensive bone removal as described in other skull base approaches.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Published online March 3, 2003
Correspondence: Makoto Nakamura, M.D., Department of Neurosurgery, Nordstadt Hospital, Haltenhoffstr. 41, 30167 Hannover, Germany.
Rights and permissions
About this article
Cite this article
Nakamura, M., Samii, M. Surgical management of a meningioma in the retrosellar region. Acta Neurochir (Wien) 145, 215–220 (2003). https://doi.org/10.1007/s00701-002-1053-z
Issue Date:
DOI: https://doi.org/10.1007/s00701-002-1053-z