Abstract
Background and purpose
We investigated the impact of postoperative changes in the psoas muscle mass index (PMI) after gastrectomy and S1 adjuvant chemotherapy (AC) on the long-term outcomes of elderly patients with gastric cancer.
Methods
We reviewed the medical records of 228 patients aged over 75 years, who underwent distal, proximal, or total gastrectomy between January, 2013 and March 2017. Among these patients, 78 with pStage IIA-IIIC who survived for at least 1 year without recurrence after gastrectomy were the subjects of this analysis.
Results
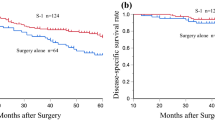
The log-rank test using the cut-off value from the rate of change in PMI from 6 to 12 months after gastrectomy (late rate of decrease) showed significantly poorer prognosis for the group above the cut-off value for both overall survival (OS) and recurrence-free survival (RFS) (RFS: PMI decrease ≥ 1.55%, p < 0.001; OS: PMI decrease ≥ 1.55%, p < 0.001). Patients with a relative dose intensity of S1 below 68.7% and a late rate of decrease in PMI above 1.55% were found to have a poor prognosis.
Conclusion
It is necessary to prevent decline in the PMI of elderly patients from 6 months after gastrectomy and to administer adjuvant chemotherapy with about two-thirds or more RDI of S1 to improve their survival prognosis.







Similar content being viewed by others
References
Kitamura K, Yamaguchi T, Taniguchi H, Hagiwara A, Yamane T, Sawai K, Takahashi T. Clinicopathological characteristics of gastric cancer in the elderly. Br J Cancer. 1996;73:798–802.
Jung KW, Won YJ, Kong HJ, Oh CM, Seo HG, Lee JS. Cancer statistics in Korea: incidence, mortality, survival and prevalence in 2010. Cancer Res Treat. 2013;45:1–14.
Saif MW, Makrilia N, Zalonis A, Merikas M, Syrigos K. Gastric cancer in the elderly: an overview. Eur J Surg Oncol. 2010;36:709–17.
Isobe Y, Nashimoto A, Akazawa K, et al. Gastric cancer treatment in Japan: 2008 annual report of the JGCA nationwide registry. Gastric Cancer. 2011;14:301–16.
Japanese Gastric Cancer Association Group. Japanese gastric cancer treatment guidelines 2014 (ver 4). Gastric Cancer. 2017;20:1–19.
Sakuramoto S, Sasako M, Yamaguchi T, et al. Adjuvant chemotherapy for gastric cancer with S-1, an oral fluoropyrimidine. N Engl J Med. 2007;357:1810–20.
Sasako M, Sakuramoto S, Katai H, et al. Five-year outcomes of a randomized phase III trial comparing adjuvant chemotherapy with S-1 versus surgery alone in stage II or III gastric cancer. J Clin Oncol. 2011;29:4387–93.
Yoshida K, Kodera Y, Kochi M, et al. Addition of docetaxel to oral fluoropyrimidine improves efficacy in patients with stage III gastric cancer: interim analysis of JACCRO GC-07, a randomized controlled trial. J Clin Oncol. 2019;37:1296–304.
Wedding U, Honecker F, Bokemeyer C, et al. Tolerance to chemotherapy in elderly patients with cancer. Cancer Control. 2007;14:44–56.
Sakuramoto S, Yamashita K, Watanabe M. Newly emerging standard chemotherapies for gastric cancer and clinical potential in elderly patients. World J Gastrointest Oncol. 2009;1:47–54.
Prado CM, Baracos VE, McCargar LJ, et al. Body composition as an independent determinant of 5-fluorouracil-based chemotherapy toxicity. Clin Cancer Res. 2007;13:3264–8.
Yamaoka Y, Fujitani K, Tsujinaka T, et al. Skeletal muscle loss after total gastrectomy, exacerbated by adjuvant chemotherapy. Gastric Cancer. 2015;18:382–9.
Kanazawa Y, Yamada T, Kakinuma D, et al. Skeletal muscle mass depletion after gastrectomy negatively affects the prognosis of patients with gastric cancer. Anticancer Res. 2020;40:4271–9.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, et al. Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in older people. Age Ageing. 2010;39:412–23.
Anker SD, Coats AJ, Morley JE, et al. Muscle wasting disease: a proposal for a new disease classifcation. J Cachexia Sarcopenia Muscle. 2014;5:1–3.
Mansoor O, Beaufrere B, Boirie Y, et al. Increased mRNA levels for components of the lysosomal, Ca2+-activated, and ATP-ubiquitin-dependent proteolytic pathways in skeletal muscle from head trauma patients. Proc Natl Acad Sci USA. 1996;93:2714–8.
Otsuji E, Fujiyama J, Takagi T, et al. Results of total gastrectomy with extended lymphadenectomy for gastric cancer in elderly patients. J Surg OncoI. 2005;91:232–6.
Sheetz KH, Zhao L, Holcombe SA, et al. Decreased core muscle size is associated with worse patient survival following esophagectomy for cancer. Dis Esophagus. 2013;26:716–22.
Onodera T, Goseki N, Kosaki G. Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai Zasshi. 1984;85:1001–5.
Adams JF. The clinical and metabolic consequences of total gastrectomy. I. Morbidity, weight, and nutrition. Scand J Gastroenterol. 1967;2:137–49.
Yong HL, Seung JH, Hyeon CK, et al. Gastrectomy for early gastric cancer is associated with decreased cardiovascular mortality in association with postsurgical metabolic changes. Ann Surg Oncol. 2013;20:1250–7.
Ji HP, Eunjung K, Eun MS, et al. Prediction model for screening patients at risk of malnutrition after gastric cancer surgery. Ann Surg Oncol. 2021;22:4471–81.
Fein M, Fuchs KH, Thalheimer A, et al. Long-term benefits of Roux-en-Y pouch reconstruction after total gastrectomy: a randomized trial. Ann Surg. 2008;247:759–65.
Tsuburaya A, Noguchi Y, Yoshikawa T, et al. Long-term effect of radical gastrectomy on nutrition and immunity. Surg Today. 1993;23:320–4.
Abdiev S, Kodera Y, Fujiwara M, et al. Nutritional recovery after open and laparoscopic gastrectomies. Gastric Cancer. 2011;14:144–9.
Kim AR, Cho J, Hsu YJ, et al. Changes of quality of life in gastric cancer patients after curative resection: a longitudinal cohort study in Korea. Ann Surg. 2012;256:1008–13.
Takachi K, Doki Y, Ishikawa O, et al. Postoperative ghrelin levels and delayed recovery from body weight loss after distal or total gastrectomy. J Surg Res. 2006;130:1–7.
Takiguchi S, Adachi S, Yamamoto K, et al. Mapping analysis of ghrelin producing cells in the human stomach associated with chronic gastritis and early cancers. Dig Dis Sci. 2012;57:1238–46.
Cesari M, Leeuwenburgh C, Lauretani F, et al. Frailty syndrome and skeletal muscle: results from the Invecchiare in Chianti study. Am J Clin Nutr. 2006;83:1142–8.
Zhuang CL, Huang DD, Pang WY, et al. Sarcopenia is an independent predictor of severe postoperative complications and long-term survival after radical gastrectomy for gastric cancer: analysis from a large-scale cohort. Medicine. 2016;95:e3164.
Tamandl D, Paireder M, Asari R, et al. Markers of sarcopenia quantified by computed tomography predict adverse long-term outcome in patients with resected oesophageal or gastro-oesophageal junction cancer. Eur Radiol. 2016;26:1359–67.
Zheng ZF, Lu J, Zheng CH, et al. A novel prognostic scoring system based on preoperative sarcopenia predicts the long-term outcome for patients after R0 resection for gastric cancer: experiences of a high-volume center. Ann Surg Oncol. 2017;24:1795–803.
Dodson S, Baracos VE, Jatoi A, et al. Muscle wasting in cancer cachexia: clinical implications, diagnosis, and emerging treatment strategies. Annu Rev Med. 2011;62:265–79.
Hojman P, Dethlefsen C, Brandt C, et al. Exercise-induced muscle-derived cytokines inhibit mammary cancer cell growth. Am J Physiol Endocrinol Metab. 2011;301:E504–10.
Pedersen BK, Febbraio MA. Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nat Rev Endocrinol. 2012;8:457–65.
Bang YJ, Kim YW, Yang HK, et al. Adjuvant capecitabine and oxaliplatin for gastric cancer after D2 gastrectomy (CLASSIC): a phase 3 open-label, randomised controlled trial. Lancet. 2012;28(379):315–21.
Karaca M, Tural D, Kocoglu H, et al. Adjuvant chemotherapy for gastric cancer in elderly patients has same benefits as in younger patients. Cancer Res Ther. 2018;14:593–6.
Jin Y, Qiu MZ, Wang DS, et al. Adjuvant chemotherapy for elderly patients with gastric cancer after D2 gastrectomy. PLoS ONE. 2013;8:e53149.
Jo JC, Baek JH, Koh SJ, et al. Adjuvant chemotherapy for elderly patients (aged 70 or older) with gastric cancer after a gastrectomy with D2 dissection: a single center experience in Korea. Asia Pac J Clin Oncol. 2015;11:282–7.
Ogawa K, Honda M, Akashi Y, et al. Comparison of 2- and 4-week S-1 administration as adjuvant chemotherapy for advanced gastric cancer. Int J Clin Oncol. 2020;25:1807–13.
Miyatani K, Saito H, Shimizu S, et al. Late start and insufficient S-1 dose in adjuvant chemotherapy can lead to poor prognosis in stage II/III gastric cancer. Int J Clin Oncol. 2019;24:1190–6.
Tatebe S, Tsujitani S, Nakamura S, et al. Feasibility study of alternate-day S-1 as adjuvant chemotherapy for gastric cancer: a randomized controlled trial. Gastric Cancer. 2014;17:508–13.
Read JA, Beale PJ, Volker DH, et al. Nutrition intervention using an eicosapentaenoic acid (EPA)—containing supplement in patients with advanced colorectal cancer. Effects on nutritional and inflammatory status: a phase II trial. Support Care Cancer. 2007;15:301–7.
Gonçalves Dias MC, de Fátima Nunes Marucci M, et al. Nutritional intervention improves the caloric and proteic ingestion of head and neck cancer patients under radiotherapy. Nutr Hosp. 2005;20:320–5.
Vikberg S, Sörlén N, Brandén L, et al. Effects of resistance training on functional strength and muscle mass in 70-year-old individuals with pre-sarcopenia: a randomized controlled trial. J Am Med Dir Assoc. 2019;20:28–34.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fujihata, S., Sakuramoto, S., Morimoto, Y. et al. Impact of loss of skeletal muscle mass within 6–12 months after gastrectomy and S1 adjuvant chemotherapy on the survival prognosis of elderly patients with gastric cancer. Surg Today 52, 1472–1483 (2022). https://doi.org/10.1007/s00595-022-02489-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-022-02489-5