Abstract
Purpose
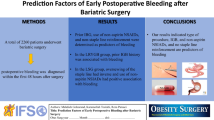
To promote proper management of postoperative bleeding, we investigated the clinical manifestations, predisposing factors, diagnostic approaches, and treatments of bleeding complications after gastric cancer surgery.
Methods
Using a prospectively constructed database, we reviewed retrospectively 39 patients who suffered bleeding complications from among a total 1027 patients who underwent surgery for gastric cancer between 2004 and 2008.
Results
Operating time (hazard ratio [HR] 1.842, 95% confidence interval [CI] 1.524–2.367) and body mass index (HR 1.454, 95% CI 1.128–1.792) were significant predisposing factors for postoperative bleeding after gastric cancer surgery. Luminal bleeding occurred in 16 patients: as simple anastomosis site bleeding, treated successfully with conservative or endoscopic treatment, in 13; and as pseudoaneurysmal bleeding in 3, treated successfully with surgery in 2, but resulting in the death of 1. Abdominal bleeding occurred in 23 patients, requiring surgery in 9 and arterial embolization in 1. The most common finding at reoperation was bleeding from the mesocolon surface. The mean hospital stay of patients with postoperative bleeding was 21 (±20) days.
Conclusions
Postoperative bleeding can be managed successfully with a tailored approach, considering its origins and clinical manifestations. Arterial pseudoaneurysms are a rare cause of luminal bleeding, but they can be fatal and should be suspected when extensive luminal bleeding presents after gastric cancer surgery.
Similar content being viewed by others
References
Hu JK, Yang K, Zhang B, Chen XZ, Chen ZX, Chen JP. D2 plus para-aortic lymphadenectomy versus standardized D2 lymphadenectomy in gastric cancer surgery. Surg Today 2009;39:207–213.
Deguili M, Sasako M, Calgaro M, Garino M, Rebecchi F, Mineccia M, et al. Morbidity and mortality after D1 and D2 gastrectomy for cancer: Interim analysis of the Italian Gastric Cancer Study Group (IGCSG) randomized surgical trial. EJSO 2004;30:303–308.
Sano T, Sasako M, Yamamoto S, Nahimoto A, Kurita A, Hiratsuka M, et al. Gastric cancer surgery: morbidity and mortality results from a prospective randomized controlled trial comparing D2 and extended para-aortic lymphadenectomy-Japan Clinical Oncology Group Study 9501. JCO 2004;22:2767–2773.
Kim MC, Kim W, Kim HH, Ryu SW, Ryu SY, Song KY, et al. Group KLGSSK. Risk factors associated with complication following laparoscopy-assisted gastrectomy for gastric cancer: A large-scale Korean multicenter study. Ann Surg Oncol 2008;15:2692–2700.
Park DJ, Lee HJ, Kim JJ, Yang HK, Lee KU, Choe KJ. Predictors of operative morbidity and mortality in gastric cancer surgery. Br J Surg 2005;92:1099–1102.
Japanese Gastric Cancer Association. Japanese Classification of Gastric Carcinoma. 2nd English Edition. Gastric Cancer 1998;1:10–24.
Uyama I, Oqiwara H, Takahara T, Kikuchi K, Lida S, Jobota T, et al. Spleen and pancreas preserving total gastrectomy with superextended lymphadenectomy including dissection of the paraaortic lymph nodes for gastric cancer. JCOI 1996;63:268–270.
Yuan Y, Wang C, Hunt RH. Endoscopic clipping for acute nonvariceal upper-GI bleeding: a meta-analysis and critical appraisal of randomized controlled trials. Gastrointest Endosc 2008;68:339–351.
Cooper GS, Chak A, Way LE, Hammar PJ, Harper DL, Rosenthal GE. Early endoscopy in upper gastrointestinal hemorrhage: association with recurrent bleeding, surgery, and length of hospital stay. Gastrointest Endosc 1999;49:145–152.
Blanc T, Cortes A, Goere D, Sibert A, Pessaux P, Belghiti J, et al. Hemorrhage after pancreaticoduodenectomy: when is surgery still indicated? Am J Surg 2007;194:3–9.
Ellison EC. Evidence-based management of hemorrhage after pancreaticoduodenectomy. Am J Surg 2007;194:10–12.
Kim DY, Joo JK, Ryu SY, Kim YJ, Kim SK, Jung YY. Pseudoaneurysm of gastroduodenal artery following radical gastrectomy for gastric carcinoma patients. World J Gastroenterol 2003;9:2878–2879.
Piffaretti G, Tozzi M, Carrafiello G, Caronno R, Legana D, Recaldini C, et al. A case of gastroduodenal artery aneurysm in a HIV-positive patient treated by combined percutaneous thrombin injection and endovascular coil embolization. J Cardiovasc Surg (Torino) 2008;49:659–661.
Lefkovitz Z, Cappell MS, Kaplan M, Mitty H, Gerard P. Radiology in the diagnosis and therapy of gastrointestinal bleeding. Gastroenterol Clin North Am 2000;29:489–512.
Neuman HB, Zarzaur BL, Meyer AA, Cairns BA, PB R. Superselective catheterization and embolization as fist line therapy for lower gastrointestinal bleeding. Am Surg 2005;71:539–544.
Moulton MJ, Creswell LL, Mackey ME, Cox JL, Rosenbloom M. Reexploration for bleeding is a risk factor for adverse outcomes after cardiac operations. J Thorac Cardiovasc Surg 1996;111:1037–1046.
Hagiwara A, Sawai K, Sakakura C, Shirasu M, Ohagaki M, Yamasaki J, et al. Complete omentectomy and extensive lymphadenectomy with gastrectomy improves the survival of gastric cancer patients with metastases in the adjacent peritoneum. Hepatogastroenterology 1998;45:1922–1929.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Jeong, O., Park, Y.K., Ryu, S.Y. et al. Predisposing factors and management of postoperative bleeding after radical gastrectomy for gastric carcinoma. Surg Today 41, 363–368 (2011). https://doi.org/10.1007/s00595-010-4284-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-010-4284-2