Abstract
Purpose
A surgical resection for locally advanced non-small cell lung carcinoma (NSCLC) remains controversial. This study analyzed the clinicopathological profile and surgical outcome of patients with locally advanced NSCLC to identify the predictors of survival.
Methods
This study retrospectively analyzed clinical data from 86 patients with pathological T3 or T4 primary NSCLC treated at Chiba University Hospital, and evaluated prognostic factors.
Results
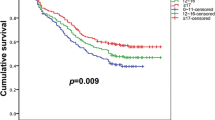
Sixty-eight of 86 cases were treated with a complete resection, and 18 were evaluated as an incomplete resection. The 5-year overall survival rate of all cases was 45.7%. Univariate analyses of survival were performed to determine the predictors of overall survival in patients with pathological T3 or T4 NSCLC. Age of 70 years or more, tumor length more than 5 cm, lymph node metastases, incomplete resection, and histology of non-adenocarcinoma were significantly associated with an unfavorable prognosis. Multivariate analyses revealed that older age, incomplete resection, and lymph node metastases were independent predictors of shorter survival.
Conclusion
A complete resection for selected cases is acceptable in the management of T3 or T4 NSCLC.
Similar content being viewed by others
References
Riquet M, Lang-Lazdunski L, Le PB, Dujon A, Souilamas R, Danel C, et al. Characteristics and prognosis of resected T3 non-small cell lung cancer. Ann Thorac Surg 2002;73:253–258.
Burkhart HM, Allen MS, Nichols FC 3rd, Deschamps C, Miller DL, Trastek VF, et al. Results of en bloc resection for bronchogenic carcinoma with chest wall invasion. J Thorac Cardiovasc Surg 2002;123:670–675.
Martini N, Yellin A, Ginsberg RJ, Bains MS, Burt ME, McCormack PM, et al. Management of non-small cell lung cancer with direct mediastinal involvement. Ann Thorac Surg 1994;58:1447–1451.
Osaki T, Sugio K, Hanagiri T, Takenoyama M, Yamashita T, Sugaya M, et al. Survival and prognostic factors of surgically resected T4 non-small cell lung cancer. Ann Thorac Surg 2003;75:1745–1751.
Perrot M, Fadel E, Mussot S, de Palma A, Chapelier A, Dartevelle P. Resection of locally advanced (T4) non-small cell lung cancer with cardiopulmonary bypass. Ann Thorac Surg 2005;79:1691–1696.
Naruke T, Tsuchiya R, Kondo H, Asamura H. Prognosis and survival after resection for bronchogenic carcinoma based on the 1997 TNM-staging classification: the Japanese experience. Ann Thorac Surg 2001;71:1759–1764.
Doddoli C, D’Journo B, Le Pimpec-Barthes F, Dujon A, Foucault C, Thomas P, et al. Lung cancer invading the chest wall: a plea for en-bloc resection but the need for new treatment strategies. Ann Thorac Surg 2005;80:2032–2040.
Downey RJ, Martini N, Rusch VW, Bains MS, Korst RJ, Ginsberg RJ. Extent of chest wall invasion and survival in patients with lung cancer. Ann Thorac Surg 1999;68:188–193.
Magdeleinat P, Alifano M, Benbrahem C, Spaggiari L, Porrello C, Puyo P, et al. Surgical treatment of lung cancer invading the chest wall: results and prognostic factors. Ann Thorac Surg 2001;71:1094–1099.
Ichinose Y, Fukuyama Y, Asoh H, Ushijima C, Okamoto T, Ikeda J, et al. Induction chemoradiotherapy and surgical resection for selected stage IIIB non-small-cell lung cancer. Ann Thorac Surg 2003;76:1810–1814.
Stamatis G, Eberhardt W, Stüben G, Bildat S, Dahler O, Hillejan L. Preoperative chemoradiotherapy and surgery for selected non-small cell lung cancer IIIB subgroups: long-term results. Ann Thorac Surg 1999;68:1144–1149.
Grunenwald DH, André F, Le Péchoux C, Girard P, Lamer C, Laplanche A, et al. Benefit of surgery after chemoradiotherapy in stage IIIB (T4 and/or N3) non-small cell lung cancer. J Thorac Cardiovasc Surg 2001;122:796–802.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Iyoda, A., Hiroshima, K., Moriya, Y. et al. Predictors of postoperative survival in patients with locally advanced non-small cell lung carcinoma. Surg Today 40, 725–728 (2010). https://doi.org/10.1007/s00595-009-4127-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-009-4127-1